Abstract
The androgen receptor (AR) is a hormone receptor that plays a critical role in prostate cancer, and depletion of its ligand has long been the cornerstone of treatment for metastatic disease. Here, we evaluate the AR ligand-binding domain (LBD) as an immunological target, seeking to identify HLA-A2-restricted epitopes recognized by T cells in prostate cancer patients. Ten AR LBD-derived, HLA-A2-binding peptides were identified and ranked with respect to HLA-A2 affinity and were used to culture peptide-specific T cells from HLA-A2+ prostate cancer patients. These T-cell cultures identified peptide-specific T cells specific for all ten peptides in at least one patient, and T cells specific for peptides AR805 and AR811 were detected in over half of patients. Peptide-specific CD8+ T-cell clones were then isolated and characterized for prostate cancer cytotoxicity and cytokine expression, identifying that AR805 and AR811 CD8+ T-cell clones could lyse prostate cancer cells in an HLA-A2-restricted fashion, but only AR811 CTL had polyfunctional cytokine expression. Epitopes were confirmed using immunization studies in HLA-A2 transgenic mice, in which the AR LBD is an autologous antigen with an identical protein sequence, which showed that mice immunized with AR811 developed peptide-specific CTL that lyse HLA-A2+ prostate cancer cells. These data show that AR805 and AR811 are HLA-A2-restricted epitopes for which CTL can be commonly detected in prostate cancer patients. Moreover, CTL responses specific for AR811 can be elicited by direct immunization of A2/DR1 mice. These findings suggest that it may be possible to elicit an anti-prostate tumor immune response by augmenting CTL populations using AR LBD-based vaccines.
Similar content being viewed by others
Introduction
Despite the progress of chemotherapeutic agents for advanced prostate cancer, the significant side effects associated with these therapies have led to increased interest in the development of alternative means of treatment for patients with metastatic disease [1, 2]. One approach is the use of antigen-specific immunotherapies that seek to utilize vaccines to harness the patient’s own immune system to attack the tumor. To date, the development of antigen-specific vaccines for prostate cancer have largely focused on targeting proteins whose expression is restricted to the prostate, such as prostate-specific antigen (PSA) and prostatic acid phosphatase (PAP) [3–5]. However, other important factors include the immunogenicity of the antigen, its role in tumor cell oncogenicity, the expression frequency and amplitude in cancer, and the number of antigenic epitopes [6]. By identifying target antigens that possess many of these qualities, it may be possible to build upon previous successes in prostate cancer immunotherapy and design vaccines that may elicit more potent immunological and clinical responses.
While current prostate cancer vaccines largely focus on targeting antigens expressed solely by the prostate, this approach runs contrary to the methods used to prioritize antigens in many other solid tumors. In diseases like breast, lung, ovarian, and colon cancer, tumor immunologists have commonly focused on targeting antigens whose function is important for the oncogenicity of tumor cells, such as HER2, MUC1, hTERT, and survivin [7–13]. One such functionally important antigen in prostate cancer is the androgen receptor (AR), a steroid hormone receptor whose molecular function has long been established to be critical to the oncogenicity of prostate tumor cells and to the development and progression of all stages of prostate cancer. Work has shown that the AR is required for androgen-dependent tumor growth and that it remains expressed and functionally active in the majority of castrate-resistant tumors [14–17]. Furthermore, while the AR is not strictly tissue-specific, it is predominantly expressed in the prostate, is commonly overexpressed in prostate cancer, and is expressed by most of the cancer cells within a tumor [15, 18, 19].
While the AR has several attractive qualities of an ideal target antigen, one of the potential issues that may arise in targeting the full-length AR is that the amino-terminal domain of this protein contains a significant amount of sequence variation, not only between species but also among human populations. However, the carboxy-terminal ligand-binding domain (LBD) is unique from the rest of the protein in that it has a completely identical protein sequence across many different species, including mice, rats, and humans, suggesting there is some evolutionary importance to the sequence of this domain. When this sequence homology is combined with the functional importance of the AR, it suggests that tumor cells might be less likely to form AR LBD deletion variants to escape the pressures of immunoselection, an observation that has been well documented in other solid tumors as a means to evade an antigen-specific immune response [20–29]. In addition, we have also previously shown that the AR LBD is an immunogenic antigen. We have demonstrated that a significantly higher percentage of patients with prostate cancer have AR LBD-specific antibodies than do healthy donors, and that these responses are present regardless of disease stage [30]. Furthermore, patients who were found to have antibody responses were also found to have concurrent AR LBD-specific cellular immune responses, both in terms of CD4+ and CD8+ T-cell proliferation, as well as IFNγ secretion [30]. This pre-existing immunogenicity, when combined with the role of the AR in tumorigenesis, its relative tissue specificity, and the frequency and amplitude of AR expression in prostate cancer, suggests that the AR LBD may be a preferable immunological target antigen for vaccine development.
In this study, we aimed to further characterize AR LBD-specific cellular immune responses, seeking to identify whether AR LBD peptide-specific CD8+ T cells can lyse prostate tumor cells, and whether there might be dominant MHC class I-restricted responses permitting more detailed study. Furthermore, we also sought to investigate whether A2/DR1 transgenic mice, in which the LBD of the AR is identical in amino acid sequence with the human protein, also have AR LBD peptide-specific T cells, to confirm identified HLA-A2-restricted epitopes, as well as to establish a potential model to evaluate the immunological efficacy of AR LBD-targeted vaccines in vivo.
Materials and methods
Subjects
With informed consent, peripheral blood or leukapheresis products were obtained from HLA-A2-expressing male subjects with prostate cancer at the University of Wisconsin between 2001 and 2009. Three subjects (D04, D05, and P24) had metastatic, castrate-resistant prostate cancer, and the remainder had early PSA-recurrent, non-castrate disease without radiographic evidence of metastatic disease. Peripheral blood mononuclear cells (PBMC) were isolated by Ficoll-Paque centrifugation (Pharmacia AB, Uppsala, Sweden) and either used immediately or cryopreserved in liquid nitrogen. HLA-A2 expression of individual subjects was confirmed serologically from PBMC samples (monoclonal antibody clone BB7.2, BD Biosciences, Franklin Lakes, NJ).
Peptides
Peptides were synthesized, purified to > 80% by HPLC, and the identity and purity confirmed by mass spectrum analysis (United Biochemical Research, Inc., Seattle, WA). Purified peptides were reconstituted in sterile DMSO, sterile filtered, and stored in aliquots at −80°C. Positive control influenza A matrix protein HLA-A2 nonamer epitope (FILGFVFTL) was also used, as previously described [31].
T2 in vitro HLA-A2-binding assay
The HLA-A2 expressing TAP-1 deficient human cell line T2 was used in an assay of HLA-A2 peptide-binding efficiency, in similar fashion to what has been described previously [32]. Briefly, T2 cells cultured in serum-free RPMI-1640 media (Thermo Fisher Scientific, Waltham, MA) and supplemented with human β2-microglobulin (Sigma, St. Louis, MO) were pulsed in triplicate with 50 μg/ml peptide overnight. The next day, cells were stained with a FITC-labeled HLA-A2 monoclonal antibody (clone BB7.2, BD Biosciences) or IgG isotype control, and analyzed by flow cytometric analysis (FACSCalibur, BD Biosciences). Results are reported as a relative mean fluorescence index (MFI) and calculated as the MFI of peptide-pulsed T2 cells compared with the MFI of vehicle-pulsed T2 cells. Assays were performed in quadruplicate, with the standard deviation for replicate analyses shown.
Generation of peptide-specific T-cell lines
Peptide-specific T-cell lines were generated by repetitive weekly in vitro stimulations with peptide-loaded antigen-presenting cells, as previously described [32]. Briefly, autologous DC were pulsed with 10 μg/ml peptide for 2 h, and cultured with autologous T cells (T cell negative isolation kit, Dynal, Carlsbad, CA) in human T-cell medium (RPMI-1640 containing l-glutamine and supplemented with 10% human AB serum (Valley Biomedical, Winchester, VA), 1% sodium pyruvate (Mediatech, Manassas, VA), 1% HEPES (Mediatech), and 0.5% penicillin/streptomycin (Mediatech)) supplemented after 24 h with IL-2 (R&D Systems, Minneapolis, MN) [32]. Cells were restimulated at weekly intervals with irradiated (3000 cGy) peptide-loaded antigen-presenting cells (autologous DC or HLA-A2-expressing B-cell lines) in similar fashion, and T-cell lines were characterized for cytolytic function after 2–8 weeks. T-cell lines found to contain peptide-specific T cells were cloned by limiting dilution. Specifically, cells were diluted to limiting concentrations in 96-well culture plates and cultured for 12–14 days with 5 × 104 irradiated (3,000 cGy) autologous PBMC, 50 U/ml IL-2, and 30 ng/ml anti-CD3 as previously described [32]. Individual clonal lines were tested for cytotoxicity, and peptide-specific lines were further expanded by incubating with 30 ng/ml anti-CD3 (BD Biosciences) along with a 100:1 ratio of feeder lymphoblastoid cell lines to effector cells and a 500:1 ratio of autologous, irradiated PBMC to effector cells. Cultures were given 30 U/ml IL-2 24 h later, and cultures continued 12–14 days with fresh media and IL-2 added every 3–4 days as needed, until suitable numbers of cells were obtained for further analysis.
Intracellular cytokine staining
Expanded T-cell clones were analyzed for intracellular cytokine staining as previously described [32]. Cells were stimulated for 2 h with media alone, a nonspecific peptide, the specific peptide (peptides at 2 μg/ml), or PMA (20 ng/ml, Sigma) and Ionomycin (2 μg/ml, MP Biomedicals). Cells were then treated with monensin (GolgiStop, 2 μM, BD Biosciences) for 4 h at 37°C/5% CO2. Cells were then stained with fluorescently labeled CD3, CD4, and CD8 antibodies, and after fixation and permeabilization, intracellular staining was conducted using fluorescently labeled antibodies for IFNγ and TNFα (BD Biosciences), or the corresponding isotype controls. Cells were subsequently analyzed using an LSR II flow cytometer (BD Biosciences), and events were analyzed by gating CD3+ CD8+ lymphocytes and analyzing this population for expression of IFNγ and/or TNFα.
Cytotoxicity assays
Cytolytic activity was measured by LDH release from target cell lines (Cytotox 96 Assay kit, Promega, Madison, WI) as previously described [32]. In brief, effector cell lines were plated in 96-well plates at various effector-to-target (E:T) cell ratios. Targets used were either T2 cells pulsed with peptide or the human prostate cancer cell lines LNCaP (expressing AR, and stably transduced to express HLA-A2), DU145 (not expressing AR, but stably transduced to express HLA-A2), and LAPC4 (naturally expressing both HLA-A2 and AR). After 4–6 h at 37°C, plates were centrifuged and 50 μl of culture supernatant was assessed for LDH concentration spectrophotometrically, according to the manufacturer’s instructions. Controls included wells with effector cells only, media only, target cells only (minimum release), and target cells with 1% Triton X-100 (maximum release). To confirm HLA-A2-restricted response, AR-expressing cell lines were preincubated with an HLA-A2-specific antibody (BD Biosciences) or nonspecific control murine IgG. The optical density (OD) signal contributed by the media alone was subtracted from all values. The percent-specific activity was then calculated as: (ODexperimental − ODeffector only − ODtarget minimum release)/(ODtarget maximum release − ODtarget minimum release). All sample conditions were evaluated in triplicate, with the standard error shown. Cytotoxic responses were defined as ‘positive’ if titratable peptide-specific lysis was significantly higher than nonspecific lysis (outside the standard error of triplicate samples) in at least two of three titrations.
Animal studies
HLA-A2 transgenic mice (A2/DR1 mice), expressing the α1 and α2 chains of human HLA-A2*01 chimeric with the intracellular α3 chain of the H-2Db allele, and expressing HLA-DR1 with mouse MHC class I (H-2b) and II (I-Ab) knocked out, were graciously provided by Dr. François Lemonnier (Institut Pasteur, Paris, France) [32–34]. Animals were housed in a facility maintained by the Laboratory Animals Resources of the University of Wisconsin Medical School, and all treatments and euthanasia were conducted under an institutional animal care and use (IACUC) committee-approved protocol. Mice were immunized subcutaneously with 100 μg of peptide given with complete Freund’s adjuvant (CFA, Sigma). One week later, splenocytes were collected as has been described [32]. Splenocytes were used ex vivo for IFNγ ELISPOT assays (R&D Systems), and underwent a 1-week peptide restimulation prior to analysis by cytotoxicity assay, as have been described previously [32].
Results
Identification of AR LBD-derived peptides and characterization of their affinity for HLA-A2
The amino acid sequence of the AR LBD was scanned for peptides that conform to the HLA-A2 consensus-binding motif (X-L/M-X-X-X-V-X-X-V/L), previously elucidated by Parker and colleagues [35]. This process identified ten peptides that contained at least two of the three HLA-A2 anchor residues, and are listed in Fig. 1a along with an influenza matrix positive control peptide [31]. These peptides were then analyzed for their predicted HLA-A2 affinity using two algorithms: BIMAS (a program based on the work of Parker and colleagues that provides a predicted t1/2 of dissociation; http://www-bimas.cit.nih.gov/molbio/hla_bind/, [35]) and SYFPEITHI (based on the work of Rammensee and colleagues, this algorithm takes into account a number of characteristics of both the HLA haplotype as well as the peptide of interest, and uses this data to provide a binding score; http://www.syfpeithi.de/, [36]). As shown in Fig. 1a, the BIMAS program predicted that peptides AR700, AR742, AR811, and AR862 have the highest affinity for HLA-A2, whereas the SYFPEITHI program predicted that peptides AR700, AR811, AR859, and AR862 have the highest binding affinity.
AR LBD-derived peptides predicted by sequence analysis to bind to HLA-A2, and characterization of their in vitro HLA-A2-binding affinity. Nonamer or decamer peptides derived from the amino acid sequence of AR LBD were chosen based on sequences conforming to the HLA-A2-binding motif (X-L/M-X-X-X-V-X-X-V/L, [35]). Panel a lists the ten peptides identified using this technique, as well as an influenza matrix peptide positive control, with the name of the peptide indicating the residue of the full-length AR at which the peptide begins. Panel a also lists the predicted HLA-A2-binding affinity of these peptides using the BIMAS (predicted t1/2 of dissociation in minutes, [35]) and SYFPEITHI (binding score, [36]) algorithms. In panel b, AR LBD-derived peptides were evaluated for their affinity for HLA-A2 in vitro using T2-binding assays. T2 cells were pulsed with an AR LBD peptide, an influenza matrix protein positive control, or a negative vehicle control. Twelve hours later, the stabilization of HLA-A2 on the surface of cells was quantified by flow cytometry. Values shown represent the mean fluorescent intensity (MFI) of quadruplicate experimental samples normalized to the MFI of the vehicle control, and can be referenced to the values of the influenza positive control, a peptide known to have strong affinity for HLA-A2
These peptides were then evaluated for their HLA-A2 affinity in vitro using TAP-deficient T2-binding assays. These data are shown in Fig. 1b, and shows that AR700, AR761, AR805, and AR811 have the strongest binding affinity for HLA-A2 in vitro, having comparable affinity to an influenza peptide that is known to have strong affinity for HLA-A2.
Prostate cancer patients have preexisting AR LBD peptide-specific T-cell responses
To determine whether prostate cancer patients have T cells specific for these peptides, T-cell lines were cultured from peripheral blood samples obtained from HLA-A2+ prostate cancer patients and were evaluated weekly for the presence of peptide-specific cytotoxic T lymphocytes (CTL). All ten AR LBD peptides (along with an influenza positive control) were evaluated in up to fifteen patients, and the results are compiled in Table 1. As this table shows, peptide-specific CTL were able to be cultured for all ten AR LBD peptides in at least one of the patients tested. In these studies, the median number of weekly stimulations required for the observation of peptide-specific lysis was between two and four for each of the individual AR LBD-derived peptides. Two of the peptides predicted and found in vitro to have strong affinity for HLA-A2 (AR805 and AR811) were each recognized by T cells in over half (8 of 15) of the patients sampled. Furthermore, all of the prostate cancer patients were found to have responses to at least one of the AR LBD-derived peptides, with some patients having responses to more than half of the peptides (for example, patient P08 had responses to 7/10 AR LBD peptides).
AR805 and AR811 are HLA-A2-restricted epitopes and peptide-specific CD8+ T-cell clones can lyse prostate cancer cells
Peptide-specific T-cell lines were then assessed for their ability to lyse prostate cancer cells, as evidence of whether they represented MHC class I-presented epitopes. As summarized in Table 1, T-cell cultures specific for AR811, in particular, were able to lyse LNCaP cells, an HLA-A2+, AR+ prostate cancer cell line. In addition, in rare instances, T cells specific for the AR761 and AR805 peptides showed some reactivity against prostate cancer cells. As these peptide-specific T cells were frequently found in prostate cancer patients and showed some ability to lyse prostate cancer cells, we sought to further characterize these peptide-specific cells by isolating and characterizing CD8+ T-cell clones.
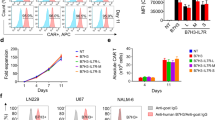
T-cell clones specific for AR761, AR805, and AR811 were isolated by limiting dilution of peptide-specific polyclonal T-cell cultures and were confirmed to be CD3+ CD8+ by flow cytometry (data not shown) and peptide-specific by their cytolytic activity against peptide-pulsed target cells (AR761, AR805, and AR811 peptide-specific lysis shown in Fig. 2a, c, and e, respectively). When these clones were evaluated for their ability to lyse prostate cancer cell lines, AR811 peptide-specific CTL clones (including clones isolated from two separate patients) could efficiently lyse prostate cancer cells in an HLA-A2-restricted and AR-restricted fashion (Fig. 2f). An AR805 peptide-specific CD8+ T-cell clone had low-level lysis against HLA-A2+, AR+ prostate cancer cells (Fig. 2d), whereas AR761 peptide-specific CD8+ T-cell clones from two different patients had no significant prostate cancer cell lysis (Fig. 2b).
AR805 and AR811 peptide-specific CD8+ T-cell clones can lyse prostate cancer cells. CD8+ T-cell clones were isolated specific for either AR761 (top panels, a and b), AR805 (middle panels, c and d), or AR811 (bottom panels, e and f) and were evaluated for cytotoxicity against a panel of target cell lines. The peptide-specificity of clonal populations was confirmed by peptide-specific cytotoxicity assays (left panels) against targets pulsed with their specific peptide (solid black) or a nonspecific peptide (dashed black). Clones were also tested for prostate cancer cytotoxicity (right panels) against LNCaP cells (HLA-A2+, AR+; solid black), LNCaP cells treated with an HLA-A2 blocking antibody (HLA-A2 “−”, AR+; dashed black), LAPC4 cells (HLA-A2+, AR+; solid gray), or DU-145 cells stably transfected to express HLA-A2 (HLA-A2+, AR− ; dashed gray)
AR811 CD8+ T-cell clones have polyfunctional cytokine expression
To investigate possible mechanisms that may contribute to this prostate cancer cytotoxicity, CD8+ T-cell clones were evaluated for polyfunctional intracellular cytokine expression of IFNγ and TNFα. All of the peptide-specific CD8+ T-cell clones were found to have peptide-specific cytokine expression; however, some of the CD3+ CD8+ cells analyzed lacked expression of either immunostimulatory cytokines. This was believed to be likely due to the repeated stimulation and expansion during the T-cell culturing, as well as the presence of residual irradiated feeder cells. However, while all clones had peptide-specific cytokine expression, a sub-analysis of the frequency of cells expressing both cytokines revealed that only AR811 peptide-specific T-cell clones had significant co-expression of both IFNγ and TNFα, whereas AR761 and AR805 clones were found to predominantly express only a single cytokine (Fig. 3).
AR811 peptide-specific CD8+ T-cell clones express both IFNγ and TNFα in a peptide-specific fashion. CD8+ T-cell clones specific for AR761 (top row), AR805 (center row), and AR811 (bottom row) were evaluated for peptide-specific intracellular cytokine expression by flow cytometry. Clones that were confirmed to be peptide-specific were stimulated with media alone (first column), a nonspecific peptide (second column), their particular specific peptide (third column), or a PMA/Ionomycin positive control (fourth column). Cells were gated on CD3+ CD8+ events and were analyzed for intracellular expression of IFNγ and TNFα. The percentage of cells expressing neither cytokine are shown in blue; the percentage of cells expressing only IFNγ are shown in red; the percentage of cells expressing only TNFα are shown in green; and the percentage of cells expressing both IFNγ and TNFα are shown in yellow
Immunization with AR811 augments peptide-specific, cytotoxic immune responses in vivo
To further evaluate these peptides as HLA-A2-restricted epitopes, direct immunization studies were performed in A2/DR1 transgenic mice. The A2/DR1 mouse is an ideal model to study AR LBD peptide-specific immune responses, as this model relies on HLA-A2 for MHC class I antigen presentation, and the amino acid sequence of the murine AR LBD is identical to that of the human. Animals were immunized once subcutaneously with 100 μg of AR761, AR805, AR811, or an influenza-positive control peptide; and one week later, splenocytes from immunized animals were analyzed for the frequency of peptide-specific immune responses by IFNγ ELISPOT. In these studies, immunization with three of the four HLA-A2-restricted peptides (AR761, AR811, and influenza) was found to significantly augment peptide-specific immune responses (Fig. 4). No AR811-specific IFNγ release was detected in control animals (data not shown). Moreover, splenocytes from peptide-immunized animals found to have peptide-specific responses by ELISPOT were also able to recognize and efficiently lyse target cells displaying the peptide of interest, but only AR811-immunized animals were able to lyse the LNCaP human prostate cancer cell line (Fig. 5).
Immunization with HLA-A2-restricted AR761, AR811, and influenza peptides augment peptide-specific immune responses in A2/DR1 transgenic mice. Splenocytes from A2/DR1 mice immunized with AR761, AR805, AR811, or an influenza matrix peptide positive control (groups along the x-axis, with mice per group indicated) were analyzed for the frequency of peptide-specific immune responses by IFNγ ELISPOT. Shown are the frequencies of peptide-specific IFNγ-secreting spot-forming units (SFU) from individual animals immunized stimulated with the specific peptide with which the mice were immunized (gray squares), a nonspecific peptide (black triangles), or a ConA positive control (light gray circles). Group averages are shown by the solid bars, and differences between groups were analyzed by a Student’s t-test (*indicates P < 0.05)
Immunization with AR811 augments peptide-specific, cytotoxic immune responses in vivo. Splenocytes from A2/DR1 animals immunized with either AR761 (a), AR811 (b), or an influenza matrix peptide positive control (c) were analyzed for cytotoxicity against peptide-pulsed (left panels) and prostate cancer (right panels) target cell lines. In the left panels, splenocytes were tested for their ability to lyse T2 cells pulsed with either the specific peptide with which the mice were immunized (black) or a nonspecific peptide (gray). In the right panels, splenocytes were tested for their ability to lyse the LNCaP prostate cancer cell line (dashed black lines) or LNCaP cells treated with an HLA-A2 blocking antibody (dashed gray lines)
Discussion
The identification of peptide-specific CD8+ T cells that can recognize and lyse tumor cells is an important component in the development and prioritization of cancer vaccine target antigens. In this report, we have identified pre-existing CD8+ T-cell responses that recognize HLA-A2-restricted peptides derived from the AR LBD using both in vitro and in vivo models. These peptides were found to have varying affinity for HLA-A2, and T cells specific for all of these peptides could be detected in at least one of the HLA-A2+ prostate cancer patients sampled. In particular, two peptide-specific CD8+ T-cell populations (specific for either AR805 or AR811) were found in over half (8/15) of the patients sampled. However, while polyclonal T-cell cultures specific for three peptides (AR761, AR805, and AR811) showed some ability to lyse prostate cancer cells, only AR805 and AR811 peptide-specific CD8+ T-cell clones could recognize and lyse these tumor cells. In addition to the work characterizing these peptide-specific immune responses in vitro, we also utilized an HLA-A2 transgenic mouse to study these responses in vivo. Using the A2/DR1 mouse strain, we found that AR811 HLA-A2-restricted peptide-specific T cells could be identified in vivo and could lyse HLA-A2-expressing cells expressing the AR, thus further confirming that AR811 is an HLA-A2-restricted epitope, whereas AR805 appears nonimmunogenic in this model. In addition, these murine studies demonstrated that AR LBD-specific CTL could be augmented through the use of an AR LBD-based vaccine. These data suggest that the AR LBD is a relevant tumor antigen for prostate cancer, is unique among commonly targeted prostate antigens in that it is not a secreted or membrane-bound protein, and has a critical function to the survival and proliferation of tumor cells. The frequency of pre-existing immune responses to the AR LBD shows that it is also an immunogenic antigen, and that AR LBD-specific T cells are not deleted during the development of immunological tolerance. The frequency of these responses, as well as the results from the peptide-immunization studies in A2/DR1 mice (a model in which the AR LBD is a self-antigen), also suggests that it may be possible to augment these peptide-specific CTL in vivo through the use of AR LBD-based therapeutics.
The identification of the AR LBD as an immunological target for the treatment of prostate cancer represents a new way of prioritizing potential target antigens for this disease. As the AR LBD has an important molecular function to the survival and proliferation of prostate tumor cells (in both androgen-dependent and castrate-resistant disease settings), it is unique when compared to commonly targeted antigens such as PAP, PSA, and PSMA, which, though tissue-specific, do not have molecular functions that likely contribute significantly to the oncogenicity of the tumor. This may lead to the outgrowth of tumor escape variants that lack expression of these antigens, whereas tumors that attempt to evade AR LBD-directed therapies by downregulating AR expression could potentially be at a growth disadvantage [21, 24–27]. In addition to its crucial oncogenic activity, the AR also benefits from being an intracellular antigen rather than a secreted protein such as PAP or PSA, allowing epitopes derived from the AR LBD to be directed processed and presented via MHC class I. These qualities, in addition to the AR’s well-documented expression in androgen-dependent and most castrate-resistant tumors, sets the AR LBD apart from other prostate cancer antigens under development and suggest that the AR LBD may be an attractive target for active immunization strategies.
In addition to these qualities, the results from the current study have confirmed previous reports showing that the AR LBD is a highly immunogenic antigen. We have previously reported that at least 17% of patients with prostate cancer have AR LBD-specific antibody responses, a higher frequency of responses than those found against other prostate cancer antigens under active development, such as PSA (5.5% of patients) and PAP (11% of patients), even though these are secreted antigens and as such might be predicted to elicit a predominantly humoral immune response [30, 37]. Similarly, we found that a high percentage of prostate cancer patients have HLA-A2-specific CTL specific for AR LBD-derived epitopes: in fact, 11/15 (73%) patients sampled had AR805 or AR811 epitope-specific CTL that could be cultured in vitro, slightly higher than the frequency of PAP-derived HLA-A2-restricted CD8+ T cells we previously identified (9/15, 60%) [32]. An AR811-bound pentamer (Proimmune, LTD) was synthesized in an attempt to characterize the frequency of AR811 peptide-specific CTL directly ex vivo; however, a lack of HLA-A2 specificity of this pentamer precluded this analysis. However, the high frequency of peptide-specific CTL detected in the in vitro culture system suggests that AR LBD-derived T cells are not deleted by the immune system, both in HLA-A2+ prostate cancer patients as well as the A2/DR1 mouse, and are in fact relatively frequent in these patient populations.
As well as detecting AR LBD peptide-specific CTL that can be cultured from patients with prostate cancer, this work has also identified specific antigenic epitopes derived from the AR LBD that are naturally presented on the surface of tumor cells. In particular, we have identified that AR811 appears to be a relatively immunodominant epitope, with AR811 peptide-specific T cells found in a high percentage of prostate cancer patients as well as having the ability to lyse prostate cancer cells in an AR- and HLA-A2-restricted fashion. AR805 was also found to be an HLA-A2-restricted epitope, with AR805 peptide-specific CTL being commonly found in prostate cancer patients and being able to lyse prostate cancer cells (albeit at lower levels than AR811-specific T cells). Intriguingly, these two epitopes, which share three residues of their primary amino acid sequence, are also in the context of several 15-mer peptides (AR802-816, AR805-819, and AR807-821) that are predicted to have strong affinity for HLA-DR1 [38]. While the importance of CD4+ helper T cells in amplifying peptide-specific CD8+ T-cell responses has long been recognized, the contribution of these hypothesized AR LBD-specific helper T-cell responses in amplifying class I-restricted responses (or even the existence of AR LBD-specific HLA-DR-restricted epitopes) remains a topic of investigation [39]. Indeed, while our group has previously identified AR LBD-specific CD4+ T cells, we have yet to evaluate the peptide-specificity of these responses and how they may contribute to the generation of CD8+ T-cell responses [30].
In the A2/DR1 mouse model, AR811 also appears to be an immunodominant epitope, with all six animals immunized with AR811 developing significant peptide-specific immune responses that could also lyse a human prostate cancer cell line. This is contrasted with the results obtained in the direct immunization studies with AR805, which was found to be nonimmunogenic in the A2/DR1 mouse, with only one animal generating a low-level IFNγ ELISPOT response. This suggests that there could be immunological tolerance to this peptide in the A2/DR1 mouse, or that the 9-mer peptide itself is simply not very immunogenic in this model.
We identified that an AR811 CD8+ T cell clone had significant levels of both IFNγ and TNFα cytokine expression. This may contribute to the apparent immunodominance of AR811-specific T cells, as research in a variety of diseases has shown that polyfunctional T cells that express multiple cytokines have higher levels of effector functions and tend to correlate with improved clinical responses [40–44]. In fact, we found that two different AR811 CD8+ T-cell clones from separate individuals (data not shown) similarly expressed high levels of both IFNγ and TNFα, whereas AR761 and AR805 T-cell clones expressed predominantly TNFα alone. Additional studies would be beneficial to evaluate the expression of a larger panel of cytokines to determine whether these different types of peptide-specific T cells have different overall cytokine profiles and if these profiles correspond with different cytolytic activity. However, the co-expression of two Th1-type cytokines by AR811 CD8+ T-cell clones may be associated with the generation of high avidity AR811 peptide-specific T cells and may contribute to the observed higher levels of prostate cancer cell lysis.
While the affinity between peptides and MHC class I has been shown to have an important role in the development of productive CD8+ T-cell responses, the results from our studies have highlighted the importance of actually culturing peptide-specific T cells to conclusively identify naturally processed and presented CD8+ T-cell epitopes. For example, in the process of identifying AR LBD-derived peptides, we found that the AR700 peptide had strong affinity for HLA-A2. However, when we examined prostate cancer patients for the presence of AR700 peptide-specific T cells, we found that only three of the patients sampled had these responses, that AR700 peptide-specific T cells could not lyse prostate cancer cells, and that these responses were not amplified in A2/DR1 mice immunized with AR700 (data not shown). These results agree with previous findings showing that peptide–MHC affinity is necessary, but not sufficient, for a MHC-restricted peptide to be a naturally processed and presented epitope [45]. In our studies, we found that the three peptides with the weakest HLA-A2 affinity (AR708, AR742, and AR814) were found to be recognized by T cells in the lowest numbers of patients, whereas two of the peptides with the highest affinity for HLA-A2 (AR805 and AR811) were found to be recognized by T cells in more than half of the patients sampled. However, this affinity does not necessarily correlate with whether these peptides are epitopes—of the four peptides with very strong in vitro affinity for HLA-A2 (AR700, AR761, AR805, and AR811), and only AR805 and AR811 were found to be able to lyse AR-expressing cells in an MHC-restricted fashion.
The utilization of A2/DR1 mice to confirm AR811 as a naturally processed and presented prostate cancer epitope also served to establish a potentially ideal model to evaluate AR LBD-based immunotherapies. As mentioned previously, the amino acid sequence of the AR LBD is identical between several species, including mice and humans. When combined with reliance on HLA-A2 for the presentation of MHC class I-derived peptides, the A2/DR1 model allows for the detailed study of the same HLA-A2-restricted immune responses that were characterized in human patients in vitro, and how these responses can be augmented following AR LBD-based immunotherapy. Furthermore, the sequence identity of the AR LBD between these two species could permit the evaluation of the natural generation of AR LBD-specific immune responses, which is not possible for most prostate cancer antigens under active development in which the target antigen is foreign in murine models. This allows the A2/DR1 mouse to serve as a directly relevant model to further study the immunological efficacy of vaccines targeting the AR LBD.
References
Berthold DR, Pond GR, Soban F, de Wit R, Eisenberger M, Tannock IF (2008) Docetaxel plus prednisone or mitoxantrone plus prednisone for advanced prostate cancer: updated survival in the TAX 327 study. J Clin Oncol 26(2):242–245
Tannock IF, de Wit R, Berry WR, Horti J, Pluzanska A, Chi KN, Oudard S, Theodore C, James ND, Turesson I, Rosenthal MA, Eisenberger MA (2004) Docetaxel plus prednisone or mitoxantrone plus prednisone for advanced prostate cancer. N Engl J Med 351(15):1502–1512
Kantoff PW, Schuetz TJ, Blumenstein BA, Glode LM, Bilhartz DL, Wyand M, Manson K, Panicali DL, Laus R, Schlom J, Dahut WL, Arlen PM, Gulley JL, Godfrey WR (2010) Overall survival analysis of a phase II randomized controlled trial of a poxviral-based PSA-targeted immunotherapy in metastatic castration-resistant prostate cancer. J Clin Oncol 28(7):1099–1105
Higano CS, Schellhammer PF, Small EJ, Burch PA, Nemunaitis J, Yuh L, Provost N, Frohlich MW (2009) Integrated data from 2 randomized, double-blind, placebo-controlled, phase 3 trials of active cellular immunotherapy with sipuleucel-T in advanced prostate cancer. Cancer 115(16):3670–3679
McNeel DG, Dunphy EJ, Davies JG, Frye TP, Johnson LE, Staab MJ, Horvath DL, Straus J, Alberti D, Marnocha R, Liu G, Eickhoff JC, Wilding G (2009) Safety and immunological efficacy of a DNA vaccine encoding prostatic acid phosphatase in patients with stage D0 prostate cancer. J Clin Oncol 27(25):4047–4054
Cheever MA, Allison JP, Ferris AS, Finn OJ, Hastings BM, Hecht TT, Mellman I, Prindiville SA, Viner JL, Weiner LM, Matrisian LM (2009) The prioritization of cancer antigens: a national cancer institute pilot project for the acceleration of translational research. Clin Cancer Res 15(17):5323–5337
Andersen MH, Svane IM, Becker JC, Straten PT (2007) The universal character of the tumor-associated antigen survivin. Clin Cancer Res 13(20):5991–5994
Acres B, Limacher JM (2005) MUC1 as a target antigen for cancer immunotherapy. Expert Rev Vaccines 4(4):493–502
Baxevanis CN, Sotiriadou NN, Gritzapis AD, Sotiropoulou PA, Perez SA, Cacoullos NT, Papamichail M (2006) Immunogenic HER-2/neu peptides as tumor vaccines. Cancer Immunol Immunother 55(1):85–95
Disis ML, Grabstein KH, Sleath PR, Cheever MA (1999) Generation of immunity to the HER-2/neu oncogenic protein in patients with breast and ovarian cancer using a peptide-based vaccine. Clin Cancer Res 5(6):1289–1297
Swanton C, Futreal A, Eisen T (2006) Her2-targeted therapies in non-small cell lung cancer. Clin Cancer Res 12(14 Pt 2):4377s–4383s
Scardino A, Gross D, Alves P, Schultze J, Graff-Dubois S, Faure O, Tourdot S, Chouaib S, Nadler L, Lemmonnier F, Bonderheide R, Cardoso A, Kosmatopoulos K (2002) HER-2/neu and hTERT cryptic epitopes as novel targets for broad spectrum tumor immunotherapy. J Immunol 168:5900–5906
Beatty GL, Vonderheide RH (2008) Telomerase as a universal tumor antigen for cancer vaccines. Expert Rev Vaccines 7(7):881–887
Yang Q, Fung KM, Day WV, Kropp BP, Lin HK (2005) Androgen receptor signaling is required for androgen-sensitive human prostate cancer cell proliferation and survival. Cancer Cell Int 5(1):8
Edwards J, Krishna NS, Grigor KM, Bartlett JM (2003) Androgen receptor gene amplification and protein expression in hormone refractory prostate cancer. Br J Cancer 89(3):552–556
Gregory CW, Hamil KG, Kim D, Hall SH, Pretlow TG, Mohler JL, French FS (1998) Androgen receptor expression in androgen-independent prostate cancer is associated with increased expression of androgen-regulated genes. Cancer Res 58(24):5718–5724
Sharifi N, Farrar WL (2006) Androgen receptor as a therapeutic target for androgen independent prostate cancer. Am J Ther 13(2):166–170
Bubendorf L, Kononen J, Koivisto P, Schraml P, Moch H, Gasser TC, Willi N, Mihatsch MJ, Sauter G, Kallioniemi OP (1999) Survey of gene amplifications during prostate cancer progression by high-throughout fluorescence in situ hybridization on tissue microarrays. Cancer Res 59(4):803–806
Heinlein CA, Chang C (2004) Androgen receptor in prostate cancer. Endocr Rev 25(2):276–308
Steinkamp MP, O’Mahony OA, Brogley M, Rehman H, Lapensee EW, Dhanasekaran S, Hofer MD, Kuefer R, Chinnaiyan A, Rubin MA, Pienta KJ, Robins DM (2009) Treatment-dependent androgen receptor mutations in prostate cancer exploit multiple mechanisms to evade therapy. Cancer Res 69(10):4434–4442
Jager E, Ringhoffer M, Altmannsberger M, Arand M, Karback J, Jager D, Oesch F, Knuth A (1997) Immunoselection in vivo: independent loss of MHC class I and melanocyte differentiation antigen expression in metastatic melanoma. Int J Cancer 71(2):142–147
Ranieri E, Kierstead LS, Zarour H, Kirkwood JM, Lotze MT, Whiteside T, Storkus WJ (2000) Dendritic cell/peptide cancer vaccines: clinical responsiveness and epitope spreading. Immunol Invest 29(2):121–125
Wojtowicz-Praga S, Verma UN, Wakefield L, Esteban JM, Hartmann D, Mazumder A (1996) Modulation of B16 melanoma growth and metastasis by anti-transforming growth factor beta antibody and interleukin-2. J Immunother Emphasis Tumor Immunol 19(3):169–175
Schreiber H, Wu TH, Nachman J, Kast WM (2002) Immunodominance and tumor escape. Semin Cancer Biol 12(1):25–31
Marincola FM, Jaffee EM, Hicklin DJ, Ferrone S (2000) Escape of human solid tumors from T-cell recognition: molecular mechanisms and functional significance. Adv Immunol 74:181–273
Riker A, Cormier J, Panelli M, Kammula U, Wang E, Abati A, Fetsch P, Lee KH, Steinberg S, Rosenberg S, Marincola F (1999) Immune selection after antigen-specific immunotherapy of melanoma. Surgery 126(2):112–120
Slingluff CL Jr, Colella TA, Thompson L, Graham DD, Skipper JC, Caldwell J, Brinckerhoff L, Kittlesen DJ, Deacon DH, Oei C, Harthun NL, Huczko EL, Hunt DF, Darrow TL, Engelhard VH (2000) Melanomas with concordant loss of multiple melanocytic differentiation proteins: immune escape that may be overcome by targeting unique or undefined antigens. Cancer Immunol Immunother 48(12):661–672
Gottlieb B, Beitel LK, Wu JH, Trifiro M (2004) The androgen receptor gene mutations database (ARDB): 2004 update. Hum Mutat 23(6):527–533
Hu R, Dunn TA, Wei S, Isharwal S, Veltri RW, Humphreys E, Han M, Partin AW, Vessella RL, Isaacs WB, Bova GS, Luo J (2009) Ligand-independent androgen receptor variants derived from splicing of cryptic exons signify hormone-refractory prostate cancer. Cancer Res 69(1):16–22
Olson BM, McNeel DG (2007) Antibody and T-cell responses specific for the androgen receptor in patients with prostate cancer. Prostate 67(16):1729–1739
Sauma S, Gammon M, Bednarek M, Cunningham B, Biddison W, Hermes J, Porter G, Tamhankar S, Hawkins J, Bush B et al (1993) Recognition by HLA-A2-restricted cytotoxic T lymphocytes of endogenously generated and exogenously provided synthetic peptide analogues of the influenza A virus matrix protein. Hum Immunol 37(4):252–258
Olson BM, Frye TP, Johnson LE, Fong L, Knutson KL, Disis ML, McNeel DG (2010) HLA-A2-restricted T-cell epitopes specific for prostatic acid phosphatase. Cancer Immunol Immunother 59(6):943–953
Pajot A, Michel ML, Fazilleau N, Pancre V, Auriault C, Ojcius DM, Lemonnier FA, Lone YC (2004) A mouse model of human adaptive immune functions: HLA-A2.1-/HLA-DR1-transgenic H-2 class I-/class II-knockout mice. Eur J Immunol 34(11):3060–3069
Johannsen A, Genolet R, Legler DF, Luther SA, Luescher IF (2010) Definition of key variables for the induction of optimal NY-ESO-1-specific T cells in HLA transgene mice. J Immunol 185(6):3445–3455
Parker K, Bednarek M, Coligan J (1994) Scheme for ranking potential HLA-A2 binding peptides based on independent binding of individual peptide side-chains. J Immunol 152:163
Rammensee HG, Friede T, Stevanoviic S (1995) MHC ligands and peptide motifs: first listing. Immunogenetics 41(4):178–228
McNeel DG, Nguyen LD, Ellis WJ, Higano CS, Lange PH, Disis ML (2001) Naturally occurring prostate cancer antigen-specific T cell responses of a Th1 phenotype can be detected in patients with prostate cancer. Prostate 47(3):222–229
Rammensee H, Bachmann J, Emmerich NP, Bachor OA, Stevanovic S (1999) SYFPEITHI: database for MHC ligands and peptide motifs. Immunogenetics 50(3–4):213–219
Zhang S, Zhang H, Zhao J (2009) The role of CD4 T cell help for CD8 CTL activation. Biochem Biophys Res Commun 384(4):405–408
Duvall MG, Precopio ML, Ambrozak DA, Jaye A, McMichael AJ, Whittle HC, Roederer M, Rowland-Jones SL, Koup RA (2008) Polyfunctional T cell responses are a hallmark of HIV-2 infection. Eur J Immunol 38(2):350–363
Precopio ML, Betts MR, Parrino J, Price DA, Gostick E, Ambrozak DR, Asher TE, Douek DC, Harari A, Pantaleo G, Bailer R, Graham BS, Roederer M, Koup RA (2007) Immunization with vaccinia virus induces polyfunctional and phenotypically distinctive CD8(+) T cell responses. J Exp Med 204(6):1405–1416
Rizzuto GA, Merghoub T, Hirschhorn-Cymerman D, Liu C, Lesokhin AM, Sahawneh D, Zhong H, Panageas KS, Perales MA, Altan-Bonnet G, Wolchok JD, Houghton AN (2009) Self-antigen-specific CD8+ T cell precursor frequency determines the quality of the antitumor immune response. J Exp Med 206(4):849–866
Seder RA, Darrah PA, Roederer M (2008) T-cell quality in memory and protection: implications for vaccine design. Nat Rev Immunol 8(4):247–258
Yuan J, Gnjatic S, Li H, Powel S, Gallardo HF, Ritter E, Ku GY, Jungbluth AA, Segal NH, Rasalan TS, Manukian G, Xu Y, Roman RA, Terzulli SL, Heywood M, Pogoriler E, Ritter G, Old LJ, Allison JP, Wolchok JD (2008) CTLA-4 blockade enhances polyfunctional NY-ESO-1 specific T cell responses in metastatic melanoma patients with clinical benefit. Proc Natl Acad Sci USA 105(51):20410–20415
Feltkamp MC, Vierboom MP, Kast WM, Melief CJ (1994) Efficient MHC class I-peptide binding is required but does not ensure MHC class I-restricted immunogenicity. Mol Immunol 31(18):1391–1401
Acknowledgments
This work was supported for BMO and DGM by NIH (K23 RR16489 and R01 CA142608) and the US Army Medical Research and Materiel Command (DAMD W81XWH-07-1-0038). The authors would also like to thank Jordan Becker, Edward Dunphy, Thomas Frye, and Laura Johnson for sera collection and peripheral blood mononuclear cell preparation. We would also like to thank Dr. François Lemonnier for his gracious provision of the A2/DR1 transgenic mice, and Heath Smith for critical reading of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Olson, B.M., McNeel, D.G. CD8+ T cells specific for the androgen receptor are common in patients with prostate cancer and are able to lyse prostate tumor cells. Cancer Immunol Immunother 60, 781–792 (2011). https://doi.org/10.1007/s00262-011-0987-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-011-0987-5