ABSTRACT
BACKGROUND
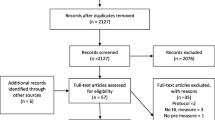
We evaluated the effectiveness and cost-effectiveness of alternative interventions designed to promote mammography in safety-net settings.
METHODS
A three-arm, quasi-experimental evaluation was conducted among eight federally qualified health clinics in predominately rural Louisiana. Mammography screening efforts included: 1) enhanced care, 2) health literacy-informed education of patients, and 3) education plus nurse support. Outcomes included mammography screening completion within 6 months and incremental cost-effectiveness.
RESULTS
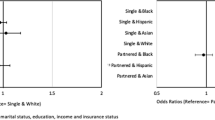
Overall, 1,181 female patients ages 40 and over who were eligible for routine mammography were recruited. Baseline screening rates were < 10 %. Post intervention screening rates were 55.7 % with enhanced care, 51.8 % with health literacy-informed education and 65.8 % with education and nurse support. After adjusting for race, marital status, self-efficacy and literacy, patients receiving health-literacy informed education were not more likely to complete mammographic screening than those receiving enhanced care; those additionally receiving nurse support were 1.37-fold more likely to complete mammographic screening than those receiving the brief education (95 % Confidence Interval 1.08–1.74, p = 0.01). The incremental cost per additional women screened was $2,457 for literacy-informed education with nurse support over literacy-informed education alone.
CONCLUSIONS
Mammography rates were increased substantially over existing baseline rates in all three arms with the educational initiative, with nurse support and follow-up being the most effective option. However, it is not likely to be cost-effective or affordable in resource-limited clinics.

Similar content being viewed by others
REFERENCES
American Cancer Society. Cancer facts & figures 2011–2012. Atlanta: ACS; 2012.
Cho Y, Lee S, Arozullah A, et al. Effects of health literacy on health status and health service utilization amongst the elderly. Soc Sci Med. 2008;66:1809–16.
White S, Chen J, Atchinson R. Relationship of Preventive Health Practices and Health Literacy: A National Study. Am J Health Behav. 2008;32(3):227–42.
Alexandraki I, Mooradian AD. Barriers related to mammography use for breast cancer screening among minority women. J Natl Med Assoc. 2010;102(3):206–18.
Kagawa-Singer M, Valdez Dadia A, Yu MC, et al. Cancer, culture, and health disparities: Time to chart a new course? CA: A Cancer Journal for Clinicians. 2010;60(1):12–39.
Rayman KM, Edwards J. Rural primary care providers’ perceptions of their role in the breast cancer care continuum. J Rural Health. 2010;26(2):189–95.
Edwards JB, Tudiver F. Women’s preventive screening in rural health clinics. Women’s Health Issues. 2008;18(3):155–66.
American Cancer Society. Breast Cancer Facts & Figures 2009-2010. Atlanta: American Cancer Society.
Brown KC, Fitzhugh EC, Neutens JJ, et al.Screening mammography utilization in Tennessee women: the association with residence. J Rural Health. 2009;25(2):167–73.
Cummings DM, Whetstone LM, Earp JA, et al. Disparities in mammography screening in rural areas: analysis of county differences in North Carolina. J Rural Health. 2002;18(1):77–83.
Harris DM, Miller JE, Davis DM. Racial differences in breast cancer screening, knowledge and compliance. J Nat Med Assoc. 2003;95(8):693–701.
Cronan T, Villalta I, Gottfried E, et al. Predictors of mammography screening among ethnically diverse low-income women. Journal of Women’s Health. 2008;17(4):527–37.
Davis TC, Arnold C, Berkel HJ, et al. Knowledge and attitude on screening mammography among low literate, low income women. Cancer. 1996;78(9):1912–20.
Eheman C, Benard V, Blackman D, et al. Breast Cancer Screening among Low-Income or Uninsured Women: Results from the National Breast and Cervical Cancer Early Detection Program, July 1995 to March 2002 (United States). Canc Causes Contr. 2006;17(1):29–38.
U.S. Department of Health and Human Services. Office of Disease Prevention and Health Promotion. Healthy People 2020. Washington, DC. Available at http://www.healthypeople.gov/2020/topicsobjectives2020/objectiveslist.aspx?topicId=5 Accessed December 4, 2013.
Agency for Healthcare Research and Quality. National Health Disparities Report 2011.
Champion V, Skinner C, Menon U. Development of a self efficacy scale for mammography. Res Nurse Health. 2005;28(4):329–36.
Clark M, Rakowski W, Bonacore L. Repeat mammography: Prevalence estimates and considerations for assessment. Ann Behav Med. 2003;26(3):201–11.
Elting LS, Cooksley CD, Bekele BN, et al. Mammography capacity: impact on screening rates and breast cancer stage at diagnosis. Am J Prev Med. 2009;37(2):102–8.
Ogedegbe G, Cassells AN, Robinson CM, et al. Perceptions of barriers and facilitators of cancer early detection among low-income minority women in community health centers. J Natl Med Assoc. 2005;97(2):162–70.
Rauscher GH, Hawley ST, Earp JAL. Baseline predictors of initiation vs. maintenance of regular mammography use among rural women. Prev Med. 2005;40(6):822–30.
O’Malley AS, Forrest CB, Mandelblatt J. Adherence of low-income women to cancer screening recommendations. J Gen Intern Med. 2002;17(2):144–55.
Engelman KK, Ellerbeck EF, Perpich D, et al. Office systems and their influence on mammography use in rural and urban primary care. J Rural Health. 2004;20(1):36–42.
Lyttle NL, Stadelman K. Assessing awareness and knowledge of breast and cervical cancer among Appalachian women. Prev Chronic Dis. 2006;3(4):A125.
Lopez EDS, Khoury AJ, Dailey AB, et al. Screening mammography: A cross-sectional study to compare characteristics of women aged 40 and older from the deep south who are current, overdue, and never screeners. Women’s Health Issues. 2009;19(6):434–45.
Tejeda S, Thompson B, Coronado GD, et al.Predisposing and enabling factors associated with mammography use among Hispanic and non-Hispanic white women living in a rural area. J Rural Health. 2009;25(1):85–92.
McAlearney AS, Reeves K, Tatum C, et al. Cost as a barrier to screening mammography among underserved women. Ethn Health. 2007;12(2):189–203.
Bennett I, Chen J, Soroui J, et al. The contribution of health literacy to disparities in self-rated health status and preventive health behaviors in older adults. Ann Fam Med. 2009;7:204–11.
Guerra C, Krumholz M, Shea J.Literacy and knowledge, attitudes and behavior about mammography in Latinas. J Health Care Poor Underserved. 2005;16:152–66.
U.S. Department of Health and Human Services. Office of Disease Prevention and Health Promotion: National Action Plan to Improve Health Literacy. Washington, D.C.: U.S. Department of Health and Human Services, 2010.
Davis TC, Berkel HJ, Arnold CL, et al. Intervention to increase mammography utilization in a public hospital. J Gen Intern Med. 1998;13(4):230–3.
Health Resources and Services Administration. www.hrsa.gov/. Accessed December 4, 2013.
Weiss B, Schwartzberg J, Davis T, et al. Health literacy and patient safety: Help patients understand: manual for clinicians. AMA Foundation, 2007.
U.S. Cancer Statistics Working Group. United States Cancer Statistics: 1999-2009 Incidence and Mortality Web-based Report. Atlanta: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention and National Cancer Institute; 2013. Available at: www.cdc.gov/uscs. Accessed December 4, 2013.
Ferreira MR, Dolan NC, Fitzgibbon ML, et al. Health care provider-directed intervention to increase colorectal cancer screening among veterans: Results of a randomized controlled trial. J Clin Oncol. 2005;23:1548–54.
Davis T, Arnold C, Rademaker A, et al. Improving colon cancer screening in community clinics. Cancer. 2013;119(21):3879–86.
US Preventive Services Task Force. Screening for breast cancer: U.S. Preventive Services Task Force Recommendation Statement. Ann Intern Med. 2009;151:716–26.
Champion V, Skinner C, Menon U. Development of a self-efficacy scale for mammography. Res Nurs Health. 2005;28:329–36.
Janz NK, Champion VL, Strecher VJ. The health belief model. In: Glanz K, Lewis F, Rimer B (eds.), Health Education Behavior, San Francisco: Jossey-Bass.
Rosenstock I. The health belief model: origins and correlates. Health Educ Monogr. 1974;2:336–53.
Rosenstock I, Strecher V, Becker M. Social learning theory and the health belief model. Health Educ Q. 1988;15(2):175–83.
Bandura A. Health promotion by social cognitive means. Health Educ Behav. 2004;31(2):143–64.
Davis TC, Arnold CL, Rademaker A, et al. Differences in Barriers to Mammography between Rural and Urban Women. Journal of Women’s Health. July 2012; 748-55.
Davis T, Long S, Jackson R, et al. Rapid estimate of adult literacy in medicine: a shortened screening instrument. Fam Med. 1993;25(6):391.
Hecht J, Borrelli B, Breger R, et al. Motivational interviewing in community-based research: Experiences from the field. Ann Behav Med. 2005;9(2):29–34.
Wolf MS, Wilson EA, Rapp DN, et al. Literacy and learning in health care. Pediatrics. 2009;124(Suppl 3):S275–81.
Phillips C, Rothstein J, Beaver K, et al.Patient navigation to increase mammography screening among inner city women. J Gen Intern Med. 2011;26(2):123–9.
Lipkus I, Rimer B, Halabi S, et al. Can tailored interventions increase mammography use among HMO women? Am J Prev Med. 2000;18(1):1–10.
Legler J, Meissner H, Coyne C, et al. The effectiveness of interventions to promote mammography among women with historically lower rates of screening. Cancer Epidemiol Biomarkers Prev. 2002;11(1):59–71.
Dietrich A, Tobin J, Cassells A, et al. Translation of an efficacious cancer-screening intervention to women enrolled in a Medicaid managed care organization. Ann of Fam Med. 2007;5(4):320–7.
Saywell R, Champion V, Skinner C, et al. A cost-effectiveness comparison of three tailored interventions to increase mammography screening. J Womens Health. 2004;13(8):909–18.
Saywell R, Champion V, Zollinger T, et al. The cost effectiveness of 5 interventions to increase mammography adherence in a managed care population. Am J Manag Care. 2003;9(1):33–44.
Acknowledgements
The authors would like to thank Ivory Davis, MSN and Cara Pugh, BSN, for their commitment to helping patients complete screening. This research was funded by the National Cancer Institute (R01- CA115869-05).
Conflict of Interest
The study authors have no potential conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Davis, T.C., Rademaker, A., Bennett, C.L. et al. Improving Mammography Screening Among the Medically Underserved. J GEN INTERN MED 29, 628–635 (2014). https://doi.org/10.1007/s11606-013-2743-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-013-2743-3