Background and Purpose:
Routine posttreatment surveillance is recommended after adjuvant radiotherapy for stage I seminoma. However, systematic studies on the value of follow-up in these patients are missing. This report addresses the efficiency of routine follow-up in stage I seminoma with particular reference to the mode of detection of relapse and the costs of posttreatment screening.
Patients and Methods:
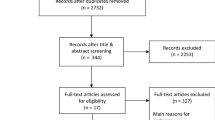
All follow-up investigations of a prospectively followed cohort of 675 patients with stage I seminoma treated with PA radiotherapy were analyzed with respect to the first indications of relapse, patterns of recurrence, risk factors of relapse, and cost-efficiency of the different technical examinations of the follow-up schedule over a 10-year period.
Results:
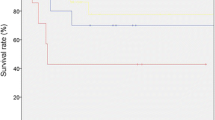
With a median time to follow-up of 61 months, recurrence was diagnosed by symptoms or physical examination in 14 out of 26 relapsing patients. Among the technical follow-up investigations abdominopelvic imaging had the highest detection rate for relapse, while thoracic imaging and marker analysis were inefficient. Abdominal sonography had the highest cost-efficiency of all technical follow-up investigations, while computed tomography (CT) scans were responsible for approximately 60% of all costs. The authors failed to identify risk factors predictive of relapse after adjuvant irradiation.
Conclusion:
Routine technical investigations during follow-up after PA radiotherapy for stage I seminoma yield only a low detection rate of relapse from cancer. The data presented here provide no evidence for the value of technical follow-up beyond the 3rd year after treatment or routine screening of the chest. Thorough physical examination of the patients should be encouraged. Patients should be informed about potential symptoms indicative of recurrence. Restrictive use of abdominopelvic CT scans will reduce exposure to ionizing radiation and considerably increase the cost-efficiency of follow-up.
Hintergrund und Ziel:
Nach adjuvanter Strahlentherapie von Seminompatienten im Stadium I wird eine Nachsorge empfohlen, systematische Studien für diese Empfehlungen fehlen jedoch. Ziel dieser Arbeit ist es, den Nutzen der Nachsorgeuntersuchungen in Bezug auf den Rezidivnachweis und die Kosten zu analysieren.
Patienten und Methodik:
Es wurde eine retrospektive Analyse einer 675 Patienten umfassenden Patientengruppe mit Seminom im Stadium I durchgeführt, die im Rahmen einer prospektiven Studie eine paraaortale Strahlentherapie erhalten hatten und systematisch nachbeobachtet worden waren. Folgende Aspekte wurden analysiert: Art des Rezidivnachweises (klinisch/symptomatisch oder durch technische Untersuchungen), Rezidivmuster (anatomisch und zeitlich), Risikofaktoren für das Auftreten eines Rezidivs, Kosten der Nachsorge.
Ergebnisse:
Nach einer medianen Nachbeobachtungszeit von 61 Monaten traten 26 Rezidive auf. Bei 14 Patienten ergab sich der erste Hinweis auf den Rückfall durch Symptome oder Befunde der körperlichen Untersuchung. Von den technischen Untersuchungen wies die abdominopelvine Bildgebung die höchste Nachweisrate von Rezidiven auf, während Thoraxbildgebung und Tumormarkerbestimmung eine geringe Nachweiswahrscheinlichkeit hatten. Die Abdomensonographie zeigte die beste Kosten-Nutzen- Relation, während die Computertomographie (CT) etwa 60% der Kosten des Nachsorgeprogramms verursachte. Risikofaktoren für das Auftreten eines Rezidivs konnten nicht nachgewiesen werden.
Schlussfolgerung:
Diese Ergebnisse weisen darauf hin, dass der Routineeinsatz technischer Untersuchungen eine geringe Detektionsrate von Rezidiven nach paraaortaler Strahlentherapie im Stadium I des Seminoms hat und nach dem 3. Jahr nicht mehr erfolgen sollte. Ein restriktiver Einsatz der CT kann die Kosten-Nutzen-Relation der Nachsorge deutlich verbessern.
Similar content being viewed by others
References
Albers P, Albrecht W, Algaba F, et al. Guidelines on testicular cancer. Eur Urol 2005;48:885–94.
Aparicio J, Germà JR, del Muro XG, et al. Risk-adapted management for patients with clinical stage I seminoma: the second Spanish Germ Cell Cancer Cooperative Group study. J Clin Oncol 2005;23:8717–23.
Bamberg M, Schmidberger H, Meisner C, et al. Radiotherapy for stage I, IIA/B testicular seminoma. Int J Cancer 1999;83:823–7.
Bölling T, Könemann S, Ernst I, et al. Late effects of thoracic irradiation in children. Strahlenther Onkol 2008;184:289–95.
Bruns F, Raub M, Schäfer U, et al. No predictive value of beta-HCG in patients with stage I seminoma - results of a long-term follow-up study after adjuvant radiotherapy. Anticancer Res 2005;25:1543–6.
Buchholz TA, Walden TL, Prestidge BR. Cost-effectiveness of posttreatment surveillance after radiation therapy for early stage seminoma. Cancer 1998;82:1126–33.
Classen J, Bamberg M. Gonadal toxicity and fertility after radiotherapy for testicular seminoma. Onkologie 1999;22:66–8.
Classen J, Schmidberger H, Meisner C, et al. Para-aortic irradiation for stage I testicular seminoma: results of a prospective study in 675 patients. A trial of the German Testicular Cancer Study Group (GTCSG). Br J Cancer 2004;90:2305–11.
Fossa SD, Horwich A, Russel JM, et al. Optimal planning target volume for stage I testicular seminoma: a Medical Research Council randomized trial. J Clin Oncol 1999;17:1146–54.
Jacobsen KD, Olsen DR, Fossa K, et al. External beam abdominal radiotherapy in patients with seminoma stage I: field type, testicular dose, and spermatogenesis. Int J Radiat Oncol Biol Phys 1997;38:95–102.
Jones WG, Fossa SD, Mead GM, et al. Randomized trial of 30 versus 20 Gy in the adjuvant treatment of stage I testicular seminoma: a report on Medical Research Council trial TE18, European Organization for the Research and Treatment of Cancer Trial 30942 (ISRCTN18525328). J Clin Oncol 2005;23:1200–8.
Kiricuta IO, Sauer J, Bohndorf W. Omission of the pelvic irradiation in stage I testicular seminoma: a study of postorchiectomy paraaortic radiotherapy. Int J Radiat Oncol Biol Phys 1996;35:293–8.
Krege S, Beyer J, Souchon S, et al. European consensus conference on diagnosis and treatment of germ cell cancer: a report of the Second Meeting of the European Germ Cell Cancer Consensus Group (EGCCCG): part I. Eur Urol 2008;53:478–96.
Livsey JE, Taylor B, Mobarek N, et al. Patterns of relapse following radiotherapy for stage I seminoma of the testis: implications for follow-up. Clin Oncol 2001;13:296–300.
Logue JP, Harris MA, Livsey JE, et al. Short course para-aortic radiation for stage I seminoma of the testis. Int J Radiat Oncol Biol Phys 2003;57:1304–9.
Ludwig V, Schwab F, Guckenberger M, et al. Comparison of wedge versus segmented techniques in whole breast irradiation. Effects on dose exposure outside the treatment volume. Strahlenther Onkol 2008;184:307–12.
Mazonakis M, Zacharopoulou F, Kachris S, et al. Scattered dose to gonads and associated risks from radiotherapy for common pediatric malignancies. A phantom study. Strahlenther Onkol 2007;183:332–7.
Müller AC, Ganswindt U, Bamberg M, et al. Risk of second malignancies after prostate irradiation? Strahlenther Onkol 2007;183:605–9.
Nathan PD, Rustin GR. The role of CT scanning in the surveillance of testicular tumours. Clin Oncol (R Coll Radiol) 2003;15:121–2.
Sharda NN, Kinsella TJ, Ritter MA. Adjuvant radiation versus observation: a cost analysis of alternate management schemes in early-stage testicular seminoma. J Clin Oncol 1996;14:2933–9.
Spermon JR, Witjes JA, Kiemeney LALM. Efficacy of routine follow-up after first-line treatment for testicular cancer. World J Urol 2004;22:235–43.
Sultanem K, Souhami L, Benk V, et al. Para-aortic irradiation only appears to be adequate treatment for patients with stage I seminoma of the testis. Int J Radiat Oncol Biol Phys 1998;40:455–9.
Travis LB, Curtis RE, Storm H, et al. Risk of second malignant neoplasms among long-term survivors of testicular cancer. J Natl Cancer Inst 1997;89:1429–39.
Travis LB, Fossa SD, Schonfeld SJ, et al. Second cancers among 40,576 testicular cancer patients: focus on long-term survivors. J Natl Cancer Inst 2005;97:1354–65.
Trigo MJ, Tabernero JM, Paz-Ares L, et al. Tumor markers at the time of recurrence in patients with germ cell tumors. Cancer 2000;88:162–8.
Warde P, Specht L, Horwich A, et al. Prognostic factors for relapse in stage I seminoma managed by surveillance: a pooled analysis. J Clin Oncol 2002;20:4448–52.
Weissbach L, Bussar-Maatz R, Löhrs U, et al. Prognostic factors in seminomas with special respect to HCG: results of a prospective multicenter study. Seminoma Study Group. Eur Urol 1999;36:601–8.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Claßen, J., Schmidberger, H., Souchon, R. et al. What is the value of routine follow-up in stage I seminoma after paraaortic radiotherapy?. Strahlenther Onkol 185, 349–354 (2009). https://doi.org/10.1007/s00066-009-1958-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-009-1958-z