Abstract
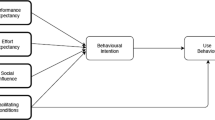
Medication errors are major safety concerns in all hospital settings. The insufficient knowledge about managerial and process improvement strategies required to reduce medication errors can be considered as one of the most important factors holding back hospitals from achieving the desired goals for patient safety. However, strategies for medication error reduction cannot be successfully implemented without a clear understanding of factors affecting medication delivery errors. This paper presents a study in which healthcare professionals’ perceptions on three factors, namely (1) technical complexity of tasks/connections; (2) resources problems; and (3) qualification of human resources, are analyzed within the medication delivery system at one community hospital. The outcomes of this research are a theoretical model for reducing medication delivery errors and a set of workflow design rules for healthcare professionals to continuously reduce medication delivery errors.



Similar content being viewed by others
References
Institute of Medicine Preventing Medication Errors. Institute of Medicine Report, Washington, D.C., 2006
Weingart S, Page D (2004) Implications for practice: challenges for healthcare leaders in fostering patient safety. Qual Saf Health Care 13:ii52–ii56
Ramanujam R, Rousseau D (2006) The challenges are organizational, not just clinical. J Organ Behav 27:811–827 doi:10.1002/job.411
Perrow C (1984) Normal accidents: Living with high-risk technologies. Princeton University Press, Princeton
Tucker A, Edmondson A (2002) Managing routine exception: a model of nurse problem solving behavior. Adv Healthc Manage 3:87–113
Tucker A, Edmondson C (2003) Why hospitals don’t learn from failures: organizational and psychological dynamics that inhibit system change. Calif Manage Rev 45:55–72
Tucker A (2004) The impact of operational failures on hospital nurses and their patients. J Oper Manage 22:151–169 doi:10.1016/j.jom.2003.12.006
Thompson D, Wolf G, Spear S (2003) Driving improvement in patient care. J Nurs Adm 33:585–595 doi:10.1097/00005110-200311000-00008
Patel V, Branch T, Arocha J (2002) Errors in interpreting quantities as procedures: the case of pharmaceutical label. Int J Med Inform 65:193–211 doi:10.1016/S1386-5056(02)00045-X
Uhlig P (2001) Improving patient care in hospital. J Innovative Manage 7:23–45
Spear S, Bowen H (1999) Decoding the DNA of the Toyota Production System. Harv Bus Rev 77:97–106
Shingo S (1989) A study of the toyota production system from an industrial engineering viewpoint. Productivity, Portland
Womack JP, Jones DT (1996) Lean Thinking. Simon and Schuster, New York
Sobek D, Jimmerson C (2003) Applying the Toyota Production System to a hospital pharmacy. Paper presented at the Industrial Engineering Research Conference, Portland, Oregon
Sobek D, Jimmerson C (2004) A3 reports: Tool for process improvement. Paper presented in the Industrial Engineering Research Conference, Houston, Texas
Jimmerson C, Weber D, Sobek D (2005) Reducing waste and errors: piloting lean principles at IHC. Jt Comm J Qual Saf 31:249–257
Spear S (2005) Fixing healthcare from the inside, today. Harv Bus Rev 83:78–91
Mazur L, Chen S (2007) Improving medication delivery using systems engineering approach. Proceedings of Industrial Engineering Research Conference, Nashville
Mazur L, Chen S (2008) Understanding and reducing waste due to medication errors via systems mapping and analysis. Health Care Manage Sci 11:55–65 doi:10.1007/s10729-007-9024-9
DeWalt K, DeWalt B (2002) Participant observation. AltaMira, Walnut Creek
Strauss A, Corbin J (1998) Basics of qualitative research: techniques and procedures for developing grounded theory. Sage, Newbury Park
Uribe CL, Schweikhart SB, Pathak DS, Dow M, Marsh GB (2002) Perceived barriers to medication error reporting: an explanatory investigation. J Healthc Manag 47:263–280
Joint Commission (2007) National Patient Safety Goals. Retrieved on May 28, 2007
Slavitt D, Stamps P, Piedmont E, Haase A (1978) Nurses’ satisfaction with their work situation. Nurs Res 27:114–120 doi:10.1097/00006199-197803000-00018
Aiken L, Patrician P (2000) Measuring organizational traits of hospitals: the revised nursing work index. Nurs Res 49:146–153 doi:10.1097/00006199-200005000-00006
Havens D, Aiken L (1999) Shaping systems to promote desired outcomes. J Nurs Adm 29:14–20 doi:10.1097/00005110-199902000-00006
Hackman J (1987) The design of work teams. In: Lorsch J (ed) Handbook of organizational behavior. Prentice-Hall, Englewood Cliffs
Roberts K (1990) Some characteristics of high reliability organizations. Organ Sci 1:160–177
Roberts K, Bea R (2001) Must accidents happen? Lessons from high reliability organizations. Acad Manag Exec 15:70–79
Reason J (2004) Beyond the organizational accident: the need for ‘error wisdom’ on the frontline. Qual Saf Health Care 13:28–33 doi:10.1136/qshc.2003.009548
Tucker A, Spear S (2006) Operational failures and interruptions in hospital nursing. Health Serv Res 41:643–662 doi:10.1111/j.1475-6773.2006.00502.x
Anderson J, Ramanujam R, Hensel D, Anderson M, Sirio C (2006) The need for organizational change in patient safety. Int J Med Inform 75:809–817 doi:10.1016/j.ijmedinf.2006.05.043
Haberstroh C (1965) Organization, Design and Systems Analysis in Handbook of Organizations. Rand McNally, Chicago
Burke T, McKee J, Wilson H, Donahue R, Batenhorst A, Pathak D (2000) A comparison of time-and-motion and self-reporting methods of work measurement. J Nurs Adm 30:118–125 doi:10.1097/00005110-200003000-00003
Miles M, Huberman A (1994) Qualitative data analysis: an expanded sourcebook. Sage, Thousand Oaks
Redelmeier DA (2005) Improving patient care. The cognitive psychology of missed diagnoses. Ann Intern Med 142:115–120
Croskerry P (2003) Cognitive forcing strategies in clinical decision-making. Ann Emerg Med 41:110–120 doi:10.1067/mem.2003.22
Croskerry P (2003) The importance of cognitive errors in diagnosis and strategies to minimize them. Acad Med 78:775–780 doi:10.1097/00001888-200308000-00003
Gilovich T, Medvec VH, Savitsky K (2000) The spotlight effect in social judgment: an egocentric bias in estimates of the salience of one’s own actions and appearance. J Pers Soc Psychol 78:211–222 doi:10.1037/0022-3514.78.2.211
Jones E, Nisbett R (1985) Sex of employee and sex of supervisor: effect on attributions for the causality of success and failure. Sex Roles J Res 12:257–269 doi:10.1007/BF00287592
Weary G, Edwards J (1994) Individual differences in causal uncertainty. J Pers Soc Psychol 67:308–318 doi:10.1037/0022-3514.67.2.308
Science Applications International Corporation: Probabilistic risk assessment of the space shuttle. NASA/HQ, 28 February, 1995
Fragola J (1996) Space shuttle probabilistic risk assessment. Proceedings Annual Reliability and Maintainability Symposium
Marx DA, Slonim AD (2003) Assessing patient safety risk before the injury occurs: an introduction to sociotechnical probabilistic risk modeling in health care. Qual Saf Health Care 12:33–38 doi:10.1136/qhc.12.suppl_2.ii33
Kanki BG, Marx D, Hale MJ (2004) Socio-technical probabilistic risk assessment: its capabilities and limitations. Proceedings of International Conference on Probabilistic Safety Assessment and Management. Berlin, Germany
Hovor C, O’Donnell LT (2007) Probabilistic risk analysis of medication error. Qual Manag Health Care 16:349–253
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mazur, L.M., Chen, SJ.(. An empirical study for medication delivery improvement based on healthcare professionals’ perceptions of medication delivery system. Health Care Manag Sci 12, 56–66 (2009). https://doi.org/10.1007/s10729-008-9076-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10729-008-9076-5