Opinion statement
-
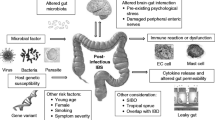
Postinfectious irritable bowel syndrome (PI-IBS) should be considered in patients who present with a change in bowel habits or an onset of new abdominal pain or discomfort following a recent confirmed or presumed exposure to infectious organisms, or in those who have recently returned from a tropical or developing country.
-
In patients who are greatly distressed by their symptoms, an extended workup early in the course of their illness may give physician and patient confidence in focusing on IBS.
-
The author favors a proactive, multicomponent approach to management, as it gives the physician and patient a sense of control.
-
Treatment should include stress management, dietary advice to minimize exposure to trigger foods, and pharmacotherapy to alleviate anxiety and target disturbed physiology.
Similar content being viewed by others
References and Recommended Reading
Hurst A: Medical Diseases of War, edn 3. London: Arnold; 1943.
Stewart GT: Post-dysenteric colitis. BMJ 1950, 1:405–409.
Chaudhary NA, Truelove SC: The irritable colon. Q J Med 1962, 31:307–322.
Gwee KA, Graham JC, McKendrick MW, et al.: Psychometric scores and persistence of irritable bowel after infectious diarrhoea. Lancet 1996, 347:150–153.
Rodriguez LAG, Ruigomez A: Increased risk of irritable bowel syndrome after bacterial gastroenteritis: cohort study. BMJ 1999, 318:565–566. This study estimates that compared with the general population, the risk of IBS is increased 10-fold after gastroenteritis, and establishing it as a major risk factor for IBS.
Pan G, Lu S, Ke M, et al.: Epidemiologic study of the irritable bowel syndrome in Beijing: stratified randomized study by cluster sampling. Chung Hua I Hsueh Tsa Chih 2000, 113:35–39.
McKendrick MW, Read NW: Irritable bowel syndrome—post Salmonella infection. J Infection 1994, 29:1–3.
Neal KR, Hebden J, Spiller R: Prevalence of gastrointestinal symptoms six months after bacterial gastroenteritis and risk factors for development of the irritable bowel syndrome: postal survey of patients. BMJ 1997, 314:779–782.
Nanda R, Baveja U, Anand BS: Entamoeba histolytica cyst passers: clinical features and outcome in untreated subjects. Lancet 1984, 2:301–303.
Hussain R, Jaferi W, Zuberi S, et al.: Significantly increased IgG2 subclass antibody levels to Blastocystis hominis in patients with irritable bowel syndrome. Am J Trop Med Hyg 1997, 56:301–306.
Giacometti A, Cirioni O, Fiorentini A, et al.: Irritable bowel syndrome in patients with Blastocystis hominis infection. Eur J Clin Microbiol Infect Dis 1999, 18:436–439.
SpillerRC, Jenkins D, Thornley JP, et al.: Increased rectal mucosal enteroendocrine cells, T lymphocytes, and increased gut permeability following acute Campylobacter enteritis and in post-dysenteric irritable bowel syndrome. Gut 2000, 47:804–811. An in-depth analysis of cellular markers of inflammation in the rectal mucosa of patients recovering from gastroenteritis. A persistent increase in inflammatory cells was reported up to 1 year after infection.
Talley NJ, Weaver AL, Zinsmeister AR, et al.: Onset and disappearance of gastrointestinal symptoms and functional gastrointestinal disorders. Am J Epidemiol 1992, 136:1–13.
McKendrick MW: Post Salmonella irritable bowel syndrome—5 year review. J Infection 1996, 32:170–171.
Connell AM, Gaafer M, Hassanein MA, Khayal MA: Motility of pelvic colon III: motility responses in patients with symptoms following amoebic dysentery. Gut 1964, 5:443–447.
Bergin AJ, Donnelly TC, McKendrick MW, Read NW: Changes in anorectal function in persistent bowel disturbance following salmonella gastroenteritis. Eur J Gastroenterol Hepatol 1993, 5:617–620.
GweeKA, Leong YL, Graham C, et al.: The role of psychological and biological factors in postinfective gut dysfunction. Gut 1999, 44:400–406. Prospective study of patients hospitalized with gastroenteritis that makes an intriguing observation that postinfection patients can have rapid colonic transit and rectal sensitivity and not complain of symptoms. Proposes an interactive psychobiologic model to explain PI-IBS.
Niaz SK, Sandrasegaran K, Renny FH, Jones BJM: Postinfective diarrhoea and bile acid malabsorption. J R Coll Physicians Lond 1997, 31:53–56.
Galatola G, and the Italian 75-SeHCAT Multicentre Study Group: The prevalence of bile acid malabsorption in irritable bowel syndrome and the effect of cholestyramine: an uncontrolled open multicentre study. Eur J Gastroenterol Hepatol 1992, 4:533–537.
Ung KA, Kilander AF, Lindgren A, Abrahamsson H: Impact of bile acid malabsorption on steatorrhoea and symptoms in patients with chronic diarrhoea. Eur J Gastroenterol Hepatol 2000, 12:541–547.
Edwards CA, Brown S, Baxter AJ, et al.: Effect of bile acid on anorectal function in man. Gut 1989, 30:383–386.
Ferguson A, MacDonald DM, Brydon WG: Prevalence of lactase deficiency in British adults. Gut 1984, 25:163–167.
Cohen R, Kalser MH, Arteaga I, et al.: Microbial intestinal flora in acute diarrhoeal disease. JAMA 1967, 201:157–162.
Stephen AM, Wiggins HS, Cummings JH: Effect of changing transit time on colonic microbial metabolism in man. Gut 1987, 28:601–609.
King TS, Elia M, Hunter JO: Abnormal colonic fermentation in irritable bowel syndrome. Lancet 1998, 352:1187–1189.
Gue M, Bonbonne C, Fioramonti J, et al.: Stressinduced enhancement of colitis in rats: CRF and arginine vasopressin are not involved. Am J Physiol 1997, 272:G84–91.
Collins SM, McHugh K, Jacobson K, et al.: Previous inflammation alters the response of the rat colon to stress. Gastroenterology 1996, 111:1509–515.
Qiu BS, Vallance BA, Blennerhassett PA, Collins SM: The role of CD4+ lymphocytes in the susceptibility of mice to stress-induced reactivation of experimental colitis. Nat Med 1999, 5:1178–1182.
Thompson WG, Longstreth GF, Drossman DA, et al.: Functional bowel disorders and functional abdominal pain. Gut 1999, 45:II43–47.
Owens DM, Nelson DK, Talley NJ: The irritable bowel syndrome: long-term prognosis and the physicianpatient interaction. Ann Intern Med 1995, 122:107–112.
Drossman DA, Thompson WG: The irritable bowel syndrome: review and a graduated multicomponent treatment approach. Ann Intern Med 1992, 116:1009–1016.
Bolin TD, Davis AE, Duncombe VM: A prospective study of persistent diarrheoa. Aust N Z J Med 1982, 12:22–26.
Sullivan MA, Cohen S, Snape WJ: Colonic myoelectrical activity in irritable bowel syndrome. Effect of eating and anticholinergic. N Engl J Med 1978, 298:878–883.
McHardy G, Sekinger D, Balart L, Cradic HE: Chlordiazepoxide-clidinium bromide in gastrointestinal disorders: controlled clinical studies. Gastroenterology 1968, 54:508–513.
Cann PA, Read NW, Holdsworth CD, et al.: Role of loperamide and placebo in management of irritable bowel syndrome (IBS). Dig Dis Sci 1984, 29:239–247.
Halpern GM, Prindiville T, Blankenburg M, et al.: Treatment of irritable bowel syndrome with Lacteol Fort: a randomized, double-blind, cross-over trial. Am J Gastroenterol 1996, 91:1579–1585.
Prior A, Colgan SM, Whorwell PJ: Changes in rectal sensitivity after hypnotherapy in patients with irritable bowel syndrome. Gut 1990, 31:896–898.
Whorwell PJ, Houghton LA, Taylor EE, Maxton DG: Physiological effects of emotion: assessment via hypnosis. Lancet 1992, 340:69–72.
Whorwell PJ, Prior A, Colgan SM: Hypnotherapy in severe irritable bowel syndrome: further experience. Gut 1987, 28:423–425.
Wolfe SG, Chey WY, Washington MK, et al.: Tolerability and safety of alosetron during long-term administration in female irritable bowel syndrome patients. Am J Gastroenterol 2001, 96:803–811.
Friedel D, Thomas R, Fisher RS: Ischemic colitis during treatment with alosetron. Gastroenterology 2001, 120:557–560.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Gwee, KA. Postinfectious irritable bowel syndrome. Curr Treat Options Gastro 4, 287–291 (2001). https://doi.org/10.1007/s11938-001-0053-z
Issue Date:
DOI: https://doi.org/10.1007/s11938-001-0053-z