Abstract
Introduction
Dorsal stabilisation has represented the standard procedure for the treatment of burst fractures of the thoracolumbar spine for a long time, but in the last few years the combined dorsoventral stabilisation has gained in significance due to its higher mechanical stability. However, there are no data yet available indicating whether the patients benefit from the combined operation with regard to their postoperative quality of life and what the advantages are in comparison with the dorsal procedures. Therefore, the question was researched in the framework of a matched-pairs analysis of patients suffering from an unstable fracture of the thoracolumbar transition.
Materials and methods
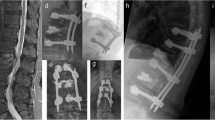
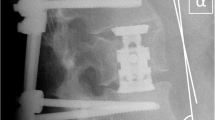
From a consecutive series of patients treated in our clinic between 1995 and 2000, 10 patients with combined and 10 patients with a purely dorsal stabilisation were selected and included in the study. Their quality of life was summed up in retrospect with the SF-36 questionnaire. The X-rays were analysed, and the Cobb angle as well as the sagittal index were calculated. Only patients with burst fractures of the thoracolumbar transition without accompanying co-morbidity and neurological deficits were included in the study. Both of the treated groups were matched with regard to sex, age and radiological patterns of injury.
Results
Patients who had undergone only a dorsal stabilisation showed a significant loss of correction according to the sagittal index at the time of the examination (0.88±0.02 postoperative vs 0.77±0.03 at 4 years postoperatively, p=0.01). In the group of patients treated with the combined therapy, there was no statistically relevant loss of correction with regard to the sagittal vertebral profile. The SF-36 questionnaire showed a reduced quality of life in both groups compared with an age-referenced norm population, especially concerning the parameters of bodily health. No statistically relevant difference was observed between the two groups. Further, there was no statistically relevant association between the parameters of the SF-36 and the clinical and radiological data. After performing several regression analyses it could be shown that the patient’s mental health is a strong predictor of the postoperative vitality (r=0.803, p<0.01). However, none of the remaining parameters was able to predict the postoperative quality of life.
Conclusion
The patients in this study showed a reduced quality of life, independent of the method of surgical treatment. Although better radiological results could be seen for the combined procedure, regarding the postoperative quality of life no advantage could be proved compared with the dorsally stabilized patients. Furthermore, there was no relation between the radiological results and the quality of life parameters. Therefore, it can be assumed that the injury itself seems to be the main cause of the decreased quality of life after a burst fracture of the thoracolumbar transition.





Similar content being viewed by others
References
Boden SD (1998) Outcome assessment after spinal fusion: why and how? Orthop Clin North Am 29:717–728
Böhler L (1972) Conservative treatment of fractures of the thoracic and lumbar spine. Z Unfallmed Berufskr 65:100–104
Briem D, Linhart W, Lehmann W, Bullinger M, Schoder V, Windolf J, Meenen NM, Rueger JM (2003) Investigation of the health-related quality of life after a dorso-ventral stabilization of the thoracolumbar transition. Unfallchirurg 106:625–632
Briem D, Meenen NM, Linhart W, Burchard W, Lehmann W, Rueger JM (2000) Dorsale Stabilisierung von Frakturen des thorakolumbalen Übergangs. Osteosynthese Int [Suppl 1]: S215–S216
Briem D, Rueger JM, Linhart W (2003) Osseous integration of autogenous bone grafts following combined dorso-ventral instrumentation of unstable thoracolumbar spine fractures. Unfallchirurg 106:195–203
Bullinger M (1995) German translation and psychometric testing of the SF-36 Health Survey: preliminary results from the IQOLA Project. International Quality of Life Assessment. Soc Sci Med 41:1359–1366
Bullinger M (1996) Assessment of health related quality of life with the SF-36 Health Survey. Rehabilitation (Stuttg) 35:XVII-XXVII
Bullinger M, Kirchberger I (1998) SF-36 Fragebogen zum Gesundheitszustand. Handanweisung. Hogrefe Verlag für Psychologie, Göttingen
Epstein NE, Hood DC (1997) A comparison of surgeon’s assessment to patient’s self analysis (short form 36) after far lateral lumbar disc surgery. An outcome study. Spine 22:2422–2428
Freidel K, Petermann F, Reichel D, Steiner A, Warschburger P, Weiss HR (2002) Quality of life in women with idiopathic scoliosis. Spine 27:E87-E91
Gelb DE, Lenke LG, Bridwell KH, Blanke K, McEnery KW (1995) An analysis of sagittal spinal alignment in 100 asymptomatic middle and older aged volunteers. Spine 20:1351–1358
Glassman SD, Dimar JR, Johnson JR, Minkow R (1998) Preoperative SF-36 responses as a predictor of reoperation following lumbar fusion. Orthopedics 21:1201–1203
Grevitt M, Khazim R, Webb J, Mulholland R, Shepperd J (1997) The short form-36 health survey questionnaire in spine surgery. J Bone Joint Surg Br 79:48–52
Hägg O, Fritzell P, Ekselius L, Nordwall A (2003) Predictors of outcome in fusion surgery for chronic low back pain. A report from the Swedish Lumbar Spine Study. Eur Spine J 12:22–33
Hall SE, Criddle RA, Comito TL, Prince RL (1999) A case-control study of quality of life and functional impairment in women with long-standing vertebral osteoporotic fracture. Osteoporos Int 9:508–515
Knop C, Blauth M, Buhren V, Arand M, Egbers HJ, Hax PM, Nothwang J, Oestern HJ, Pizanis A, Roth R, Weckbach A, Wentzensen A (2001) Surgical treatment of injuries of the thoracolumbar transition 3. Follow-up examination. Results of a prospective multi-center study by the ‘Spinal’ Study Group of the German Society of Trauma Surgery. Unfallchirurg 104:583–600
Knop C, Blauth M, Buhren V, Hax PM, Kinzl L, Mutschler W, Pommer A, Ulrich C, Wagner S, Weckbach A, Wentzensen A, Worsdorfer O (2000) Surgical treatment of injuries of the thoracolumbar transition. 2. Operation and roentgenologic findings. Unfallchirurg 103:1032–1047
Knop C, Fabian HF, Bastian L, Blauth M (2001) Late results of thoracolumbar fractures after posterior instrumentation and transpedicular bone grafting. Spine 26:88–99
Knop C, Oeser M, Bastian L, Lange U, Zdichavsky M, Blauth M (2001) Development and validation of the Visual Analogue Scale (VAS) Spine Score. Unfallchirurg 104:488–497
Kraemer WJ, Schemitsch EH, Lever J, McBroom RJ, McKee MD, Waddell JP (1996) Functional outcome of thoracolumbar burst fractures without neurological deficit. J Orthop Trauma 10:541–544
Lee SW, Lim TH, You JW, An HS (2000) Biomechanical effect of anterior grafting devices on the rotational stability of spinal constructs. J Spinal Disord 13:150–155
Leferink VJ, Keizer HJ, Oosterhuis JK, Sluis CK van der, Duis HJ ten (2003) Functional outcome in patients with thoracolumbar burst fractures treated with dorsal instrumentation and transpedicular cancellous bone grafting. Eur Spine J 12:261–267
Leferink VJ, Nijboer JM, Zimmerman KW, Veldhuis EF, Vergert EM ten, Duis H ten (2002) Thoracolumbar spinal fractures: segmental range of motion after dorsal spondylodesis in 82 patients: a prospective study. Eur Spine J 11:2-7
Leferink VJ, Zimmerman KW, Veldhuis EF, Vergert EM ten, Duis HJ ten (2001) Thoracolumbar spinal fractures: radiological results of transpedicular fixation combined with transpedicular cancellous bone graft and posterior fusion in 183 patients. Eur Spine J 10:517–523
Magerl F, Aebi M, Gertzbein SD, Harms J, Nazarian S (1994) A comprehensive classification of thoracic and lumbar injuries. Eur Spine J 3:184–201
Nickel R, Egle UT, Eysel P, Rompe JD, Zollner J, Hoffmann SO (2001) Health-related quality of life and somatization in patients with long-term low back pain: a prospective study with 109 patients. Spine 26:2271–2277
Pirente N, Gregor A, Bouillon B, Neugebauer E (2001) Quality of life of severely injured patients 1 year after trauma. A matched-pair study compared with a healthy control group. Unfallchirurg 104:57–63
Reinhold M, Knop C, Lange U, Bastian L, Blauth M (2003) Non-operative treatment of thoracolumbar spinal fractures. Long-term clinical results over 16 years. Unfallchirurg 106:566–576
Seybold EA, Sweeney CA, Fredrickson BE, Warhold LG, Bernini PM (1999) Functional outcome of low lumbar burst fractures. A multicenter review of operative and nonoperative treatment of L3–L5. Spine 24:2154–2161
Shen WJ, Liu TJ, Shen YS (2001) Nonoperative treatment versus posterior fixation for thoracolumbar transition burst fractures without neurologic deficit. Spine 26:1038–1045
Sjölie AN (2002) Psychosocial correlates of low-back pain in adolescents. Eur Spine J 11:582–588
Von Gumppenberg S, Vieweg J, Claudi B, Harms J (1991) Primary management of fresh injuries of the thoracic and lumbar vertebrae. Aktuelle Traumatol 21:265–273
Walchli B, Heini P, Berlemann U (2001) Loss of correction after dorsal stabilization of burst fractures of the thoracolumbar transition. The role of transpedicular spongiosa plasty. Unfallchirurg 104:742–747
Weinstein JN, Collalto P, Lehmann TR (1988) Thoracolumbar ‘burst’ fractures treated conservatively: a long-term follow-up. Spine 13:33–38
Westphal T, Halm JP, Piatek S, Schubert S, Winckler S (2003) Quality of life after calcaneal fractures. A matched-pairs trial with a standardised German control group. Unfallchirurg 106:313–318
Wilke HJ, Kemmerich V, Claes LE, Arand M (2001) Combined anteroposterior spinal fixation provides superior stabilisation to a single anterior or posterior procedure. J Bone Joint Surg Br 83:609–617
Wood K, Butterman G, Mehbod A, Garvey T, Jhanjee R, Sechriest V (2003) Operative compared with nonoperative treatment of a thoracolumbar burst fracture without neurological deficit. A prospective, randomized study. J Bone Joint Surg Am 85:773–781
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Briem, D., Lehmann, W., Ruecker, A.H. et al. Factors influencing the quality of life after burst fractures of the thoracolumbar transition. Arch Orthop Trauma Surg 124, 461–468 (2004). https://doi.org/10.1007/s00402-004-0710-5
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-004-0710-5