Abstract
Purpose
The unilateral 6-hydroxydopamine (6-OHDA) lesion rat model is a well-known acute model for Parkinson’s disease (PD). Its validity has been supported by invasive histology, behavioral studies and electrophysiology. Here, we have characterized this model in vivo by multitracer imaging [glucose metabolism and dopamine transporter (DAT)] in relation to behavioral and histological parameters.
Methods
Eighteen female adult Wistar rats (eight 6-OHDA-lesioned, ten controls) were investigated using multitracer [18F]-fluoro-2-deoxy-D-glucose (FDG) and [18F]-FECT {2′-[18F]-fluoroethyl-(1R-2-exo-3-exe)-8-methyl-3-(4-chlorophenyl)-8-azabicyclo(3.2.1)-octane-2-carboxylate} small animal positron emission tomography (PET). Relative glucose metabolism and parametric DAT binding images were anatomically standardized to Paxinos space and analyzed on a voxel-basis using SPM2, supplemented by a template-based predefined volumes-of-interest approach. Behavior was characterized by the limb-use asymmetry test; dopaminergic innervation was validated by in vitro tyrosine hydroxylase staining.
Results
In the 6-OHDA model, significant glucose hypometabolism is present in the ipsilateral sensory-motor cortex (−6.3%; p = 4 × 10−6). DAT binding was severely decreased in the ipsilateral caudate-putamen, nucleus accumbens and substantia nigra (all p < 5 × 10−9), as confirmed by the behavioral and histological outcomes. Correlation analysis revealed a positive relationship between the degree of DAT impairment and the change in glucose metabolism in the ipsilateral hippocampus (p = 3 × 10−5), while cerebellar glucose metabolism was inversely correlated to the level of DAT impairment (p < 3 × 10−4).
Conclusions
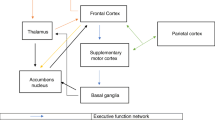
In vivo cerebral mapping of 6-OHDA-lesioned rats using [18F]-FDG and [18F]-FECT small animal PET shows molecular–functional correspondence to the cortico-subcortical network impairments observed in PD patients. This provides a further molecular validation supporting the validity of the 6-OHDA lesion model to mimic multiple aspects of human PD.





Similar content being viewed by others
References
Bove J, Prou D, Perier C, Przedborski S. Toxin-induced models of Parkinson’s disease. NeuroRx 2005;2:484–94.
Cohen G. Oxy-radical toxicity in catecholamine neurons. Neurotoxicology 1984;5:77–82.
Schwarting RK, Huston JP. Unilateral 6-hydroxydopamine lesions of meso-striatal dopamine neurons and their physiological sequelae. Prog Neurobiol 1996;49:215–66.
Schwarting RK, Huston JP. The unilateral 6-hydroxydopamine lesion model in behavioral brain research. Analysis of functional deficits, recovery and treatments. Prog Neurobiol 1996;50:275–331.
Inaji M, Okauchi T, Ando K, Maeda J, Nagai Y, Yoshizaki T, et al. Correlation between quantitative imaging and behavior in unilaterally 6-OHDA-lesioned rats. Brain Res 2005;1064:136–45.
Thobois S, Guillouet S, Broussolle E. Contributions of PET and SPECT to the understanding of the pathophysiology of Parkinson’s disease. Neurophysiol Clin 2001;31:321–40.
Ravina B, Eidelberg D, Ahlskog JE, Albin RL, Brooks DJ, Carbon M, et al. The role of radiotracer imaging in Parkinson disease. Neurology 2005;64:208–15.
Wienhard K. Measurement of glucose consumption using [(18)F]fluorodeoxyglucose. Methods 2002;27:218–25.
Kuhl DE, Metter EJ, Riege WH. Patterns of local cerebral glucose utilization determined in Parkinson’s disease by the [18F]fluorodeoxyglucose method. Ann Neurol 1984;15:419–24.
Lozza C, Baron JC, Eidelberg D, Mentis MJ, Carbon M, Marie RM. Executive processes in Parkinson’s disease: FDG-PET and network analysis. Hum Brain Mapp 2004;22:236–45.
Asanuma K, Tang C, Ma Y, Dhawan V, Mattis P, Edwards C, et al. Network modulation in the treatment of Parkinson’s disease. Brain 2006.
Eckert T, Barnes A, Dhawan V, Frucht S, Gordon MF, Feigin AS, et al. FDG PET in the differential diagnosis of parkinsonian disorders. Neuroimage 2005;26:912–21.
Ishida Y, Kawai K, Magata Y, Abe H, Yoshimoto M, Takeda R, et al. Alteration of striatal [11C]raclopride and 6-[18F]fluoro-L-3,4-dihydroxyphenylalanine uptake precedes development of methamphetamine-induced rotation following unilateral 6-hydroxydopamine lesions of medial forebrain bundle in rats. Neurosci Lett 2005;389:30–4.
Strome EM, Cepeda IL, Sossi V, Doudet DJ. Evaluation of the integrity of the dopamine system in a rodent model of Parkinson’s disease: small animal positron emission tomography compared to behavioral assessment and autoradiography. Mol Imaging Biol 2006;8:292–9.
Inaji M, Yoshizaki T, Okauchi T, Maeda J, Nagai Y, Nariai T, et al. In vivo PET measurements with [11C]PE2I to evaluate fetal mesencephalic transplantations to unilateral 6-OHDA-lesioned rats. Cell Transplant 2005;14:655–63.
Wilson AA, DaSilva JN, Houle S. In vivo evaluation of [11C]- and [18F]-labelled cocaine analogues as potential dopamine transporter ligands for positron emission tomography. Nucl Med Biol 1996;23:141–6.
Casteels C, Vermaelen P, Nuyts J, Van Der Linden A, Baekelandt V, Mortelmans L, et al. Construction and evaluation of multitracer small-animal PET probabilistic atlases for voxel-based functional mapping of the rat brain. J Nucl Med 2006;47:1858–66.
Schallert T, Tillerson JL. Intervention strategies for degeneration of dopamine neurons in Parkinsonism: optimizing behavioral assessment of outcome. In: Emerich DF, Dean RL, Sanberg PR, editors. Central nervous system disease : innovative models of CNS diseases from molecule to therapy. Totowa: Humana Press; 2000. pp. 131–51.
Iancu R, Mohapel P, Brundin P, Paul G. Behavioral characterization of a unilateral 6-OHDA-lesion model of Parkinson’s disease in mice. Behav Brain Res 2005;162:1–10.
Lundblad M, Andersson M, Winkler C, Kirik D, Wierup N, Cenci MA. Pharmacological validation of behavioural measures of akinesia and dyskinesia in a rat model of Parkinson’s disease. Eur J Neurosci 2002;15:120–32.
Schweinhardt P, Fransson P, Olson L, Spenger C, Andersson JL. A template for spatial normalisation of MR images of the rat brain. J Neurosci Methods 2003;129:105–13.
Hefti F, Melamed E, Wurtman RJ. Partial lesions of the dopaminergic nigrostriatal system in rat brain: biochemical characterization. Brain Res 1980;195:123–37.
Blum D, Torch S, Lambeng N, Nissou M, Benabid AL, Sadoul R, et al. Molecular pathways involved in the neurotoxicity of 6-OHDA, dopamine and MPTP: contribution to the apoptotic theory in Parkinson’s disease. Prog Neurobiol 2001;65:135–72.
Carlson JD, Pearlstein RD, Buchholz J, Iacono RP, Maeda G. Regional metabolic changes in the pedunculopontine nucleus of unilateral 6-hydroxydopamine Parkinson’s model rats. Brain Res 1999;828:12–9.
Engber TM, Susel Z, Kuo S, Chase TN. Chronic levodopa treatment alters basal and dopamine agonist-stimulated cerebral glucose utilization. J Neurosci 1990;10:3889–95.
Morelli M, Pontieri FE, Linfante I, Orzi F, Di CG. Local cerebral glucose utilization after D1 receptor stimulation in 6-OHDA lesioned rats: effect of sensitization (priming) with a dopaminergic agonist. Synapse 1993;13:264–9.
Wooten GF, Collins RC. Metabolic effects of unilateral lesion of the substantia nigra. J Neurosci 1981;1:285–91.
Cicchetti F, Brownell AL, Williams K, Chen YI, Livni E, Isacson O. Neuroinflammation of the nigrostriatal pathway during progressive 6-OHDA dopamine degeneration in rats monitored by immunohistochemistry and PET imaging. Eur J Neurosci 2002;15:991–8.
Eidelberg D, Moeller JR, Dhawan V, Spetsieris P, Takikawa S, Ishikawa T, et al. The metabolic topography of parkinsonism. J Cereb Blood Flow Metab 1994;14:783–801.
Berding G, Odin P, Brooks DJ, Nikkhah G, Matthies C, Peschel T, et al. Resting regional cerebral glucose metabolism in advanced Parkinson’s disease studied in the off and on conditions with [(18)F]FDG-PET. Mov Disord 2001;16:1014–22.
Huang C, Mattis P, Tang C, Perrine K, Carbon M, Eidelberg D. Metabolic brain networks associated with cognitive function in Parkinson’s disease. Neuroimage 2007;34:714–23.
Gasbarri A, Verney C, Innocenzi R, Campana E, Pacitti C. Mesolimbic dopaminergic neurons innervating the hippocampal formation in the rat: a combined retrograde tracing and immunohistochemical study. Brain Res 1994;668:71–9.
Dagher A, Owen AM, Boecker H, Brooks DJ. The role of the striatum and hippocampus in planning: a PET activation study in Parkinson’s disease. Brain 2001;124:1020–32.
Hilker R, Voges J, Weisenbach S, Kalbe E, Burghaus L, Ghaemi M, et al. Subthalamic nucleus stimulation restores glucose metabolism in associative and limbic cortices and in cerebellum: evidence from a FDG-PET study in advanced Parkinson’s disease. J Cereb Blood Flow Metab 2004;24:7–16.
Chalon S, Emond P, Bodard S, Vilar MP, Thiercelin C, Besnard JC, et al. Time course of changes in striatal dopamine transporters and D2 receptors with specific iodinated markers in a rat model of Parkinson’s disease. Synapse 1999;31:134–9.
Forsback S, Niemi R, Marjamaki P, Eskola O, Bergman J, Gronroos T, et al. Uptake of 6-[18F]fluoro-L-dopa and [18F]CFT reflect nigral neuronal loss in a rat model of Parkinson’s disease. Synapse 2004;51:119–27.
Jeon BS, Jackson-Lewis V, Burke RE. 6-Hydroxydopamine lesion of the rat substantia nigra: time course and morphology of cell death. Neurodegeneration 1995;4:131–7.
Andringa G, Drukarch B, Bol JG, de BK, Sorman K, Habraken JB, et al. Pinhole SPECT imaging of dopamine transporters correlates with dopamine transporter immunohistochemical analysis in the MPTP mouse model of Parkinson’s disease. Neuroimage 2005;26:1150–8.
Kawachi T, Ishii K, Sakamoto S, Matsui M, Mori T, Sasaki M. Gender differences in cerebral glucose metabolism: a PET study. J Neurol Sci 2002;199:79–83.
Otsuka T, Wei L, Bereczki D, Acuff V, Patlak C, Fenstermacher J. Pentobarbital produces dissimilar changes in glucose influx and utilization in brain. Am J Physiol 1991;261:R265–75.
Votaw JR, Byas-Smith MG, Voll R, Halkar R, Goodman MM. Isoflurane alters the amount of dopamine transporter expressed on the plasma membrane in humans. Anesthesiology 2004;101:1128–35.
Araujo DM, Cherry SR, Tatsukawa KJ, Toyokuni T, Kornblum HI. Deficits in striatal dopamine D(2) receptors and energy metabolism detected by in vivo microPET imaging in a rat model of Huntington’s disease. Exp Neurol 2000;166:287–97.
Acknowledgements
The authors acknowledge Peter Vermaelen and Frea Coun for their invaluable assistance in animal preparation and data acquisition. We also thank the PET radiopharmacy staff (M. Bex, T. de Groot ScD, D. Vanderghinste PharmD) for their expert support. KVL is Senior Clinical Researcher and VB a Postdoctoral Researcher for the Fund for Scientific Research Flanders (FWO), Belgium. Financial support of the Research Council of the Katholieke Universiteit Leuven (OT/05/58), the Fund for Scientific Research, Flanders, Belgium (FWO/G.0548.06), and the Institute for Science and Technology SBO project 030238 (AniMoNe) is gratefully acknowledged. This work was funded in part by the European Community FP6 Network-of-Excellence DIMI (LSHB-CT-2005-512146). This experiment was approved by the local Animal Ethics Committee and was according to European Ethics Committee guidelines (decree 86/609/EEC).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Casteels, C., Lauwers, E., Bormans, G. et al. Metabolic–dopaminergic mapping of the 6-hydroxydopamine rat model for Parkinson’s disease. Eur J Nucl Med Mol Imaging 35, 124–134 (2008). https://doi.org/10.1007/s00259-007-0558-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-007-0558-3