Abstract
Purpose
The aim of this study was to evaluate the safety and efficiency, as well as the incorporation characteristics of a specific type of xenograft used for iliac crest defects post-harvesting tri-cortical iliac crest bone graft.
Methods
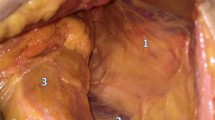
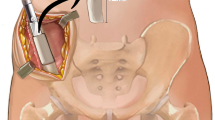
Sixteen patients diagnosed with chronic anterior pelvic pain were operated for pubic symphysis fusion. The tri-cortical graft harvested from the iliac crest was inserted into the pubic symphysis and compressed with a reconstruction plate. The defect in the iliac crest was filled with a block of cancellous bovine substitute (Tutobone®). The length of iliac crest defect, time to fusion of pubic symphysis, time to incorporation of the graft and complications were recorded. The postoperative pain and patients’ satisfaction were evaluated.
Results
The median age of patients was 36.5 years (range 27–75). Fusion was obtained in 15 patients (94 %). The median time to fusion was four months (range three to seven). The length of the iliac crest bone defect ranged from 40 to 70 mm. Integration of the bovine substitute was achieved in 15 patients (94 %) over a median period of three months (range two to six). The postoperative median pain score was 2 (range 1–5). Twelve patients (75 %) reported good satisfaction. No major complications or allergic reactions were observed.
Conclusions
The xenograft used in this study provided a safe and effective method of reconstruction of iliac crest donor site defects. It has satisfactory incorporation, high biocompatibility and no signs of inflammatory reactions. This new technique is simple and easily reproducible in routine clinical practice.


Similar content being viewed by others
References
Mazock JB, Schow SR, Triplett RG (2003) Posterior iliac crest bone harvest: review of technique, complications, and use of an epidural catheter for postoperative pain control. J Oral Maxillofac Surg: Off J Am Assoc Oral Maxillofac Surg 61:1497–1503
Guerado E, Fuerstenberg CH (2011) What bone graft substitutes should we use in post-traumatic spinal fusion? Injury 42(Suppl 2):S64–S71
Dimitriou R, Mataliotakis GI, Angoules AG, Kanakaris NK, Giannoudis PV (2011) Complications following autologous bone graft harvesting from the iliac crest and using the RIA: a systematic review. Injury 42(Suppl 2):S3–S15
Banwart JC, Asher MA, Hassanein RS (1995) Iliac crest bone graft harvest donor site morbidity. A statistical evaluation. Spine 20:1055–1060
Younger EM, Chapman MW (1989) Morbidity at bone graft donor sites. J Orthop Trauma 3:192–195
Westrich GH, Geller DS, O'Malley MJ, Deland JT, Helfet DL (2001) Anterior iliac crest bone graft harvesting using the corticocancellous reamer system. J Orthop Trauma 15:500–506
Halsnad SM, Dhariwal DK, Bocca AP, Evans PL, Hodder SC (2004) Titanium plate reconstruction of the osseous defect after harvest of a composite free flap using the deep circumflex iliac artery. Br J Oral Maxillofac Surg 42:254–256
Huemer GM, Puelacher W, Schoeller T (2004) Improving the iliac crest donor site by plate insertion after harvesting vascularized bone. J Craniomaxillofac Surg 32:387–390
Acharya NK, Mahajan CV, Kumar RJ, Varma HK, Menon VK (2010) Can iliac crest reconstruction reduce donor site morbidity?: a study using degradable hydroxyapatite-bioactive glass ceramic composite. J Spinal Disord Tech 23:266–271
Asano S, Kaneda K, Satoh S, Abumi K, Hashimoto T, Fujiya M (1994) Reconstruction of an iliac crest defect with a bioactive ceramic prosthesis. Eur Spine J 3:39–44
Ito M, Abumi K, Moridaira H, Shono Y, Kotani Y, Minami A, Kaneda K (2005) Iliac crest reconstruction with a bioactive ceramic spacer. Eur Spine J 14:99–102
Defino HL, Rodriguez-Fuentes AE (1999) Reconstruction of anterior iliac crest bone graft donor sites: presentation of a surgical technique. Eur Spine J 8:491–494
Scotti C, Wirz D, Wolf F, Schaefer DJ, Burgin V, Daniels AU, Valderrabano V, Candrian C, Jakob M, Martin I, Barbero A (2010) Engineering human cell-based, functionally integrated osteochondral grafts by biological bonding of engineered cartilage tissues to bony scaffolds. Biomaterials 31:2252–2259
Kubosch D, Milz S, Sprecher CM, Sudkamp NP, Muller CA, Strohm PC (2010) Effect of graft size on graft fracture rate after anterior lumbar spinal fusion in a sheep model. Injury 41:768–771
Candrian C, Barbero A, Bonacina E, Francioli S, Hirschmann MT, Milz S, Valderrabano V, Heberer M, Martin I, Jakob M (2009) A novel implantation technique for engineered osteo-chondral grafts. Knee Surg Sports Traumatol Arthrosc 17:1377–1383
Gil-Albarova J, Gil-Albarova R (2011) Donor site reconstruction in iliac crest tricortical bone graft: surgical technique. Injury. 11 Oct 2011 [Epub ahead of print]
Gogolewski S, Gorna K, Turner AS (2006) Regeneration of bicortical defects in the iliac crest of estrogen-deficient sheep, using new biodegradable polyurethane bone graft substitutes. J Biomed Mater Res A 77:802–810
Resnick DK (2005) Reconstruction of anterior iliac crest after bone graft harvest decreases pain: a randomized, controlled clinical trial. Neurosurgery 57:526–529, discussion 526–529
Bojescul JA, Polly DW Jr, Kuklo TR, Allen TW, Wieand KE (2005) Backfill for iliac-crest donor sites: a prospective, randomized study of coralline hydroxyapatite. Am J Orthop 34:377–382
Bapat MR, Chaudhary K, Garg H, Laheri V (2008) Reconstruction of large iliac crest defects after graft harvest using autogenous rib graft: a prospective controlled study. Spine 33:2570–2575
Dave B, Modi H, Gupta A, Nanda A (2007) Reconstruction of iliac crest with rib to prevent donor site complications: A prospective study of 26 cases. Indian J Orthop 41:180–182
Harris MB, Davis J, Gertzbein SD (1994) Iliac crest reconstruction after tricortical graft harvesting. J Spinal Disord 7:216–221
Corrales LA, Morshed S, Bhandari M, Miclau T 3rd (2008) Variability in the assessment of fracture-healing in orthopaedic trauma studies. J Bone Joint Surg Am 90:1862–1868
Shibuya N, Jupiter DC, Clawson LD, La Fontaine J (2012) Incorporation of bovine-based structural bone grafts used in reconstructive foot surgery. J Foot Ankle Surg 51(1):30–33
Kanakaris NK, Roberts CS, Giannoudis PV (2011) Pregnancy-related pelvic girdle pain: an update. BMC Med 9:15
Kanakaris NK, Angoules AG, Nikolaou VS, Kontakis G, Giannoudis PV (2009) Treatment and outcomes of pelvic malunions and nonunions: a systematic review. Clin Orthop Relat Res 467:2112–2124
Sharma S, Schneider LF, Barr J, Aarabi S, Chibbaro P, Grayson B, Cutting CB (2011) Comparison of minimally invasive versus conventional open harvesting techniques for iliac bone graft in secondary alveolar cleft patients. Plast Reconstr Surg 128:485–491
Delloye C, Cornu O, Druez V, Barbier O (2007) Bone allografts: What they can offer and what they cannot. J Bone Joint Surg Br 89:574–579
Enneking WF, Burchardt H, Puhl JJ, Piotrowski G (1975) Physical and biological aspects of repair in dog cortical-bone transplants. J Bone Joint Surg Am 57:237–252
Enneking WF, Mindell ER (1991) Observations on massive retrieved human allografts. J Bone Joint Surg Am 73:1123–1142
Thull R, Sturm A, Pesch H-J (1993) Mechanische Eigenschaften nativer und praparierter Spongiosa. In: Pesch H-J, Stob H, Kummer B (eds) Osteologie aktuell VII. Springer, Heideberg, pp 157–163
Patil S, Auyeung J, Gower A (2011) Outcome of subtalar fusion using bovine cancellous bone graft: a retrospective case series. J Foot Ankle Surg 50:388–390
Lakdawala A, Todo S, Scott G (2005) The significance of surface changes on retrieved femoral components after total knee replacement. J Bone Joint Surg Br 87:796–799
Meyer S, Floerkemeier T, Windhagen H (2008) Histological osseointegration of Tutobone: first results in human. Arch Orthop Trauma Surg 128:539–544
Conflict of interest
No benefits have been received in any form by any of the authors with regard to the preparation of this manuscript. All authors declare that there is no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Makridis, K.G., Ahmad, M.A., Kanakaris, N.K. et al. Reconstruction of iliac crest with bovine cancellous allograft after bone graft harvest for symphysis pubis arthrodesis. International Orthopaedics (SICOT) 36, 1701–1707 (2012). https://doi.org/10.1007/s00264-012-1572-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-012-1572-z