Abstract
Objective
To determine the prevalence of post traumatic stress disorder in survivors of intensive care treatment.
Design
Systematic literature review including Medline, Embase, CINAHL, PsycINFO and references from identified papers.
Study selection
Studies determining the prevalence of PTSD in adult patients who had at least 24 h treatment on an intensive care unit. Independent duplicate data extraction. Study quality was evaluated in terms of study design and method and timing of PTSD assessment.
Data synthesis and results
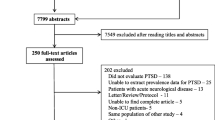
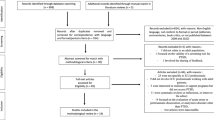
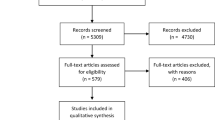
Of the 1472 citations identified, 30 studies meeting the selection criteria were reviewed. PTSD was diagnosed by standardised clinical interview alone in 2 studies. A self-report measure alone was used in 19 studies to measure PTSD symptomatology. The remaining 9 studies applied both standardised clinical interview and a self-report measure. The reported prevalence of PTSD was 0–64% when diagnosed by standardised clinical interview and 5–64% by self-report measure. PTSD assessments occurred 7 days to 8 years after intensive care discharge.
Conclusion
The true prevalence of PTSD and the optimum timing and method of PTSD assessment have not yet been determined in intensive care unit survivors. Deficiencies in design, methodology and reporting make interpretation and comparison of quoted prevalence rates difficult, and rigorous longitudinal studies are needed.

Similar content being viewed by others
References
Broomhead LR, Brett SJ (2002) Clinical review: Intensive care follow-up – what has it told us? Crit Care 6:411–417
Kapfhammer HP, Rothenhausler HB, Krauseneck T, Stoll C, Schelling G (2004) Posttraumatic stress disorder and health-related quality of life in long-term survivors of acute respiratory distress syndrome. Am J Psychiatry 161:45–52
Jones C, Griffiths RD, Humphris G, Skirrow PM (2001) Memory, delusions, and the development of acute posttraumatic stress disorder-related symptoms after intensive care. Crit Care Med 29:573–580
Cuthbertson BH, Hull A, Strachan M, Scott J (2004) Post-traumatic stress disorder after critical illness requiring general intensive care. Intensive Care Med 30:450–455
American Psychiatric Association (2000) Diagnostic and statistical manual of mental disorders, 4th edn, text revision. American Psychiatric Association, Arlington, VA
Spitzer RL, Williams JB, Gibbon M, First MB (1992) The Structured Clinical Interview for DSM-III-R (SCID). I. History, rationale, and description. Arch Gen Psychiatry 49:624–629
Blake DD, Weathers FW, Nagy LM, Kaloupek DG, Gusman FD, Charney DS, Keane TM (1995) The development of a clinician-administered PTSD scale. J Trauma Stress 8:75–90
Davidson JR, Book SW, Colket JT, Tupler LA, Roth S, David D, Hertzberg M, Mellman T, Beckham JC, Smith RD, Davison RM, Katz R, Feldman ME (1997) Assessment of a new self-rating scale for post-traumatic stress disorder. Psychol Med 27:153–160
Horowitz M, Wilner W, Alvarez W (1979) Impact of Event Scale: A measure of subjective stress. Psychosomat Med 41:209–218
Weiss DS, Marmar CR (1997) The Impact of Event Scale – revised. In: Wilson JP, Keane TM (eds) Assessing psychological trauma and PTSD. Guilford, New York, pp 399–411
Stoll C, Kapfhammer HP, Rothenhausler HB, Haller M, Briegel J, Schmidt M, Krauseneck T, Durst K, Schelling G (1999) Sensitivity and specificity of a screening test to document traumatic experiences and to diagnose post-traumatic stress disorder in ARDS patients after intensive care treatment. Intensive Care Med 25:697–704
Harris RP, Helfand M, Woolf SH, Lohr KN, Mulrow CD, Teutsch SM, Atkins D (2001) Current methods of the US Preventive Services Task Force: a review of the process. Am J Prev Med 20:21–35
Dowdy DW, Eid MP, Sedrakyan A, Mendez-Tellez PA, Pronovost PJ, Herridge MS, Needham DM (2005) Quality of life in adult survivors of critical illness: a systematic review of the literature. Intensive Care Med 31:611–620
Capuzzo M, Valpondi V, Cingolani E, Gianstefani G, De Luca S, Grassi L, Alvisi R (2005) Post-traumatic stress disorder-related symptoms after intensive care. Minerva Anestesiol 71:167–179
Mahler C, Boer K, Unlu C, Vroom M, Lamme B, Gouma D, de Borgie C, Boermeester M (2005) Prevalence of symptoms related to post-traumatic stress disorder during long-term follow-up in patients after surgical treatment for secondary peritonitis. Crit Care 9:243
Schelling G, Stoll C, Kapfhammer HP, Rothenhausler HB, Krauseneck T, Durst K, Haller M, Briegel J (1999) The effect of stress doses of hydrocortisone during septic shock on posttraumatic stress disorder and health-related quality of life in survivors. Crit Care Med 27:2678–2683
Schelling G, Stoll C, Haller M, Briegel J, Manert W, Hummel T, Lenhart A, Heyduck M, Polasek J, Meier M, Preuss U, Bullinger M, Schuffel W, Peter K (1998) Health-related quality of life and posttraumatic stress disorder in survivors of the acute respiratory distress syndrome. Crit Care Med 26:651–659
Schelling G, Kilger E, Roozendaal B, de Quervain DJ, Briegel J, Dagge A, Rothenhausler HB, Krauseneck T, Nollert G, Kapfhammer HP (2004) Stress doses of hydrocortisone, traumatic memories, and symptoms of posttraumatic stress disorder in patients after cardiac surgery: a randomized study. Biol Psychiatry 55:627–633
Stoll C, Schelling G, Goetz AE, Kilger E, Bayer A, Kapfhammer HP, Rothenhausler HB, Kreuzer E, Reichart B, Peter K (2000) Health-related quality of life and post-traumatic stress disorder in patients after cardiac surgery and intensive care treatment. J Thorac Cardiovasc Surg 120:505–512
Weis F, Kilger E, Roozendaal B, de Quervain DJ, Lamm P, Schmidt M, Schmolz M, Briegel J, Schelling G (2006) Stress doses of hydrocortisone reduce chronic stress symptoms and improve health-related quality of life in high-risk patients after cardiac surgery: a randomized study. J Thorac Cardiovasc Surg 131:277–282
Schelling G, Richter M, Roozendaal B, Rothenhausler HB, Krauseneck T, Stoll C, Nollert G, Schmidt M, Kapfhammer HP (2003) Exposure to high stress in the intensive care unit may have negative effects on health-related quality-of-life outcomes after cardiac surgery. Crit Care Med 31:1971–1980
Schelling G, Briegel J, Roozendaal B, Stoll C, Rothenhausler HB, Kapfhammer HP (2001) The effect of stress doses of hydrocortisone during septic shock on posttraumatic stress disorder in survivors. Biol Psychiatry 50:978–985
Rothenhausler HB, Grieser B, Nollert G, Reichart B, Schelling G, Kapfhammer HP (2005) Psychiatric and psychosocial outcome of cardiac surgery with cardiopulmonary bypass: a prospective 12-month follow-up study. Gen Hosp Psychiatry 27:18–28
Shaw RJ, Harvey JE, Nelson KL, Gunary R, Kruk H, Steiner H (2001) Linguistic analysis to assess medically related posttraumatic stress symptoms. Psychosomatics 42:35–40
Nickel M, Leiberich P, Nickel C, Tritt K, Mitterlehner F, Rother W, Loew T (2004) The occurrence of posttraumatic stress disorder in patients following intensive care treatment: a cross-sectional study in a random sample. J Intensive Care Med 19:285–290
Wehler M, Stolle M, Riek A, Loew T, Reulbach U, Hahn E, Strauss R (2004) Post-traumatic stress disorder after medical intensive care. Crit Care 8:343
Richter JC, Waydhas C, Pajonk FG (2006) Incidence of posttraumatic stress disorder after prolonged surgical intensive care unit treatment. Psychosomatics 47:223–230
Schnyder U, Morgeli H, Nigg C, Klaghofer R, Renner N, Trentz O, Buddeberg C (2000) Early psychological reactions to life-threatening injuries. Crit Care Med 28:86–92
Schnyder U, Moergeli H, Klaghofer R, Buddeberg C (2001) Incidence and prediction of posttraumatic stress disorder symptoms in severely injured accident victims. Am J Psychiatry 158:594–599
Badia-Castello M, Trujillano-Cabello J, Servia-Goixart L, March-Llanes J, Rodriguez-Pozo A (2006) Recall and memory after intensive care unit stay. Development of posttraumatic stress disorder. Med Clin (Barc) 126:561–566
Hepp U, Moergeli H, Buchi S, Wittmann L, Schnyder U (2005) Coping with serious accidental injury: a one-year follow-up study. Psychother Psychosom 74:379–386
Griffiths J, Gager M, Alder N, Fawcett D, Waldmann C, Quinlan J (2006) A self-report-based study of the incidence and associations of sexual dysfunction in survivors of intensive care treatment. Intensive Care Med 32:445–451
Scragg P, Jones A, Fauvel N (2001) Psychological problems following ICU treatment. Anaesthesia 56:9–14
Jones C, Skirrow P, Griffiths RD, Humphris GH, Ingleby S, Eddleston J, Waldmann C, Gager M (2003) Rehabilitation after critical illness: a randomized, controlled trial. Crit Care Med 31:2456–2461
Perrins J, King N, Collings J (1998) Assessment of long-term psychological well-being following intensive care. Intensive Crit Care Nursing 14:108–116
Rattray JE, Johnston M, Wildsmith JA (2005) Predictors of emotional outcomes of intensive care. Anaesthesia 60:1085–1092
Kress JP, Gehlbach B, Lacy M, Pliskin N, Pohlman AS, Hall JB (2003) The long-term psychological effects of daily sedative interruption on critically ill patients. Am J Respir Crit Care 168:1457–1461
Liberzon I, Abelson JL, Amdur RL, King AP, Cardneau JD, Henke P, Graham LM (2006) Increased psychiatric morbidity after abdominal aortic surgery: risk factors for stress-related disorders. J Vasc Surg 43:929–934
Nelson BJ, Weinert CR, Bury CL, Marinelli WA, Gross CR (2000) Intensive care unit drug use and subsequent quality of life in acute lung injury patients. Crit Care Med 28:3626–3630
Ridley S, Burchett K, Gunning K, Burns A, Kong A, Wright M, Hunt P, Ross S (1997) Heterogeneity in intensive care units: fact or fiction? Anaesthesia 52:531–537
Sirio CA, Tajimi K, Taenaka N, Ujike Y, Okamoto K, Katsuya H (2002) A cross-cultural comparison of critical care delivery: Japan and the United States. Chest 121:539–548
Angus DC, Sirio CA, Clermont G, Bion J (1997) International comparisons of critical care outcome and resource consumption. Crit Care Clin 13:389–407
Galea S, Nandi A, Vlahov D (2005) The epidemiology of post-traumatic stress disorder after disasters. Epidemiol Rev 27:78–91
Fazel M, Wheeler J, Danesh J (2005) Prevalence of serious mental disorder in 7000 refugees resettled in western countries: a systematic review. Lancet 365:1309–1314
Kangas M, Henry JL, Bryant RA (2002) Posttraumatic stress disorder following cancer. A conceptual and empirical review. Clin Psychol Rev 22:499–524
Spindler H, Pedersen SS (2005) Posttraumatic stress disorder in the wake of heart disease: prevalence, risk factors, and future research directions. Psychosom Med 67:715–723
Stoddard FJ, Todres ID (2001) A new frontier: posttraumatic stress and its prevention, diagnosis, and treatment. Crit Care Med 29:687–688
Schelling G, Roozendaal B, De Quervain DJ (2004) Can posttraumatic stress disorder be prevented with glucocorticoids? Ann N Y Acad Sci 1032:158–166
Czarnocka J, Slade P (2000) Prevalence and predictors of post-traumatic stress symptoms following childbirth. Br J Clin Psychol 39(1):35–51
Pedersen SS, Middel B, Larsen ML (2003) Posttraumatic stress disorder in first-time myocardial infarction patients. Heart Lung 32:300–307
Gil S, Caspi Y, Ben-Ari IZ, Koren D, Klein E (2005) Does memory of a traumatic event increase the risk for posttraumatic stress disorder in patients with traumatic brain injury? A prospective study. Am J Psychiatry 162:963–969
Jones C, Harvey AG, Brewin CR (2005) Traumatic brain injury, dissociation, and posttraumatic stress disorder in road traffic accident survivors. J Trauma Stress 18:181–191
Bombardier CH, Fann JR, Temkin N, Esselman PC, Pelzer E, Keough M, Dikmen S (2006) Posttraumatic stress disorder symptoms during the first six months after traumatic brain injury. J Neuropsychiatry Clin Neurosci 18:501–508
Bennun IS (2004) A critique of the research assessing post traumatic stress disorder in critical care patients. Care Crit Ill 20:102–106
Breslau N, Reboussin BA, Anthony JC, Storr CL (2005) The structure of posttraumatic stress disorder: latent class analysis in 2 community samples. Arch Gen Psychiatry 62:1343–1351
Joseph S (2005) Psychometric evaluation of Horowitz's impact of event scale: A review. J Trauma Stress 13:101–113
Author information
Authors and Affiliations
Corresponding author
Additional information
Contributors: J. G. and J. D. Y. initiated the project. J. G. and V. B. searched, extracted, and analysed the data. J. G., V. B. and G. F. cross-checked the extracted data. All authors participated in discussing the results and in writing the paper. J. G. is the guarantor for the paper.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Griffiths, J., Fortune, G., Barber, V. et al. The prevalence of post traumatic stress disorder in survivors of ICU treatment: a systematic review. Intensive Care Med 33, 1506–1518 (2007). https://doi.org/10.1007/s00134-007-0730-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-007-0730-z