Abstract
Aims
Inconsistent results relating dietary red and processed meat intake and risk of esophageal adenocarcinoma (EAC) have been reported. This article summarizes and quantifies the current evidence in a meta-analysis of observational studies.
Methods
Electronic search of MEDLINE and EMBASE databases was performed to identify peer-reviewed manuscripts up to 31 May 2012. Random-effects models were used to pool study results.
Results
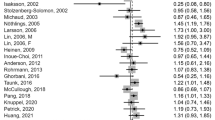
Ten manuscripts from 3 cohort studies and 7 case–control studies were identified. The summary relative risks (SRRs) of EAC for highest versus lowest intake categories were 1.31 (95 % confidence intervals [CIs]: 1.05–1.64) for red meat consumption, and 1.41 (95 % CIs 1.09–1.83) for processed meat consumption. Subgroup analyses indicated that these positive relations were seen in case–control studies, but not in cohort studies. Based on dose–response analysis, similar results were found; the SRRs were 1.45(95 % CIs 1.09–1.93) per 100 g/day of red meat intake and 1.37 (95 % CIs 1.03–1.81) per 50 g/day of processed meat intake.
Conclusions
The results of this meta-analysis indicate that consumption of red and processed meat may be associated with increased risk of esophageal adenocarcinoma. More studies, particularly prospective studies, are needed.




Similar content being viewed by others

Abbreviations
- EC:
-
Esophageal cancer
- ESCC:
-
Esophageal squamous cell carcinoma
- EAC:
-
Esophageal adenocarcinoma
- SRRs:
-
Summary relative risks
- CI:
-
Confidence intervals
- BMI:
-
Body mass index
- GOR:
-
Gastroesophageal reflux
- NOCs:
-
N-nitroso compounds
- HCAs:
-
Heterocyclic amines
- PAHs:
-
Polycyclic aromatic hydrocarbons
References
Thrift AP, Whiteman DC The incidence of esophageal adenocarcinoma continues to rise: analysis of period and birth cohort effects on recent trends. Ann Oncol (in press)
Ferlay J, Shin HR, Bray F et al (2010) Estimates of worldwide burden of cancer in 2008: GLOBOCAN 2008. Int J Cancer 127:2893–2917
Holmes RS, Vaughan TL (2007) Epidemiology and pathogenesis of esophageal cancer. Semin Radiat Oncol 17:2–9
Allum WH, Blazeby JM, Griffin SM et al (2011) Guidelines for the management of oesophageal and gastric cancer. Gut 60:1449–1472
Erichsen R, Robertson D, Farkas DK et al (2012) Erosive reflux disease increases risk for esophageal adenocarcinoma, compared with nonerosive reflux. Clin Gastroenterol Hepatol 10(475–480):e471
Reid BJ, Li X, Galipeau PC, Vaughan TL (2010) Barrett’s oesophagus and oesophageal adenocarcinoma: time for a new synthesis. Nat Rev Cancer 10:87–101
Kubo A, Corley DA (2006) Body mass index and adenocarcinomas of the esophagus or gastric cardia: a systematic review and meta-analysis. Cancer Epidemiol Biomarkers Prev 15:872–878
Tramacere I, La Vecchia C, Negri E (2011) Tobacco smoking and esophageal and gastric cardia adenocarcinoma: a meta-analysis. Epidemiology 22:344–349
Tramacere I, Pelucchi C, Bagnardi V et al (2012) A meta-analysis on alcohol drinking and esophageal and gastric cardia adenocarcinoma risk. Ann Oncol 23:287–297
Ward MH, Sinha R, Heineman EF et al (1997) Risk of adenocarcinoma of the stomach and esophagus with meat cooking method and doneness preference. Int J Cancer 71:14–19
Zhang ZF, Kurtz RC, Yu GP et al (1997) Adenocarcinomas of the esophagus and gastric cardia: the role of diet. Nutr Cancer 27:298–309
Chen H, Ward MH, Graubard BI et al (2002) Dietary patterns and adenocarcinoma of the esophagus and distal stomach. Am J Clin Nutr 75:137–144
Gonzalez CA, Jakszyn P, Pera G et al (2006) Meat intake and risk of stomach and esophageal adenocarcinoma within the European prospective investigation into cancer and nutrition (EPIC). J Natl Cancer Inst 98:345–354
Wu AH, Tseng CC, Hankin J, Bernstein L (2007) Fiber intake and risk of adenocarcinomas of the esophagus and stomach. Cancer Causes Control 18:713–722
Navarro Silvera SA, Mayne ST, Risch H et al (2008) Food group intake and risk of subtypes of esophageal and gastric cancer. Int J Cancer 123:852–860
Cross AJ, Freedman ND, Ren J et al (2011) Meat consumption and risk of esophageal and gastric cancer in a large prospective study. Am J Gastroenterol 106:432–442
Mulholland HG, Murray LJ, Anderson LA, Cantwell MM (2011) Vitamin D, calcium and dairy intake, and risk of oesophageal adenocarcinoma and its precursor conditions. Br J Nutr 106:732–741
O’doherty MG, Cantwell MM, Murray LJ, Anderson LA, Abnet CC (2011) Dietary fat and meat intakes and risk of reflux esophagitis, Barrett’s esophagus and esophageal adenocarcinoma. Int J Cancer 129:1493–1502
Keszei AP, Schouten LJ, Goldbohm RA, Van Den Brandt PA (2012) Red and processed meat consumption and the risk of esophageal and gastric cancer subtypes in The Netherlands Cohort Study. Ann Oncol 23:2319–2326
Ward MH, Cross AJ, Abnet CC et al (2012) Heme iron from meat and risk of adenocarcinoma of the esophagus and stomach. Eur J Cancer Prev 21:134–138
Cross AJ, Sinha R (2008) Meat consumption and cancer. In: Heggenhougen HK (ed) International encyclopedia of public health, vol 4. Academic Press, San Diego, pp 272–281
Hakami R, Mohtadinia J, Etemadi A et al (2008) Dietary intake of benzo(a)pyrene and risk of esophageal cancer in north of Iran. Nutr Cancer 60:216–221
Mirvish SS (1995) Role of N-nitroso compounds (NOC) and N-nitrosation in etiology of gastric, esophageal, nasopharyngeal and bladder cancer and contribution to cancer of known exposures to NOC. Cancer Lett 93:17–48
Kamangar F, Chow WH, Abnet CC, Dawsey SM (2009) Environmental causes of esophageal cancer. Gastroenterol Clin North Am 38:27–57, vii
Stroup DF, Berlin JA, Morton SC et al (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 283:2008–2012
Dersimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7:177–188
Greenland S, Longnecker MP (1992) Methods for trend estimation from summarized dose-response data, with applications to meta-analysis. Am J Epidemiol 135:1301–1309
Orsini N, Bellocco R, Greenland S (2006) Generalized least squares for trend estimation of summarized dose-response data. Stata J 6:40–57
Chen X, Yang G, Ding WY et al (1999) An esophagogastroduodenal anastomosis model for esophageal adenocarcinogenesis in rats and enhancement by iron overload. Carcinogenesis 20:1801–1808
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315:629–634
Terry PD, Lagergren J, Wolk A, Steineck G, Nyren O (2003) Dietary intake of heterocyclic amines and cancers of the esophagus and gastric cardia. Cancer Epidemiol Biomarkers Prev 12:940–944
Ward MH, Heineman EF, Markin RS, Weisenburger DD (2008) Adenocarcinoma of the stomach and esophagus and drinking water and dietary sources of nitrate and nitrite. Int J Occup Environ Health 14:193–197
O’doherty MG, Abnet CC, Murray LJ et al (2010) Iron intake and markers of iron status and risk of Barrett’s esophagus and esophageal adenocarcinoma. Cancer Causes Control 21:2269–2279
Cross AJ, Pollock JR, Bingham SA (2003) Haem, not protein or inorganic iron, is responsible for endogenous intestinal N-nitrosation arising from red meat. Cancer Res 63:2358–2360
Prentice RL (2003) Dietary assessment and the reliability of nutritional epidemiology reports. Lancet 362:182–183
Willett WC, Sampson L, Stampfer MJ et al (1985) Reproducibility and validity of a semiquantitative food frequency questionnaire. Am J Epidemiol 122:51–65
Gonzalez CA, Pera G, Agudo A et al (2006) Fruit and vegetable intake and the risk of stomach and oesophagus adenocarcinoma in the European Prospective Investigation into Cancer and Nutrition (EPIC-EURGAST). Int J Cancer 118:2559–2566
Willett WC, Howe GR, Kushi LH (1997) Adjustment for total energy intake in epidemiologic studies. Am J Clin Nutr 65:1220S–1228S discussion 1229S–1231S
Xue W, Warshawsky D (2005) Metabolic activation of polycyclic and heterocyclic aromatic hydrocarbons and DNA damage: a review. Toxicol Appl Pharmacol 206:73–93
Conflicts of interests
The authors disclose no conflicts of interests.
Author information
Authors and Affiliations
Corresponding author
Additional information
Wen Huang and Yujing Han contributed equally to this work.
Rights and permissions
About this article
Cite this article
Huang, W., Han, Y., Xu, J. et al. Red and processed meat intake and risk of esophageal adenocarcinoma: a meta-analysis of observational studies. Cancer Causes Control 24, 193–201 (2013). https://doi.org/10.1007/s10552-012-0105-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-012-0105-9