Abstract
Background
The attempt to further reduce operative trauma in laparoscopic cholecystectomy has led to new techniques such as natural orifice transluminal endoscopic surgery (NOTES) and single-incision laparoscopic surgery (SILS). These new techniques are considered to be painless procedures, but no published studies investigate the possibility of different pain scores in these new techniques versus classic laparoscopic cholecystectomy. In this randomized control study, we investigated pain scores in SILS cholecystectomy versus classic laparoscopic cholecystectomy.
Patients and methods
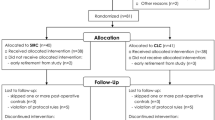
Forty patients (34 women and 6 men) were randomly assigned to two groups. In group A (n = 20) four-port classic laparoscopic cholecystectomy was performed. Patients in group B (n = 20) underwent SILS cholecystectomy. In all patients, preincisional local infiltration of ropivacaine around the trocar wounds was performed. Infusion of ropivacaine solution in the right subdiaphragmatic area at the beginning of the procedure plus normal saline infusion in the same area at the end of the procedure was performed in all patients as well. Shoulder tip and abdominal pain were registered at 2, 6, 12, 24, 48, and 72 h postoperatively using visual analog scale (VAS).
Results
Significantly lower pain scores were observed in the SILS group versus the classic laparoscopic cholecystectomy group after the first 12 h for abdominal pain, and after the first 6 h for shoulder pain. Total pain after the first 24 h was nonexistent in the SILS group. Also, requests for analgesics were significantly less in the SILS group, while no difference was observed in incidence of nausea and vomiting between the two groups.
Conclusion
SILS cholecystectomy, as well as the invisible scar, has significantly lower abdominal and shoulder pain scores, especially after the first 24 h postoperatively, when this pain is nonexistent. (Registration Clinical Trial number: NTC00872287, www.clinicaltrials.gov).
Similar content being viewed by others
References
Zorron R, Maggioni LC, Pombo L, Oliveira AL, Carvalho GL, Filgueiras M (2008) NOTES transvaginal cholecystectomy: preliminary clinical application. Surg Endosc 22:542–547
McGee MF, Rosen MJ, Marks J, Onders RP, Chak A, Faulx A, Chen VK, Ponsky J (2006) A primer on natural orifice transluminal endoscopic surgery: building a new paradigm. Surg Inn 13:86–93
Rattner D, Kalloo A (2006) ASGE/SAGES working group on natural orifice transluminal endoscopic surgery. Surg Endosc 20:329–333
Cuesta MA, Berends F, Veenhof AAFA (2008) The “invisible cholecystectomy”: a transumbilical laparoscopic operation without a scar. Surg Endosc 22:1211–1213
Tacchino R, Greco F, Matera D (2008) Single-incision laparoscopic cholecystectomy: surgery without a visible scar. Surg Endosc 23:896–899
Pappas-Gogos G, Tsimogiannis KE, Zikos N, Nikas K, Manataki A, Tsimoyiannis EC (2008) Preincisional and intraperitoneal ropivacaine plus normal saline infusion for postoperative pain relief after laparoscopic cholecystectomy: a randomized double-blind controlled trial. Surg Endosc 22:2036–2045
Tsimoyiannis EC, Siakas P, Tassis A, Lekkas ET, Tzourou H, Kambili M (1998) Intraperitoneal normal saline infusion for postoperative pain after laparoscopic cholecystectomy. World J Surg 22:824–828
Tsimoyiannis EC, Glantzounis G, Lekkas ET, Siakas P, Jabarin M, Tzourou H (1998) Intraperitoneal normal saline and bupivacaine infusion for reduction of postoperative pain after laparoscopic cholecystectomy. Surg Laparosc Endosc Percutan Tech 8:416–420
Leggett PL, Churchman-Winn R, Miller G (2000) Minimizing ports to improve laparoscopic cholecystectomy. Surg Endosc 14:32–36
Sarli S, Iusco D, Gobbi S, Porrini C, Ferro M, Roncoroni L (2003) Randomized clinical trial of laparoscopic cholecystectomy performed with mini-instruments. Br J Surg 90:1345–1348
Papagiannopoulou P, Argiriadou H, Georgiou M, Papaziogas B, Sfyra E, Kanakoudis F (2003) Preincisional local infiltration of levobupivacaine vs ropivacaine for pain control after laparoscopic cholecystectomy. Surg Endosc 17:1961–1964
Elfberg BA, Sjovall-Mjoberg S (2000) Intraperitoneal bupivacaine does not effectively reduce pain after laparoscopic cholecystectomy: a randomized, placebo-controlled and double blind study. Surg Laparosc Endosc Percutan Tech 10:375–379
Kucuk C, Kadiogullari N, Canoler O, Savli S (2007) A placebo-controlled comparison of bupivacaine and ropivacaine instillation for preventing postoperative pain after laparoscopic cholecystectomy. Surg Today 37:396–400
Bisgaard T, Klarskov B, Kristiansen VB, Callesen T, Svend D, Kehlet H, Rosenberg J (1999) Multiregional local anesthetic infiltration during laparoscopic cholecystectomy in patients receiving prophylactic multimodal analgesia: a randomized, double-blinded, placebo-controlled study. Anesth Analg 89:1017–1024
Korell M, Schmaus F, Strowitzki T, Schneeweiss SG, Hepp H (1996) Pain intensity following laparoscopy. Surg Laparosc Endosc Percutan Tech 6:375–379
Disclosures
Evangelos Tsimoyiannis, Konstadinos Tsimogiannis, George Pappas-Gogos, Charalampos Farantos, Nikolaos Benetatos, Paraskevi Mavridou, and Manataki Adamantia have no financial support from any private institution, and the authors have no financial relationships with any pharmaceutical or device company.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tsimoyiannis, E.C., Tsimogiannis, K.E., Pappas-Gogos, G. et al. Different pain scores in single transumbilical incision laparoscopic cholecystectomy versus classic laparoscopic cholecystectomy: a randomized controlled trial. Surg Endosc 24, 1842–1848 (2010). https://doi.org/10.1007/s00464-010-0887-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-010-0887-3