Summary
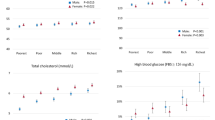
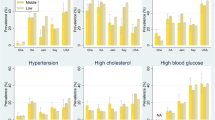
This report describes the social distribution of central obesity and the metabolic syndrome at the Whitehall II study phase 3 examination, and assesses the contribution of health related behaviours to their distribution. Cross-sectional analyses were conducted utilising data collected in 1991–1993 from 4978 men and 2035 women aged 39–63 years who completed an oral glucose tolerance test. There was an inverse social gradient in prevalence of the metabolic syndrome. The odds ratio (95 % confidence interval) for having the metabolic syndrome comparing lowest with highest employment grade was: men 2.2 (1.6–2.9), women 2.8 (1.6–4.8). Odds ratios for occupying the top quintile of the following variables, comparing lowest with highest grade, were, for waist-hip ratio: men 2.2 (1.8-2.8), women 1.6 (1.1-2.4); post-load glucose: men 1.4 (1.1-1.8), women 1.8 (1.2-2.6); triglycerides: men 1.6 (1.2-2.0), women 2.2 (1.5-3.3); fibrinogen: men 1.7 (1.4-2.3), women 1.9 (1.2-2.8). Current smoking status, alcohol consumption and exercise level made a small contribution (men 11%, women 9%) to the inverse association between socioeconomic status and metabolic syndrome prevalence. In conclusion, central obesity, components of the metabolic syndrome and plasma fibrinogen are strongly and inversely associated with socioeconomic status. Our findings suggest the metabolic syndrome may contribute to the biological explanation of social inequalities in coronary risk. Health related behaviours appear to account for little of the social patterning of metabolic syndrome prevalence.
Article PDF
Similar content being viewed by others
Abbreviations
- vWF:
-
von Willebrand factor
References
Marmot MG, Rose G, Shipley M, Hamilton PJS (1978) Employment grade and coronary heart disease in British civil servants. J Epidemiol Community Health 32: 244–249
Blane D, Brunner EJ, Wilkinson RG (1996) Health and social organization. Routledge, London
Marmot MG, Davey Smith G, Stansfeld S, et al. (1991) Health inequalities among British Civil Servants: the Whitehall II study. Lancet 337: 1387–1393
Davey Smith G, Neaton JD, Wentworth D, Stamler R, Stamler J (1996) Socioeconomic differentials in mortality risk among men screened for the Multiple Risk Factor Intervention Trial; I. white men. Am J Public Health 86: 486–496
Wilkinson RG (1995) “Variations” in health – The costs of government timidity. BMJ 311: 1177–1178
Brunner E (1997) Stress and the biology of inequality. BMJ 314:1472–1476
Davey Smith G, Shipley MJ, Rose G (1990) Magnitude and causes of socioeconomic differentials in mortality: further evidence from the Whitehall Study. J Epidemiol Community Health 44: 265–270
Hein HO, Suadicani P, Gyntelberg F (1992) Ischaemic heart disease incidence by social class and form of smoking: the Copenhagen male study — 17 years’ follow-up. J Int Med 231: 477–483
Gregory J, Foster K, Tyler H, Wiseman M (1990) The Diet and Nutrition Survey of British adults. HMSO, London
OPCS (1995) Health Survey for England, 1993. HMSO, London
Stamler R, Shipley M, Elliott P, Dyer A, Sans S, Stamler J (1992) Higher blood pressure in adults with less education. Some explanations from INTERSALT. Hypertension 19: 237–241
Brunner EJ, Davey Smith G, Marmot M, Canner R, Beksinska M, O’Brien J (1996) Childhood social circumstances and psychosocial and behavioural factors as determinants of plasma fibrinogen. Lancet 347: 1008–1013
Larsson B, Svardsudd K, Welin L, Wilhelmsen L, Bjorntorp P, Tibblin G (1984) Abdominal adipose tissue distribution, obesity, and risk of cardiovascular disease and death: 13 year follow up of participants in the study of men born in 1913. BMJ 288: 1401–1404
Lapidus L, Bengtsson C, Larsson B, Pennert K, Rybo E, Sjostrom L (1984) Distribution of adipose tissue and risk of cardiovascular disease and death: a 12 year follow up of participants in the population study of women in Gothenburg, Sweden. BMJ 289:1257–1261
Welin L, Svardsudd K, Wilhelmsen L, Larsson B, Tibblin G (1987) Analysis of risk factors for stroke in a cohort of men born in 1913. N Engl J Med 317: 521–526
Folsom AR, Kaye SA, Sellers TA, et al. (1993) Body fat distribution and 5-year risk of death in older women. JAMA 269: 483–487
Ohlson LO, Larsson B, Svardsudd K, et al. (1985) The influence of body fat distribution on the incidence of diabetes mellitus. 13.5 years of follow-up of the participants in the study of men born in 1913. Diabetes 34: 1055–1058
McKeigue PM, Shah B, Marmot MG (1991) Relation of central obesity and insulin resistance with high diabetes prevalence and cardiovascular risk in South Asians. Lancet 337: 382–386
Kissebah AH, Vydelingum N, Murray R, et al. (1982) Relation of body fat distribution to metabolic complications of obesity. J Clin Endocrinol Metab 54: 254–260
Reaven GM (1993) Role of insulin resistance in human disease (syndrome X): an expanded definition. Ann Rev Med 44: 121–131
Juhan-Vague I, Thompson SJ, Jespersen J (1993) Involvement of the hemostatic system in the insulin resistance syndrome. Art Thromb 13: 1865–1873
Brunner EJ, Marmot MG, White IR, et al. (1993) Gender and employment grade differences in blood cholesterol, apolipoproteins and haemostatic factors in the Whitehall II study. Atherosclerosis 102: 195–207
Marmot MG, Adelstein AM, Bulusu L (1981) Cardiovascular mortality among immigrants to England and Wales. Postgraduate Medical Journal 57: 760–762
Beksinska M, Yea L, Brunner EJ (1995) Whitehall II study manual for screening examination 1991-93. DEPH, London
Friedewald WT, Levy RI, Fredrickson DS (1972) Estimation of the concentration of low-density lipoprotein cholesterol in plasma, without use of the preparative ultracentrifuge. Clin Chem 18: 499–502
WHO Study Group (1985) Diabetes mellitus: Report of a WHO Study Group. World Health Organization, Geneva
Laakso M (1993) How good a marker is insulin level for insulin resistance? Am J Epidemiol 137: 959–965
Davidson J, Woodbury MA, Pelton S, Krishnan R (1988) A study of depressive typologies using grade of membership analysis. Psychol Med 18: 179–189
Vague J (1956) The degree of masculine differentiation of obesities: a factor determining predisposition to diabetes, atherosclerosis, gout, and uric calculous disease. Am J Clin Nutr 4: 20–34
Folsom AR, Burke GL, Ballew C, Jacobs DR, Haskell WL, Donahue RP (1989) Relation of body fatness and its distribution to cardiovascular risk factors in young blacks and whites. Am J Epidemiol 130: 911–924
Seidell JC, Bjorntorp P, Sjostrom L, Kvist H, Sannerstedt R (1990) Visceral fat accumulation in men is positively associated with insulin, glucose, and C-peptide levels, but negatively with testosterone levels. Metabolism 39: 897–901
Marmot MG, Shipley MJ, Rose G (1984) Inequalities in death — specific explanations of a general pattern. Lancet i:1003–1006
Fox J (ed) (1989) Health inequalities in European coutries. Gower Publishing Co Ltd, Aldershot
Kaplan GA, Keil JE (1993) Socioeconomic factors and cardiovascular disease: a review of the literature. Circulation 88: 1973–1998
Heiss G, Haskell W, Mowery R, Criqui MH, Brockway M, Tyroler HA (1980) Plasma high-density lipoprotein cholesterol and socioeconomic status. Circulation 62 (Suppl IV): 108–115
Larsson B, Bengtsson C, Bjorntorp P, et al. (1992) Is abdominal body fat distribution a major explanation for the sex difference in the incidence of myocardial infarction? Am J Epidemiol 135: 266–273
Eames M, Ben-Shlomo Y, Marmot MG (1993) Social deprivation and premature mortality: regional comparison across England. BMJ 307: 1097–1102
Marmot MG (1986) Social inequalities in mortality: the social environment. In: Wilkinson RG (ed) Class and health. Tavistock Publications, London, pp 21–34
Egolf B, Lasker J, Wolf S, Potvin L (1992) The Roseto effect: a 50-year comparison of mortality rates. Am J Public Health 82: 1089–1092
Bjorntorp P (1991) Visceral fat accumulation: the missing link between psychosocial factors and cardiovascular disease? J Int Med 230: 195–201
Ullah P (1990) The association between income, financial strain and psychological well-being among unemployed youths. J Occup Psychol 63: 317–330
Gallie D, Vogler C (1994) Labour market deprivation, welfare, and collectivism. In: Gallie D, Marsh C, Vogler C (eds) Social change and the experience of unemployment. Oxford University Press, Oxford, pp 299–317
Kopp MS, Skrabski A, Szedmak S (1995) Socioeconomic factors, severity of depressive symptomatology, and sickness absence rate in the Hungarian population. J Psychosom Res 39: 1019–1029
Brown GW (1986) Social support, self esteem and depression. Psychol Med 16: 813–831
Williams RB (1990) The role of the brain in physical disease. Folklore, normal science, or paradigm shift? JAMA 263: 1971–1972
Cook WW, Medley DM (1954) Proposed hostility and pharisaic- virtue scales for the MMPI. J Appl Psychol 38: 414–418
Kaye SA, Folsom AR, Jacobs DR, Hughes GH, Flack JM (1993) Psychosocial correlates of body fat distribution in black and white young adults. Int J Obes 17: 271–277
Sapolsky RM, Mott GE (1987) Social subordinance in wild baboons is associated with suppressed high density lipoprotein-cholesterol concentrations: the possible role of chronic social stress. Endocrinology 121: 1605–1610
Johnston DG, Alberti KGMM, Nattrass M, Barnes AJ, Bloom SR, Joplin GF (1980) Hormonal and metabolic rhythms in Cushing’s syndrome. Metabolism 29: 1047–1051
Eaker ED, Pinsky J, Castelli WP (1992) Myocardial infarction and coronary death among women: psychosocial predictors from a 20 year follow-up of women in the Framingham study. Am J Epidemiol 135: 854–864
Bartley M, Power C, Blane D, Davey Smith G, Shipley M (1994) Birth weight and later socioeconomic disadvantage: evidence from the 1958 British cohort study. BMJ 309: 1475–1479
Hales CN, Barker DJP (1992) Type 2 (non-insulin-dependent) diabetes mellitus: the thrifty phenotype hypothesis. Diabetologia 35: 595–601
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Brunner, E.J., Marmot, M.G., Nanchahal, K. et al. Social inequality in coronary risk: Central obesity and the metabolic syndrome. Evidence from the Whitehall II study. Diabetologia 40, 1341–1349 (1997). https://doi.org/10.1007/s001250050830
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s001250050830