Abstract
Purpose
This systematic review is aimed at answering the following questions: 1) Is near-infrared spectroscopy (NIRS) clinically effective in detecting cerebral desaturation during heart surgery? 2) Are these results based on studies with solid methodology?
Sources
MEDLINE, internet, and hand searches up to February 2004 for English and French papers on NIRS.
Principal findings
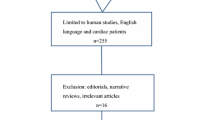
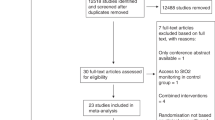
Forty-eight papers were retrieved, with a total of 5,931 cardiac surgery patients monitored by NIRS. More than 83% of patients underwent coronary artery bypass graft surgery. The majority of studies were prospective for the monitored group. Clinically, NIRS monitoring appears to detect brain desaturation episodes encountered during surgery. However, the majority of studies retrieved suffered from major methodological limitations and a low level of evidence. NIRS validity vs jugular bulb oximetry is questioned together with its predictive value in identifying those who will suffer postoperatively from neurological deficits. The sole randomized controlled trial appears to have recorded negative results in this respect.
Conclusion
The clinical application of NIRS in heart surgery as a brain-monitoring device seems interesting. However, NIRS has to be investigated more rigorously to prove its clinical utility in cardiac surgery.
Résumé
Objectif
Répondre à ces questions: 1) La spectroscopie par infrarouge (SPIR) est-elle efficace pour la détection clinique de la désaturation cérébrale en chirurgie cardiaque? 2) Les résultats sont-ils fondés sur une solide méthodologie des études?
Sources
MEDLINE, Internet et une recherche manuelle jusqu’en février 2004 pour les articles en anglais et en français sur la SPIR. Constatations principales: Nous avons revu 48 articles, pour un total de 5931 interventions en cardiochirurgie avec monitorage par la SPIR. Plus de 83 % des patients avaient eu un pontage aortocoronarien. La majorité des études avec monitorage étaient prospectives. Du point de vue clinique, le monitorage avec la SPIR permet de détecter les épisodes de désaturation cérébrale survenus pendant la chirurgie. Cependant, la majorité des études avaient d’importantes limites méthodologiques et un faible niveau de preuve. La validité de la SPIR vs l’oxymétrie du bulbe jugulaire est mise en question, ainsi que sa valeur prédictive à détecter les patients qui vont souffrir de déficits neurologiques postopératoires. Le seul essai randomisé et contrôlé avait des résultats négatifs à cet égard.
Conclusion
L’application clinique de la SPIR en cardiochirurgie comme moniteur cérébral semble intéressante. Cependant, la SPIR doit être étudiée plus rigoureusement si on veut prouver son utilité clinique en chirurgie cardiaque.
Article PDF
Similar content being viewed by others
References
Arrowsmith JE, Grocott HP, Reves JG, Newman MF. Central nervous system complications of cardiac surgery. Br J Anaesth 2000; 84: 378–93.
Roach GW, Kanchuger M, Mangano CM, et al. Adverse cerebral outcomes after coronary bypass surgery. N Engl J Med 1996; 335: 1857–63.
Newman MF, Kirchner JL, Phillips-Bute B, et al. Longitudinal assessment of neurocognitive function after coronary-artery bypass surgery. N Engl J Med 2001; 344: 395–402.
Ahlgren F, Aren C. Cerebral complications after coronary artery bypass and heart valve surgery: risk factors and onset of symptoms. J Cardiothorac Vasc Anesth 1998; 12: 270–3.
Gill R, Murkin JM. Neuropsychologic dysfunction after cardiac surgery: what is the problem? J Cardiothorac Vasc Anesth 1996; 10: 91–8.
Murkin JM. Etiology and incidence of brain dysfunction after cardiac surgery. J Cardiothorac Vasc Anesth 1999; 13(Suppl. 1): 12–7.
Edmonds HL Jr, Rodriguez RA, Audenaert SM, Austin EH III,Pollock SB Jr, Ganzel BL. The role of neuromonitoring in cardiovascular surgery. J Cardiothorac Vasc Anesth 1996; 10: 15–23.
Edmonds HL Jr, Singer I, Sehic A, Strickland TJ. Multimodality neuromonitoring for neurocardiology. J Interv Cardiol 1998; 11: 197–204.
Edmonds HL Jr. Detection and treatment of cerebral hypoxia key to avoiding intraoperative brain injuries. Anesthesia Patient Safety Foundation 1999; 14: 25–32.
Edmonds HL Jr. Advances in neuromonitoring for cardiothoracic and vascular surgery. J Cardiothorac Vasc Anesth 2001; 15: 241–50.
Dujovny M, Misra M, Widman R. Cerebral oximetry-Techniques. Neurol Res 1998; 20(Suppl. 1): S5–12.
Madsen PL, Secher NH. Near-infrared oximetry of the brain. Prog Neurobiol 1999; 58: 541–60.
Wahr JA, Tremper KK, Samra S, Delpy DT. Nearinfrared spectroscopy: theory and applications. J Cardiothorac Vasc Anesth 1996; 10: 406–18.
Cruz J. The first decade of continuous monitoring of jugular bulb oxyhemoglobin saturation: management strategies and clinical outcome. Crit Care Med 1998; 26: 344–51.
Hans P, Damas F. Evaluation of cerebral metabolism (French). Ann Fr Anesth Reanim 1999; 18: 599–603.
Mayberg TS, Lam AM. Jugular bulb oximetry for the monitoring of cerebral blood flow and metabolism. Neurosurg Clin N Am 1996; 7: 755–65.
Schell RM, Cole DJ. Cerebral monitoring: jugular venous oximetry. Anesth Analg 2000; 90: 559–66.
Shaaban Ali M, Harmer M, Latto IP. Jugular bulb oximetry during cardiac surgery. Anaesthesia 2001; 56: 24–37.
Simonson SG, Piantadosi CA. Monitoring cardiac function and tissue perfusion. Near-infrared spectrascopy. Crit Care Clin 1996; 12: 1–17.
Owen-Reece H, Smith M, Elwell CE, Goldstone JC Near infrared spectroscopy. Br J Anaesth 1999; 82: 418–26.
Sackett DL. Rules of evidence and clinical recommendations on the use of antithrombotic agents. Chest 1989; 95(Suppl.): 2S-4S.
Webster GK, Sibbald WJ. Using evidence to teach. In: Core Health Services (Ed.). Fluid Management in the Acutely Ill. An Evidence-Based Education Program. Concord: Canada; 2001: 8–14.
Baris RR, Israel AL, Amory DW, Henni P. Regional cerebral oxygenation during cardiopulmonary bypass. Perfusion 1995; 10: 245–8.
Chen CS, Leu BK, Liu K. Detection of cerebral desaturation during cardiopulmonary bypass by cerebral oximetry. Acta Anaesthesiol Sin 1996; 34: 173–8.
Katoh T, Esato K, Gohra H, et al. Evaluation of brain oxygenation during selective cerebral perfusion by near-infrared spectroscopy. Ann Thorac Surg 1997; 64: 432–6.
Newman ME, Lowry E, Croughwell ND, White W, Kirchner J, Blumenthal J. Near-infrared spectroscopy (INVOS 3100A) and cognitive outcome after cardiac surgery. Anesth Analg 1997; 82(Suppl.): Ill (abstract).
Sapire KJ, Gopinath SP, Farhat G, et al. Cerebral oxygenation during warming after cardiopulmonary bypass. Crit Care Med 1997; 25: 1655–62.
Bhasker Rao B, VanHimbergen D, Edmonds HL Jr, et al. Evidence for improved cerebral function after minimally invasive bypass surgery. J Card Surg 1998; 13: 27–31.
Edmonds HL Jr, Sehic A, Pollock SB Jr, Ganzel BL. Low cerebrovenous oxygen saturation predicts disorientation. Anesthesiology 1998; 89: 941 (abstract).
Edmonds HL Jr, Thomas MH, Sehic A, Pollock SB Jr, Ganzel BL. Cerebral oxygen desaturation during myocardial revascularization is associated with frontal lobe injury. Anesth Analg 1998; 86: 13 (abstract).
Liu R, Sun D, Hang Y, Ishibe T. Evaluation of cerebral oxygen balance by cerebral oximeter and transcranial doppler during hypothermic cardiopulmonary bypass. Anesthesiology 1998; 89: 309 (abstract).
Nemoto EM, Mofrad P, Dyke CM. Cerebral oxygenation during cardiac surgery. J Neurosurg Anesthesiol 1998; 10: 283 (abstract).
Edmonds HL Jr, Thomas MH, Yu QJ, Pollock SB Jr. Cost of coronary artery bypass graft (CABG) surgery reduced by multimodality neuromonitoring. Anesth Analg 1999; 88: 26 (abstract).
Kadoi Y, Kawahara F, Saito S, et al. Effects of hypothermie and normothermic cardiopulmonary bypass on brain oxygenation. Ann Thorac Surg 1999; 68: 34–9.
Lassnigg A, Hiesmayr M, Keznickl P, Mullner T, Ehrlich M, Grubhofer G. Cerebral oxygenation during cardiopulmonary bypass measured by near-infrared spectroscopy: effects of hemodilution, temperature, and flow. J Cardiothorac Vasc Anesth 1999; 13: 544–8.
Razumovsky A, Varelas PN, Wijman CA, McBee N, Hanley DF, Baumgartner WA. Cerebral and systemic hemodynamic changes during and after CABG. Preliminary results. Ann Thorac Surg 1999; 68: 1459 (abstract).
Yao FS, Tseng CC, Boyd WC, Shukla K, Hartman GS. Cognitive dysfunction following cardiac surgery is associated with cerebral oxygen desaturation. Anesthesiology 1999; 91: 73 (abstract).
Yao FS, Tseng CC, Braverman JM, Levin SK, Illner P. Cerebral oxygen desaturation is associated with prolonged lengths of stay in the intensive care unit (ICU) and hospital. Anesthesiology 1999; 91: 123 (abstract).
Edmonds HL Jr, Thomas MH, Pollock SB Jr, Spence PA. Conventional coronary artery bypass graft (CABG) surgery vs. off-pump CABG (OP-CABG): impact of neuromonitoring. Anesthesiology 2000; 93: 296 (abstract).
Grubhofer G, Mares P, Rajek A, et al. Pulsatility does not change cerebral oxygenation during cardiopulmonary bypass. Acta Anaesthesiol Scand 2000; 44: 586–91.
Novitzky D, Boswell BB. Total myocardial revascularization without cardiopulmonary bypass utilizing computer-processed monitoring to assess cerebral perfusion. Heart Surg Forum 2000; 3: 198–202.
Schmahl TM. Operative changes effecting incidence of perioperative stroke (IPS) using cerebral oximetry (CO) and aortic ultrasonography (AU). Anesthesiology 2000; (Suppl.): 399 (abstract).
Yao FS, Tseng CC, Trifiletti RR, et al. Neurologic complications following cardiac surgery is associated with cerebral oxygen desaturation. Anesth Analg 2000; 90: 76 (abstract).
Yao FS, Tseng CC, Trifiletti RR, Crockett S, Isom OW. Low preoperative cerebral oxygen saturation is associated with postoperative frontal lobe and cognitive dysfunction and prolonged ICU and hospital stays. Anesth Analg 2000; 90: 30 (abstract).
Alexander JC Jr, Kronenfeld MA, Dance GR. Reduced postoperative length of stay may result from using cerebral oximetry monitoring to guide treatment. Key West, FL. May 23–27, Outcomes 2001.
Fearn SJ, Pole R, Wesnes K, Faragher EB, Hooper TL, McCollum CN. Cerebral injury during cardiopulmonary bypass: emboli impair memory. J Thorac Cardiovasc Surg 2001; 121: 1150–60.
McKowen RL, Paxton TP, Bretz GE, Brown LT. Cerebral oxygenation monitoring during cardiac surgery at a community hospital. Ann Thorac Surg 2002; 73: S372 (abstract).
Shaaban Ali M, Harmer M, Vaughan RS, Dunne JA, Latto IP. Spatially resolved spectroscopy (NIRO-300) does not agree with jugular bulb oxygen saturation in patients undergoing warm bypass surgery. Can J Anesth 2001; 48: 497–501.
Yamashita K, Kazui T, Terada H, Washiyama N, Suzuki K, Basher AH. Cerebral oxygenation monitoring for total arch replacement using selective cerebral perfusion. Ann Thorac Surg 2001; 72: 503–8.
Yao FS, Tseng CC, Woo D, Huang SW, Levin SK. Maintaining cerebral oxygen saturation during cardiac surgery decreased neurological complications. Anesthesiology 2001; 95: 152 (abstract).
Yao FS, Levin SIC, Wu D, et al. Maintaining cerebral oxygen saturation during cardiac surgery shortened ICU and hospital stays. Anesth Analg 2001; 92: 86 (abstract).
Edmonds HL Jr. Multi-modality neurophysiologic monitoring for cardiac surgery. Heart Surg Forum 2002; 5: 225–8.
Edmonds HL Jr, Cao L, Yu QJ. In the elderly, coronary artery bypass grafting associated with more brain O2 desaturation and cognitive dysfunction. Ann Thorac Surg 2002; 73: 375 (abstract).
Edmonds HL Jr, Thomas MH, Ganzel BL, Pollock SB Jr, Etoch SW, Spence PA. Brain O2 desaturation despite preserved autoregulation during cardiopulmonary bypass. Ann Thorac Surg 2002; 73: 373 (abstract).
Ganzel BL, Cerrito PB, Edmonds HL Jr. Multimodality neuromonitoring improves CABG recovery. Fort Lauderdale, FL. Society of Thoracic Surgeons, 38th Annual Meeting; January 28–30, 2002.
Goldman S. Utilization of cerebral oximetric monitoring and optimized cerebral oximetry values decrease incidence of stroke for cardiac surgical patients. Miami Beach, FL. 40th Annual Meeting of the Pennsylvania Association of Thoracic Surgery; October 16–20, 2002.
Janelle GM, Mnookin S, Gravenstein N, Martin TD, Urdaneta F. Unilateral cerebral oxygen desaturation during emergent repair of a DeBakey type 1 aortic dissection: potential aversion of a major catastrophe. Anesthesiology 2002; 96: 1263–5.
Novitzky D, Bowen TE, Larson A, Powe J, Ebra G. Aiming towards complete myocardial revascularization without cardiopulmonary bypass: a systematic approach. Heart Surg Forum 2002; 5: 214–20.
Prabhune A, Sehic A, Spence PA, Church T, Edmonds HL Jr. Cerebral oximetry provides early warning of oxygen delivery failure during cardiopulmonary bypass. J Cardiothorac Vasc Anesth 2002; 16: 204–6.
Reents W, Muellges W, Franke D, Babin-Ebell J, Elert O. Cerebral oxygen saturation assessed by near-infrared spectroscopy during coronary artery bypass grafting and early postoperative cognitive function. Ann Thorac Surg 2002; 74: 109–14.
Takahashi K. Changes in cerebral blood flow velocity and regional cerebral oxygen saturation during coronary and valve surgery. Anesth Analg 2002; 94: 81 (abstract).
Yao FF, Ho CA, Huang SW, Tseng C Maintaining adequate cerebral oxygen saturation during cardiac surgery shortened intensive care unit stay in female gender. Anesth Analg 2002; 94: 83 (abstract).
Iglesias I, Murkin JM, Bainbridge D, Adams S. Monitoring cerebral oxygen saturation significantly decreases postoperative length of stay: a prospective randomized blinded study. Heart Surg Forum 2003; 6: 204.
Jalali S, Hesselvik F, Pierce ET, Crowley R, Shemin RJ. Routine cerebral oxygen monitoring fails to improve neurological outcome in cardiac surgery. Anesth Analg 2003; 96: 8 (abstract).
Laschinger J, Razumovsky AT, Stierer KA, Owen J. Cardiac surgery: value of neuromonitoring. Key West, FL. The Key West Meeting; May 21–24, Outcomes 2003.
Likosky DS, O’Connor GT, Saykin AJ, et al. A novel approach to identifying mechanisms of neurologic injury after cardiac surgery. Key West, FL. The Key West Meeting; May 21–24, Outcomes 2003.
Talpahewa SP, Ascione R, Angelini GD, Lovell AT. Cerebral cortical oxygenation changes during OPCAB surgery. Ann Thorac Surg 2003; 76: 1516–22.
Vijay V, McCusker K, Stasko A, et al. Cerebral oximetry directed permissive hypercapnia enhances cerebral perfusion during CPB for heart failure surgery. Key West, FL. The Key West Meeting; May 21–24, Outcomes 2003.
Vijay V, McCusker K, Stasko A, et al. Cerebral oxymetry based comparison of cerebral perfusion with standard versus condensed extra-corporeal circuits in adult cardiac surgery. Key West, FL. The Key West Meeting; May 21–24, Outcomes 2003.
Bilfinger TV, Rampil IJ. Invited commentary: Cerebral cortical oxygenation changes during OPCAB surgery. Ann Thorac Surg 2003; 76: 1522.
Nemoto EM, Yonas H, Kassam A. Clinical experience with cerebral oximetry in stroke and cardiac arrest. Crit Care Med 2000; 28: 1052–4.
Maeda H, Fukita K, Oritani S, Ishida K, Zhu BL. Evaluation of post-mortem oxymetry with reference to the causes of death. Forensic Sci Int 1997; 87: 201–10.
Moehle DA. Neuromonitoring in the cardiopulmonary bypass surgical patient: clinical applications. J Extra Corpor Technol 2001; 33: 126–34.
Kim MB, Ward DS, Cartwright CR, Kolano J, Chlebowski S, Henson LC. Estimation of jugular venous O2 saturation from cerebral oximetry or arterial O2 saturation during isocapnic hypoxia. J Clin Monit Comput 2000; 16: 191–9.
Edmonds HL Jr, Toney KA, Thomas MH, Pollock SB Jr, Strickland TJ. Neuromonitoring cost-benefit for adult cardiac surgery. Anesthesiology 1997; 87: 426 (abstract).
Author information
Authors and Affiliations
Corresponding author
Additional information
Funding sources: Montreal Heart Institute and Fonds de la recherche en santé du Québec
Conflict of interest: None.
Rights and permissions
About this article
Cite this article
Taillefer, M.C., Denault, A.Y. Cerebral near-infrared spectroscopy in adult heart surgery: systematic review of its clinical efficacy. Can J Anesth 52, 79–87 (2005). https://doi.org/10.1007/BF03018586
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03018586