Abstract
BACKGROUND
Low health literacy (HL) is an important risk factor for cancer health disparities.
OBJECTIVE
Describe a continuing medical education (CME) program to teach primary care physicians (PCP) cancer risk communication and shared decision-making (SDM) with low HL patients and baseline skills assessment.
DESIGN
Cluster randomized controlled trial in five primary care clinics in New Orleans, LA.
PARTICIPANTS
Eighteen PCPs and 73 low HL patients overdue for cancer screening.
INTERVENTION
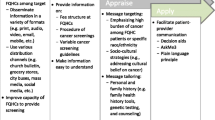
Primary care physicians completed unannounced standardized patient (SP) encounters at baseline. Intervention physicians received SP verbal feedback; academic detailing to review cancer screening guidelines, red flags for identifying low HL, and strategies for effective counseling; and web-based tutorial of SP comments and checklist items hyperlinked to reference articles/websites.
MAIN MEASURES
Baseline PCP self-rated proficiency, SP ratings of physician general cancer risk communication and SDM skills, patient perceived involvement in care.
RESULTS
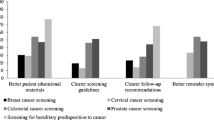
Baseline assessments show physicians rated their proficiency in discussing cancer risks and eliciting patient preference for treatment/decision-making as “very good”. SPs rated physician exploration of perceived cancer susceptibility, screening barriers/motivators, checking understanding, explaining screening options and associated risks/benefits, and eliciting preferences for screening as “satisfactory”. Clinic patients rated their doctor’s facilitation of involvement in care and information exchange as “good”. However, they rated their participation in decision-making as “poor”.
DISCUSSION
The baseline skills assessment suggests a need for physician training in cancer risk communication and shared decision making for patients with low HL. We are determining the effectiveness of teaching methods, required resources and long-term feasibility for a CME program.
Similar content being viewed by others
References
Selden C, Zorn M, Ratzan SC, Parker RM, compilers. Current Bibliographies in Medicine: Health literacy. Bethesda, MD: National Library of Medicine; 2000. Available from: http://www.nlm.nih.gov/pubs/cbm/hliteracy.html Accessed November 1, 2009.
DeWalt DA, Berkman ND, Sheridan S, Lohr KN, Pignone M. Literacy and health outcomes: a systematic review of the literature. J Gen Intern Med. 2004;19:1228–39.
Davis TC, Williams MV, Marin E, Parker RM, Glass J. Health literacy and cancer communication. CA Cancer J Clin. 2002;52:134–49.
Katz MG, Jacobson TA, Veledar E, Kripalani S. Patient literacy and question-asking behavior during the medical encounter: a mixed-methods analysis. J Gen Intern Med. 2007;22:782–6.
Sheridan SL, Harris RP, Woolf SH. Shared decision making about screening and chemoprevention. A suggested approach from the U.S. Preventive Services Task Force. Am J Prev Med. 2004;26:56–66.
Mika VS, Kelly PJ, Price MA, Franquiz M, Villarreal R. The ABCs of health literacy. Fam Commun Health. 2005;28:351–7.
Davis TC, Crouch MA, Long SW, et al. Rapid assessment of literacy levels of adult primary care patients. Fam Med. 1991;23:433–5.
Smith RA, Cokkinides V, Brawley OW. Cancer screening in the United States, 2008: a review of current American Cancer Society guidelines and cancer screening issues. CA Cancer J Clin. 2008;58:161–79.
Stretcher VJ, Rosenstock JM. The Health Belief Model. Health Behavior and Health Education. San Francisco: Jossey-Bass; 1997:41–59.
WebSP. Available at http://websp.tulane.edu. Accessed November 1, 2009.
Charles C, Gafni A, Whelan T. Decision-making in the physician-patient encounter: revisiting the shared treatment decision-making model. Soc Sci Med. 1999;49:651–61.
Braddock CH III, Edwards KA, Hasenberg NM, Laidley TL, Levinson W. Informed decision making in outpatient practice: time to get back to basics. JAMA. 1999;282:2313–20.
US Department of Health and Human Services. Plain language: a promising strategy for clearly communicating health information and and improving health literacy. Available at http://www.health.gov/communication/literacy/plainlanguage/IssueBrief.pdf. Accessed November 1, 2009.
Glanz K, Rimer BK. Theory at a Glance: Guide for Health Promotion Practice, 2nd edn. National Cancer Institute, 2005. NIH Pub. No. 05–3896. Available at http://www.cancer.gov/PDF/481f5d53–63df-41bc-bfaf-5aa48ee1da4d/TAAG3.pdf. Accessed November 1, 2009.
Epstein RM, Street RL. Framework for patient-centered communication in cancer care. Available at http://outcomes.cancer.gov/areas/pcc/communication/pccm_ch2.pdf. Accessed November 1, 2009.
National Cancer Institute. Cancer prevention. Available at http://www.cancer.gov/cancertopics/prevention-genetics-causes/prevention. Accessed November 1, 2009.
Lerman CE, Brody DS, Caputo GC, Smith DG, Lazaro CG, Wolfson HG. Patients' perceived involvement in care scale: relationship to attitudes about illness and medical care. J Gen Intern Med. 1990: 5(1):29–33.
Schillinger D, Piette J, Grumbach K, et al. Closing the loop: physician communication with diabetic patients who have low health literacy. Arch Intern Med. 2003;163:83–90.
Davis DA, Mazmanian PE, Fordis M, Harrison RV, Thorpe KE, Perrier L. Accuracy of physician self-assessment compared to observed measures of competence. JAMA. 2006;296:1094–102.
Frank P, Friscella K, Shiedls CG, Meldrum SC, Duberstein P, Jerant AF, et al. Are patient ratings of their physicians related to health outcomes? Ann Fam Med. 2005;3:229–34.
Peabody JW, Luck J, Glassman P, Dresselhaus TR, Lee M. Comparison of vignettes, standardized patients, and chart abstraction: a prospective validation study of 3 methods for measuring quality. JAMA. 2000;283:1715–22.
Srinivasan M, Franks P, Meredith LS, Fiscella K, Epstein RM, Kravitz RL. Connoisseurs of care? Unannounced standardized patients' ratings of physicians. Med Care. 2006;44:1092–8.
Acknowledgement
Dr. Price-Haywood is Robert Wood Johnson Foundation Harold Amos Faculty Development Program Scholar. The study sponsor has no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; and preparation, review, or approval of the manuscript. Dr. Price-Haywood and Katherine Roth had full access to all of the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. Dr. Cooper is supported by a grant from the National Heart, Lung, and Blood Institute (K24HL083113). The authors wish to acknowledge Karen B DeSalvo, MD, MPH, MSc for providing a project coordinator for this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Price-Haywood, E.G., Roth, K.G., Shelby, K. et al. Cancer Risk Communication with Low Health Literacy Patients: A Continuing Medical Education Program. J GEN INTERN MED 25 (Suppl 2), 126–129 (2010). https://doi.org/10.1007/s11606-009-1211-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-009-1211-6