Abstract
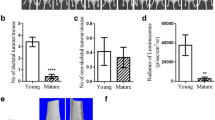
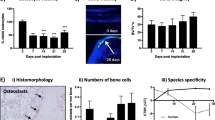
Osteosclerotic metastases account for 20% of breast cancer metastases with the remainder osteolytic or mixed. In mouse models, osteolytic metastases are dependent on bone resorption for their growth. However, whether the growth of osteosclerotic bone metastases depends on osteoclast or osteoblast actions is uncertain. In this study, we investigate the effects of high and low bone resorption on tumour growth in a mouse model of osteosclerotic metastasis. We implanted human breast cancer, MCF-7, cells into the tibiae of mice. Low and high levels of bone resorption were induced by osteoprotegerin (OPG) treatment or calcium deficient diet respectively. We demonstrate that OPG treatment significantly reduces tumour area compared to vehicle (0.42 ± 0.06 vs. 1.27 ± 0.16 mm2, P < 0.01) in association with complete inhibition of osteoclast differentiation. In contrast, low calcium diet increases tumour area compared to normal diet (0.90 ± 0.30 vs. 0.58 ± 0.20 mm2, P < 0.05) in association with increased osteoclast numbers (84.44 ± 5.18 vs. 71.11 ± 3.56 per mm2 bone lesion area, P < 0.05). Osteoblast surfaces and new woven bone formation were similarly increased within the tumour boundaries in all treatment groups. Tumour growth in this model of osteosclerotic metastasis is dependent on ongoing bone resorption, as has been observed in osteolytic models. Bone resorption, rather than bone formation, apparently mediates this effect as osteoblast surfaces in the tumour mass were unchanged by treatments. Treatment of breast cancer patients through correction of calcium deficiency and/or with anti-resorptive agents such as OPG, may improve patient outcomes in the adjuvant as well as palliative settings.



Similar content being viewed by others
Abbreviations
- OPG:
-
Osteoprotegerin
- PTH:
-
Parathyroid hormone
- TRAcP:
-
Tartrate-resistant acid phosphatase
- PTHrP:
-
Parathyroid hormone related protein
- TGFbeta:
-
Transforming growth factor beta
- IGF-1:
-
Insulin-like growth factor-1
- ET-1:
-
Endothelin-1
- BV/TV:
-
Bone volume/tissue volume
- Ob.S/BS:
-
Osteoblast surface/bone surface
References
Coleman RE (2001) Metastatic bone disease: clinical features, pathophysiology and treatment strategies. Cancer Treat Rev 27(3):165–176
Roodman GD (2004) Mechanisms of bone metastasis. N Engl J Med 350(16):1655–1664
Blair JM, Zhou H, Seibel MJ et al (2006) Mechanisms of Disease: roles of OPG, RANKL and RANK in the pathophysiology of skeletal metastasis. Nat Clin Pract Oncol 3(1):41–49
Diel IJ, Solomayer EF, Seibel MJ et al (1999) Serum bone sialoprotein in patients with primary breast cancer is a prognostic marker for subsequent bone metastasis. Clin Cancer Res 5(12):3914–3919
Brown JE, Thomson CS, Ellis SP et al (2003) Bone resorption predicts for skeletal complications in metastatic bone disease. Br J Cancer 89(11):2031–2037
Ali SM, Demers LM, Leitzel K et al (2004) Baseline serum NTx levels are prognostic in metastatic breast cancer patients with bone-only metastasis. Ann Oncol 15(3):455–459
Brown JE, Cook RJ, Major P et al (2005) Bone turnover markers as predictors of skeletal complications in prostate cancer, lung cancer, and other solid tumors. J Natl Cancer Inst 97(1):59–69
Cook RJ, Coleman R, Brown J et al (2006) Markers of bone metabolism and survival in men with hormone-refractory metastatic prostate cancer. Clin Cancer Res 12(11 Pt 1):3361–3367
Seibel MJ (2005) Clinical use of markers of bone turnover in metastatic bone disease. Nat Clin Pract Oncol 2(10):504–517; quiz 501p following 533
Mundy GR (2002) Metastasis to bone: causes, consequences and therapeutic opportunities. Nat Rev Cancer 2(8):584–593
Morony S, Capparelli C, Sarosi I et al (2001) Osteoprotegerin inhibits osteolysis and decreases skeletal tumor burden in syngeneic and nude mouse models of experimental bone metastasis. Cancer Res 61(11):4432–4436
Hiraga T, Williams PJ, Mundy GR et al (2001) The bisphosphonate ibandronate promotes apoptosis in MDA-MB-231 human breast cancer cells in bone metastases. Cancer Res 61(11):4418–4424
Neudert M, Fischer C, Krempien B et al (2003) Site-specific human breast cancer (MDA-MB-231) metastases in nude rats: model characterisation and in vivo effects of ibandronate on tumour growth. Int J Cancer 107(3):468–477
Zheng Y, Zhou H, Brennan K et al (2007) Inhibition of bone resorption, rather than direct cytotoxicity, mediates the anti-tumour actions of ibandronate and osteoprotegerin in a murine model of breast cancer bone metastasis. Bone 40(2):471–478
Clines GA, Guise TA (2005) Hypercalcaemia of malignancy and basic research on mechanisms responsible for osteolytic and osteoblastic metastasis to bone. Endocr Relat Cancer 12(3):549–583
Lee Y-P, Schwarz EM, Davies M et al (2002) Use of zoledronate to treat osteoblastic versus osteolytic lesions in a severe-combined-immunodeficient mouse model. Cancer Res 62(19):5564–5570
Guise TA (2000) Molecular mechanisms of osteolytic bone metastases. Cancer 88(12 Suppl):2892–2898
Zhang J, Dai J, Qi Y et al (2001) Osteoprotegerin inhibits prostate cancer-induced osteoclastogenesis and prevents prostate tumor growth in the bone. J Clin Invest 107(10):1235–1244
Yi B, Williams PJ, Niewolna M et al (2002) Tumor-derived platelet-derived growth factor-BB plays a critical role in osteosclerotic bone metastasis in an animal model of human breast cancer. Cancer Res 62(3):917–923
Kitazawa S, Kitazawa R (2002) RANK ligand is a prerequisite for cancer-associated osteolytic lesions. J Pathol 198(2):228–236
Zheng Y, Zhou H, Modzelewski JR et al (2007) Accelerated bone resorption, due to dietary calcium deficiency, promotes breast cancer tumor growth in bone. Cancer Res 67(19):9542–9548
van der Pluijm G, Que I, Sijmons B et al (2005) Interference with the microenvironmental support impairs the de novo formation of bone metastases in vivo. Cancer Res 65(17):7682–7690
Hirbe AC, Uluckan O, Morgan EA et al (2007) Granulocyte colony-stimulating factor enhances bone tumor growth in mice in an osteoclast-dependent manner. Blood 109(8):3424–3431
Price JT, Quinn JM, Sims NA et al (2005) The heat shock protein 90 inhibitor, 17-allylamino-17-demethoxygeldanamycin, enhances osteoclast formation and potentiates bone metastasis of a human breast cancer cell line. Cancer Res 65(11):4929–4938
Libouban H, Moreau MF, Basle MF et al (2003) Increased bone remodeling due to ovariectomy dramatically increases tumoral growth in the 5T2 multiple myeloma mouse model. Bone 33(3):283–292
Guise TA, Mohammad KS, Clines G et al (2006) Basic mechanisms responsible for osteolytic and osteoblastic bone metastases. Clin Cancer Res 12(20):6213s–6216
Guise TA, Mundy GR (1998) Cancer and bone. Endocr Rev 19(1):18–54
Kiefer JA, Vessella RL, Quinn JE et al (2004) The effect of osteoprotegerin administration on the intra-tibial growth of the osteoblastic LuCaP 23.1 prostate cancer xenograft. Clin Exp Metastasis 21(5):381–387
Parfitt AM (2000) The mechanism of coupling: a role for the vasculature. Bone 26(4):319–323
Yin JJ, Mohammad KS, Kakonen SM et al (2003) From the cover: a causal role for endothelin-1 in the pathogenesis of osteoblastic bone metastases. PNAS 100(19):10954–10959
Schwaninger R, Rentsch CA, Wetterwald A et al (2007) Lack of Noggin Expression by Cancer Cells Is a Determinant of the Osteoblast Response in Bone Metastases. Am J Pathol 170(1):160–175
Hall CL, Kang S, MacDougald OA et al (2006) Role of Wnts in prostate cancer bone metastases. J Cell Biochem 97(4):661–672
Hall CL, Keller ET (2006) The role of Wnts in bone metastases. Cancer Metastasis Rev 25(4):551–558
Pecherstorfer M, Seibel MJ, Woitge HW et al (1997) Bone resorption in multiple myeloma and in monoclonal gammopathy of undetermined significance: quantification by urinary pyridinium cross-links of collagen. Blood 90(9):3743–3750
Woitge HW, Pecherstorfer M, Horn E et al (2001) Serum bone sialoprotein as a marker of tumour burden and neoplastic bone involvement and as a prognostic factor in multiple myeloma. Br J Cancer 84(3):344–351
Chapuy MC, Arlot ME, Duboeuf F et al (1992) Vitamin D3 and calcium to prevent hip fractures in the elderly women. N Engl J Med 327(23):1637–1642
McKane WR, Khosla S, Egan KS et al (1996) Role of calcium intake in modulating age-related increases in parathyroid function and bone resorption. J Clin Endocrinol Metab 81(5):1699–1703
Saleh F, Jorde R, Sundsfjord J et al (2006) Causes of secondary hyperparathyroidism in a healthy population: the Tromso study. J Bone Miner Metab 24(1):58–64
McKenna MJ, Freaney R (1998) Secondary hyperparathyroidism in the elderly: means to defining hypovitaminosis D. Osteoporos Int 8(Suppl 2):S3–6
Lips P (2001) Vitamin D deficiency and secondary hyperparathyroidism in the elderly: consequences for bone loss and fractures and therapeutic implications. Endocr Rev 22(4):477–501
Harris SS, Soteriades E, Dawson-Hughes B (2001) Secondary hyperparathyroidism and bone turnover in elderly blacks and whites. J Clin Endocrinol Metab 86(8):3801–3804
Giusti A, Barone A, Razzano M et al (2006) High prevalence of secondary hyperparathyroidism due to hypovitaminosis D in hospitalized elderly with and without hip fracture. J Endocrinol Invest 29(9):809–813
Horsman A, Jones M, Francis R et al (1983) The effect of estrogen dose on postmenopausal bone loss. N Engl J Med 309(23):1405–1407
Ferlay J, Autier P, Boniol M, et al (2007) Estimates of the cancer incidence and mortality in Europe in 2006. Ann Oncol
Deapen D, Liu L, Perkins C et al (2002) Rapidly rising breast cancer incidence rates among Asian-American women. Int J Cancer 99(5):747–750
Acknowledgments
This study was supported by the National Health and Medical Research Council of Australia (NHMRC project grant # 352332) and by the New South Wales Government (BioFirst Award). Osteoprotegerin was provided by Amgen Inc, California.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zheng, Y., Zhou, H., Fong-Yee, C. et al. Bone resorption increases tumour growth in a mouse model of osteosclerotic breast cancer metastasis. Clin Exp Metastasis 25, 559–567 (2008). https://doi.org/10.1007/s10585-008-9172-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10585-008-9172-4