Abstract
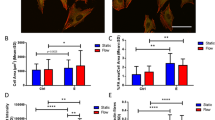
Mechanical loading is thought to provoke a cellular response via loading-induced flow of interstitial fluid through the lacuno-canalicular network of osteocytes. This response supposedly leads to an adaptation of local bone mass and architecture. It has been suggested that loss of estrogen during menopause alters the sensitivity of bone tissue to mechanical load, thereby contributing to the rapid loss of bone. The present study aimed to determine whether estrogen modulates the mechanoresponsiveness of bone cells from osteoporotic women. Bone cell cultures from nine osteoporotic women (aged 62–90 years) were pre-cultured for 24 h with 10−11 mol/l 17β-estradiol (E2) or vehicle, and subjected to 1 h of pulsating fluid flow (PFF) or static culture. E2 alone enhanced prostaglandin E2 (PGE2) and nitric oxide (NO) production by 2.8-fold and 2.0-fold, respectively, and stimulated endothelial nitric oxide synthase protein expression by 2.5-fold. PFF, in the absence of E2, stimulated PGE2 production by 3.1-fold and NO production by 3.9-fold. Combined treatment with E2 and PFF increased PGE2 and NO production in an additive manner. When expressed as PFF-treatment-over-control ratio, the response to fluid shear stress was similar in the absence or presence of E2. These results suggest that E2 does not affect the early response to stress in bone cells. Rather, E2 and shear stress both promote the production of paracrine factors such as NO and PGE2 in an additive manner.




Similar content being viewed by others
References
Parfitt AM (1976) The actions of parathyroid hormone on bone: relation to bone remodeling and turnover, calcium homeostasis, and metabolic bone diseases II. PTH and bone cells: bone turnover and plasma calcium regulation. Metabolism 25:909–955
Pondel M (2000) Calcitonin and calcitonin receptors: bone and beyond. Int J Exp Pathol 81:405–422
Lips P (2001) Vitamin D deficiency and secondary hyperparathyroidism in the elderly: consequences for bone loss and fractures and therapeutic implications. Endocr Rev 22:477–501
Rubin CT, Lanyon LE (1984) Regulation of bone formation by applied dynamic loads. J Bone Joint Surg Am 66:397–402
Mosley JR, Lanyon LE (1998) Strain rate as a controlling influence on adaptive modeling in response to dynamic loading of the ulna in growing male rats. Bone 23:313–318
Turner CH, Forwood MR, Otter MW (1994) Mechanotransduction in bone: do bone cells act as sensors of fluid flow? FASEB J 8:875–878
Piekarski K, Munro M (1977) Transport mechanism operating between blood supply and osteocytes in long bones. Nature 269:80–82
Cowin SC, Weinbaum S (1998) Strain amplification in the bone mechanosensory system. Am J Med Sci 316:184–188
Knothe Tate ML, Knothe U (2000) An ex vivo model to study transport processes and fluid flow in loaded bone. J Biomech 33:247–254
Luo G, Cowin SC, Sadegh AM, Arramon YP (1995) Implementation of strain rate as a bone remodeling stimulus. J Biomech Eng 117:329–338
Lanyon LE, Rubin CT (1984) Static versus dynamic loads as an influence on bone remodelling. J Biomech 17:897–905
Turner CH, Owan I, Takano Y (1995) Mechanotransduction in bone: role of strain rate. Am J Physiol 269:E438–E442
Klein-Nulend J, van der Plas A, Semeins CM, Ajubi NE, Frangos JA, Nijweide PJ, Burger EH (1995) Sensitivity of osteocytes to biomechanical stress in vitro. FASEB J 9:441–445
Bakker AD, Soejima K, Klein-Nulend J, Burger EH (2001) The production of nitric oxide and prostaglandin E2 by primary bone cells is shear stress dependent. J Biomech 34:671–677
Burger EH, Klein-Nulend J (1999) Mechanotransduction in bone—role of the lacunocanalicular network. FASEB J 13:S101–S112
Turner RT, Riggs BL, Spelsberg TC (1994) Skeletal effects of estrogen. Endocr Rev 15:275–300
Cheng S, Sipila S, Taaffe DR, Puolakka J, Suominen H (2002) Change in bone mass distribution induced by hormone replacement therapy and high-impact physical exercise in post-menopausal women. Bone 31:126–135
Kohrt WM, Snead DB, Slatopolsky E, Birge SJ Jr (1995) Additive effects of weight-bearing exercise and estrogen on bone mineral density in older women. J Bone Miner Res 10:1303–1311
Samuels A, Perry MJ, Tobias JH (1999) High-dose estrogen induces de novo medullary bone formation in female mice. J Bone Miner Res 14:178–186
Samuels A, Perry MJ, Gibson RL, Colley S, Tobias JH (2001) Role of endothelial nitric oxide synthase in estrogen-induced osteogenesis. Bone 29:24–29
Chow J, Tobias JH, Colston KW, Chambers TJ (1992) Estrogen maintains trabecular bone volume in rats not only by suppression of bone resorption but also by stimulation of bone formation. J Clin Invest 89:74–78
Frost HM (1987) The mechanostat: A proposed pathogenic mechanism of osteoporoses and the bone mass effects of mechanical and nonmechanical agents. Bone Miner 2:73–85
Cheng MZ, Zaman G, Rawlinson SC, Suswillo RF, Lanyon LE (1996) Mechanical loading and sex hormone interactions in organ cultures of rat ulna. J Bone Miner Res 11:502–511
Jagger CJ, Chow JW, Chambers TJ (1996) Estrogen suppresses activation but enhances formation phase of osteogenic response to mechanical stimulation in rat bone. J Clin Invest 98:2351–2357
Tromp AM, Bravenboer N, Tanck E, Kostense PJ, Lips P (2002) The effects of additional weight bearing during exercise and estrogen on bone mass and structure in female rats. Acta Bioeng Biomech 4 [Suppl 1]:399
Järvinen TLN, Kannus P, Pajamäki I, Vuohelainen T, Tuukkanen J, Järvinen M, Sievänen H (2003) Estrogen deposits extra mineral into bones of female rats in puberty, but simultaneously seems to suppress the responsiveness of female skeleton to mechanical loading. Bone 32:642–651
Forwood MR (1996) Inducible cyclo-oxygenase (COX-2) mediates the induction of bone formation by mechanical loading in vivo. J Bone Miner Res 11:1688–1693
Turner CH, Takano Y, Owan I, Murrell GA (1996) Nitric oxide inhibitor L-NAME suppresses mechanically induced bone formation in rats. Am J Physiol 270:E634–E639
Lowry OH (1955) Micromethods for the assay of enzyme. II Specific procedure. Alkaline phosphatase. Methods Enzymol 4:371
Klein-Nulend J, Semeins CM, Ajubi NE, Nijweide PJ, Burger EH (1995) Pulsating fluid flow increases nitric oxide (NO) synthesis by osteocytes but not periosteal fibroblasts: correlation with prostaglandin upregulation. Biochem Biophys Res Commun 217:640–648
Nijweide PJ, Van der Plas A, Scherft JP (1981) Biochemical and histological studies on various bone cell preparations. Calcif Tissue Int 33:529–540
Sterck JG, Klein-Nulend J, Lips P, Burger EH (1998) Response of normal and osteoporotic human bone cells to mechanical stress in vitro. Am J Physiol 274:E1113–E1120
Klein-Nulend J, Helfrich MH, Sterck JG, MacPherson H, Joldersma M, Ralston SH, Semeins CM, Burger EH (1998) Nitric oxide response to shear stress by human bone cell cultures is endothelial nitric oxide synthase dependent. Biochem Biophys Res Commun 250:108–114
Samuels A, Perry MJ, Tobias JH (1999) High-dose estrogen-induced osteogenesis in the mouse is partially suppressed by indomethacin. Bone 25:675–680
Armour KE, Ralston SH (1998) Estrogen upregulates endothelial constitutive nitric oxide synthase expression in human osteoblast-like cells. Endocrinology 139:799–802
Riancho JA, Zarrabeitia MT, Fernandez-Luna J, Gonzales-Macias J (1995) Mechanisms controlling nitric oxide synthesis in osteoblasts. Mol Cell Endocrinol 107:87–92
Chambliss KL, Shaul PW (2002) Estrogen modulation of endothelial nitric oxide synthase. Endocr Rev 23:665–686
Armour KE, Armour KJ, Gallagher ME, Godecke A, Helfrich MH, Ralston SH (2001) Defective bone formation and anabolic response to exogenous estrogen in mice with targeted disruption of endothelial nitric oxide synthase. Endocrinology 142:760–766
Stewart KG, Zhang Y, Davidge ST (1999) Estrogen decreases prostaglandin H synthase products from endothelial cells. J Soc Gynecol Investig 6:322–327
Joldersma M, Klein-Nulend J, Oleksik AM, Heyligers IC, Burger EH (2001) Estrogen enhances mechanical stress-induced prostaglandin production by bone cells from elderly women. Am J Physiol 280:E436–E442
Damien E, Price JS, Lanyon LE (1998) The estrogen receptor’s involvement in osteoblasts’ adaptive response to mechanical strain. J Bone Miner Res 13:1275–1282
Jessop HL, Sjoberg M, Cheng MZ, Zaman G, Wheeler-Jones CP, Lanyon LE (2001) Mechanical strain and estrogen activate estrogen receptor alpha in bone cells. J Bone Miner Res 16:1045–1055
Zaman G, Cheng MZ, Jessop HL, White R, Lanyon LE (2000) Mechanical strain activates estrogen response elements in bone cells. Bone 27:233–239
Cheng MZ, Rawlinson SCF, Pitsillides AA, Zaman G, Mohan S, Baylink DJ, Lanyon LE (2002) Human osteoblasts’ proliferative responses to strain and 17β-estradiol are mediated by the estrogen receptor and the receptor for insulin-like growth factor I. J Bone Miner Res 17:593–602
Jessop HL, Suswillo RFL, Rawlinson SCF, Zaman G, Lee K, Das-Gupta V, Pitsillides AA, Lanyon LE (2004) Osteoblast-like cells from estrogen receptor α knockout mice have deficient responses to mechanical strain. J Bone Miner Res 19:938–946
Lee K, Jessop HL, Suswillo RFL, Zaman G, Lanyon LE (2003) Bone adaptation requires estrogen receptor-α. Nature 424:389
Acknowledgments
The authors thank C.M. Semeins and H.F. Teshale for their expert technical assistance. We thank Drs P. Patka, A. van Kampen, E. Hoebink and T. Patt for their assistance in obtaining osteoporotic bone material, M.N. Helder for kindly providing PCR-primers for cbfa1, and M. Joldersma for providing the raw data of her study on osteoarthritic women. The Netherlands Organization for Scientific Research supported the work of A.D. Bakker (NWO Grant 903-41-193) who also received a financial contribution from the Stichting Anna Fonds. The European Community supported the work of J. Klein-Nulend (fifth framework grant QLK3-1999-00559).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bakker, A.D., Klein-Nulend, J., Tanck, E. et al. Additive effects of estrogen and mechanical stress on nitric oxide and prostaglandin E2 production by bone cells from osteoporotic donors. Osteoporos Int 16, 983–989 (2005). https://doi.org/10.1007/s00198-004-1785-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-004-1785-0