Abstract
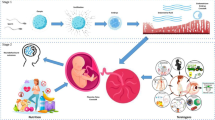
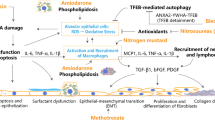
There is extensive epidemiologic and experimental evidence from both animal and human studies that demonstrates detrimental long-term pulmonary outcomes in the offspring of mothers who smoke during pregnancy. However, the molecular mechanisms underlying these associations are not understood. Therefore, it is not surprising that that there is no effective intervention to prevent the damaging effects of perinatal smoke exposure. Using a biologic model of lung development, homeostasis, and repair, we have determined that in utero nicotine exposure disrupts specific molecular paracrine communications between epithelium and interstitium that are driven by parathyroid hormone-related protein and peroxisome proliferator-activated receptor (PPAR)γ, resulting in transdifferentiation of lung lipofibroblasts to myofibroblasts, i.e., the conversion of the lipofibroblast phenotype to a cell type that is not conducive to alveolar homeostasis, and is the cellular hallmark of chronic lung disease, including asthma. Furthermore, we have shown that by molecularly targeting PPARγ expression, nicotine-induced lung injury can not only be significantly averted, it can also be reverted. The concept outlined by us differs from the traditional paradigm of teratogenic and toxicological effects of tobacco smoke that has been proposed in the past. We have argued that since nicotine alters the normal homeostatic epithelial-mesenchymal paracrine signaling in the developing alveolus, rather than causing totally disruptive structural changes, it offers a unique opportunity to prevent, halt, and/or reverse this process through targeted molecular manipulations.

Similar content being viewed by others
References
Editorial (2007) Beyond the lungs—a new view of COPD. Lancet 370:713
Britton J, Edwards R (2008) Tobacco smoking, harm reduction, and nicotine product regulation. Lancet 371:443–445
Rehan VK, Wang Y, Sugano S, Romero S, Chen X, Santos J, Khazanchi A, Torday JS (2005) Mechanism of nicotine-induced pulmonary fibroblast transdifferentiation. Am J Physiol Lung Cell Mol Physiol 289:L667–L676
Rehan VK, Wang Y, Sugano S, Santos J, Patel S, Sakurai R, Boros LG, Lee WP, Torday JS (2007) In utero nicotine exposure alters fetal rat lung alveolar type II cell proliferation, differentiation, and metabolism. Am J Physiol Lung Cell Mol Physiol 292:L323–L333
Rehan VK, Sakurai R, Wang Y, Huynh K, Torday JS (2007) Reversal of nicotine-induced alveolar lipofibroblast-to-myofibroblast transdifferentiation by stimulants of parathyroid hormone-related protein signaling. Lung 185:151–159
Tager IB, Weiss ST, Muñoz A, Rosner B, Speizer FE (1983) Longitudinal study of the effects of maternal smoking on pulmonary function in children. N Engl J Med 309:699–703
Lieberman E, Torday J, Barbieri R, Cohen A, Van Vunakis H, Weiss ST (1992) Association of intrauterine cigarette smoke exposure with indices of fetal lung maturation. Obstet Gynecol 79:564–570
Barker DJ, Osmond C, Golding J, Kuh D, Wadsworth ME (1989) Growth in utero, blood pressure in childhood and adult life, and mortality from cardiovascular disease. BMJ 298:564–567
Liggins GC, Liggins GC, Howie RN (1972) A controlled trial of antepartum glucocorticoid treatment for prevention of the respiratory distress syndrome in premature infants. Pediatrics 50:515–525
Sanchez-Esteban J, Tsai SW, Sang J, Qin J, Torday JS, Rubin LP (1998) Effects of mechanical forces on lung-specific gene expression. Am J Med Sci 316:200–204
Rehan VK, Wang Y, Patel S, Santos J, Torday JS (2006) Rosiglitazone, a peroxisome proliferator-activated receptor-gamma agonist, prevents hyperoxia-induced neonatal rat lung injury in vivo. Pediatr Pulmonol 41:558–569
Dasgupta C, Wang Y, Sakurai R, Torday JS, Rehan VK (2009) Hyperoxia-induced neonatal lung injury involves activation of TGF-β and Wnt signaling: protection by rosiglitazone. Am J Physiol Lung Cell Mol Physiol 296:L1031–L1041
Rehan VK, Dargan-Batra SK, Wang Y, Cerny L, Sakurai R, Santos J, Beloosesky R, Gayle D, Torday JS (2007) A paradoxical temporal response of the PTHrP/PPARgamma signaling pathway to lipopolysaccharide in an in vitro model of the developing rat lung. Am J Physiol Lung Cell Mol Physiol 293:L182–L190
Smith BT (1979) Lung maturation in the fetal rat: acceleration by injection of fibroblast-pneumonocyte factor. Science 204:1094–1095
Heuberger B, Fitzka I, Wasner G, Kratochwil K (1982) Induction of androgen receptor formation by epithelium-mesenchyme interaction in embryonic mouse mammary gland. Proc Natl Acad Sci USA 79:2957–2961
Vaccaro C, Brody JS (1978) Ultrastructure of developing alveoli. I. The role of the interstitial fibroblast. Anat Rec 192:467–479
Torday J, Hua J, Slavin R (1995) Metabolism and fate of neutral lipids of fetal lung fibroblast origin. Biochim Biophys Acta 1254:198–206
Torday JS, Sun H, Qin J (1998) Prostaglandin E2 integrates the effects of fluid distension and glucocorticoid on lung maturation. Am J Physiol 274:L106–L111
Faridy EE, Permutt S, Riley RL (1966) Effect of ventilation on surface forces in excised dogs’ lungs. J Appl Physiol 21:1453–1462
Wyszogrodski I, Kyei-Aboagye K, Taeusch HW Jr, Avery ME (1975) Surfactant inactivation by hyperventilation: conservation by end-expiratory pressure. J Appl Physiol 38:461–466
Oyarzun MJ, Clements JA, Baritussio A (1980) Ventilation enhances pulmonary alveolar clearance of radioactive dipalmitoyl phosphatidylcholine in liposomes. Am Rev Respir Dis 121:709–721
Hastings RH, Duong H, Burton DW, Deftos LJ (1994) Alveolar epithelial cells express and secrete parathyroid hormone-related protein. Am J Respir Cell Mol Biol 11:701–706
Lee K, Deeds JD, Segre GV (1995) Expression of parathyroid hormone-related peptide and its receptor messenger ribonucleic acids during fetal development of rats. Endocrinology 136:453–463
Yamamoto M, Harm SC, Grasser WA, Thiede MA (1992) Parathyroid hormone-related protein in the rat urinary bladder: a smooth muscle relaxant produced locally in response to mechanical stretch. Proc Natl Acad Sci USA 89:5326–5330
Daifotis AG, Weir EC, Dreyer BE, Broadus AE (1992) Stretch-induced parathyroid hormone-related peptide gene expression in the rat uterus. J Biol Chem 267:23455–23458
Alcorn D, Adamson TM, Lambert TF, Maloney JE, Ritchie BC, Robinson PM (1977) Morphological effects of chronic tracheal ligation and drainage in the fetal lamb lung. J Anat 123:649–660
Rubin LP, Kovacs CS, De Paepe ME, Tsai SW, Torday JS, Kronenberg HM (2004) Arrested pulmonary alveolar cytodifferentiation and defective surfactant synthesis in mice missing the gene for parathyroid hormone-related protein. Dev Dyn 230:278–289
Rubin LP, Kifor O, Hua J, Brown EM, Torday JS (1994) Parathyroid hormone (PTH) and PTH-related protein stimulate surfactant phospholipid synthesis in rat fetal lung, apparently by a mesenchymal-epithelial mechanism. Biochim Biophys Acta 1223:91–100
Torday JS, Sanchez-Esteban J, Rubin LP (1998) Paracrine mediators of mechanotransduction in lung development. Am J Med Sci 316:205–208
McGowan SE, Torday JS (1997) The pulmonary lipofibroblast (lipid interstitial cell) and its contributions to alveolar development. Annu Rev Physiol 59:43–62
Gao J, Serrero G (1999) Adipose differentiation related protein (ADRP) expressed in transfected COS-7 cells selectively stimulates long chain fatty acid uptake. J Biol Chem 274:16825–16830
Schultz CJ, Torres E, Londos C, Torday JS (2002) Role of adipocyte differentiation-related protein in surfactant phospholipid synthesis by type II cells. Am J Physiol Lung Cell Mol Physiol 283:L288–L296
Torday JS, Sun H, Wang L, Torres E, Sunday ME, Rubin LP (2002) Leptin mediates the parathyroid hormone-related protein paracrine stimulation of fetal lung maturation. Am J Physiol Lung Cell Mol Physiol 282:L405–L410
Torday JS, Rehan VK (2002) Stretch-stimulated surfactant synthesis is coordinated by the paracrine actions of PTHrP and leptin. Am J Physiol Lung Cell Mol Physiol 283:L130–L135
Torday JS, Torres E, Rehan VK (2003) The role of fibroblast transdifferentiation in lung epithelial cell proliferation, differentiation and repair in vitro. Pediatr Pathol Mol Med 22:189–207
Blacquière MJ, Timens W, Melgert BN, Geerlings M, Postma DS, Hylkema MN (2009) Maternal smoking during pregnancy induces airway remodeling in mice offspring. Eur Respir J 33:1133–1140
Moshammer H, Hoek G, Luttmann-Gibson H, Neuberger MA (2006) Parental smoking and lung function in children: an international study. Am J Respir Crit Care Med 173:1255–1263
Hofhuis W, de Jongste JC, Merkus PJ (2003) Adverse health effects of prenatal and postnatal tobacco smoke exposure on children. Arch Dis Child 88:1086–1090
Collins MH, Moessinger AC, Kleinerman J (1985) Fetal lung hypoplasia associated with maternal smoking: a morphometric analysis. Pediatr Res 19:408–412
Bassi JA, Rosso P, Moessinger AC, Blanc WA, James LS (1984) Fetal lung growth retardation due to maternal tobacco smoke exposure in the rat. Pediatr Res 18:127–130
Maritz GS, Dennis H (1998) Maternal nicotine exposure during gestation and lactation interferes with alveolar development in the neonatal lung. Reprod Fertil Dev 10:255–261
Cunningham J, Dockery DW, Speizer FE (1994) Maternal smoking during pregnancy as a predictor of lung function in children. Am J Epidemiol 139:1139–1152
Hanrahan JP, Tager IB, Segal MR (1992) The effect of maternal smoking during pregnancy on early infant lung function. Am Rev Respir Dis 145:1129–1135
Strachan DP, Cook DG (1997) Health effects of passive smoking. 1. Parental smoking and lower respiratory illness in infancy and early childhood. Thorax 52:905–914
DiFranza JR, Aligne CA, Weitzman M (2004) Prenatal and postnatal environmental tobacco smoke exposure and children’s health. Pediatrics 113:1007–1015
Haberg SE, Stigum H, Nystad W, Nafstad P (2007) Effects of pre- and postnatal exposure to parental smoking on early childhood respiratory health. Am J Epidemiol 166:679–686
Shah T, Sullivan K, Carter J (2006) Sudden infant death syndrome and reported maternal smoking during pregnancy. Am J Public Health 96:1757–1759
Eugenín J, Otárola M, Bravo E, Coddou C, Cerpa V, Reyes-Parada M, Llona I, von Bernhardi R (2008) Prenatal to early postnatal nicotine exposure impairs central chemoreception and modifies breathing pattern in mouse neonates: a probable link to sudden infant death syndrome. J Neurosci 28:13907–13917
Stick SM, Burton PR, Gurrin L, Sly PD, LeSouef PN (1996) Effects of maternal smoking during pregnancy and a family history of asthma on respiratory function in newborn infants. Lancet 348:1060–1064
Gilliland FD, Berhane K, McConnell R, Gauderman WJ, Vora H, Rappaport EB, Avol E, Peters JM (2000) Maternal smoking during pregnancy, environmental tobacco smoke exposure and childhood lung function. Thorax 55:271–276
von Mutius E (2002) Environmental factors influencing the development and progression of pediatric asthma. J Allergy Clin Immunol 109:5525–5532
Strachan DP, Cook DG (1998) Health effects of passive smoking. 1. Parental smoking and childhood asthma: longitudinal and case control studies. Thorax 53:204–212
Rennard SI, Togo S, Holz O (2006) Cigarette smoke inhibits alveolar repair. Proc Am Thorac Soc 3:703–708
Coultas DB (1998) Health effects of passive smoking. 8. passive smoking and risk of adult asthma and COPD. Thorax 53:381–387
Le Souef PN (2000) Pediatric origins of adult lung diseases. 4. Tobacco related lung diseases begin in childhood. Thorax 55:1063–1067
Hinz B, Phan SH, Thannickal VJ, Galli A, Bochaton-Piallat ML, Gabbiani G (2007) The myofibroblast: one function, multiple origins. Am J Pathol 170:1807–1816
Luck W, Nau H (1984) Nicotine and cotinine concentrations in serum and milk of nursing smokers. Br J Clin Pharmacol 18:9–15
Dempsey D, Jacob P 3rd, Benowitz NL (2002) Accelerated metabolism of nicotine and cotinine in pregnant smokers. J Pharmacol Exp Ther 301:594–598
Luck W, Nau H, Hansen R, Steldinger R (1985) Extent of nicotine and cotinine transfer to the human fetus, placenta and amniotic fluid of smoking mothers. Dev Pharmacol Ther 8:384–395
Szuts T, Olsson S, Lindquist NG, Ullberg S, Pilotti A, Enzell C (1978) Long-term fate of [14C]nicotine in the mouse: retention in the bronchi, melanin-containing tissues and urinary bladder wall. Toxicology 10:207–220
Maritz GS, Thomas RA (1995) Maternal nicotine exposure: response of type II pneumocytes of neonatal rat pups. Cell Biol Int 19:323–331
Roman J, Ritzenthaler JD, Gil Costa A, Rivera HN, Roser-Page S (2004) Nicotine and fibronectin expression in lung fibroblasts: implications for tobacco-related lung tissue remodeling. FASEB J 18:1436–1438
Wuenschell CW, Zhao J, Tefft JD, Warburton D (1998) Nicotine stimulates branching and expression of SP-A and SP-C mRNA in embryonic mouse lung culture. Am J Physiol 278:L165–L170
Matta SG, Balfour DJ, Benowitz NL, Boyd RT (2007) Guidelines on nicotine dose selection for in vivo research. Psychopharmacology (Berl) 190:269–319
Maritz GS, Woolward KM (1992) Effect of maternal nicotine exposure on neonatal lung elastic tissue and possible consequences. S Afr Med J 81:517–519
Benowitz NL (1988) Pharmacologic aspects of cigarette smoking and nicotine addiction. N Eng J Med 319:1318–1330
Sekhon HS, Keller JA, Proskocil BJ, Martin EL, Spindel ER (2002) Maternal nicotine exposure upregulates collagen gene expression in fetal monkey lung: association with α7 nicotinic acetylcholine receptors. Am J Respir Cell Mol Biol 26:31–41
Chen CM, Wang LF, Yeh TF (2005) Effects of maternal nicotine exposure on lung surfactant system in rats. Pediatr Pulmon 39:97–102
Pierce RA, Nguyen NM (2002) Prenatal nicotine exposure and abnormal lung function. Am J Respir Cell Mol Biol 26:1013
Proskocil BJ, Sekhon HS, Clark JA, Lupo SL (2005) Vitamin C prevents the effects of prenatal nicotine on pulmonary function in newborn monkeys. Am J Respir Crit Care Med 171:1032–1039
Sekhon HS, Jia Y, Raab R, Kuryatov A (1999) Prenatal nicotine increases pulmonary alpha7 nicotinic receptor expression and alters fetal lung development in monkeys. J Clin Invest 103:637–647
Sekhon HS, Keller JA, Benowitz NL, Spindel ER (2001) Prenatal nicotine exposure alters pulmonary function in newborn rhesus monkeys. Am J Respir Crit Care Med 164:989–994
Maritz GS, Matthews HL, Aalbers J (2000) Maternal copper supplementation protects the neonatal rat lung against adverse effects of maternal nicotine exposure. Reprod Fertil Dev 12:97–103
Kordom C, Maritz GS, De Kock M (2003) Maternal nicotine exposure during pregnancy and lactation: I. Effect on glycolysis in the lungs of the offspring. Exp Lung Res 29:29–89
Tager IB, Ngo L, Hanrahan JP (1995) Maternal smoking during pregnancy. Effects on lung function during the first 18 months of life. Am J Respir Crit Care Med 152:977–983
Hoo AF, Henschen M, Dezateux C, Costeloe K, Stocks J (1998) Respiratory function among preterm infants whose mothers smoked during pregnancy. Am J Respir Crit Care Med 158:700–705
Sandberg K, Poole SD, Hamdan A, Arbogast P, Sundell HW (2004) Altered lung development after prenatal nicotine exposure in young lambs. Pediatr Res 56:432–439
Van Lommel A (2001) Pulmonary neuroendocrine cells (PNEC) and neuroepithelial bodies (NEB): chemoreceptors and regulators of lung development. Paediatr Respir Rev 2:171–176
Martin JA, Hamilton BE, Sutton PD, Ventura SJ, Menacker F, Munson ML (2003) Births: final data for 2002. Natl Vital Stat Rep 52:1–113
Wang Y, Santos J, Sakurai R, O’Roark E, Kenyon N, Torday JS, Rehan VK (2007) Prevention of perinatal nicotine exposure-induced alterations in pulmonary function by Peroxisome Proliferator Activated Receptor gamma (PPARγ) agonists. J Invest Med 56:A124
Cerny LM, Sakurai R, Wang Y, Guo P, Torday JS, Rehan VK (2008) Mechanism of nicotine-induced up-regulation of wingless/int (Wnt) signaling in human alveolar interstitial fibroblasts. J Invest Med 56:A287
Mannino DM, Moorman JE, Kingsley B, Rose D, Repace J (2001) Health effects related to environmental tobacco smoke exposure in children in the United States: data from the Third National Health and Nutrition Examination Survey. Arch Pediatr Adolesc Med 155:36–41
Landau LI (2008) Tobacco smoke exposure and tracking of lung function into adult life. Paediatr Respir Rev 9:39–43
National Institutes of Health (1994) Effect of corticosteroids for fetal maturation on perinatal outcomes. NIH Consens Statement 12:1–24
Nielsen HC (1992) Testosterone regulation of sex differences in fetal lung development. Proc Soc Exp Biol Med 199:446–452
Rodriguez A, Viscardi RM, Torday JS (2001) Fetal androgen exposure inhibits fetal rat lung fibroblast lipid uptake and release. Exp Lung Res 27:13–24
Torday JS (1985) Dihydrotestosterone inhibits fibroblast-pneumonocyte factor-mediated synthesis of saturated phosphatidylcholine by fetal rat lung cells. Biochim Biophys Acta 835:23–28
Singh R, Artaza JN, Taylor WE, Braga M, Yuan X, Gonzalez-Cadavid NF, Bhasin S (2006) Testosterone inhibits adipogenic differentiation in 3T3–L1 cells: nuclear translocation of androgen receptor complex with beta-catenin and T-cell factor 4 may bypass canonical Wnt signaling to down-regulate adipogenic transcription factors. Endocrinology 147:141–154
Wang Y, Sakurai R, Cerny L, Torday JS, Rehan VK (2009) Peroxisome Proliferator-Activated Receptor (PPAR) γ agonist enhance lung maturation in a neonatal rat model. Pediatric Res 65:150–155
Acknowledgments
This study was supported by research grants from the National Institutes of Health (HL075405, HL55268, HD51857) and the California Tobacco-Related Disease Research Program (14RT-0073, 15IT-0250 and 17RT-0170) to VKR and JST, and to KA from the National Institutes of Health (R13 ES016516), Flight Attendant Medical Research Institute, Society for Free Radical Research International, and the California Oxygen Club.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rehan, V.K., Asotra, K. & Torday, J.S. The Effects of Smoking on the Developing Lung: Insights from a Biologic Model for Lung Development, Homeostasis, and Repair. Lung 187, 281–289 (2009). https://doi.org/10.1007/s00408-009-9158-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-009-9158-2