Abstract
Background
In patients with cirrhosis, subclinical hepatic encephalopathy, which negatively affects the activity of daily living, is often unidentified. In a multicenter observational study, we investigated the possibility of detecting minimal neurological changes consistent with subclinical hepatic encephalopathy by using the Trail Making Test in a cohort of patients with liver cirrhosis at hospital admission.
Methods
Seventy-seven consecutive patients with liver cirrhosis were studied (mean age, 69.5 ± 9.1; 95% confidence interval, 67.5–71.6 years). In all patients, possible encephalopathy was investigated according to the West Haven criteria. All those free of any sign of encephalopathy (West Haven 0) were also studied by the Trail Making Test forms A and B. The Child-Pugh score was determined in all patients, and results were compared with the West Haven stage. Exclusion criteria were use of benzodiazepine, beta adrenergic blockers, alcohol, or antiepileptic drugs, or coexistence of depression, dementia, Parkinson’s disease, or chronic or acute cerebral vasculopathy.
Results
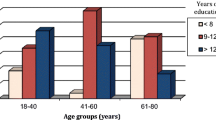
Of the 77 patients, 44 (57.1%, 23 men and 21 women) had West Haven score 0, but among these, 26 (59.1%) were diagnosed with mental impairment likely linked to minimal hepatic encephalopathy. Severity of liver disease correlated with the presence of likely minimal hepatic encephalopathy, because the prevalence of abnormal Trail Making Test results increased from 22.2% in Child-Pugh A, to 63.4% and 74.0% in Child-Pugh B and C, respectively.
Conclusions
The investigation of patients with cirrhosis by the West Haven test is not sufficient to identify subclinical forms of encephalopathy. The Trail Making Test (a simple, inexpensive test) in our series evidenced poor psychometric performance in more than half of the patients who were free of manifest encephalopathy. Subclinical hepatic encephalopathy was present mostly in patients with HCV-related cirrhosis. Detecting minimal hepatic encephalopathy in patients with cirrhosis may help improve their quality of life.
Similar content being viewed by others
References
L Rikkers P Jenko D Rudman D Freides (1978) ArticleTitleSubclinical hepatic encephalopathy: detection, prevalence, and relationship to nitrogen metabolism Gastroenterology 75 462–9 Occurrence Handle1:STN:280:DyaE1c3jvF2jug%3D%3D Occurrence Handle680502
M Groeneweg JC Quero I De Bruijn IJ Hartmann ML Essink-bot WC Hop et al. (1998) ArticleTitleSubclinical hepatic encephalopathy impairs daily functioning Hepatology 28 45–9 10.1002/hep.510280108 Occurrence Handle10.1002/hep.510280108 Occurrence Handle1:STN:280:DyaK1czhvFWktQ%3D%3D Occurrence Handle9657095
C Wein H Koch B Popp G Oehler P Schauder (2004) ArticleTitleMinimal hepatic encephalopathy impairs fitness to drive Hepatology 39 599–601 10.1002/hep.20095 Occurrence Handle10.1002/hep.20095
JC Quero IJ Hartmann J Meulstee WC Hop SW Schalm (1996) ArticleTitleThe diagnosis of subclinical hepatic encephalopathy in patients with cirrhosis using neuropsychological tests and automated electroencephalogram analysis Hepatology 24 556–60 10.1002/hep.510240316 Occurrence Handle10.1002/hep.510240316 Occurrence Handle1:STN:280:DyaK28znsV2nsA%3D%3D Occurrence Handle8781324
P Amodio JC Quero F Del Piccolo A Gatta SW Schalm (1996) ArticleTitleDiagnostic tools for the detection of subclinical hepatic encephalopathy: comparison of standard and computerized psychometric tests with spectral-EEG Metab Brain Dis 11 315–27 10.1007/BF02029493 Occurrence Handle10.1007/BF02029493 Occurrence Handle1:STN:280:DyaK2s7jtlymtA%3D%3D Occurrence Handle8979251
NL Sandford RE Saul (1988) ArticleTitleAssessment of hepatic encephalopathy with visual evoked potentials compared with conventional methods Hepatology 8 1094–8 Occurrence Handle10.1002/hep.1840080519 Occurrence Handle1:STN:280:DyaL1czivF2ntg%3D%3D Occurrence Handle3417229
PS Kharbanda VA Saraswat RK Dhiman (2003) ArticleTitleMinimal hepatic encephalopathy: diagnosis by neuropsychological and neurophysiologic methods Indian J Gastroenterol 22 S37–41 Occurrence Handle15025253
P Amodio P Valenti F Del Piccolo A Pellegrini S Schiff P Angeli et al. (2005) ArticleTitleP300 latency for the diagnosis of minimal hepatic encephalopathy: evidence that spectral EEG analysis and psychometric tests are enough Dig Liver Dis 7 861–8 10.1016/j.dld.2005.06.009 Occurrence Handle10.1016/j.dld.2005.06.009
M Plauth A Raible TA Graser IL Noldeke P Furst W Dolle et al. (1994) ArticleTitleLactulose or paromomycin do not affect ammonia generation in the isolated perfused rat small intestine Z Gastroenterol 32 141–5 Occurrence Handle1:CAS:528:DyaK2cXmsVGrsbc%3D Occurrence Handle8197808
A Duseja RK Dhiman VA Saraswat Y Chawla (2003) ArticleTitleMinimal hepatic encephalopathy: natural history, impact on daily functioning, and role of treatment Indian J Gastroenterol 22 S42–4 Occurrence Handle15025254
AR Giovagnoli M Del Pesce S Mascheroni M Simoncelli M Laiacona E Capitani (1996) ArticleTitleTrail Making Test: normative values from 287 normal adult controls Ital J Neurol Sci 17 305–9 10.1007/BF01997792 Occurrence Handle10.1007/BF01997792 Occurrence Handle1:STN:280:DyaK2s%2FntlSitA%3D%3D Occurrence Handle8915764
JC Quero Guillen M Groeneweg M Jimenez Saenz JM Herrerias Gutierrez (2002) ArticleTitleIs it a medical error if we do not screen cirrhotic patients for minimal hepatic encephalopathy? Rev Esp Enferm Dig 94 544–57 Occurrence Handle1:STN:280:DC%2BD3s%2Fns12hsw%3D%3D Occurrence Handle12587235
M Vergara-Gomez M Flavia-Olivella M Gil-Prades B Dalmau-Obrador J Cordoba-Cardona (2006) ArticleTitleDiagnosis and treatment of hepatic encephalopathy in Spain: results of a survey of hepatologists Gastroenterol Hepatol 29 1–6 10.1157/13083245 Occurrence Handle10.1157/13083245 Occurrence Handle1:STN:280:DC%2BD28%2Fgslygtw%3D%3D Occurrence Handle16393622
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Citro, V., Milan, G., Tripodi, F. et al. Mental status impairment in patients with West Haven grade zero hepatic encephalopathy: the role of HCV infection. J Gastroenterol 42, 79–82 (2007). https://doi.org/10.1007/s00535-006-1978-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-006-1978-8