Abstract
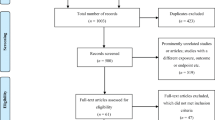
Aim of the review In low and middle income countries private pharmacies are considered a valuable resource for health advice and medicines in many communities. However the quality of the service they provide has often been questioned and is unclear. This paper reviews the evidence regarding the quality of professional services from private pharmacies in low and middle-income countries. Method A literature search (computer and hand searches) was undertaken to identify all studies which included an assessment of the quality of some aspect of private pharmacy services in low and middle income countries. Results 30 studies were identified which spanned all regions in the developing world. These included 9 which examined the scope and/or quality of a range of professional services, 14 which assessed the quality of advice provided in response to specific symptoms and 7 which investigated the supply of medicines without a prescription. A range of methods were employed, in particular, questionnaire surveys with staff and/or clients and assessment of practice using simulated client methodology. Whilst many authors identified a potential for pharmacies to contribute more effectively to primary health care, virtually all studies identified deficiencies in the quality of current professional practice. In particular authors highlighted the lack of presence of pharmacists or other trained personnel, the provision of advice for common symptoms which was not in accordance with guidelines and the inappropriate supply of medicines. Conclusion The evidence-base regarding the quality of professional services from pharmacies in low and middle income countries is limited, but indicates that standards are often deficient. If pharmacists are to contribute effectively to health care, the barriers to the provision of higher quality care and ways in which these might be overcome must be identified and examined.
Similar content being viewed by others
References
World Health Organisation. The role of the pharmacist in the health care system. Geneva: WHO; 1994. Available at: http://whqlibdoc.who.int/hq/1994/WHO_PHARM_94.569.pdf. Accessed 25 Feb 2009.
World Health Organisation. Good Pharmacy Practice. Guidelines in community and hospital settings. Geneva: WHO; 1996. Available at: http://whqlibdoc.who.int/hq/1996/WHO_PHARM_DAP_96.1.pdf. Accessed 25 Feb 2009.
FIP. Standards for quality of pharmacy services. International Pharmaceutical Federation; 1993. Available at http://www.fip.ul/www/uploads/?page=statements. Accessed 25 Feb 2009.
World Health Organisation. The role of the pharmacist in self-care and self-medication. Geneva: WHO; 1998. Available at: http://whqlibdoc.who.int/hq/1998/WHO_DAP_98.13.pdf. Accessed 25 Feb 2009.
Owusu-Daaku FTK. Pharmacy in Ghana’s health care system: which way forward? Ghana Pharm J. 2002;25:20–3.
Smith FJ. Community pharmacy in Ghana: enhancing the contribution to primary health care. Health Policy Plan. 2004;19:234–41. doi:10.1093/heapol/czh028.
Kumari RP, Raman R, Sharma T. Physicians, pharmacists, and people with diabetes in India. Pharm World Sci. 2008;30:750–2. doi:10.1007/s11096-008-9225-4.
Yousef AMM, Al-Bakri AG, Bustanji Y, Wazaify M. Self-medication practices in Jordan. Pharm World Sci. 2008;30:24–30. doi:10.1007/s11096-007-9135-x.
World Health Organisation. The essential medicines concept: from its beginning until today. Geneva: WHO; 2004. Available at http://whqlibdoc.who.int/hq/1994/WHO_EDM_2004.3.pdf. Accessed 25 Feb 2009.
UN Millenium Project. Prescription for healthy development: access to essential medicines. London: Earthscan; 2005. ISBN 1 84407 227-4.
Van der Geest S. The illegal distribution of Western Medicines in developing countries. Med Anthropol. 1982;6:197–219.
Van der Geest S. Pharmaceuticals in the third world: the local perspective. Soc Sci Med. 1987;25:273–6. doi:10.1016/0277-9536(87)90230-9.
Fabricant SJ, Hirschhorn N. Deranged distribution, perverse prescription, unprotected use: irrationality of pharmaceuticals in the developing world. Health Policy Plan. 1987;2:204–13. doi:10.1093/heapol/2.3.204.
Le Grand A, Hogerzeil HV, Haaijer-Ruskamp FM. Interventional research in rational use of drugs: a review. Health Policy Plan. 1999;14:89–102. doi:10.1093/heapol/14.2.89.
Preux PM, Tiemagni F, Fodzo L, Kandem P, Ngouafong P, Ndonko F, et al. Antiepileptic therapies in the Mifi province in Cameroon. Epilepsia. 2000;41:432–9. doi:10.1111/j.1528-1157.2000.tb00185.x.
Smith FJ. Pharmacy in developing countries. In: Harding G, Taylor K, editors. Pharmacy practice: chapter 6. Amsterdam: Harwood Academic Publishers; 2001. ISBN 0 415 27159 2.
Goodman C, Brieger W, Unwin A, Mills A, Meek S, Greer G. Medicine sellers and malaria treatment in sub-Saharan Africa: what do they do and how can their practice be improved? Am J Trop Med Hyg. 2007;77(supplement):213–8.
Buabeng KO, Duwiejua M, Matowe LK, Smith F, Enlund H. Availability and choice of anti-malarials at medicine outlets in Ghana: the question of access to effective medicines for malaria control. Clin Pharmacol Ther. 2008;84:613–9. doi:10.1038/clpt.2008.130.
Holloway K. Promoting rational use of medicines. International Network for the Rational Use of Drugs. INRUD News, July 2008. Available at: http://www.inrud.org/documents/upload/vol16no1.pdf Accessed 25 Feb 2009.
World Health Organisation. The World health report 2006: working together for health. Geneva: WHO; 2006. ISBN: 92 4 156 317 6.
Wuliji T. Global pharmacy workforce and migration report: a call for action. Int Pharm J. 2006;20:2–4.
DFID. Priority countries. London: Department for International Development; 2008. Available at: http://www.dfid.gov.uk/africa. Accessed 25 Feb 2009.
Oparah AC, Arigbe-Osula EM. Evaluation of community pharmacists’ involvement in primary health care. Trop J Pharm Res. 2002;1:67–74.
Oparah CA, Enato EFO, Odili UV, Aghomo OE. Activities of community pharmacy counter staff in Benin City, Nigeria. J Soc Adm Pharm. 2002;19:141–4.
Benjamin H, Motawi A, Smith F. Community pharmacists in primary health care in Alexandria. J Soc Adm Pharm. 1995;12:3–11.
Anyama N, Adome RO. Community pharmaceutical care: an 8-month critical review of two pharmacies in Kampala. Afr Health Sci. 2003;3:87–93.
Chuc NTK, Tomson G. ‘Doi moi’ and private pharmacies: a case study on dispensing and financial issues in Hanoi, Vietnam. Eur J Clin Pharmacol. 1999;55:325–32. doi:10.1007/s002280050636.
Stenson B, Syhakhang L, Eriksson B, Tomson G. Real world pharmacy: assessing the quality of private pharmacy practice in the Lao People’s Democratic Republic. Soc Sci Med. 2001;52:393–404. doi:10.1016/S0277-9536(00)00142-8.
Syhakhang L, Stenson B, Wahlstrom R, Tomson G. The quality of public and private pharmacy practices: a cross-sectional study in the Savannakhet province, Lao PDR. Eur J Clin Pharmacol. 2001;57:221–7. doi:10.1007/s002280100295.
Basak SC, Arunkumar A, Masilamani K. Community pharmacists’ attitudes towards use of medicines in rural India. International Pharmacy Journal 2002; 32–5.
Abula T, Worku A, Thomas K. Assessment of the dispensing practices of drug retail outlets in selected towns, North West Ethiopia. Ethiop Med J. 2006;44:145–50.
Duong DV, Binns CW, Le TV. Availability of antibiotics as over-the-counter drugs in pharmacies: a threat to public health in Vietnam. Trop Med Int Health. 1997;2:1133–9. doi:10.1046/j.1365-3156.1997.d01-213.x.
Wachter DA, Joshi MP, Rimal B. Antibiotic dispensing by drug retailers in Kathmandu, Nepal. Trop Med Int Health. 1999;4:782–8. doi:10.1046/j.1365-3156.1999.00476.x.
Oladipo OB, Lamikanra A. Patterns of antibiotic purchases in community pharmacies in South Western, Nigeria. J Soc Adm Pharm. 2002;19:33–8.
Volpato DE, de Souza BV, Rosa LGD, Melo LH, Daudt CAS, Deboni L. Braz J Infect Dis. 2005;3:288–91.
Nyazema N, Viberg N, Khoza S, Vyas S, Kumaranayake L, Tomson G, et al. Low sales of antibiotics without a prescription: a cross-sectional study in Zimbabwean private pharmacies. J Antimicrob Chemother. 2007;59:718–26. doi:10.1093/jac/dkm013.
Apisarnthanarak A, Tunpornchai J, Tanawitt K, Mundy LM. Nonjudicious dispensing of antibiotics by drug stores in Pratumthani, Thailand. Infect Control Hosp Epidemiol. 2008;29:572–5. doi:10.1086/587496.
Mac TL, Le VT, Vu AN, Preux PM, Ratsimbazafy V. AEDs availability and professional practices in delivery outlets in a city centre in Vietnam. Epilepsia. 2006;47:300–4. doi:10.1111/j.1528-1167.2006.00425.x.
Mayhew S, Nzambi K, Pepin J, Adjei S. Pharmacists’ role in managing sexually transmitted infections: policy issues and options for Ghana. Health Policy Plan. 2001;16:152–60. doi:10.1093/heapol/16.2.152.
Chalker J, Chuc NTK, Falkenberg T, Do NT, Tomson G. STD management by private pharmacies in Hanoi: practice and knowledge of drug sellers. Sex Transm Infect. 2000;76:299–302. doi:10.1136/sti.76.4.299.
Leiva A, Shaw M, Paine K, Manneh K, McAdam K, Mayaud P. Management of sexually transmitted disease in urban pharmacies in The Gambia. Int J STD AIDS. 2001;12:442–52. doi:10.1258/0956462011923471.
Ramos MC, da Silva RDC, Gobbato RO, da Rocha FC, de Lucca G, Vossky J, et al. Pharmacy clerks’ prescribing practices for STD patients in Porto Alegre, Brazil. Int J STD AIDS. 2004;15:333–6. doi:10.1258/095646204323012832.
Turner AN, Ellertson C, Thomas S, Garcia S. Diagnosis and treatment if presumed STIs at Mexican pharmacies: survey results from a random sample of Mexico City pharmacy attendants. Sex Transm Infect. 2003;79:224–8. doi:10.1136/sti.79.3.224.
Erhun WO. Management of sexually transmitted diseases in retail drug outlets in Nigeria. J Soc Adm Pharm. 2002;19:145–50.
Van Duong D, Le TV, Binns CW. Diarrhoea management by pharmacy staff in retail pharmacies in Hanoi Vietnam. Int J Pharm Pract. 1997;5:97–100.
Benjamin Sokar-Todd H, Smith FJ. Management of diarrhoea at community pharmacies in Alexandria, Egypt. J Soc Adm Pharm. 2003;20(1):32–8.
Igun UA. Reported and actual prescription of oral rehydration therapy for childhood diarrhoeas by retail pharmacists in Nigeria. Soc Sci Med. 1994;39:797–806. doi:10.1016/0277-9536(94)90041-8.
Tumwikirize WA, Ekwaru PJ, Mohammed K, Ogwal-Okeng JW, Aupont O. Management of acute respiratory infections in drug shops and private pharmacies in Uganda: a study of counter-attendants’ knowledge and reported behaviour. East Afr Med J. 2004;81(supplement):S33–40.
Chuc NT, Larsson M, Falkenburg T, Do NT, Binh NT, Tomson GB. Management of childhood infections at private pharmacies in Vietnam. Ann Pharmacother. 2001;35:1283–8. doi:10.1345/aph.10313.
Rajeswari R, Balasubramanian R, Bose SC, Rahman SF. Private pharmacies in tuberculosis control: a neglected link. Int J Tuberc Lung Dis. 2002;6:171–3.
Lonnroth K, Lambregts K, Nhien DTT, Quy HT, Diwan VK. Private pharmacies and tuberculosis control: a survey of case detection skills and reported anti-tuberculosis drug dispensing in private pharmacies in Ho Chi Minh City, Vietnam. Int J Tuberc Lung Dis. 2000;4:1052–9.
Van Sickle D. Management of asthma at private pharmacies in India. Int J Tuberc Lung Dis. 2006;10:1386–92.
Madden JM, Quick JD, Ross-Degnan D, Kafle KK. Undercover care-seekers: simulated clients in the study of health provider behaviour in developing countries. Soc Sci Med. 1997;45:1465–82. doi:10.1016/S0277-9536(97)00076-2.
Watson MC, Norris P, Granas AG. A systematic review of the use of simulated patients and pharmacy practice research. Int J Pharm Pract. 2006;14:83–93. doi:10.1211/ijpp.14.2.0002.
Cerderlof C, Tomson G. Private pharmacies and health sector reform in developing countries—professional and commercial highlights. J Soc Adm Pharm. 1995;12:101–11.
Gastelurrutia MA, Benrimoj SIC, Castrillon CC, Casado de Amezua MJ, Fernandez-Llimos F, Faus MJ. Facilitators for practice change in Spanish community pharmacy. Pharm World Sci. 2009;31:32–9.
Babar ZUD, Jamshed S. Social Pharmacy strengthening clinical pharmacy: why pharmaceutical policy research is needed in Pakistan. Pharm World Sci. 2008;30:617–9. doi:10.1007/s11096-008-9246-z.
Benjamin H, Smith FJ, Motawi A. Drugs supplied, with and without a prescription from a conurbation in Egypt. East Mediterr Health J. 1996;2:506–14.
Acknowledgement
I would like to thank Joann Hong for her assistance in the literature searching and data extraction for this review.
Funding
No external sources of funding for this work were obtained.
Conflicts of interest
There are no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Smith, F. The quality of private pharmacy services in low and middle-income countries: A systematic review. Pharm World Sci 31, 351–361 (2009). https://doi.org/10.1007/s11096-009-9294-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11096-009-9294-z