Abstract
Keratan sulphate (KS) proteoglycans (PGs) are key molecules in the corneal stroma for tissue organisation and transparency. Macular corneal dystrophy (MCD) is a rare, autosomal recessive disease characterised by disturbances in KS expression. MCD is caused by mutations in CHST6, a gene encoding the enzyme responsible for KS sulphation. Sulphated KS is absent in type I disease causing corneal opacity and loss of vision. Genetic studies have highlighted the mutational heterogeneity in MCD, but supportive immunohistochemical studies on corneal KS have previously been limited by the availability of antibodies mostly reactive only with highly sulphated KS epitopes. In this study, we employed four antibodies against specific KS sulphation patterns, including one against unsulphated KS, to investigate their reactivity in a case of MCD compared with normal cornea using high-resolution immunogold electron microscopy. Mutation analysis indicated type I MCD with deletion of the entire open reading frame of CHST6. Contrast enhanced fixation revealed larger PG structures in MCD than normal. Unlike normal cornea, MCD cornea showed positive labelling with antibody to unsulphated KSPG, but was negative with antibodies to sulphated KSPG. These antibodies will thus facilitate high-resolution investigations of phenotypic heterogeneity in support of genetic studies in this disease.
Similar content being viewed by others
Introduction
The gamut of molecular interactions which bestow upon the cornea its unique transparent qualities have yet to be fully elucidated. Small leucine-rich keratan sulphate (KS) and chondroitin/dermatan sulphate (CS/DS) proteoglycans (PGs) in the corneal stroma are currently believed to fulfil an essential contributory role by influencing collagen fibril organisation and tissue hydration. KSPGs in cornea are characterised by glycosaminoglycan chains attached via a mono- or bi-antennary oligosaccharide, N-linked to asparagine residues on one of the three KSPG core proteins, lumican, keratocan or mimecan (Funderburgh 2000). KS chains are highly sulphated in cornea with a potential for considerable heterogeneity in the distribution of unsulphated, monosulphated and disulphated disaccharides along the KS chain.
KSPGs are closely associated with collagen fibrils in cornea to which they appear to bind specifically at sites on the ‘a’ and ‘c’ bands along the D period (Scott and Haigh 1988). They may therefore act to control corneal collagen fibril spacing and in this role their water binding properties may be crucial. KSPGs are normally underhydrated, thus perhaps providing a mechanism for subtle regulation of stromal hydration to maintain tissue transparency.
Transgenic mice with null mutations for the KSPG, lumican, develop stromal opacity with sulphated KS levels reduced by 25% (Chakravarti et al. 1998). Further evidence for the importance to corneal transparency of KSPGs and in particular their sulphation, is presented by the rare autosomal recessive disease macular corneal dystrophy (MCD) (OMIM #217800). Patients with this disorder develop corneal haze in their early teenage years which later progresses to corneal opacity and loss of vision. The severity is such that a corneal transplant is required to restore sight. MCD was found to be caused by mutations in CHST6 (OMIM *605294), a gene coding for a sulphotransferase enzyme which catalyses the addition of sulphate to the 6-O-position of GlcNAc on the poly-N-acetyllactosamine chains of KS (Akama et al. 2000, 2001). CHST6 mutations are apparently not highly conserved, as demonstrated by the recent discovery of twenty distinct mutations in a study of 51 southern Indian families with MCD (Warren et al. 2003). Increasing numbers of mutations in CHST6 have been identified in recent years in groups of patients with MCD from different ethnic backgrounds (Sultana et al. 2005; El-Ashry et al. 2005; Warren et al. 2003; Iida-Hasegawa et al. 2003). A recent comprehensive review concluded that subtle changes in CHST6 or genetic heterogeneity may underlie the mutational diversity recorded in this condition (Klintworth et al. 2006).
In contrast, there is little evidence of phenotypic heterogeneity in MCD. Immunoassays and immunohistochemical analyses have previously identified three main variants of MCD: type I, the commonest form, where sulphated KS is undetectable in cornea and serum (Yang et al. 1988; Edward et al. 1988); type II where sulphated KS is present in serum and cornea but at much reduced levels (Yang et al. 1988); and type IA where it is absent from serum and corneal matrix, but present within stromal keratocytes (Klintworth et al. 1997). Phenotypic classification of MCD subtypes has previously relied upon the demonstration of corneal immunoreactivity when probed with the anti-KS monoclonal antibody 5D4 (Caterson et al. 1985; Iida-Hasegawa et al. 2003). The antibody is well characterised, reacting with linear penta-sulphated, or larger, sequences of N-acetyl lactosamine disaccharides where both GalNAc and Gal are sulphated on glycosaminoglycan chains of KSPGs (Mehmet et al. 1986). 5D4 antibody thus only allows identification of the presence, or absence, of highly sulphated KSPG. KSPGs with lesser sulphated or unsulphated chains cannot be detected. Consequently, more detailed investigation of KSPG sulphation profiles in MCD subtypes has hitherto been impossible. To date, only one previous study has successfully detected unsulphated KS in MCD using the lectin Erythrina cristagalli agglutinin (Lewis et al. 2000). Here, we report KS immunodetection in normal and MCD cornea using a panel of four monoclonal antibodies with different specificities for sulphation patterns on KSPG. One of these reagents, anti-‘i’ antibody recognises poly-N acetyllactosamine structures present in unsulphated KS.
Materials and methods
Tissue samples
All samples were obtained with patients’ informed consent and treated in accordance with the tenets of the Declaration of Helsinki and local ethical regulations.
A 20-year-old man of Iranian origin with MCD underwent an 8 mm penetrating keratoplasty in the treatment of the corneal opacity in his left eye. The corneal button excised at surgery and a 10-ml sample of peripheral venous blood were obtained for laboratory investigation.
Control corneal tissue for KS localisation by immunoelectron microscopy and Cupromeronic blue staining, respectively, were obtained from the eye of a 55-year-old male donated for corneal transplantation, and a 54-year-old female patient whose pseudotumour required enucleation. Corneal tissue was isolated from the MCD patient and control enucleated eye within minutes of surgery and transferred immediately to fixative solutions as described below. Control specimens for immunoelectron microscopy were dissected from the transplant donor eye and transferred to fixative within 24 h post-mortem, the eye having been stored in a sterile, moist chamber at 4°C for approximately 10 h.
KS sulphation levels are known to undergo dramatic alterations in the cornea during embryonic development closely associated with the acquisition and maintenance of corneal transparency, and are likely to be tightly regulated after birth in young and old individuals. Consequently, age differences between the control and MCD corneas were considered unlikely to influence comparisons in this study. Age-related changes in human corneal KS sulphation levels have not been studied in detail between young adult and late middle age. However, in cartilage average chain molecular weight was found to exhibit little change between 18–85 years and levels of sulphation also remain fairly constant.
Molecular genetic analysis
DNA was prepared from peripheral leukocytes isolated from the patient’s blood sample using the Nucleon III BACC3 genomic DNA extraction kit according to the manufacturer’s instructions (GE Healthcare). The coding region of CHST6 was amplified using sets of primers described previously (Akama et al. 2000). Amplification was carried out in a 25-μl mixture containing 12.5 μl of Reddy Mix PCR Master Mix (ABgene), 50 pmol gene-specific primers and approximately 50 ng of genomic DNA.
Tissue preparation for electron microscopy
Tissue blocks (approximately 1 × 5 mm) from the central region of the excised corneal button were fixed either:
-
1.
In 2.5% glutaraldehyde in 25 mM sodium acetate buffer plus 0.1 M magnesium chloride and 0.05% Cupromeronic blue™ (USBiological) at pH 5.7 for 18 h, and embedded in epoxy resin according to published methods (Scott and Haigh 1988; Quantock et al. 1993), for visualisation of all stromal PGs. Ultrathin sections were cut on a Leica UC6 ultramicrotome, collected on uncoated 300-mesh copper grids and contrasted with 1% aqueous phosphotungstic acid (1 min at 20°C) and uranyl acetate (30 min at 50°C); or,
-
2.
In 1% glutaraldehyde or 4% paraformaldehyde in 0.1 M Sörensen’s phosphate buffer at pH 7.4 for 2 h. After immersion in 0.5 M ammonium chloride solution for 4 h at 4°C to block free aldehyde groups, samples were dehydrated in graded concentrations of ethanol by progressive lowering of temperature. They were infiltrated and embedded in Lowicryl® K4 M resin (Agar Scientific, Stansted, UK), with UV polymerisation at −25°C in a Leica AFS. Sections were collected on formvar-coated 300-mesh nickel grids for immunolocalisation of KSPGs.
Postembedding immunogold labelling
Non-specific binding was blocked by first floating grids sections downwards on 1% bovine serum albumin in phosphate buffered saline (PBS), followed by a 2 h incubation on primary antibodies shown in Table 1. Sections exposed to the monoclonal antibody BKS-1 were first pre-treated with keratanase (EC 3.2.103: 5 U/ml in 0.1 M Tris acetate buffer, pH 6.8 for 1 h at 37°C), in order to expose the epitope. Incubation on anti-‘i’ antibody was carried out at 4°C for 12 h and all subsequent steps were also undertaken at 4°C to prevent dissociation of the antigen–antibody complex. Grids were washed in several changes of PBS/1% BSA then incubated for 1 h on secondary anti-mouse or anti-human antibodies (IgG or IgM), as appropriate, conjugated to 10 nm colloidal gold (British Biocell International, Cardiff, UK). Sections exposed to anti-‘i’ antibody were then washed in PBS and fixed in 1% glutaraldehyde in PBS for 1 min to stabilise immune complexes. After further washes in distilled water, all sections were contrasted as described above prior to examination in a Philips EM 208 transmission electron microscope operated at 80 kv. Non-specific labelling by secondary antibodies was assessed in sections exposed to PBS/BSA alone with omission of primary antibodies.
Results and discussion
The diseased cornea examined in this study was considered to be type I MCD as monoclonal antibody 5D4 immunoreactivity was absent throughout the stroma and keratocytes, whilst an antibody to poly-N-acetyllactosamine (unsulphated KS) produced a strong positive signal. Genetic analysis also provided supportive evidence as no amplified product was detected for the coding sequence of CHST6.
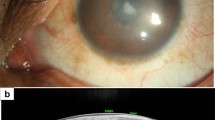
Cupromeronic blue localisation of PGs showed considerably different staining patterns between normal and MCD corneas (Fig. 1a, b), consistent with previous observations using Cuprolinic blue (Quantock et al. 1993). Collagen-associated PGs appeared larger in MCD, with more evident D-periodicity than in normal cornea, presumably owing to the inability of the dye to bind and reveal unsulphated KSPGs, located on ‘a’ and ‘c’ bands (Scott and Haigh 1988). We conclude that in MCD only sulphated CS/DS PGs were localised by Cupromeronic blue. Increased dye binding and thus larger appearance of CS/DS PG complexes, as seen here, would be expected from the 60–70% increase in CS/DS chain concentration reported in MCD (Plaas et al. 2001). Unusually large, strap-like PGs visualised by cupromeronic blue in MCD (Fig. 1b) appear to be another response to KSPG under-sulphation in the cornea. These structures are chondroitinase ABC-sensitive, but have yet to be fully characterised by immunolabelling with specific CS/DS antibodies. Similar large PGs which are also degraded by chondroitinase ABC, are a conspicuous feature of murine cornea that also expresses undersulphated KSPGs (Young et al. 2005). These observations taken together support the view (Meek et al. 1989; Plaas et al. 2001), that the metabolic response of cornea to a matrix deficient in sulphated KS might be oversulphation of other tissue components, such as CS/DS PGs.
Electron micrographs from the mid stromal region in a normal and b MCD corneas showing localisation of proteoglycans with cupromeronic blue dye. Proteoglycans appear as complex arrays of fine collagen-associated filaments in normal and as larger, D-periodic filaments together with large strap-like structures in MCD. Bar = 300 nm
Antibodies recognising KSPGs, such as 5D4, have been widely used diagnostically in MCD, distinguishing at least three phenotypes based on the reduction in expression of highly sulphated KS chains (Klintworth et al. 1997). Negative antibody reactivity, equivalent to absence of consecutive penta-sulphated (or larger) sequences of GlcNAc and Gal, has therefore been critical rather than a positive identification of specific alterations in sulphation patterns. High levels of KSPG labelling in normal cornea by antibody 5D4 (Fig. 2a) can be reduced substantially by pre-treatment of sections with keratanase (data not shown), providing further confirmation of the localisation of high sulphated KS chains as the enzyme cleaves galactosidic linkages between N-acetyl glucosamine (sulphated) and galactose (unsulphated) residues. In contrast, keratanase treatment does not perturb anti-‘i’ antibody labelling in MCD where presumably the enzyme cleavage site is not recognised because sulphated moieties on the polylactosamine chain are absent. Antibody 1B4 gave similar patterns of labelling to 5D4 in normal compared to MCD corneas (Fig. 2c, d), but at reduced intensity, consistent with its known reactivity for lower levels of disulphated disaccharides on KSPGs. Such antibodies, recognising lesser sulphated motifs should facilitate future studies of MCD mutations. Here, minimal activity of GlcNAc 6-sulphotransferase or other sulphotransferases may lead to corneal poly-N-acetyllactosamine chains with increased ratios of mono- and non-sulphated to disulphated disaccharides (Iida-Hasegawa et al. 2003). These have hitherto been undetectable by antibodies with high sulphate motif-specificity. A new N-acetyl-glucosamine-6-sulphate neoepitope antibody, BKS-1, labelled normal but not MCD cornea (Fig. 2e, f). This result was unsurprising owing to the requirement for keratanase cleavage to expose the epitope in the poly-N-acetyllactosamine chain and the inactivity of the enzyme in the absence of appropriate sulphate recognition moieties in MCD KSPG.
Immunogold localisation of KS PGs in normal (a, c, e, g, i) and MCD (b, d, f, h, j) corneas. Non-specific background levels of gold labelling are shown in control preparations where primary antibody was omitted in normal (i) and MCD (j) corneas. Labelling of 5D4 epitope appears intense in normal (a), but is absent in MCD (b). Labelling of normal cornea for 1B4 (c) and BKS-1 (e) epitopes are both positive, but negative in MCD (d, f). Anti-‘i’ epitope is absent in normal cornea (g), but evident from intense clustered gold particle deposition in MCD (h). Bar = 300 nm
Anti-‘i’ antibody was the only one of the four antibodies to show immunoreactivity with corneal matrix in MCD (Fig. 2h), clearly illustrating that KSPGs were unsulphated in the case examined. Antibodies provide greater specificity for recognition of carbohydrate domain structure than lectins (Lewis et al. 2000) and thus offer advantages of improved resolution in immunophenotyping corneal stroma in CHST6 mutations. The anti-‘i’ antibody used here was derived from a patient with autoimmune haemolytic anaemia and had reactivity in common with the cold agglutinins, such as Den and Tho, which recognise two repeating N-acetyllactosamine structures (Galß1–4GlcNAc; Kaufer and Hakomori 1983). Anti-‘i’ antibody would also bind any domains of the poly-N-acetyllactosamine backbone with unsulphated disaccharides in otherwise undersulphated KSPG, yet no positive labelling was recorded in normal cornea (Fig. 2g).
Although based on observations from only one case, the results of this study using immunodetection of highly sulphated compared with unsulphated KSPGs were clearly defined, with reciprocal labelling for these epitopes in MCD and normal corneas, respectively. Further sulphation-motif specific antibody analyses of cornea and serum from cases where MCD mutations are well characterised should facilitate phenotypic classification of this genetically heterogeneous disorder.
References
Akama TO, Nishida K, Nakayama J, Watanabe H, Ozaki K, Nakamura T, Dota A, Kawasaki S, Inoue Y, Maeda N, Yamamoto S, Fujiwara T, Thonar EJ, Shimomura Y, Kinoshita S, Tanigami A, Fukuda MN (2000) Macular corneal dystrophy type I and type II are caused by distinct mutations in a new sulphotransferase gene. Nat Genet 26:237–241
Akama TO, Nakayama J, Nishida K, Hiraoka N, Suzuki M, McAuliffe J, Hindsgaul O, Fukuda M, Fukuda MN (2001) Human corneal GlcNac 6-O-sulfotransferase and mouse intestinal GlcNac 6-O-sulfotransferase both produce keratan sulphate. J Biol Chem 276:16271–16278
Caterson B, Christner JE, Baker JR, Couchman JR (1985) Production and characterization of monoclonal antibodies directed against connective tissue proteoglycans. Federation Proc 44:386–393
Chakravarti S, Magnuson T, Lass JH, Jepsen KJ, LaMantia C, Carroll H (1998) Lumican regulates collagen fibril assembly: skin fragility and corneal opacity in the absence of lumican. J Cell Biol 141:1277–1286
Edward DP, Yue BY, Sugar J, Thonar EJ, SunderRaj N, Stock EL, Tso MO (1988) Heterogeneity in macular corneal dystrophy. Arch Ophthalmol 106:1579–83
El-Ashry MF, Abd El-Aziz MM, Shalaby O, Wilkins S, Poopalasundaram S, Cheetham M, Tuft SJ, Hardcastle AJ, Bhattacharya SS, Ebenezer ND (2005) Novel CHST6 nonsense and missense mutations responsible for macular corneal dystrophy. Am J Ophthalmol 139:192–193
Funderburgh JL (2000) Keratan sulfate: structure, biosynthesis, and function. Glycobiology 10:951–958
Iida-Hasegawa N, Furuhata A, Hayatsu H, Murakami A, Fujiki K, Nakayasu K, Kanai A (2003) Mutations in the CHST6 gene in patients with macular corneal dystrophy: immunohistochemical evidence of heterogeneity. Invest Ophthalmol Vis Sci 44:3272–3277
Kaufer JN, Hakomori S (1983) Glycolipid antigens and genetic markers. In: Hanahan DJ (eds) Handbook of lipid research—sphingolipid biochemistry. Plenum, New York, pp 409–429
Klintworth GK, Oshima E, al-Rajhi A, al-Salif A, Thonar EJ, Karcioglu ZA (1997) Macular corneal dystrophy in Saudi Arabia: a study of 56 cases and recognition of a new immunophenotype. Am J Ophthalmol 124:9–18
Klintworth GK, Smith CF, Bowling BL (2006) CHST6 mutations in North American subjects with macular corneal dystrophy: a comprehensive molecular genetic review. Mol Vis 12:159–176
Lewis D, Davies Y, Nieduszynski IA, Lawrence F, Quantock AJ, Bonshek R, Fullwood NJ (2000) Ultrastructural localization of sulphated and unsulfated keratan sulphate in normal and macular corneal dystrophy type I. Glycobiology 10:305–312
Meek KM, Quantock AJ, Elliott GF, Ridgway AE, Tullo AB, Bron AJ, Thonar EJ (1989) Macular corneal dystrophy: the macromolecular structure of the stroma observed using electron microscopy and synchrotron X-ray diffraction. Exp Eye Res 49:941–958
Mehmet H, Scudder P, Tang PW, Hounsell EF, Caterson B, Feizi T (1986) The antigenic determinants recognized by three monoclonal antibodies to keratan sulphate involve sulphated hepta- or larger oligosaccharides of the poly(N-acetyllactosamine) series. Eur J Biochem 157:385–391
Plaas AH, West LA, Thonar EJ, Karcioglu ZA, Smith CJ, Klintworth GK, Hascall VC (2001) Altered fine structures of corneal and skeletal keratan sulphate and chondroitin/dermatan sulphate in macular corneal dystrophy. J Biol Chem 276:39788–39796
Quantock AJ, Meek KM, Thonar EJ, Assil KK (1993) Synchrotron X-ray diffraction in atypical macular dystrophy. Eye 7:779–784
Scott JE, Haigh M (1988) Identification of specific binding sites for keratan sulfate proteoglycans and chondroitin-dermatan sulfate proteoglycans on collagen fibrils in cornea by the use of cupromeronic blue in ‘critical-electrolyte-concentration’ techniques. Biochem J 253:607–610
Sultana A, Sridhar MS, Klintworth GK, Balasubramanian D, Kannabiran C (2005) Allelic heterogeneity of the carbohydrate sulfotransferase-6 gene in patients with macular corneal dystrophy. Clin Genet 68:454–460
Warren JF, Aldave AJ, Srinivasan M, Thonar EJ, Kumar AB, Cevallos V et al (2003) Novel mutations in the CHST6 gene associated with macular corneal dystrophy in southern India. Arch Ophthalmol 121:1608–1612
Yang CJ, SundarRaj N, Thonar EJ, KlintworthGK (1988) Immunohistochemical evidence of heterogeneity in macular corneal dystrophy. Am J Ophthalmol 106:65–71
Young RD, Tudor D, Hayes AJ, Kerr B, Hayashida Y, Nishida K, Meek KM, Caterson B, Quantock AJ (2005) Atypical composition and ultrastructure of proteoglycans in the mouse corneal stroma. Invest Ophthalmol Vis Sci 46:1973–1978
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Young, R.D., Akama, T.O., Liskova, P. et al. Differential immunogold localisation of sulphated and unsulphated keratan sulphate proteoglycans in normal and macular dystrophy cornea using sulphation motif-specific antibodies. Histochem Cell Biol 127, 115–120 (2007). https://doi.org/10.1007/s00418-006-0228-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00418-006-0228-8