Abstract
Mitochondria are known to combine life-supporting functions with participation in apoptosis by controlling caspase activity. Here, we report that in human blood neutrophils the mitochondria are different, because they preserve mainly death-mediating abilities. Neutrophil mitochondria hardly participate in ATP synthesis, and have a very low activity of the tested marker enzymes. The presence of mitochondria in neutrophils was confirmed by quantification of mitochondrial DNA copy number, by detection of mitochondrial porin, and by JC-1 measurement of Δψm. During neutrophilic differentiation, HL-60 cells demonstrated a profound cytochrome c depletion and mitochondrial shape change reminiscent of neutrophils. However, blood neutrophils containing extremely low amounts of cytochrome c displayed strong caspase-9 activation during apoptosis, which was also observed in apoptotic neutrophil-derived cytoplasts lacking any detectable cytochrome c. We suggest that other proapoptotic factors such as Smac/DIABLO and HtrA2/Omi, which are massively released from the mitochondria, have an important role in neutrophil apoptosis.
Similar content being viewed by others
Introduction
Mitochondria are known as organelles in which a large amount of energy, required for cell maintenance and function, is processed in the form of ATP. During the last decade, it has been shown that the mitochondria possess additional functions in cell death.1 These organelles contain a number of proteins in the intermembrane space, which, once released into the cytosol, induce and/or amplify the activation of apoptotic caspases. One of these proteins, cytochrome c, plays a key role in mitochondrial respiration, transferring electrons from complex III to complex IV of the respiratory chain. Cytochrome c also participates in the assembly of a multimolecular complex known as the apoptosome, which promotes activation of the initiator caspase-9 and constitutes a core element of the intrinsic (mitochondrial, stress-induced) pathway of apoptosis. For other mitochondrial proteins, such as AIF, Smac/DIABLO and Omi/HtrA2, only proapoptotic functions have been identified so far.1 Apparently, in most cell types, the mitochondria combine functions related to cellular life and death.
In this light, the human neutrophil seems to be an exceptional cell for several reasons. For a long time, the abundance and function of mitochondria in neutrophils have been debated. It was believed that neutrophils possess no or only a few mitochondria, which do not play a role in their function. This point of view was mainly based on the observation that mitochondrial poisons like cyanides do not influence cellular functions in neutrophils.2 Moreover, electron microscopy studies identified hardly any mitochondria in neutrophils (see the references in Fossati et al.3), and mitochondrial respiration was found to be very low in these cells.4 However, mitochondria have been recently visualized in neutrophils as a tubular network, by means of specific fluorescent dyes.3,5 Furthermore, in neutrophils undergoing spontaneous or induced apoptosis, the mitochondria form clusters to which the proapoptotic Bax protein also is localized.5,6,7 Such a subcellular redistribution of Bax to mitochondria upon apoptosis is known to result in the permeabilization of the outer mitochondrial membrane, with the subsequent release of additional proapoptotic proteins.1 Hence, this finding gave some evidence that the mitochondria in neutrophils are involved in apoptosis.
In the present study, we show that the mitochondria, although limited in number, do participate in the neutrophil apoptosis. These organelles hardly display any marker mitochondrial enzymatic activity, do not synthesize much ATP, but preserve their transmembrane potential (Δψm) and are loaded with proapoptotic proteins, which are released into the cytosol upon induction of neutrophil apoptosis. During maturation of the myeloid HL-60 cells into neutrophil-like cells, cytochrome c is strongly reduced and almost completely absent in human neutrophils. Moreover, we show that, apparently, cytochrome c-independent caspase-9 activation occurs in neutrophil-derived cytoplasts, which lack mitochondria and are devoid of cytochrome c.
Results
Neutrophils possess mitochondria, which do not synthesize ATP, have limited specific enzymatic activity, but maintain the transmembrane potential (Δψm)
Mitochondria in neutrophils have been identified by means of specific fluorescent dyes as a network of tubular elongated structures.3,5,6 However, in neutrophils, these organelles hardly play a role in energy metabolism as they do in other cells. This conclusion was derived from the experiment shown in Figure 1, where ATP concentrations in neutrophils were measured under various conditions. We found a modest decrease (about 30%) of ATP levels in untreated neutrophils after 6 h of culture in comparison to fresh neutrophils, which probably reflects a constitutive senescence process.8 The inhibitors of mitochondrial respiration rotenone, TTFA, and sodium azide9 caused no or only little additional reduction in the neutrophil ATP levels (Figure 1), whereas in the myeloid HL-60 cell line, for instance, rotenone induced a pronounced (∼70%) ATP depletion, decreasing the ATP concentration after a 6 h incubation from 4900±461 to 1466±183 pmol per 106 cells (mean±S.D.; n=3). This can be explained by the fact that neutrophils mainly use glycolysis rather than mitochondrial oxidative phosphorylation for their energy supply.2 Accordingly, inhibitors of glycolysis such as sodium iodoacetate and 2-deoxyglucose caused a profound ATP loss with less than 1% of ATP remaining in comparison to untreated neutrophils (Figure 1; and data not shown). Moreover, two important mitochondrial enzymes, glutamate dehydrogenase (GDH) and fumarase, which are often used as markers of mitochondria,10,11,12 displayed a borderline low activity in neutrophils in contrast to HL-60 cells, which have actively respiring mitochondria13,14 (Figure 2). At the same time, the activity of the cytoplasmic marker lactate dehydrogenase (LDH) was nearly identical in neutrophils and HL-60 cells, confirming an overall intactness of enzymes in the neutrophil cell lysates (Figure 2). Also, the activity of GDH and fumarase in the neutrophil+HL-60 T-X100 colysates was similar to that of the only HL-60 T-X100 lysates, excluding thus a possibility of nonspecific proteolytic degradation (see below) of these enzymes in the neutrophil T-X100 cell lysates (not shown).
ATP concentrations in neutrophils. Fresh neutrophils or neutrophils treated for 6 h with or without inhibitors of mitochondrial respiration rotenone (0.1 mM), TTFA (0.3 mM) or Na Azide (2 mM) or the inhibitor of glycolysis sodium iodoacetate (SIA; 0.5 mM) were collected, and ATP concentration was measured by a luciferase-based assay. The data represent the mean±S.D. from four independent experiments
Enzymatic activity of GDH, fumarase and LDH in neutrophils and HL-60 cells. Specific enzymatic reactions for the mitochondrial marker enzymes GDH (left panel) and fumarase (middle panel) or for the cytoplasmic enzyme LDH (right panel) were measured spectrophotometrically in the Triton-X100 cell extracts from neutrophils (closed bars) or HL-60 cells (open bars). Results show the slope of the OD340 nm decrease (−ΔOD340 nm per min) for GDH and LDH or a slope of the OD250 nm increase (ΔOD250 nm per min) for fumarase. The total content of protein was ∼50 μg (GDH, fumarase) or ∼5 μg (LDH) per reaction; data (mean±S.E.M.) obtained in six separate experiments
However, despite the virtually absent oxidative phosphorylation, neutrophil mitochondria do maintain their Δψm. This was monitored by staining neutrophils with JC-1, a fluorescent dye, which differentially stains mitochondria in accordance to their Δψm.15 Active mitochondria with high Δψm accumulate JC-1 aggregates, which are red, whereas, in the mitochondria with low Δψm (inactive), JC-1 stays in a monomeric, green form. This renders the red/green ratio, a sensitive indicator of the mitochondrial Δψm changes, which does not depend on other factors such as mitochondrial size, shape and density, that may influence single-component fluorescent signals.16 Analyzed in this way in a real-time plate reader assay, Δψm stayed relatively stable in untreated fresh neutrophils, while it was rapidly (within 5 min) dissipated by the uncoupler CCCP or by the K+ ionophore valinomycin (Figure 3). The same was observed in HL-60 cells (Figure 3). These results were confirmed by FACS analysis of the neutrophil cell suspension stained by JC-1 (data not shown).
Δψm in neutrophils and HL-60 cells measured by JC-1 staining. Neutrophils (top graph) or HL-60 cells (bottom graph) were stained with JC-1 (1 μg/ml) and analyzed in a real-time plate reader assay. Δψm was monitored for 20 min without additions (open circles), with 5 μM CCCP (closed squares) or with 5 μM valinomycin (closed triangles). Results are expressed as a change in the ratio between red JC-1 fluorescence (Em 590 nm), and green JC-1 fluorescence (Em 535 nm) over time. Each point represents the mean±S.E.M. from three (neutrophils) or six (HL-60) experiments
The number of the mitochondrial DNA copies in neutrophils is low
The data shown above confirm that neutrophils do possess mitochondria. However, regarding the findings that neutrophils hardly display any mitochondrial oxidative phosphorylation and show a lack of mitochondrial marker enzyme activities (see Figures 1 and 2), the relative number of mitochondria in neutrophils remained unclear. To resolve this question, we employed a quantitative PCR on the human cytochrome c oxidase subunit I (CCOI) gene encoded by mitochondrial DNA,17 because mitochondria are unique organelles with a separate, autonomously replicating DNA genome.18 The CCOI PCR, paralleled by PCR on the nuclear gene for the human albumin, which have two copies per nuclear genome, yields a relative estimation of the number of mtDNA copies per cell. As shown in Figure 4, neutrophils had 30–40 and 10–15 times less copies of the mitochondrial genome in comparison to HL-60 cells and PBMC, respectively.
Quantification of the mtDNA copy number by real-time PCR. Total DNA was extracted from indicated cells, and LightCycler real-time quantitative PCR was performed with primers specific for the human mitochondrial gene cytochrome c oxidase subunit I (CCOI) and for the human nuclear gene albumin. Values indicate the number of CCOI copies per albumin copy, calculated as described in Materials and Methods; the individual values and means (±S.E.M.) of four independent experiments
During the neutrophilic lineage maturation, HL-60 cells gain tubular mitochondria and lose cytochrome c expression
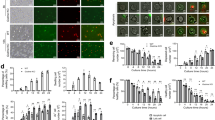
Despite a limited role of neutrophil mitochondria in cellular metabolism, our recent studies have suggested that these organelles might be involved in neutrophil cell death.5,6 In an attempt to clarify the role of mitochondria in apoptosis, we studied the expression of a number of proapoptotic mitochondrial proteins.1,19 Unexpectedly, none of the tested proteins, including cytochrome c, AIF, Omi and Smac gave a positive signal in Western blot (Figure 5, lane 1), whereas a mitochondrial isoform of superoxide dismutase (MnSOD) or the cytoplasmic protein Bax were readily detectable (Figure 5, lane 1). In contrast, all proteins of interest were present in HL-60, primary monocyte and lymphocyte cell lysates (Figure 5, lanes 2, 7 and 8). At this point, we supposed that neutrophils may have lost most of the cytochrome c during maturation. To address this possibility, the HL-60 cells were induced to differentiate to the neutrophilic lineage by DMSO. The maturing cells showed a gradual increase in NADPH-oxidase activity (Figure 6a), which after 5 days of maturation was about half of that of primary neutrophils (3315±693 relative fluorescence units (RFU)/min for 5-day-DMSO-treated HL-60 and 6725±1156 RFU/min for primary neutrophils; mean±S.E.M., n=3). In parallel, the shape of the mitochondria was monitored. As shown in Figure 6b (left panel), undifferentiated HL-60 cells had punctate mitochondria. Remarkably, in the maturing cells, the mitochondria changed their shape into tubular structures (Figure 6b, right panel), as previously found in neutrophils.5 The number of cells with tubular mitochondria was growing in correspondence to the increase in the NADPH-oxidase activity (Figure 6a and c). Then, we measured the expression of the proapoptotic mitochondrial proteins during HL-60 maturation by Western blot. Cytochrome c expression was found to rapidly drop just after the first day of DMSO treatment, reaching the detection limit on the fifth day, whereas the expression of AIF, Omi and Smac remained relatively stable during the whole period of maturation (Figure 6d). These data indicate that, during the neutrophilic maturation, HL-60 cells selectively lose cytochrome c expression and form tubular mitochondria, which may be considered as indicators of neutrophil maturation.
Expression of mitochondrial proteins and Bax in primary leukocytes and in HL-60 cells. Whole-cell lysates were prepared without (lanes 1–3, 7, 8) or with (lanes 4–6) DFP preincubation before lysis (see Materials and Methods). Equivalents of 1 × 106 neutrophils (lanes 1 and 3), 0.25 × 106 HL-60 cells (lanes 2 and 5) or of their colysates (lanes 3 and 6), of 0.5 × 106 monocytes and lymphocytes (lanes 7 and 8, respectively) were subjected to SDS-PAGE. Western blot was performed with specific antibodies for the indicated proteins. The results represent three independent experiments
Mitochondrial changes during DMSO-induced HL-60 cell maturation. The HL-60 cells were induced to mature towards the neutrophilic lineage by culturing in the presence of 1.25% DMSO, and samples were taken at the indicated time points. (a) The PMA-dependent NADPH-oxidase activity was determined with a fluorimetric assay based on H2O2-mediated oxidation of Amplex Red and expressed in RFU (mean±S.E.M.; n=3) per min. (b, c) The cells stained with MitoTracker GreenFM were analyzed by a fluorescence microscope. A minimum of 200–300 cells was scored for each sample and the percentages of cells with tubular mitochondria (shown in (b), right image) were determined ((c); mean±S.E.M.; n=3). The bar in (b) is 5 μm. (d) Total cell lysates were tested by Western blot with specific antibodies for the indicated proteins
In the neutrophil cell lysates, detection of mitochondrial proteins is limited due to nonspecific proteolysis
Our failure to detect mitochondrial proteins in neutrophil lysates may reflect the low number of mitochondria per neutrophil (see Figure 4), with the quantity of proteins below the Western blot detection limit. Alternatively, the tremendous proteolytic potential of neutrophils may cause aspecific degradation of proteins, leading to loss of their detection.7,20
As shown in Figure 5, lane 1, together with apoptosis-related mitochondrial proteins, porin, a channel-forming protein in the outer mitochondrial membrane (also known as voltage-dependent anion channel, VDAC),21 was undetectable. Due to its abundance, porin is often used as a reference standard in Western blot when assaying other mitochondrial proteins.22 At the same time, another mitochondrial marker MnSOD23,24 gave a strong signal (Figure 5, lane 1). This contradiction suggested a selective nonspecific proteolysis of mitochondrial proteins in the conventional neutrophil lysates. Indeed, when neutrophils and HL-60 cells, in numbers loaded in lanes 1 and 2, respectively (Figure 5), were lysed together, the signals from cytochrome c, AIF, Omi, Smac and porin, normally present in the HL-60 lysates, were dramatically reduced (Figure 5, lane 3). This happened despite the presence of a broad-spectrum protease inhibitor cocktail during the lysis procedure, which allowed detection of the signals in the other cell preparations (Figure 5, lanes 2, 7 and 8). Detection of MnSOD and Bax remained good in all the three preparations (Figure 5, lanes 1–3). Preincubation of cells with the serine protease inhibitor DFP before lysis (see Materials and Methods section) enabled detection in the neutrophil lysates of AIF, Omi, Smac and porin (Figure 4, lane 4). For all further immunoblotting analyses, the cell lysates were prepared in the presence of DFP. However, cytochrome c was still undetectable, and this could not be explained by aspecific proteolysis, because cytochrome c displayed a strong signal in the DFP-protected colysate of neutrophils and HL-60 cells (Figure 5, lane 6).
Neutrophil mitochondria release proapoptotic proteins into the cytosol during apoptosis
To show that the neutrophil mitochondria release their proapoptotic proteins into the cytosol upon apoptosis, subcellular fractionation into cytosolic and mitochondria fractions was performed. As a model of apoptosis, we used the 3-h TNF-α/CHX-treated neutrophils, which die rapidly and massively by classical caspase-dependent apoptosis.25,26,27 These conditions appeared to be optimal, because the majority of neutrophils become apoptotic (70–80% bind Annexin-V (see the legend of Figure 7) and display morphological apoptosis (not shown)), while preserving the intactness of the plasma membrane (PI staining in <5%). These circumstances thus minimize the possibility for proteins to leak out of the cell, which is real during an overnight culture, when ∼15–30% of cells become PI-permeable. The same reasons are applicable for the etoposide-induced HL-60 apoptosis, used in our study.
Release of proteins from mitochondria to the cytosol in neutrophils and HL-60 cells during apoptosis. Digitonin-based cell fractionation was performed in fresh neutrophils (lanes 1 and 4; <5% Annexin-V+ cells), in neutrophils incubated for 3 h without additions (lanes 2 and 5; 10±2% Annexin-V+ cells) or with TNF-α/CHX to induce apoptosis (T/C; lanes 3 and 6; 74±3% Annexin-V+ cells). The same procedure was applied to the untreated (lanes 7 and 9; <5% Annexin-V+ cells) or etoposide-treated HL-60 cells (+Eto; lanes 8 and 10; 29±2% Annexin-V+ cells). The percentage of Annexin-V+ cells is given as mean±S.E.M. (n=3). All steps were performed in the presence of 2 mM DFP. Thereafter, the cytosol (lanes 1–3, 7, 8) and the mitochondrial (lanes 4–6, 9, 10) fractions were subjected to SDS-PAGE. Western blot was performed with specific antibodies for the indicated proteins. Each neutrophil fraction represents ∼2 × 106 cells, each HL-60 fraction represents ∼0.4 × 106 HL-60 cells. The probe with antiporin and anti-Apaf-1 Ab served as a reference for mitochondria and cytosol, respectively. The results represent three independent experiments
Subcellular fractionation discovered a weak cytochrome c expression in the neutrophil mitochondrial fraction (Figure 7, lanes 4 and 5), apparently due to the increased protein concentration. As shown in Figure 7, none of the mitochondrial proteins was present in the cytosol of freshly purified neutrophils (lane 1) or neutrophils cultured without additions for 3 h (lane 2). The cytosol of untreated HL-60 cells was also free of those proteins (Figure 7, lane 7). Induction of apoptosis with TNF-α/CHX coincided with a massive release of Omi and Smac from the mitochondria, where they are normally present in intact cells (Figure 7, lanes 4 and 5), into the cytosol (Figure 7, lane 3), with a concomitant decrease in signal from the mitochondrial fraction (Figure 6, lane 6). The same was happening in HL-60 cells treated with etoposide (Figure 7, lanes 8 and 10). A faint band of cytochrome c was found in the TNF-α/CHX-treated neutrophil cytosol only after film overexposure (not shown), whereas it was readily detectable in the cytosol of the etoposide-treated HL-60 cells (Figure 7, lane 8). AIF was present only in the mitochondrial fraction, irrespective of the extent of apoptosis, both in neutrophils and HL-60 cells (Figure 7, lanes 4–6, 9 and 10). Pellet fractions after the mitochondrial lysis step, which contained unsolubilized proteins, possessed a small amount of AIF, as determined by Western blot (data not shown). This supposed that, under our experimental settings, AIF did not undergo the nuclear translocation observed in other cell types.19 The purity of subcellular fractions was confirmed by detection of porin (see above), which was exclusively present in the mitochondrial fractions of neutrophils and HL-60 cells (Figure 7, lanes 4–6, 9 and 10). In contrast, the cytosolic protein Apaf-1 was indeed found only in the cytosol fractions, both in neutrophils and HL-60 cells (Figure 7, lanes 1–3, 7 and 8), irrespective of apoptosis. Bax protein is known to have a cytosolic localization in intact neutrophils (Figure 7, lanes 1 and 2), and translocates to the mitochondria upon apoptosis,5,6 as is evident in Figure 7, lanes 3 and 6. In HL-60 cells, Bax was localized both in the cytosol and mitochondria without significant changes during apoptosis (Figure 7, lanes 7–10). Thus, the neutrophil mitochondria actively participate in cell death, releasing a number of proapoptotic proteins into the cytosol upon induction of apoptosis.
Neutrophils activate caspase-9 during apoptosis
There are two major pathways of apoptosis within a cell. The extrinsic (death receptor-dependent) pathway proceeds through caspase-8 activation, whereas the intrinsic (mitochondrial, stress-induced) route of apoptosis involves a cytochrome c/Apaf-1-dependent assembly of apoptosome and activation of caspase-9. However, this division is somewhat artificial, because both pathways overlap and can amplify each other, with active caspase-3 as a common final effector. Considering the very low expression of cytochrome c in neutrophils, which was only detectable after subcellular fractionation (see Figure 5, lane 4, and Figure 7), the question emerged as to whether the classical apoptosome-dependent caspase-9 activation is operative in neutrophils. Data in Figure 7 (lanes 1–3) show the other component of the apoptosome (Apaf-1) to be present in the neutrophil cytosol. Moreover, the Apaf-1 expression in neutrophils was much higher compared to HL-60 cells (Figure 8a, lanes 1 and 2). Next, caspase-9 activation was studied by specific antibodies on Western blot. In neutrophil preparations in which apoptosis was minimal, the full-length caspase-9 proenzyme was present, whereas it was almost absent in apoptotic cells (Figure 9, caspase-9, upper panel, lanes 1–4), indicating proteolytic activation. Complete caspase-9 activation was evident in neutrophils that went into apoptosis after induction of the extrinsic death pathway (TNF-α+CHX), which is believed to be initiated by processing of caspase-8 (Figure 9, lane 3). On the other hand, overnight cultured neutrophils (81±4.6% Annexin-V+ cells; mean±S.E.M., n=3), which die without external stimulation through intrinsic mechanisms, displayed both caspase-9 and -8 (Figure 9, lane 4) activation as well. Activation of caspase-9 and -8 was also observed in etoposide-treated HL-60 cells (Figure 9, lane 8). Finally, promotion of either pathway led to caspase-3 activation (Figure 9, lanes 3 and 4), which was also found in apoptotic HL-60 cells (Figure 9, lane 8). Thus, despite the extremely low expression of cytochrome c, the activation of caspase-9 is functional in neutrophils. Moreover, processing of caspase-9 was also followed by an increase in enzymatic activity of caspase-9 in apoptotic neutrophils, which was monitored by cleavage of the specific fluorogenic caspase-9 substrate Ac-LEHD-AMC,28 as described earlier29 (data not shown).
No expression of cytochrome c and porin in neutrophil-derived cytoplasts. (a) Total cell lysates were prepared from HL-60 cells (lane 1), neutrophils (lane 2), or cytoplasts (lane 3) in the presence of 2 mM DFP, and equal amounts of protein (∼30 μg) were separated by SDS-PAGE. Western blot was performed with antibodies specific for the indicated proteins. (b) Cytochrome c was immunoprecipitated from the cell lysates (∼100 μg of total protein), the precipitates were resolved by SDS-PAGE followed by Western blot. The blot was probed with an anticytochrome c monoclonal Ab. The results are representative for three independent experiments
Activation of caspases in neutrophils, neutrophil-derived cytoplasts and HL-60 cells upon apoptosis. Total cell lysates were prepared in the presence of 2 mM DFP from fresh neutrophils (lane 1), from neutrophils cultured for 3 h or overnight without additions (lanes 2 and 4, respectively) or with TNF-α/CHX (lane 3); from fresh cytoplasts (lane 5) or from cytoplasts cultured untreated overnight (lane 6); and from untreated (lane 7) or etoposide-treated HL-60 cells (lane 8). The equivalent of ∼30 μg total protein was subjected to SDS-PAGE, and Western blot was performed with specific Abs for indicated proteins. The expression of Bax was used as a control for protein loading. The results are representative of three independent experiments
Mitochondria-free neutrophil-derived cytoplasts still activate caspase-9
In our recent studies, we have reported a model of neutrophil apoptosis that we consider as a ‘mitochondria-free’ system, namely the cytoplast cell death.5,6 In the present study, the absence of mitochondria in cytoplasts was confirmed by the lack of porin expression (Figure 8a, lane 3). In the neutrophil cytoplasts, from which the organelles had been removed by a discontinuous gradient ultracentrifugation, we still observed apoptotic changes after overnight culturing reminiscent of those of intact neutrophils, including membrane flip-flop with phosphatidylserine exposure on the cell surface (54±7% Annexin-V+ cytoplasts; mean±S.E.M., n=3) and the activation of caspase-8 and -3, which were all absent in fresh cytoplasts (Figure 9, lanes 5 and 6; see Maianski et al.5). When we now checked the processing of procaspase-9 in apoptotic cytoplasts, it was found to be normal, and, moreover, complete cleavage of the 47-kDa procaspase-9 was accompanied by detection of a 37-kDa active fragment of capsase-9 in cytoplasts (Figure 9, caspase-9, upper and lower panels, lane 6), which was missing in lanes with the apoptotic neutrophil cell lysates (Figure 9, caspase-9, lower panel, lanes 3 and 4). This may be explained by enhanced apoptotic degradation or by nonspecific proteolysis during sample preparation (see above) of the active caspase-9 in the neutrophils, because cytoplasts are devoid of granules (and their proteases). Also, in apoptotic HL-60 cells, which have a weak proteolytic potential, the active caspase-9 was detectable (Figure 9, caspase-9, lower panel, lane 8).
The intact activation of caspase-9 in cytoplasts stimulated us to investigate their apoptosome pathway of cell death in more detail. Apaf-1 was present in the cytoplast lysate (Figure 8a, lane 3). At the same time, we were unable to detect any cytochrome c in cytoplasts, either by conventional Western blot or by cytochrome c immunoprecipitation (Figure 8a and b, lane 3), whereas cytochrome c was immunoprecipitated from the HL-60 and – to a minute extent – from neutrophil preparations (Figure 8b, lanes 1 and 2, respectively).
Discussion
In the present study, we investigated the role of mitochondria in neutrophil physiology. The neutrophil mitochondria appeared to be peculiar organelles compared to mitochondria in other cell types. The best known function of mitochondria is their leading role in cellular energy metabolism, that is, oxidative phosphorylation to produce ATP. The oxidative reactions proceed in the mitochondrial respiratory chain, which consists of several inner membrane-embedded enzymatic complexes. In neutrophils, the mitochondria hardly contribute to the ATP level, as was evident from experiments with specific inhibitors of different respiratory complexes (Figure 1). They also lack activity of marker enzymes such as GDH and fumarase (Figure 2). At the same time, an important component of the outer mitochondrial membrane, porin, which regulates the transmembrane ion flow,21 is expressed in neutrophils, proving the presence of mitochondria in these cells (Figures 7 and 8a). The mitochondria in neutrophils do maintain Δψm, which is sensitive to CCCP and to valinomycin (Figure 3; see below). Furthermore, employing the real-time quantitative PCR, we discovered that neutrophils possess mtDNA, an indispensable and absolute marker of mitochondria. This technique also demonstrated that the mitochondria in neutrophils are much less abundant than in other primary leukocytes or HL-60 cells (Figure 4), but their number is higher than 5–6 per cell, as previously estimated by electron microscopy.30
A growing body of evidence demonstrates that mitochondria combine well-known metabolic functions with an involvement in the control of cell death.1 In neutrophils, the mitochondria lack life-supporting activity, but regulate neutrophil cell death, thus representing an exceptional type of organelle. The neutrophil mitochondria express and release into the cytosol a number of proapoptotic proteins during apoptosis, among which are cytochrome c, Smac/DIABLO and Omi/HtrA2 (see below). This was established only after we prevented the loss of Western blot signal due to nonspecific proteolysis by the addition of DFP. Nonspecific degradation of other proteins, including for instance STAT20 and procaspase-3,7 leading to loss of their detection, has been reported. This underscores that in neutrophils, which possess a powerful proteolytic potential, the absence of protein detection does not necessarily indicate that a protein is not expressed. Indeed, the use of the DFP-treated neutrophil lysates enabled us to detect the mitochondrial proapoptotic effector Smac and caspase-9 (Figures 7 and 9), whereas other investigators7,24 have failed to detect these in neutrophils.
Cytochrome c is believed to be one of the principal apoptotic players. It is released from mitochondria upon an apoptotic insult and participates in the assembly of the apoptosome to promote caspase-9 activation.31,32 However, the present data and the results from other studies7,24,25 indicate that neutrophils express an extremely low amount of cytochrome c. In our hands, cytochrome c was only detectable by Western blot after concentration procedures such as subcellular fractionation or immunoprecipitation (see Figures 5, 7 and 8b). Moreover, during the DMSO-induced neutrophilic differentiation of HL-60 cells, we observed a gradual depletion of cytochrome c expression, coinciding with increased expression of the NADPH-oxidase system and elongation of mitochondria (see Figure 6). This was not a nonspecific loss of signal due to an increase of proteolytic capacity in maturing cells, because the level of other tested proteins remained stable. Probably, the cytochrome c deficiency is a ‘genuine’ feature of mature neutrophils, which may explain particular features of their physiology.
A lack of cytochrome c means a lack of the mitochondrial respiratory chain complex IV activity, which was indeed undetectable in neutrophils by a cytochrome c-oxidase activity assay33 (data not shown). Theoretically, this situation (absence or lack of cytochrome c) may lead to accumulation of electrons in the respiratory chain and subsequent formation of reactive oxygen species (ROS), if the other respiratory complexes, which do not need cytochrome c, are still active. The latter is currently under investigation, although we expect that cytochrome c-independent mitochondrial complexes are likely to preserve some activity in neutrophils, because mitochondria-derived ROS have been shown to mediate the TNF-α-induced caspase-independent neutrophil cell death.6 In this respect, also a high expression of the mitochondrial anti-oxidant enzyme MnSOD in neutrophils seems to be logical (see Figure 5, lane 4 and Murphy et al.24), because this enzyme may have the important physiological role of inactivating excessive ROS in the absence of the functional ‘natural’ sink of electrons – complex IV. Increased oxidant injury due to loss of the protective function of MnSOD has been proposed to play a role in glucocorticoid-induced apoptosis of eosinophils,34 which are believed to have a defective mitochondrial respiration like neutrophils.4
Neutrophil mitochondria lacking cytochrome c and having no complex IV activity do, however, create Δψm (Figure 3), although the underlying mechanism remains unclear. It has been hypothesized that eosinophils, close ‘relatives’ of neutrophils, which also rely on glycolysis for their energy demands, use ATP transported from the cytoplasm into the mitochondria to maintain Δψm.4 However, this hypothesis seems not to be applicable to neutrophils, because the inhibitor of the mitochondrial adenine translocator, bongkrekic acid, which blocks the ATP transport to the mitochondrial matrix, had no effect on Δψm in neutrophils (not shown). Similarly, inhibition of glycolysis by sodium iodoacetate did not influence Δψm in neutrophils (during a 90 min incubation), despite a 99% depletion of ATP (not shown). More likely, here is again a role for the remaining respiratory complexes, whose proton-pumping activity may control Δψm. In agreement with this suggestion is the sensitivity of the neutrophil Δψm to uncouplers or K+ ionophores, such as CCCP and valinomycin, observed by us (see Figure 3) and others.3,35
The cytochrome c deficiency raised the question about functionality of the intrinsic (mitochondrial) pathway of apoptosis in neutrophils, which has not yet been studied before. This pathway is initiated by release of cytochrome c from the mitochondria, promoting the oligomerization of Apaf-1 and recruitment of the caspase-9 zymogen. Such a multimolecular complex consisting of cytochrome c, Apaf-1 and caspase-9 is called an apoptosome and contains enzymatically active caspase-9.32 Our present results indicate that caspase-9 is activated in neutrophils during either spontaneous or TNF-α-induced apoptosis despite the scarcity of cytochrome c (Figure 9). This finding suggests that the intrinsic death pathway in neutrophils is different from that in other cell types. While this manuscript was in preparation, Murphy et al.24 have published a study in which they proposed that, in neutrophils, the cytochrome-c-dependent apoptotic pathway displays a dramatic reduction in the requirement for cytochrome c. It was suggested that neutrophils have a lowered threshold requirement for cytochrome c, and their low content of cytochrome c is partially compensated by the increased expression of Apaf-1.24 This is in keeping with the present results, which show a relatively high content of Apaf-1 in neutrophils in comparison to HL-60 cells (Figure 8a), and with the hypothesis that upregulation of Apaf-1 contributes to the increased sensitivity of apoptosome activation to cytochrome c.36 On the other hand, neutrophil-derived cytoplasts, which are devoid of any detectable cytochrome c (Figure 8), still displayed intact activation of caspase-9 (Figure 9). Perhaps, the apoptosome pathway of caspase-9 activation in neutrophils demands even less cytochrome c than has been proposed.24 Although we cannot rule out the possibility that cytoplasts contain an exceptionally low number of cytochrome c molecules, we believe that, in neutrophils and neutrophil-derived cytoplasts, cytochrome c-independent caspase-9 activation may occur. The fact that, in cytochrome c−/− cells, stress-induced apoptosis (i.e. the intrinsic death pathway) is attenuated but not abrogated,37 suggests the existence of additional mechanisms, which are cytochrome c-independent and can mediate the intrinsic activation of caspases. Capsase-9 processing and activity has not been studied in the cytochrome c−/− cells,37 but a cell-free system of endoplasmic reticulum stress-induced apoptosis, lacking cytochrome c and Apaf-1, has reportedly been capable of caspase-9 cleavage.38 Thus, the mechanism of caspase-9 activation in neutrophils requires further clarification, because the existing experimental data do not allow a firm conclusion whether cytochrome c is required for it or not. Nevertheless, whatever the activation mechanism is, caspase-9 seems to play an important role in neutrophil apoptosis since caspase-9 (and caspase-3) activation precedes the activation of caspase-8, at least after TNF-α/CHX treatment (N.A.M., unpublished data). Hence, neutrophils likely belong to the type II cells.39 This finding also circumstantially underscores the importance of mitochondria in the neutrophil cell death machinery, irrespective of the precise role of these organelles – inducers or amplifiers of caspase activation.
The questionable role of cytochrome c in neutrophil apoptosis advances other mitochondrial proteins to the scene. The present results show a massive release of the mitochondrial proapoptotic effector proteins Smac/DIABLO and Omi/HtrA240,41,42,43,44,45 into the cytosol during neutrophil apoptosis (Figure 7). Both proteins are capable of promoting caspase-9 activation by binding to inhibitor of apoptosis proteins (IAPs)46 and removing, therefore, their inhibitory activity. Probably, this mechanism controls the intrinsic pathway of apoptosis in neutrophils, since the expression of several members of the IAP family has recently been reported in these cells.24,47,48 Moreover, delay of neutrophil apoptosis due to impaired degradation of XIAP has been associated with the pathological neutrophil accumulation in chronic neutrophilic leukemia,46,47 underlining the importance of IAP-dependent regulation of neutrophil cell death. At the same time, an intact activation of caspase-9 in cytoplasts, which are devoid of mitochondrial structures (porin), does not exclude that a cytoplasmic factor also might be involved. However, as mentioned above, some leakage of proteins from mitochondria during cytoplast preparation cannot be ruled out.
In conclusion, our present results indicate that neutrophil mitochondria, although deficient in life-maintaining functions and limited in number, still preserve the potential to support apoptotic caspase activation. Further studies are required to fully elucidate the unusual physiology of neutrophil mitochondria.
Materials and Methods
Cell preparation and culture
Neutrophils were isolated from heparinized venous blood of healthy volunteers49 after obtaining informed consent as described. Peripheral blood mononuclear cells (PBMCs) and platelets were removed by density gradient centrifugation over isotonic Percoll (Pharmacia, Uppsala, Sweden) with a specific gravity of 1.078 g/ml, which decreased the PBMC contamination of neutrophil preparations to about 0.2%, as assessed by flow cytometry. PBMCs were separated into monocytes and lymphocytes by means of elutriation centrifugation.50 Both preparations were more than 95% pure. For induction of apoptosis, 1 ml of neutrophil cell suspension (5 × 106/ml) in Iscove's modified Dulbecco's medium (complete IMDM5) was added to a 24-well plate and treated with a combination of tumor necrosis factor α (TNF-α; 50 ng/ml; Calbiochem, Bad Soden, Germany) and cycloheximide (CHX; 2 μg/ml; Calbiochem) in a humidified CO2 incubator at 37°C for 3 h, or left untreated for 16–18 h at 37°C.
Cytoplasts were prepared by ultracentrifugation over a discontinuous Ficoll-70 gradient.5 For culturing, cytoplasts were resuspended at a final concentration of 10 × 106/ml in complete IMDM, and were incubated overnight (16–18 h) at 37°C.
Neutrophilic maturation of the HL-60 cell line was induced in the exponentially growing cells, which were seeded at 0.5 × 106 cells/ml of the IMDM complete containing 1.25% dimethyl sulfoxide (DMSO; J.T. Baker BV, Deventer, The Netherlands).51 Fresh medium with DMSO was added every other day of culture to prevent cell overgrowth.
Apoptosis was induced in undifferentiated HL-60 cells by treatment with 100 μM etoposide (Calbiochem) for 4–5 h.
ATP concentration
ATP concentration was measured by a luciferase-based bioluminescence assay, as described.4
Measurement of enzymatic activity of GDH, LDH and fumarase
Cells were lysed in PBS containing 1% Triton-X100 (v/v; T-X100; Sigma, St. Louis, MO, USA), at a concentration of 10–100 × 106/ml for 10–15 min on ice. After a 5-min centrifugation at 22 000 × g, the supernatants were collected, and protein concentration was determined by a BCA protein assay kit (Pierce, Rockford, IL, USA). GDH52 and LDH53 reactions were assessed in a transparent 96-well plate. An aliquot of the cell extract (∼50 μg protein for GDH and ∼5 μg protein for LDH) diluted in 50 mM potassium phosphate buffer (PPB; pH 7.4) was added to a well preloaded with: for GDH measurement – 110 μl of reaction mixture (20 mM NH4Cl, 0.5 mM ADP in PPB) and 20 μl NADH (2.1 mg/ml); for LDH measurement – 120 μl PPB and 10 μl NADH. Reactions were started by addition of 20 μl of an appropriate substrate (5 mM α-ketoglutarate or 1 mM pyruvate (final concentrations) for GDH or LDH reaction, respectively). The decrease in absorbance (optical density, OD) at 340 nm, resulting from conversion of NADH to NAD, was monitored at 10-s intervals for 5 min by the HTS7000+ plate reader (Perkin Elmer, Norwalk, CT, USA), and expressed as −ΔOD340 nm per min.
Fumarase activity was assessed as described,54 in a cuvette of 1 cm light path containing 950 μl of 50 mM L-malate in PPB and 50 μl (∼50 μg protein) of a cell extract. The increase in absorbance at 250 nm (ΔOD250 nm) was recorded at 10-s intervals for 5 min by a spectrophotometer (Lambda 2; Perkin-Elmer).
Mitochondrial stainings
To assess the mitochondrial transmembrane potential (Δψm), an equal number of neutrophils or HL-60 cells (1 × 106) were resuspended in 1 ml HEPES buffer5 containing 1 μg/ml JC-1 (Molecular Probes; Eugene, OR, USA), and incubated for 15 min at 37°C in a water bath. After washing, the cells were resuspended in 1 ml of stain-free HEPES. The resulting cell suspensions (50 μl) were added to a 96-well plate, and the fluorescence was measured as a time 0 point by the HTS7000+ plate reader (Perkin-Elmer; Ex 485 nm; Em JC-1-Red 590 nm, Em JC-1-Green 535 nm). Afterwards, 50 μl of carbonyl cyanide 3-chlorophenylhydrazone (CCCP; Calbiochem) or valinomycin (Sigma), both at a final concentration of 5 μM, or buffer were added to the wells, and the fluorescence was assessed every 2 min for 20 min. For each time point, a red/green fluorescence ratio was calculated.
To evaluate the shape of the mitochondria during HL-60 maturation, the cells were stained with 100 μM MitoTracker GreenFM (Molecular Probes), and were analyzed by a confocal laser-scanning microscope (LSM510, Carl Zeiss, Heidelberg, Germany), as described.5
Measurement of NADPH-oxidase activity
The PMA-induced NADPH-oxidase activity during HL-60 maturation was assessed with a plate reader fluorimetric assay, based on hydrogen peroxide-mediated oxidation of Amplex Red (Molecular Probes).29
Measurement of apoptosis
Apoptosis was assessed by flow cytometry with the Annexin-V-fluorescein isothiocyanate (FITC)/propidium iodide (PI) kit (Bender MedSystems, Vienna, Austria), or by morphological evaluation of cytospins stained with May–Grünwald–Giemsa solution, as described.6 Cytoplast apoptosis was assessed by Annexin-V-FITC binding, without the PI step.
Subcellular fractionation and Western blotting
Whole-cell lysates were prepared as follows. The cell pellets were resuspended in a protease inhibitor mixture (PIM; one tablet of Complete Mini protease inhibitor cocktail (Roche, Mannheim, Germany) in 5 ml of PBS containing 5 mM EDTA) with or without 2 mM diisopropyl fluorophosphate (DFP; Acros Organics, New Jersey, NJ, USA), and incubated for 15 min on ice before lysis. The neutrophil+HL-60 colysates shown in Figure 5, lanes 3 and 6, were prepared by pelleting these cells together in the same tube. After addition of an equal amount of 2 × SDS sample buffer (SDS-SB) with 4% mercaptoethanol, the preparations were boiled for 15 min and kept at −20°C before use.
To obtain subcellular fractions, cells treated under various conditions were washed in ice-cold PBS and resuspended in the ice-cold cytosol extraction buffer (250 mM sucrose, 70 mM KCl, 250 μg/ml digitonin, PIM, 2 mM DFP in PBS) at final concentrations of 100 × 106/ml (neutrophils) and 40 × 106/ml (HL-60). After a 10–15 min incubation on ice, when >90% cells became trypan blue positive, the preparations were spun at 1000 × g for 5 min, and the supernatants were kept as cytosolic fractions. The pellets were resuspended in the same volume (as the cytosol extraction buffer) of the ice-cold mitochondria lysis buffer (100 mM NaCl, 10 mM MgCl2·6H2O, 2 mM EGTA, 2 mM EDTA, 1% NP-40 (v/v), 10% glycerol (v/v), PIM, 2 mM DFP in 50 mM Tris, pH 7.5) and incubated for 10 min on ice, followed by a 10-min centrifugation at 10 000 × g. The supernatants were taken as mitochondrial fractions. To prepare samples for Western blotting, 24 μl of either the cytosolic or the mitochondrial fraction were mixed with 8 μl of 4 × SDS-SB, containing 8% mercaptoethanol, and boiled for 5 min. Pellet fractions, which contained unsolubilized proteins, were obtained from the pellets remaining after the mitochondria lysis step, by addition of PIM+DFP in a volume equal to that of the cytosol extraction buffer used for the cytosolic fraction preparation. After addition of 4 × SDS-SB, the samples were boiled for 5 min and kept at −20°C before use.
Western blotting was performed as described.5 The blots were probed with monoclonal Ab against cytochrome c (7H8.2C12; Pharmingen, San Diego, CA, USA), porin (20B12; Molecular Probes), caspase-8 (1C12; Cell Signaling Technology, Beverly, MA, USA), polyclonal Ab against Smac/DIABLO (Ab-1, Oncogene, San Diego, CA, USA), AIF (H-300; Santa Cruz Biotechnology, Santa Cruz, CA, USA), Bax, Apaf-1, caspase-3 (Pharmingen), Mn superoxide dismutase (MnSOD; Stressgen, Canada), total and cleaved caspase-9 (Cell Signaling Technology). All monoclonal Abs were used at a final concentration of 1 μg/ml, and polyclonal Abs at a dilution of 1 : 1000. Anti-Omi/HtrA2 polyclonal Ab40 was used at a dilution of 1 : 5000.
Cytochrome c immunoprecipitation (IP)
Cells (10 × 106 neutrophils; 25 × 106 cytoplasts; 4 × 106 HL-60) were lysed in 750 μl of IP lysis buffer (100 mM NaCl, 10 mM MgCl2·6H2O, 1% NP-40 (v/v), 10% glycerol (v/v), PIM, 2 mM DFP in 50 mM Tris, pH 7.5) for 15 min on ice. After a 10-min centrifugation at 20 000 × g, the supernatants were precleared by continuous rotation for 1 h with 30 μl of a 50% slurry of protein G sepharose beads (Amersham Pharmacia Biotech, Uppsala, Sweden). IP was performed from ∼100 μg of total protein with 5 μg anticytochrome c monoclonal Ab (6H2.B4; BD Pharmingen) during a 1-h incubation under rotation at 4°C, and the precipitates were washed three times in the IP lysis buffer. Afterwards, the complexes were boiled for 5 min in 30 μl of SDS-SB with 2% mercaptoethanol, spun down, and 10 μl of the resulting supernatants were loaded on 15% SDS-PAGE with subsequent Western blotting.
Quantitative real-time PCR
Quantitative real-time PCR was performed as described.17 Total DNA was extracted from purified neutrophils, HL-60 cells or PBMC with the QIAamp DNA mini kit (Qiagen, Valencia, CA, USA). For each DNA extract, the nuclear gene human albumin and the mitochondrial gene human cytochrome-c oxidase subunit I (CCOI) were quantified separately by real-time quantitative PCR using a Roche LightCycler (Roche Applied Science, Laval, Que, Canada). For the CCOI gene, the CCOI-F 5′CTC CCA CCC TGG AGC CTC CGT AGA C3′ and CCOI-R 5′GGG AGA TTA TTC CGA AGC CTG GTA G3′ primers were used for PCR amplification. The mitochondrial DNA (mtDNA) copy number per cell was calculated as the ratio between the number of CCOI copies and the number of albumin copies.55 Specificity of the CCOI PCR product was confirmed by sequence analysis (not shown).
Abbreviations
- Ab:
-
antibody
- CCOI:
-
cytochrome-c oxidase subunit I
- CHX:
-
cycloheximide
- DFP:
-
diisopropyl fluorophosphate
- Δψm:
-
transmembrane mitochondrial potential
- GDH:
-
glutamate dehydrogenase
- IP:
-
immunoprecipitation
- LDH:
-
lactate dehydrogenase
- mtDNA:
-
mitochondrial DNA
- PI:
-
propidium iodide
- PIM:
-
protease inhibitor mixture
- ROS:
-
reactive oxygen species
- TNF-α:
-
tumor necrosis factor α
- TTFA:
-
thenoyltrifluoroacetone
References
Newmeyer DD and Ferguson-Miller S (2003) Mitochondria: releasing power for life and unleashing the machineries of death. Cell 112: 481–490
Borregaard N and Herlin T (1982) Energy metabolism of human neutrophils during phagocytosis. J. Clin. Invest. 70: 550–557
Fossati G, Moulding DA, Spiller DG, Moots RJ, White MRH and Edwards SW (2003) The mitochondrial network of human neutrophils: role in chemotaxis, phagocytosis, respiratory burst activation, and commitment to apoptosis. J. Immunol. 170: 1964–1972
Peachman KK, Lyles DS and Baas DA (2001) Mitochondria in eosinophils: functional role in apoptosis but not respiration. Proc. Natl. Acad. Sci. USA 98: 1717–1722
Maianski NA, Mul FPJ, van Buul JD, Roos D and Kuijpers TW (2002) Granulocyte colony-stimulating factor inhibits the mitochondria-dependent activation of caspase-3 in neutrophils. Blood 99: 672–679
Maianski NA, Roos D and Kuijpers TW (2003) Tumor necrosis factor alpha induces a caspase-independent death pathway in human neutrophils. Blood 101: 1987–1995
Pryde JG, Walker A, Rossi AG, Hannah S and Haslett C (2000) Temperature-dependent arrest of neutrophil apoptosis. Failure of Bax insertion into mitochondria at 15°C prevents the release of cytochrome c. J. Biol. Chem. 275: 33574–33584
Adachi S, Kubota M, Wakazono Y, Hirota H, Matsubara K, Kuwakado K, Akiyama Y and Mikawa H (1993) Mechanism of enhancement of neutrophil survival by granulocyte colony-stimulating factor and adenine. Exp. Hematol. 21: 1213–1218
Schulze-Osthoff K, Bakker AC, Vanhaesebroeck B, Beyaert R, Jacob WA and Fiers W (1992) Cytotoxic activity of tumor necrosis factor is mediated by early damage of mitochondrial functions. Evidence for the involvement of mitochondrial radical generation. J. Biol. Chem. 267: 5317–5323
Hochachka PW, Bianconcini MS, Parkhouse WS and Dobson GP (1991) On the role of actomyosin ATPases in regulation of ATP turnover rates during intense exercise. Proc. Natl. Acad. Sci. USA 88: 5764–5768
McEnery MW, Dawson TM, Verma A, Gurley D, Colombini M and Snyder SH (1993) Mitochondrial voltage-dependent anion channel. Immunochemical and immunohistochemical characterization in rat brain. J. Biol. Chem. 268: 23289–23296
Siskind LJ, Kolesnick RN and Colombini M (2002) Ceramide channels increase the permeability of the mitochondrial outer membrane to small proteins. J. Biol. Chem. 277: 26796–26803
Collins JM and Foster KA (1983) Differentiation of promyelocytic (HL-60) cells into mature granulocytes: mitochondrial-specific rhodamine 123 fluorescence. J. Cell Biol. 96: 94–99
Li N, Ragheb K, Lawler G, Sturgis J, Rajwa B, Melendez JA and Robinson JP (2003) Mitochondrial complex I inhibitor rotenone induces apoptosis through enhancing mitochondrial reactive oxygen species production. J. Biol. Chem. 278: 8516–8525
Reers M, Smiley ST, Mottola-Hartshorn C, Chen A, Lin M and Chen LB (1995) Mitochondrial mebrane potential monitored by JC-1 dye. Methods Enzymol. 26: 406–417
Salvioli S, Ardizzoni A, Franceschi C and Cossarizza A (1997) JC-1, but not DiOC6(3) or rhodamine 123, is a reliable fluorescent probe to assess delta psi changes in intact cells: implications for studies on mitochondrial functionality during apoptosis. FEBS Lett. 411: 77–82
Cote HC, Brumme ZL, Craib KJ, Alexander CS, Wynhoven B, Ting L, Wong H, Harris M, Harrigan PR, O'Shaughnessy MV and Montaner JS (2002) Changes in mitochondrial DNA as a marker of nucleoside toxicity in HIV-infected patients. N. Engl. J. Med. 346: 811–820
Anderson S, Bankier AT, Barrell BG, de Bruijn MH, Coulson AR, Drouin J, Eperon IC, Nierlich DP, Roe BA, Sanger F, Schreier PH, Smith AJ, Staden R and Young IG (1981) Sequence and organization of the human mitochondrial genome. Nature 290: 457–465
Ravagnan L, Roumier T and Kroemer G (2002) Mitochondria, the killer organelles and their weapons. J. Cell Physiol. 192: 131–137
McDonald PP, Bovolenta C and Cassatella MA (1998) Activation of distinct transcription factors in neutrophils by bacterial LPS, interferon-gamma, and GM-CSF and the necessity to overcome the action of endogenous proteases. Biochemistry 37: 13165–13173
Blachly-Dyson E and Forte M (2001) VDAC channels. IUBMB Life 52: 113–118
Hanson BJ, Carrozzo R, Piemonte F, Tessa A, Robinson BH and Capaldi RA (2001) Cytochrome c oxidase-deficient patients have distinct subunit assembly profiles. J. Biol. Chem. 276: 16296–16301
Wong GH, Elwell JH, Oberley LW and Goeddel DV (1989) Manganous superoxide dismutase is essential for cellular resistance to cytotoxicity of tumor necrosis factor. Cell 58: 923–931
Murphy BM, O'Neill AJ, Adrain C, Watson RW and Martin SJ (2003) The apoptosome pathway to caspase activation in primary human neutrophils exhibits dramatically reduced requirements for cytochrome c. J. Exp. Med. 197: 625–632
Liu CY, Takemasa A, Liles WC, Goodman RB, Jonas M, Rosen H, Chi E, Winn RK, Harlan JM and Chuang PI (2003) Broad-spectrum caspase inhibition paradoxically augments cell death in TNF-alpha-stimulated neutrophils. Blood 101: 295–304
Yamashita K, Takahashi A, Kobayashi S, Hirata H, Mesner Jr PW, Kaufmann SH, Yonehara S, Yamamoto K, Uchiyama T and Sasada M (1999) Caspases mediate tumor necrosis factor-alpha-induced neutrophil apoptosis and downregulation of reactive oxygen production. Blood 93: 674–685
Suzuki K, Hasegawa T, Sakamoto C, Zhou YM, Hato F, Hino M, Tatsumi N and Kitagawa S (2001) Cleavage of mitogen-activated protein kinases in human neutrophils undergoing apoptosis: role in decreased responsiveness to inflammatory cytokines. J. Immunol. 166: 1185–1192
Thornberry NA, Rano TA, Peterson EP, Rasper DM, Timkey T, Garcia-Calvo M, Houtzager VM, Nordstrom PA, Roy S, Vaillancourt JP, Chapman KT and Nicholson DW (1997) A combinatorial approach defines specificities of members of the caspase family and granzyme B. Functional relationships established for key mediators of apoptosis. J. Biol. Chem. 272: 17907–17911
Kuijpers TW, Maianski NA, Tool AT, Smit GPA, Rake JP, Roos D and Visser G (2003) Apoptotic neutrophils in the circulation of patients with glycogen storage disease type 1b (GSD1b). Blood 101: 5021–5024
Korchak HM, Roos D, Giedd KN, Wynkoop EM, Vienne K, Rutherford LE, Buyon JP, Rich AM and Weissmann G (1983) Granulocytes without degranulation: neutrophil function in granule-depleted cytoplasts. Proc. Natl. Acad. Sci. USA 80: 4968–4972
Liu X, Kim CN, Yang J, Jemmerson R and Wang X (1996) Induction of apoptotic program in cell-free extracts: requirement for dATP and cytochrome c. Cell 86: 147–157
Adams JM and Cory S (2002) Apoptosomes: engines for caspase activation. Curr. Opin. Cell Biol. 14: 715–720
Storrie B and Madden EA (1990) Isolation of subcellular organelles. Methods Enzymol. 182: 203–225
Gardai SJ, Hoontrakoon R, Goddard CD, Day BJ, Chang LY, Henson PM and Bratton DL (2003) Oxidant-mediated mitochondrial injury in eosinophil apoptosis: enhancement by glucocorticoids and inhibition by granulocyte-macrophage colony-stimulating factor. J. Immunol. 170: 556–566
Lavastre V, Pelletier M, Saller R, Hostanska K and Girard D (2002) Mechanisms involved in spontaneous and Viscum album agglutinin-I-induced human neutrophil apoptosis: Viscum album agglutinin-I accelerates the loss of antiapoptotic Mcl-1 expression and the degradation of cytoskeletal paxillin and vimentin proteins via caspases. J. Immunol. 168: 1419–1427
Green DR and Evan GI (2002) A matter of life and death. Cancer Cell 1: 19–30
Li K, Li Y, Shelton JM, Richardson JA, Spencer E, Chen ZJ, Wang X and Williams RS (2000) Cytochrome c deficiency causes embryonic lethality and attenuates stress-induced apoptosis. Cell 101: 389–399
Rao RV, Castro-Obregon S, Frankowski H, Schuler M, Stoka V, del Rio G, Bredesen DE and Ellerby HM (2002) Coupling endoplasmic reticulum stress to the cell death program. An Apaf-1-independent intrinsic pathway. J. Biol. Chem. 277: 21836–21842
Scaffidi C, Fulda S, Srinivasan A, Friesen C, Li F, Tomaselli KJ, Debatin KM, Krammer PH and Peter ME (1998) Two CD95 (APO-1/Fas) signaling pathways. EMBO J. 17: 1675–1687
Hegde R, Srinivasula SM, Zhang Z, Wassell R, Mukattash R, Cilenti L, DuBois G, Lazebnik Y, Zervos AS, Fernandes-Alnemri T and Alnemri ES (2002) Identification of Omi/HtrA2 as a mitochondrial apoptotic serine protease that disrupts inhibitor of apoptosis protein–caspase interaction. J. Biol. Chem. 277: 432–438
Du C, Fang M, Li Y, Li L and Wang X (2000) Smac, a mitochondrial protein that promotes cytochrome c-dependent caspase activation by eliminating IAP inhibition. Cell 102: 33–42
Verhagen AM, Ekert PG, Pakusch M, Silke J, Connolly LM, Reid GE, Moritz RL, Simpson RJ and Vaux DL (2000) Identification of DIABLO, a mammalian protein that promotes apoptosis by binding to and antagonizing IAP proteins. Cell 102: 43–53
Suzuki Y, Imai Y, Nakayama H, Takahashi K, Takio K and Takahashi R (2001) A serine protease, HtrA2, is released from the mitochondria and interacts with XIAP, inducing cell death. Mol. Cell 8: 613–621
Martins LM, Iaccarino I, Tenev T, Gschmeissner S, Totty NF, Lemoine NR, Savopoulos J, Gray CW, Creasy CL, Dingwall C and Downward J (2002) The serine protease Omi/HtrA2 regulates apoptosis by binding XIAP through a reaper-like motif. J. Biol. Chem. 277: 439–444
Verhagen AM, Silke J, Ekert PG, Pakusch M, Kaufmann H, Connolly LM, Day CL, Tikoo A, Burke R, Wrobel C, Moritz RL, Simpson RJ and Vaux DL (2002) HtrA2 promotes cell death through its serine protease activity and its ability to antagonize inhibitor of apoptosis proteins. J. Biol. Chem. 277: 445–454
Salvesen GS and Duckett CS (2002) IAP proteins: blocking the road to death's door. Nat. Rev. Mol. Cell Biol. 3: 401–410
Kobayashi S, Yamashita K, Takeoka T, Ohtsuki T, Suzuki Y, Takahashi R, Yamamoto K, Kaufmann SH, Uchiyama T, Sasada M and Takahashi A (2002) Calpain-mediated X-linked inhibitor of apoptosis degradation in neutrophil apoptosis and its impairment in chronic neutrophilic leukemia. J. Biol. Chem. 277: 33968–33977
Hasegawa T, Suzuki K, Sakamoto C, Ohta K, Nishiki S, Hino M, Tatsumi N and Kitagawa S (2003) Expression of the inhibitor of apoptosis (IAP) family members in human neutrophils: up-regulation of cIAP2 by granulocyte colony-stimulating factor and overexpression of cIAP2 in chronic neutrophilic leukemia. Blood 101: 1164–1171
Roos D and Voetman AA (1986) Preparation and cryopreservation of cytoplasts from human phagocytes. Methods Enzymol. 132: 250–257
de Boer M and Roos D (1986) Metabolic comparison between basophils and other leukocytes from human blood. J. Immunol. 136: 3447–3454
Arroyo A, Modriansky M, Serinkan FB, Bello RI, Matsura T, Jiang J, Tyurin VA, Tyurina YY, Fadeel B and Kagan VE (2002) NADPH oxidase-dependent oxidation and externalization of phosphatidylserine during apoptosis in Me2SO-differentiated HL-60 cells. Role in phagocytic clearance. J. Biol. Chem. 277: 49965–49975
Herrero-Yraola A, Bakhit SM, Franke P, Weise C, Schweiger M, Jorcke D and Ziegler M (2001) Regulation of glutamate dehydrogenase by reversible ADP-ribosylation in mitochondria. EMBO J. 20: 2404–2412
Brown SB, Clarke MC, Magowan L, Sanderson H and Savill J (2000) Constitutive death of platelets leading to scavenger receptor-mediated phagocytosis. A caspase-independent cell clearance program. J. Biol. Chem. 275: 5987–5996
Hill RL and Bradshaw RA (1969) Fumarase. Methods Enzymol. 13: 91–99
Meuer S, Wittwer C and Nakagawara K-I (Eds.) (2001) Rapid Cycle Real-Time PCR. Methods and Applications. (Heidelberg, Germany: Springer), 408pp
Acknowledgements
We are grateful to Dr. W Sluiter and Professor HR Scholte for fruitful collaboration. We thank M de Boer and R Dee for help in quantitative PCR, E Mul for technical assistance, and Dr. A Tool, Dr. A Verhoeven and Dr. K Krab for helpful suggestions.
Author information
Authors and Affiliations
Corresponding author
Additional information
Edited by JC Martinou
Rights and permissions
About this article
Cite this article
Maianski, N., Geissler, J., Srinivasula, S. et al. Functional characterization of mitochondria in neutrophils: a role restricted to apoptosis. Cell Death Differ 11, 143–153 (2004). https://doi.org/10.1038/sj.cdd.4401320
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.cdd.4401320
Keywords
This article is cited by
-
Mitochondrial and metabolic dysfunction of peripheral immune cells in multiple sclerosis
Journal of Neuroinflammation (2024)
-
The Role of Innate Immune Cells in Cardiac Injury and Repair: A Metabolic Perspective
Current Cardiology Reports (2023)
-
Neutrophil (dys)function due to altered immuno-metabolic axis in type 2 diabetes: implications in combating infections
Human Cell (2023)
-
The metabolic function of pyruvate kinase M2 regulates reactive oxygen species production and microbial killing by neutrophils
Nature Communications (2023)
-
Immunometabolic rewiring in tumorigenesis and anti-tumor immunotherapy
Molecular Cancer (2022)