Abstract
Brain ischemia induces apoptosis in neuronal cells, but the mechanism is not well understood. When wild-type mice were subjected to bilateral common carotid arteries occlusion (BCCAO) for 15 min, apoptosis-associated morphological changes and appearance of TUNEL-positive cells were observed in the striatum and in the hippocampus at 48 h after occlusion. RT-PCR analysis revealed that mRNAs for ER stress-associated proapoptotic factor CHOP and an ER chaperone BiP are markedly induced at 12 h after BCCAO. Immunohistochemical analysis showed that CHOP protein is induced in nuclei of damaged neurons at 24 h after occlusion. In contrast, ischemia-associated apoptotic loss of neurons was decreased in CHOP−/− mice. Primary hippocampal neurons from CHOP−/− mice were more resistant to hypoxia-reoxygenation-induced apoptosis than those from wild-type animals. These results indicate that ischemia-induced neuronal cell death is mediated by the ER stress pathway involving CHOP induction.
Similar content being viewed by others
Introduction
Neuronal cells are particularly vulnerable to ischemia and disturbance in the central nervous system leads to serious after-effects such as paresis, memory disturbance and even death can occur. Brain ischemia induces hypoxia and hypoglycemia, and depolarization of neuronal cell membrane, release of glutamate from neuron and axon can occur. Glutamate induces cell death by increasing [Ca2+]i in neurons,1,2 and production of free radicals such as nitric oxide (NO) and superoxide accelerates cell death cascade to apoptosis due to DNA fragmentation or mitochondrial disturbance.3 However, various therapies targeting glutamate receptors or maintenance of intracellular Ca2+ homeostasis had little effect.4
Neuronal cells have highly developed endoplasmic reticulum (ER).5 ER has several important functions involving glycosylation, formation of disulfide bonds, folding and assembly of newly synthesized secretory proteins. ER also serves as a cellular Ca2+ store. Perturbation of ER functions can induce cellular damages and result in cell death. Under various conditions such as disturbance of Ca2+ homeostasis, hypoxia, hypoglycemia and treatment with various agents, ER functions are disturbed and ER stress is induced.6,7
In an attempt to survive under ER stress conditions, cells have self-protective mechanisms against this stress. Induction of molecular chaperones in ER, translational attenuation and ER-associated degradation (ERAD), which are collectively termed ‘unfolded protein response’8,9 are involved. However, when cells are subjected to severe and prolonged ER stress, a proapoptotic factor CHOP/GADD153, a member of the C/EBP family of transcription factors, is induced and apoptosis follows in some cell types.10,11,12 CHOP is expressed at low levels under physiological conditions, but is strongly induced at the transcription level in response to ER stress.10 Transcriptional induction of the CHOP gene is one of the most important pathways leading to apoptosis.9,13 When cells are subjected to ER stress, three major sensor and transducer proteins on the ER membrane, including IRE1, ATF6 and PERK, are activated.14,15,16 CHOP exists downstream of all these three pathways, and overexpression of CHOP leads to growth arrest and apoptosis.8,17,18 CHOP was reported to increase the sensitivity to ER stress by decreasing Bcl-2 expression, and to enhance oxidant injury.19
We found that NO-induced apoptosis is mediated by the ER stress pathway involving CHOP.20,21,18 Impaired ER functions may cause various human diseases.22 We showed that ER stress-induced apoptosis in pancreatic β-cells leads to diabetes.12 In brain ischemia, neuronal cells cannot receive sufficient glucose and oxygen required for modification of proteins in ER, and ER stress may occur.23 The induction of CHOP mRNA by brain ischemia or hypoxia has been reported.24,25,26,27 However, the exact role of CHOP in ER stress-mediated neuronal apoptosis in brain ischemia or hypoxia remains to be clarified. We hypothesized that brain ischemia-induced apoptosis is mediated by the ER stress pathway including CHOP. We now report that brain ischemia in mice causes ER stress-mediated apoptosis of neuronal cells in the striatum and hippocampus, and that CHOP plays a crucial role in this cell death.
Results
Neuronal cell death is induced by 15 min-BCCAO in the mouse striatum and hippocampus
BCCAO is a simple method of global cerebral ischemia in mice compared with middle cerebral artery occlusion. It has been reported that BCCAO for 15–18 min causes extensive neuronal damage in C57BL/6 mice.28,29,30 To optimize the duration of BCCAO, survival rates of mice were examined after 10, 15 and 20 min-BCCAO. None of 10 min-BCCAO mice (n=9) had died at 7 days (mortality rate, 0%), and there were no apparent histological changes in the striatum and the hippocampus (data not shown). After 15 min-BCCAO, four of the nine mice died within 7 days (mortality rate, 44%), whereas after 20 min-BCCAO, seven of the nine mice died within 7 days (mortality rate, 78%). Based on our observations and previous reports, we used 15 min-BCCAO for all further analysis.
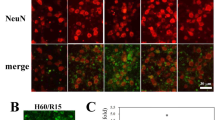
To assess ischemia-induced neuronal cell death in striatum and hippocampus, histological analysis with Nissl's staining was done. In the striatum at 7 days after 15 min-BCCAO, cells were diffusely shrunken and nuclei were irregularly condensed (Figure 1A, c and d). In hippocampal CA1 subfields, pyramidal neurons were scattered and shrunken, and the nuclei were markedly condensed (Figure 1A, g and h). To detect apoptosis, TUNEL and propidium iodide (PI) stainings were done. In the striatum, scattered TUNEL-positive cells appeared at 24 h after ischemic insult, increased at 48 h, and remained for up to 7 days. PI staining showed neuronal cells with normal morphologic properties exhibiting round nuclei at 0 h, but some cells began to shrink at 24 h and most nuclei were condensed at 48 h (Figure 1B). In the hippocampus, TUNEL-positive cells appeared in the medial area of the CA1 subfields at 48 h and extended to the lateral part of CA1 and CA3 subfields for up to 7 days (Figure 1C).
Induction of neuronal cell apoptosis by brain ischemia. (A) Induction of neuronal cell death is induced by 15 min-BCCAO in the mouse striatum and hippocampus. BCCAO was done in C57 BL/6 male mice (6–7 weeks old, 20–30 g), as described under Materials and Methods. Sham operation was done with the expose to bilateral common carotid arteries and without occlusion. Representative Nissl's stains in the striatum (a-d) and in the hippocampus (e-h) at 7 days after sham operation (a, b, e and f) or 15 min-BCCAO (c, d, g and h) are shown. b, d, f and h (× 200) are the magnification of squares in a, c, e and g (× 40), respectively. VT, ventricle; DG, dentate gyrus; so, stratum oriens; sp, stratum pyramidale; sr, stratum radiatum. (B) Brain ischemia-induced apoptosis in the striatum. Sequential apoptotic changes were observed with use of TUNEL and propidium iodide (PI) staining. Representative photographs at 0 h (sham; a and b), 24 h (c and d), 48 h (e and f), 4 days (g and h), and 7 days (i and j) after 15 min-BCCAO are shown (× 400). (C) Brain ischemia-induced apoptosis in the hippocampus. Sequential apoptotic changes were observed with use of TUNEL and propidium iodide (PI) staining. Representative photographs at 0 h (sham; a and b), 24 h (c and d), 48 h (e and f), 4 days (g and h), and 7 days (i and j) after 15 min-BCCAO are shown (× 400)
(Continued) Induction of neuronal cell apoptosis by brain ischemia. (A) Induction of neuronal cell death is induced by 15 min-BCCAO in the mouse striatum and hippocampus. BCCAO was done in C57 BL/6 male mice (6–7 weeks old, 20–30 g), as described under Materials and Methods. Sham operation was done with the expose to bilateral common carotid arteries and without occlusion. Representative Nissl's stains in the striatum (a-d) and in the hippocampus (e-h) at 7 days after sham operation (a, b, e and f) or 15 min-BCCAO (c, d, g and h) are shown. b, d, f and h (× 200) are the magnification of squares in a, c, e and g (× 40), respectively. VT, ventricle; DG, dentate gyrus; so, stratum oriens; sp, stratum pyramidale; sr, stratum radiatum. (B) Brain ischemia-induced apoptosis in the striatum. Sequential apoptotic changes were observed with use of TUNEL and propidium iodide (PI) staining. Representative photographs at 0 h (sham; a and b), 24 h (c and d), 48 h (e and f), 4 days (g and h), and 7 days (i and j) after 15 min-BCCAO are shown (× 400). (C) Brain ischemia-induced apoptosis in the hippocampus. Sequential apoptotic changes were observed with use of TUNEL and propidium iodide (PI) staining. Representative photographs at 0 h (sham; a and b), 24 h (c and d), 48 h (e and f), 4 days (g and h), and 7 days (i and j) after 15 min-BCCAO are shown (× 400)
Brain ischemia induces the ER stress-associated proapoptotic factor CHOP
Next, we determined if ischemia-induced neuronal apoptosis is mediated by the ER stress pathway by assessing expression of mRNAs for the ER stress-associated proapoptotic factor CHOP and an ER chaperone BiP in the striatum and in the hippocampus of C57 BL/6 (wild-type) mice using RT-PCR analysis (Figure 2). In the striatum, CHOP mRNA was expressed at a low level before treatment, began to increase at 6 h, increased markedly at 12 h, was somewhat decreased at 24 h, and clearly decreased at 48 h. BiP mRNA was similarly induced. In the hippocampus, CHOP mRNA was increased at 6 h, reached a maximum at 12 h, was somewhat decreased at 24 h, and decreased to a near control level at 48 h. No induction of CHOP and BiP mRNAs was seen at 12 h in sham-operated animals (data not shown).
Induction of CHOP and BiP mRNAs in the striatum and hippocampus of wild-type mice by brain ischemia. RT-PCR analysis was performed using total RNAs obtained from the striatum (A and B) and the hippocampus (C and D) at 0, 6, 12, 24, 48 and 96 h after 15 min-BCCAO. GAPDH mRNAs was used as an internal control. Results were quantified by densitometry, normalized for GAPDH mRNAs and are shown as mean±S.D. (n=6)
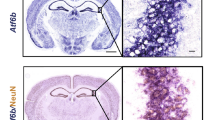
Expression of the CHOP protein in the striatum and in the hippocampal CA1 subfields was studied by means of an immunohistochemical analysis (Figure 3). CHOP was not detected in sham-operated mice (Figure 3A, a, c and B, a). In contrast, CHOP was detected in nuclei of cells in the striatum and hippocampal CA1 subfields at 24 h after BCCAO (Figure 3A, b, e and B, c). Most, but not all cells were positive for CHOP. CHOP-positive nuclei were morphologically normal, thereby suggesting that they are proapoptotic. In the hippocampal CA1 subfields, the cellular arrangements of the pyramidal layers were markedly disturbed and many nuclei were positive for CHOP at 24 h after BCCAO.
Immunohistochemical analysis of CHOP in the striatum and hippocampus after brain ischemia. Immunostaining of CHOP in superior regions of striatum (A, a and b; × 40), and CA1 (B, a and c; × 200) subfields in hippocampus in sham operated (A, a, c and B, a) and 15 min-BCCAO (A, b, e and B, c) mice was performed after 24 h. A, c and e are amplification (× 400) of the indicated regions in A, a and b, respectively. A, d, f and B, b, d show nuclear staining with propidium iodide (PI) of the same fields of A, c, e and B, a, c respectively. Arrows indicate representative cells positive for CHOP in nuclei
Disruption of the CHOP gene protects ischemia-induced neuronal cell death in mice
To examine a role of CHOP in ischemia-induced neuronal cell death in vivo, we used CHOP−/− mice. Table 1 shows physiological parameters during BCCAO in wild-type and CHOP−/− mice. There was no significant difference between wild-type and CHOP−/− mice in arterial blood pH, arterial blood gases (PaO2 and PaCO2), blood glucose and rectal temperature. Mean arterial blood pressure increased similarly in both wild-type and CHOP−/− mice during BCCAO. Regional cerebral blood flow decreased to about 22 and 18% of control in wild-type and CHOP−/− mice, respectively, during BCCAO. These results indicate that there is little difference in physiological parameters between wild-type and CHOP−/− mice during BCCAO.
To assess whether the ER stress pathway was activated in CHOP−/− mice after 15 min-BCCAO, we examined the expression of BiP mRNA by RT-PCR analysis (Figure 4). In both striatum and hippocampus, BiP mRNA was expressed at low levels before treatment, increased markedly at 6 h, somewhat decreased at 12 h, and further decreased at 24 h. These results confirm that the ER stress pathway is activated in CHOP−/− mice after ischemic insult.
Induction of BiP mRNAs in the striatum and hippocampus of CHOP−/− mice by brain ischemia. RT-PCR analysis was performed using total RNAs obtained from the striatum (A) and the hippocampus (B) at 0, 6, 12 and 24 h after 15 min-BCCAO. GAPDH mRNAs was used as an internal control. Results were quantified by densitometry, normalized for GAPDH mRNAs and are shown as mean±S.D. (n=3)
To examine the activation of the ER stress pathway upstream of CHOP induction in CHOP−/− mice and in wild-type mice, we performed RT-PCR analysis of XBP1 mRNA (Figure 5). XBP1 is a member of the CREB/ATF4 family of transcription factors, is specifically induced by ER stress. Upon ER stress, XBP1 mRNA is subjected to unique and specific splicing by activated IRE1, and the induced XBP1 activates the expression of the ER stress-response genes.31,32 XBP1 mRNA is also known to be induced by activated ATF6 and by XBP1 itself. Therefore, induction and splicing of XBP1 mRNA is a good marker of ER stress. In the hippocampus of wild-type and CHOP−/− mice, unspliced XBP1 mRNA was expressed at low levels before ischemic insult and spliced XBP1 mRNA was not detected. Unspliced XBP1 mRNA was markedly induced at 2 and 4 h in both wild-type and CHOP−/− mice, and spliced XBP1 mRNA was formed in both animals. In the striatum of wild-type and CHOP−/− mice, similar induction and splicing of XBP1 mRNA were observed (data not shown). These results confirm that 15 min-BCCAO activates the ER stress response pathway similarly in wild-type and CHOP−/− mice.
Induction and splicing of XBP1 mRNA in the hippocampus of wild-type and CHOP−/− mice by brain ischemia. RT-PCR analysis was performed using total RNAs from the hippocampus at 0, 2 and 4 h after 15 min-BCCAO with a primer set encompassing the spliced-out region in XBP1 mRNA. PCR products were resolved on 3% agarose gels to separate unspliced (XBP1u) and spliced (XBP1s, arrowheads) XBP1 mRNAs. PC12 cells treated with or without 1 μM thapsigargin (Tg) for 6 h were used as positive control. GAPDH mRNA was used as an internal control. M; size marker
We analyzed neuronal cell death in the striatum and in the hippocampal CA1 subfields by immunohistochemical analysis of Ca2+/calmodulin-dependent protein kinase IV (CaMKIV), an enzyme which is abundantly expressed in neurons. CaMKIV plays an important role as a multifunctional serine/threonine protein kinase such as activation of cAMP response element-binding protein (CREB), that is involved in hippocampal long-term potentiation.33 Many neuronal cells positive for CaMKIV were observed in the striatum of sham-operated mice (Figure 6A, a and d). In wild-type mice with 15 min-BCCAO, CaMKIV-positive cells disappeared in most areas of the striatum after 7 days, although they did remain in some areas (Figure 6A, b and e). In contrast, these cells were widely preserved in CHOP−/− mice, except for dorso-lateral region which is readily affected by ischemia (Figure 6A, c and f). The number of CaMKIV-positive cells in each hemisphere was counted and the average number was markedly decreased in wild-type mice after BCCAO (29% of sham-control mice), whereas this decrease was markedly attenuated in CHOP−/− mice (90% of sham) (Figure 6B,C). In some of both wild-type and CHOP−/− mice, the numbers of remaining CaMKIV-positive cells differed markedly between right and left hemispheres, probably because of patency of the posterior communicating artery hypoplasticity in the circle of Willis.28,29,30 CaMKIV-positive neurons were observed in the hippocampal CA1 subfields of sham-operated mice (Figure 7A, a). In CA1 pyramidal cells of wild-type mice with ischemia, CaMKIV-positive cells were frequently destroyed and disappeared (Figure 7A, b and e), yet were widely preserved in CHOP−/− mice (Figure 7A, c and f). When the numbers of CaMKIV-positive cells in each hemisphere were counted and averaged (Figure 7B,C), the average was markedly decreased in wild-type mice after BCCAO (27% of sham-control mice), whereas this decrease was attenuated in CHOP−/− mice (62% of sham). Therefore, in the striatum and the hippocampus, CHOP−/− mice are more resistant to brain ischemia, especially in the striatum. Loss of CaMKIV-positive cells induced by ischemia in each hemisphere was more asymmetric in hippocampus than in the striatum. This finding agrees well with documented data.30
Attenuation of ischemia-induced neuronal cell death in the striatum of CHOP−/− mice. (A) Ca2+/calmodulin-dependent protein kinase IV (CaMKIV) was immunostained as a marker of neuronal cells. Coronal slices (30 μm) of wild-type mouse with sham operation (a), wild-type mouse with 15 min-BCCAO (b) and CHOP−/− mouse with 15 min-BCCAO (c) were immunostained with an anti-CaMKIV antibody, and stains at anterior commissure level are shown. d, e and f are magnifications (× 200) of the squares indicated in a, b and c (× 40), respectively. (B) The striatum was divided into superior and inferior regions in each hemisphere, and CaMKIV-positive cells in each region were counted, as described under Materials and Methods. (C) The results in B were analyzed statistically and are shown as mean (n=2) for sham-operated mouse, and mean±S.D. (n=14) for wild-type and CHOP−/− mice with 15 min-BCCAO (*; P<0.01)
Attenuation of ischemia-induced neuronal cell death in the hippocampal CA1 subfield of CHOP−/− mice. (A) Coronal slices (30 μm) of wild-type mouse with sham operation (a and d), wild-type mouse with 15 min-BCCAO (b and e) and CHOP−/− mouse with 15 min-BCCAO (c and f), were immunostained with anti-CaMKIV antibody, and stains at the level of dorsal hippocampus were shown (a–c). Lower panels (d–f) show the nuclear staining with propidium iodide (PI) of the same fields. The PI-positive cells outside the hippocampus in e are infiltrating inflammatory cells and reactive astrocytes. (B) CaMKIV-positive cells in each CA1 subfield were counted, as described under Materials and Methods. (C) The results in B were analyzed statistically and are shown as the mean (n=2) for sham-operated mouse, and mean±S.D. (n=10) for wild-type and CHOP−/− mice with 15 min-BCCAO (*; P<0.05)
Primary neurons from CHOP−/− mice are resistant to hypoxia-reoxygenation-induced apoptosis
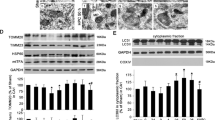
We examined the effects of hypoxia-reoxygenation on primary cultured neurons from wild-type and CHOP−/− mice. The hippocampal primary cultured neurons were subjected to hypoxia for 1 h and then reoxygenated for various periods. To assess the activation of the ER stress pathway under our experimental conditions, we examined expression of mRNAs for CHOP and BiP (Figure 8A). In primary cultured neurons from wild-type mice, CHOP mRNA was expressed at a low level after 1 h-hypoxia (reoxygenation for 0 h), began to increase at 2 h after reoxygenation, reached a maximum at 4 h, and decreased thereafter. No expression of CHOP mRNA was observed in CHOP−/− neurons. On the other hand, BiP mRNA was induced similarly in wild-type and CHOP−/− neurons. It was induced at 2–6 h after reoxygenation and decreased at 8 h. We next examined induction and splicing of XBP1 mRNA (Figure 8B). Induction of unspliced XBP1 mRNA and formation of the spliced form were observed after hypoxia-reoxygenation similarly in wild-type and CHOP−/− neurons.
Attenuation of apoptosis in primary cultured neuronal cells from CHOP−/− mice induced by hypoxia-reoxygenation. (A) Induction of CHOP and BiP mRNAs in primary cultured neurons. (a) RT-PCR analysis was performed using total RNAs of hippocampal primary cultured neurons from embryonic mice at days 16–18 of gestation. Cells were subjected to 1 h hypoxia followed by reoxygenation for indicated hours. Results for CHOP (b) and BiP (c) mRNAs were quantified and are shown as mean±S.D. (n=3). (B) Induction and splicing of XBP1 mRNA. RT-PCR analysis was performed as in Figure 5. (C) Hippocampal cells from wild-type (a–h) and CHOP−/− (i–p) mice at embryonic 16–18 days were cultured without cytosine arabinocide and subjected to 1 h hypoxia followed by reoxygenation for 0 h (a, e, i and m), 6 h (b, f, j and n), 9 h (c, g, k and o) and 12 h (d, h, l and p). Sequential morphological changes of neurons (a–d and i–l), and glial cells (e–h and m–p) were observed with double immunostaining using anti-microtubule associated protein 2 (MAP2) antibody and anti-glial fibrillary acidic protein (GFAP) antibody, respectively. a–d and i–l show the same fields of e–h and m–p, respectively. Bar; 100 μm. (D) The low magnification images of hippocampal neurons from wild-type (a) and CHOP−/− (b) mice. Primary cultured neurons were subjected to 1 h hypoxia followed by reoxygenation for 6 h, and immunostained with MAP2 antibody. Bar; 100 μm. (E) The hippocampal primary cultured neurons from wild-type (a and b) and CHOP−/− (c and d) mice were subjected to 1 h hypoxia and 9 h reoxygenation, and then stained with anti-MAP2 antibody (a and c). Apoptosis was detected by the TUNEL method (b and d). Bar; 20 μm. (F) Phosphorylation of JNK. Primary cultured neurons from wild-type and CHOP−/− mice were subjected to 1 h hypoxia followed by reoxygenation for indicated periods. Cells extracts were subjected to immunoblot analysis with antibodies against phosphorylated-JNK or JNK1 (arrows). Cells without hypoxia treatment were used as control (Cont)
We then examined hypoxia-reoxygenation-induced morphological changes in neurons and glial cells from wild-type and CHOP−/− mice by immunohistochemical analysis (Figure 8C). When cytosine arabinocide was omitted from the medium, neurons positive for microtubule-associated protein 2 (MAP2) and glial cells positive for glial fibrillary acidic protein (GFAP) grew. The number of neurons from wild-type mice was markedly decreased at 6 h after reoxygenation (Figure 8D, a), dendrites disappeared almost completely at 9 h, and cell bodies disappeared almost completely at 12 h. In contrast, many neurons from CHOP−/− mice were apparently intact at 6 h (Figure 8D, b), dendrites remained partly retained at 9 h, and many cell bodies remained at 12 h. This indicates that neurons from CHOP−/− mice are more resistant to hypoxia-reoxygenation-induced morphological changes and cell death than those from wild-type animals. On the other hand, glial cells from wild-type and CHOP−/− mice remained apparently intact at 9 h and underwent some morphological changes at 12 h. Therefore, glial cells were more resistant to hypoxia-reoxygenation than neurons. Wild-type neurons, which lost their dendrites at 9 h after reoxygenation, were positive for TUNEL staining, whereas CHOP−/− neurons at 9 h retaining almost dendrites were negative for TUNEL staining (Figure 8E). This indicates that primary cultured neurons undergo apoptotic cell death by hypoxia-reoxygenation.
(Continued) Attenuation of apoptosis in primary cultured neuronal cells from CHOP−/− mice induced by hypoxia-reoxygenation. (A) Induction of CHOP and BiP mRNAs in primary cultured neurons. (a) RT-PCR analysis was performed using total RNAs of hippocampal primary cultured neurons from embryonic mice at days 16–18 of gestation. Cells were subjected to 1 h hypoxia followed by reoxygenation for indicated hours. Results for CHOP (b) and BiP (c) mRNAs were quantified and are shown as mean±S.D. (n=3). (B) Induction and splicing of XBP1 mRNA. RT-PCR analysis was performed as in Figure 5. (C) Hippocampal cells from wild-type (a–h) and CHOP−/− (i–p) mice at embryonic 16–18 days were cultured without cytosine arabinocide and subjected to 1 h hypoxia followed by reoxygenation for 0 h (a, e, i and m), 6 h (b, f, j and n), 9 h (c, g, k and o) and 12 h (d, h, l and p). Sequential morphological changes of neurons (a–d and i–l), and glial cells (e–h and m–p) were observed with double immunostaining using anti-microtubule associated protein 2 (MAP2) antibody and anti-glial fibrillary acidic protein (GFAP) antibody, respectively. a–d and i–l show the same fields of e–h and m–p, respectively. Bar; 100 μm. (D) The low magnification images of hippocampal neurons from wild-type (a) and CHOP−/− (b) mice. Primary cultured neurons were subjected to 1 h hypoxia followed by reoxygenation for 6 h, and immunostained with MAP2 antibody. Bar; 100 μm. (E) The hippocampal primary cultured neurons from wild-type (a and b) and CHOP−/− (c and d) mice were subjected to 1 h hypoxia and 9 h reoxygenation, and then stained with anti-MAP2 antibody (a and c). Apoptosis was detected by the TUNEL method (b and d). Bar; 20 μm. (F) Phosphorylation of JNK. Primary cultured neurons from wild-type and CHOP−/− mice were subjected to 1 h hypoxia followed by reoxygenation for indicated periods. Cells extracts were subjected to immunoblot analysis with antibodies against phosphorylated-JNK or JNK1 (arrows). Cells without hypoxia treatment were used as control (Cont)
(Continued) Attenuation of apoptosis in primary cultured neuronal cells from CHOP−/− mice induced by hypoxia-reoxygenation. (A) Induction of CHOP and BiP mRNAs in primary cultured neurons. (a) RT-PCR analysis was performed using total RNAs of hippocampal primary cultured neurons from embryonic mice at days 16–18 of gestation. Cells were subjected to 1 h hypoxia followed by reoxygenation for indicated hours. Results for CHOP (b) and BiP (c) mRNAs were quantified and are shown as mean±S.D. (n=3). (B) Induction and splicing of XBP1 mRNA. RT-PCR analysis was performed as in Figure 5. (C) Hippocampal cells from wild-type (a–h) and CHOP−/− (i–p) mice at embryonic 16–18 days were cultured without cytosine arabinocide and subjected to 1 h hypoxia followed by reoxygenation for 0 h (a, e, i and m), 6 h (b, f, j and n), 9 h (c, g, k and o) and 12 h (d, h, l and p). Sequential morphological changes of neurons (a–d and i–l), and glial cells (e–h and m–p) were observed with double immunostaining using anti-microtubule associated protein 2 (MAP2) antibody and anti-glial fibrillary acidic protein (GFAP) antibody, respectively. a–d and i–l show the same fields of e–h and m–p, respectively. Bar; 100 μm. (D) The low magnification images of hippocampal neurons from wild-type (a) and CHOP−/− (b) mice. Primary cultured neurons were subjected to 1 h hypoxia followed by reoxygenation for 6 h, and immunostained with MAP2 antibody. Bar; 100 μm. (E) The hippocampal primary cultured neurons from wild-type (a and b) and CHOP−/− (c and d) mice were subjected to 1 h hypoxia and 9 h reoxygenation, and then stained with anti-MAP2 antibody (a and c). Apoptosis was detected by the TUNEL method (b and d). Bar; 20 μm. (F) Phosphorylation of JNK. Primary cultured neurons from wild-type and CHOP−/− mice were subjected to 1 h hypoxia followed by reoxygenation for indicated periods. Cells extracts were subjected to immunoblot analysis with antibodies against phosphorylated-JNK or JNK1 (arrows). Cells without hypoxia treatment were used as control
Finally, to assess the activation of another ER stress–mediated apoptosis pathway, we investigated the phosphorylation of c-Jun-N-terminal-kinase (JNK), one of the mitogen-activated protein kinase (MAPK) (Figure 8F). Upon ER stress, IRE1 is activated by autophosphorylation and the IRE1-TRAF2-ASK1 complex is formed, and the ASK1–JNK pathway is activated.34 In the primary cultured neurons from both mice, phosphorylated-JNK levels were moderately increased after 1 h hypoxia, remained high after reoxygenation for 10 min, and then decreased. The level of JNK remained little changed in wild-type and CHOP−/− neurons during treatment. These results indicate that the hypoxia-reoxygenation stress activates not only the CHOP pathway, but also the JNK pathway. We think this is the reason why hypoxia-reoxygenation-induced apoptosis is not completely inhibited in CHOP−/− neurons.
Discussion
In the present study, we found that brain ischemia induces neuronal cell death via ER stress in vivo and in vitro. There are several explanations regarding the mechanism of ischemia-induced ER stress. Ischemia results in deprivation of oxygen and glucose in neuronal cells and depletion of ATP can follow. ER functions as an intracellular Ca2+ store and plays an important role in Ca2+ homeostasis by pumping Ca2+ into ER lumen via sarcoplasmic/endoplasmic reticulum Ca2+-ATPase (SERCA), and by releasing Ca2+ from the ER by the inositol 1, 4, 5-trisphosphate (IP3) receptor and/or ryanodine receptor. When ATP is decreased, SERCA is inhibited and ER Ca2+ may be depleted. This depletion impairs protein folding in the ER and leads to ER stress.35 On the other hand, increased cytosolic Ca2+ presumably stimulates neuronal nitric oxide (NO) syntheses, and NO further depletes ER Ca2+.20 NO depletes ER Ca2+ probably by inhibiting Ca2+ uptake by SERCA36 or by stimulating Ca2+ release by the ryanodine receptor.37 IP3 receptor density is high in the hippocampal CA1 and in the striatum.36 We reported that overexpression of calreticulin, a major Ca2+ binding protein in ER, increases ER Ca2+ stores in MIN6 β-cells and protects against NO-induced apoptosis.20 Xestospongin, an inhibitor of the IP3 receptor, and dantrolene, an inhibitor of the ryanodine receptor, were reported to prevent cell death of neurons derived from presenilin-1 mutant mice.38 Association of brain ischemia with ER stress has also been reported. Brain ischemia and reperfusion activated the eukaryotic initiation factor 2α kinase PERK, an ER stress sensor and transducer protein which is activated by ER stress.39 Expression of 150 kDa oxygen-regulated protein (ORP150), an ER chaperone in the hippocampus, suppressed delayed neuronal cell death.40
In this report, we showed that brain ischemia-induced neuronal cell death is mediated by CHOP. CHOP was induced by brain ischemia in the striatum and the hippocampus, and ischemia-induced neuronal cell death was attenuated in CHOP-deficient mice. In our experiments, CHOP mRNA was highly induced at 12 h after 15 min-BCCAO (Figure 2) and CHOP protein was induced at 24 h (Figure 3), but apoptosis continued up to 7 days (Figure 1). We speculate that CHOP-induced apoptosis occurs in early phase after ischemia and that apoptosis in later phase is induced through other death pathways.13 Induction of XBP1 mRNA and its splicing were very similar between wild-type and CHOP−/− mice (Figure 5), whereas induction of BiP mRNAs were somewhat differed between the two (Figures 2 and 4). It is known that induction and splicing of XBP1 mRNA are regulated mainly by IRE1 and ATF6, whereas expression of BiP mRNA is regulated mainly by ATF6 and XBP1.31,32 Because there are crosstalks among the ER stress response pathways, the difference in BiP mRNA induction between wild-type and CHOP−/− mice may occur under complex pathological conditions such as ischemia-reperfusion.
Moreover, we showed that primary hippocampal neurons from embryonic brain of CHOP−/− mice are more resistant against hypoxia-reoxygenation than those from wild-type animals, and that neurons are much more sensitive to hypoxia-reoxygenation than glial cells (Figure 8). However, although disruption of the CHOP gene delayed neuronal apoptosis, ischemia-induced apoptosis could not be suppressed completely. Similar results were obtained for pancreatic β cells from CHOP−/− mice.12 We speculate that CHOP-independent ER stress pathways including caspase-1241 or TRAF2-ASK1-JNK,34 or other cell death mechanisms such as oxidative stress might cause neuronal apoptosis in CHOP-deficient mice. Actually, phosphorylation of JNK was increased by hypoxia-reoxygenation in primary cultured neurons from CHOP−/− mice. Further studies on ER stress-mediated apoptosis are expected to provide new insights into the pathogenesis of brain ischemia and degenerative disease and new therapeutic approaches for prevention of these and related diseases can be designed.
Materials and Methods
Ischemia model
All procedures involving these animals were approved by the Animal Care and Use Committee of Kumamoto University. Mice lacking the CHOP gene (C57 BL/6 background) were provided by Dr. Shizuo Akira (Osaka University, Japan).20 CHOP−/− mice show normal growth, development and fertility.42 C57 BL/6 male mice (wild-type) and CHOP−/− mice weighing 20–30 g (6–7 weeks old) were allowed free access to food and water, and were housed under constant environmental conditions (temperature, 22±2°C; humidity, 55±5% and a 12/12 h light/dark cycle). Brain ischemia was induced by bilateral common carotid arteries occlusion (BCCAO) for 15 min under 2% halothane in a mixture 70% N2O and 30% O2 using a face mask essentially as described.30 Rectal temperature, monitored using a digital thermometer (Small Animals Heat Controller, Unique Medical, Tokyo, Japan) inserted 9 mm into the anus, was maintained at 37±0.5°C using a heating lamp and a blanket until the mice were completely awake. Control animals were sham-operated without occlusion.
Measurements of physiological parameters
pH, PaO2 and PaCO2 were measured using a blood gas analyzer (SL Blood Analysis System Series 2000, Diametrics Medical, MN, USA). Glucose was measured using blood glucose analyzer (Precision QID System, Abbott Laboratories, IL, USA). Rectal temperature was maintained at 37±0.5°C as described above. Mean arterial blood pressure was measured via a tail artery using a sphygmomanometer (TK-340 Rat-Mouse Manometer-Tachometer, Unicom, Chiba, Japan). Regional cerebral blood flow was measured by laser-Doppler flowmeter (ALF21, Advance, Tokyo, Japan). Craniectomy was performed on the skull over the bilateral cortex (1 mm caudal and 2 mm lateral from the bregma) using a drill and with extreme care. After the hollow plastic tubes were fixed to the skull with resin, the flowmeter probe was inserted into tubes. Values for right and left cortex were averaged.
Histological analysis and detection of apoptosis
After the indicated days, animals were reanesthetized by giving sodium pentobarbital (50 mg/g, i.p.) then were perfused with ice-cold phosphate-buffered saline (PBS) followed by 4% paraformaldehyde via left ventricle of the heart. The whole brain was removed and post-fixed in 4% paraformaldehyde in PBS for 24 h. For histological analysis with Nissl's staining, consecutive coronal sections of 20 μm in thickness were prepared using Vibratome Sectioning techniques (Technical Products International, MO, USA). Neuronal cell death was assessed at 7 days after 15 min-BCCAO or sham operation. Striatum at the level of the anterior commissure and dorsal hippocampus was examined and neuronal damages were evaluated in each hemisphere. Apoptosis was detected by TUNEL method using an in situ apoptosis detection kit (Takara Shuzo, Otsu, Japan). TUNEL signals were amplified with Streptavidin Alexa Fluora 488 conjugate (diluted 1 : 200; Molecular Probes, Leiden, The Netherlands) using the TSA Biotin System (PerkinElmer Life Sciences Inc., Boston, MA, USA).
RT-PCR analysis
Mice were deeply anesthetized and decapitated at indicated times after ischemic insult. Bilateral striatum and the whole hippocampus were removed and frozen immediately on dry ice then stored at −80°C. Total RNA was isolated using the acid guanidium thiocyanate phenol–chloroform extraction procedure. cDNA was synthesized using the Superscript One-Step RT-PCR System (Invitrogen, Grand Island, NY, USA). The primers used are as follows: sense primer, 5′-CATACACCACCACACCTGAAAG-3′ and antisense primer, 5′-CCGTTTCCTAGTTCTTCCTTGC-3′ for CHOP; sense primer, 5′-GAAAGGATGGTTAATGATGCTGAG-3′ and antisense primer, 5′-GTCTTCAATGTCCGCATCCTG-3′ for BiP; sense primer, 5′-AAACAGAGTAGCAGCGCAGACTGC-3′ and antisense primer, 5′-GGATCTCTAAAACTAGAGGCTTGGTG-3′ for XBP1;32 sense primer, 5′-TGGCACAGTCAAGGCTGAGA-3′ and antisense primer, 5′-CTTCTGAGTGGCAGTGATGG-3′ for glyceraldehyde-3-phosphate dehydrogenase (GAPDH). The primer sets for CHOP, BiP, unspliced form XBP1, spliced form XBP1 and GAPDH are expected to give PCR products with a size of 357, 231, 600, 574 and 380 bp, respectively. PCR consisted of an initial denaturation cycle at 94°C for 2 min, followed by the 30 cycles for CHOP and GAPDH, 25 cycles for XBP1 and the 22 cycles for BiP consisted of denaturation at 94°C for 15 s, annealing at 55°C for 30 s, and elongation at 68°C for 1 min. An additional cycle at 72°C for 7 min completed the amplification process. Amplified PCR products were separated by 2% for CHOP, BiP, GAPDH or 3% for XBP1 agarose gel electrophoresis and visualized with the use of ethidium bromide staining. Densitometric quantification was done using MacBas software (Fuji Photo Film Co., Tokyo, Japan) and the results are shown as mean±S.D.
Immunohistochemical analysis
To detect surviving neurons in vivo, CaMKIV-immunohistochemical analysis was done as described by Yano et al.43.In brief, sections were incubated by floating for 30 min in PBS containing 0.5% Triton X-100, 30 min in PBS with 3% bovine serum albumin, and overnight with anti-mouse CaMKIV antibody (diluted 1 : 1000; Transduction Lab. Lexington, KY, USA) in PBS. The sections were then labeled for 2 h with FITC-labeled anti-mouse IgG (diluted 1 : 200; Vector Lab. Burlingame, CA, USA) and nuclei were stained for 15 min with PI. The sections were analyzed using a confocal laser microscope (Fluoview, Olympus, Tokyo, Japan). To quantify neuronal cell death in the striatum, each hemisphere was divided into superior and inferior regions, and CaMKIV-positive cells were counted in each area using software (Scicon image, MD, USA). For the hippocampus, medial CA1 subfields were captured on the computer at the same magnification (× 400), and CaMKIV-positive cells were counted. The total number of CaMKIV-positive cells in each area of left and right hippocampus was averaged by two independent observers without the knowledge of treatment conditions. The sections were also prepared with Nissl's staining, and the number of viable neurons exhibiting normal morphologic properties with round nuclei was the same as CaMKIV-positive cells (data not shown). To detect CHOP protein, 5 μm paraffin-embedded sections were stained with anti-mouse CHOP monoclonal antibody (diluted 1 : 200; Santa Cruz Biotechnology Inc., Santa Cruz, CA, USA), followed by anti-mouse IgG (diluted 1 : 500; Amersham Life Science). Signals were amplified with Streptavidin Alexa Fluora 488 conjugate (diluted 1 : 200; Molecular Probes) using the TSA Biotin System (Perkin-Elmer). Primary cultured hippocampus cells were fixed with 4% formaldehyde in PBS and were observed with double staining using anti-mouse MAP2 monoclonal antibody (diluted 1 : 1000; Sigma Chemical Co., St. Louis, MO, USA) for neurons and anti-rabbit GFAP polyclonal antibody (diluted 1 : 2000; Santa Cruz Biotechnology Inc.) for glial cells as primary antibodies. Then, Cy3-labeled anti-mouse IgG (diluted 1 : 400; Amersham Life Science) and Alexa Fluora 488-labeled anti-rabbit IgG (diluted 1 : 400; Molecular Probes) were used as secondary antibodies.
Western blot analysis
Primary cultured neurons were homogenized in 150 mM NaCl containing, 50 mM Tris-HCl (pH 7.2), 1% Triton X-100 and complete mini protease inhibitor mixture tablets (Roche Molecular Biochemicals). After centrifugation, the supernatants were used for immunoblot analysis. Immunodetection was performed using the ECL kit (Amersham Life Science), according to the protocol provided by the manufacturer. Chemiluminescence signals were quantified with a chemiluminescence image analyzer (Las-1000 plus; Fuji Photo Film Co.). Anti-JNK1 polyclonal antibody (diluted 1 : 1000; Santa Cruz Biotechnology Inc.) and antiphospho-JNK polyclonal antibody (diluted 1 : 1000; Cell Signaling Technology Inc.) were used as primary antibodies.
Primary culture of hippocampal cells
Primary cultured cells were prepared from the hippocampus of embryonic wild-type or CHOP−/− mice at days 16–18 of gestation (E16-18) as described by Yanagisawa et al.44 with minor modifications. Briefly, neuron-rich hippocampi were dissected and cells were dissociated in Ca2+- and Mg2+-free Hanks' balanced salt solution containing 0.2% papain and 0.05% DNase I at 37°C for 15 min.45 After enzymes were inactivated by the addition of fetal calf serum, cells were suspended in the neurobasal medium with 0.5 mM L-glutamine, 25 μM glutamate, 100 U/ml penicillin, 50 μg/ml streptomycin, 8 μM cytosine arabinocide and 2% B27 supplement (Invitrogen). Cells were plated at a density of 1 × 105 cells per well on poly-D-lysine-coated 24-well plates (Clontech Laboratories, Inc., NJ, USA) and cultured at 37°C in a humidified atmosphere containing 5% CO2 for 2 days and then for 8 days without cytosine arabinocide. When neurons and glial cells were cultured, cytosine arabinocide was omitted.
Hypoxia-reoxygenation
Hypoxia was induced with an anaerobic culture kit (Mitsubishi Gas Chemicals Inc., Japan) using disposable O2-absorbing and CO2-generating agents (O2, <1% CO2, 5%). This system can create a hypoxic condition without changing pH in the medium. Reoxygenation was performed by removing cultured plates from the anaerobic chamber, the medium was exchanged and the plates were returned to the CO2 incubator.
Statistical analysis
Quantitative results were expressed as mean±S.D. and analyzed using Student's t-test. The significance in difference was assigned at the level of less than 5% probability (P<0.05).
Abbreviations
- BCCAO:
-
bilateral common carotid arteries occlusion
- CaMKIV:
-
Ca2+/calmodulin-dependent protein kinase IV
- CHOP:
-
C/EBP homologues protein
- ER:
-
endoplasmic reticulum
- GFAP:
-
glial fibrillary acidic protein
- MAP2:
-
microtubule-associated protein 2
- NO:
-
nitric oxide
- PI:
-
propidium iodide
- TUNEL:
-
terminal transferase-mediated dUTP-biotin nick end labeling
References
Ankarcrona M, Dypbukt JM, Bonfoco E, Zhivotovsky B, Orrenius S, Lipton SA and Nicotera P (1995) Glutamate-induced neuronal death: a succession of necrosis or apoptosis depending on mitochondrial function. Neuron 15: 961–973
Lipton SA and Rosenberg PA (1994) Excitatory amino acids as a final common pathway for neurologic disorders. N. Engl. J. Med. 330: 613–622
Pellegrini-Giampietro DE, Gorter JA, Bennett MV and Zukin RS (1997) The GluR2 (GluR-B) hypothesis: Ca2+-permeable AMPA receptors in neurological disorders. Trends Neurosci. 20: 464–470
Snider BJ, Tee LY, Canzoniero LM, Babcock DJ and Choi DW (2002) NMDA antagonists exacerbate neuronal death caused by proteasome inhibition in cultured cortical and striatal neurons. Eur. J. Neurosci. 15: 419–428
Fawcett DW (1981) In The Cell. London: W. B. Saunders Company pp. 318–319
Kaufman RJ, Scheuner D, Schroder M, Shen X, Lee K, Liu CY and Arnold SM (2002) The unfolded protein response in nutrient sensing and differentiation. Nat. Rev. Mol. Cell Biol. 3: 411–421
Oyadomari S, Araki E and Mori M (2002) Endoplasmic reticulum stress-mediated apoptosis in pancreatic β-cells. Apoptosis 7: 335–345
Kaufman RJ (1999) Stress signaling from the lumen of the endoplasmic reticulum: coordination of gene transcriptional and translational controls. Genes Dev. 13: 1211–1233
Mori K (2000) Tripartite management of unfolded proteins in the endoplasmic reticulum. Cell 101: 451–454
Ron D and Habener JF (1992) CHOP, a novel developmentally regulated nuclear protein that dimerizes with transcription factors C/EBP and LAP and functions as a dominant-negative inhibitor of gene transcription. Genes Dev. 6: 439–453
Barone MV, Crozat A, Tabaee A, Philipson L and Ron D (1994) CHOP (GADD153) and its oncogenic variant, TLS-CHOP, have opposing effects on the induction of G1/S arrest. Genes Dev. 8: 453–464
Oyadomari S, Koizumi A, Takeda K, Gotoh T, Akira S, Araki E and Mori M (2002) Targeted disruption of the Chop gene delays endoplasmic reticulum stress-mediated diabetes. J. Clin. Invest. 109: 525–532
Ferri KF and Kroemer G (2001) Organelle-specific initiation of cell death pathways. Nat. Cell Biol. 3: E255–263
Wang XZ, Harding HP, Zhang Y, Jolicoeur EM, Kuroda M and Ron D (1998) Cloning of mammalian Ire1 reveals diversity in the ER stress responses. EMBO J. 17: 5708–5717
Haze K, Yoshida H, Yanagi H, Yura T and Mori K (1999) Mammalian transcription factor ATF6 is synthesized as a transmembrane protein and activated by proteolysis in response to endoplasmic reticulum stress. Mol. Biol. Cell 10: 3787–3799
Harding HP, Zhang Y, Bertolotti A, Zeng H and Ron D (2000) Perk is essential for translational regulation and cell survival during the unfolded protein response. Mol. Cell 5: 897–904
Matsumoto M, Minami M, Takeda K, Sakao Y and Akira S (1996) Ectopic expression of CHOP (GADD153) induces apoptosis in M1 myeloblastic leukemia cells. FEBS Lett. 395: 143–147
Gotoh T, Oyadomari S, Mori K and Mori M (2002) Nitric oxide-induced apoptosis in RAW 264. 7 macrophages is mediated by endoplasmic reticulum stress pathway involving ATF6 and CHOP. J. Biol. Chem. 277: 12343–12350
McCullough KD, Martindale JL, Klotz LO, Aw TY and Holbrook NJ (2001) Gadd153 sensitizes cells to endoplasmic reticulum stress by down-regulating Bcl2 and perturbing the cellular redox state. Mol. Cell Biol. 21: 1249–1259
Oyadomari S, Takeda K, Takiguchi M, Gotoh T, Matsumoto M, Wada I, Akira S, Araki E and Mori M (2001) Nitric oxide-induced apoptosis in pancreatic beta cells is mediated by the endoplasmic reticulum stress pathway. Proc. Natl. Acad. Sci. USA 98: 10845–10850
Kawahara K, Oyadomari S, Gotoh T, Kohsaka S, Nakayama H and Mori M (2001) Induction of CHOP and apoptosis by nitric oxide in p53-deficient microglial cells. FEBS Lett. 506: 135–139
Ron D (2002) Proteotoxicity in the endoplasmic reticulum: lessons from the Akita diabetic mouse. J. Clin. Invest. 109: 443–445
DeGracia DJ, Kumar R, Owen CR, Krause GS and White BC (2002) Molecular pathways of protein synthesis inhibition during brain reperfusion: implications for neuronal survival or death. J. Cereb. Blood Flow Metab. 22: 127–141
Doutheil J, Gissel C, Oschlies U, Hossmann KA and Paschen W (1997) Relation of neuronal endoplasmic reticulum calcium homeostasis to ribosomal aggregation and protein synthesis: implications for stress-induced suppression of protein synthesis. Brain Res. 775: 43–51
Carmeliet P, Dor Y, Herbert JM, Fukumura D, Brusselmans K, Dewerchin M, Neeman M, Bono F, Abramovitch R, Maxwell P, Koch CJ, Ratcliffe P, Moons L, Jain RK, Collen D, Keshert E and Keshet E (1998) Role of HIF-1α in hypoxia-mediated apoptosis, cell proliferation and tumour angiogenesis. Nature 394: 485–490
Paschen W, Gissel C, Linden T, Althausen S and Doutheil J (1998) Activation of gadd153 expression through transient cerebral ischemia: evidence that ischemia causes endoplasmic reticulum dysfunction. Mol. Brain Res. 60: 115–122
Jin K, Mao XO, Eshoo MW, Nagayama T, Minami M, Simon RP and Greenberg DA (2001) Microarray analysis of hippocampal gene expression in global cerebral ischemia. Ann. Neurol. 50: 93–103
Murakami K, Kondo T, Kawase M and Chan PH (1998) The development of a new mouse model of global ischemia: focus on the relationships between ischemia duration, anesthesia, cerebral vasculature, and neuronal injury following global ischemia in mice. Brain Res. 780: 304–310
Stephen K, James M and Karen H (2001) Minimal ischemic neuronal damage and HSP70 expression in MF1 strain mice following bilateral common carotid arteryocclusion. Brain Res. 914: 185–195
Wu C, Zhan RZ, Qi S, Fujihara H, Taga K and Shimoji K (2001) A forebrain ischemic preconditioning model established in C57Black/Crj6 mice. J. Neurosci. Methods 107: 101–106
Yoshida H, Matsui T, Yamamoto A, Okada T and Mori K (2001) XBP1 mRNA is induced by ATF6 and spliced by IRE1 in response to ER stress to produce a highly active transcription factor. Cell 107: 881–891
Calfon M, Zeng H, Urano F, Till JH, Hubbard SR, Harding HP, Clark SG and Ron D (2002) IRE1 couples endoplasmic reticulum load to secretory capacity by processing the XBP-1 mRNA. Nature 415: 92–96
Kang H, Sun LD, Atkins CM, Soderling TR, Wilson MA and Tonegawa S (2001) An important role of neural activity-dependent CaMKIV signaling in the consolidation of long-term memory. Cell 106: 771–783
Nishitoh H, Matsuzawa A, Tobiume K, Saegusa K, Takeda K, Inoue K, Hori S, Kakizuka A and Ichijo H (2002) ASK1 is essential for endoplasmic reticulum stress-induced neuronal cell death triggered by expanded polyglutamine repeats. Genes Dev. 16: 1345–1355
Paschen W and Doutheil J (1999) Disturbances of the functioning of endoplasmic reticulum: a key mechanism underlying neuronal cell injury? J. Cereb. Blood Flow Metab. 19: 1–18
He H, Lam M, McCormick TS and Distelhorst CW (1997) Maintenance of calcium homeostasis in the endoplasmic reticulum by Bcl-2. J. Cell Biol. 138: 1219–1228
Xu L, Eu JP, Meissner G and Stamler JS (1998) Activation of the cardiac calcium release channel (ryanodine receptor) by poly-S-nitrosylation. Science 279: 234–237
Mattson MP, Zhu H, Yu J and Kindy MS (2000) Presenilin-1 mutation increases neuronal vulnerability to focal ischemia in vivo and to hypoxia and glucose deprivation in cell culture: involvement of perturbed calcium homeostasis. J. Neurosci. 20: 1358–1364
Kumar R, Azam S, Sullivan JM, Owen C, Cavener DR, Zhang P, Ron D, Harding HP, Chen JJ, Han A, White BC, Krause GS and DeGracia DJ (2001) Brain ischemia and reperfusion activates the eukaryotic initiation factor 2á kinase, PERK. J. Neurochem. 77: 1418–1421
Miyazaki M, Ozawa K, Hori O, Kitao Y, Matsushita K, Ogawa S and Matsuyama T (2002) Expression of 150-kD oxygen-regulated protein in the hippocampus suppresses delayed neuronal cell death. J. Cereb. Blood Flow Metab. 22: 979–987
Nakagawa T, Zhu H, Morishima N, Li E, Xu J, Yankner BA and Yuan J (2000) Caspase-12 mediates endoplasmic-reticulum-specific apoptosis and cytotoxicity by amyloid-beta. Nature 403: 98–103
Zinszner H, Kuroda M, Wang X, Batchvarova N, Lightfoot RT, Remotti H, Stevens JL and Ron D (1998) CHOP is implicated in programmed cell death in response to impaired function of the endoplasmic reticulum. Genes Dev. 12: 982–999
Yano S, Morioka M, Fukunaga K, Kawano T, Hara T, Kai Y, Hamada J, Miyamoto E and Ushio Y (2001) Activation of Akt/protein kinase B contributes to induction of ischemic tolerance in the CA1 subfield of gerbil hippocampus. J. Cereb. Blood Flow Metab. 21: 351–360
Yanagisawa M, Nakashima K, Arakawa H, Ikenaka K, Yoshida K, Kishimoto T, Hisatsune T and Taga T (2000) Astrocyte differentiation of fetal neuroepithelial cells by interleukin-11 via activation of a common cytokine signal transducer, gp130, and a transcription factor, STAT3. J. Neurochem. 74: 1498–1504
Verma A, Hirsch DJ and Snyder SH (1992) Calcium pools mobilized by calcium or inositol 1,4,5-trisphosphate are differentially localized in rat heart and brain. Mol. Biol. Cell 3: 621–631
Acknowledgements
We thank R Shindo and M Obata for technical assistance, and M Ohara (Fukuoka, Japan) for comments on the manuscript. We also thank M Yanagisawa (Institute of Molecular Embryology and Genetics, Kumamoto University) and Y Hasegawa (Departments of Neurosurgery, Kumamoto University, Graduate School of Medical Sciences, Japan) for technical suggestions. This work was supported in part by Grants-in-Aid for Scientific Research 14037257 and 14370047 (to MM) and 13671446 (to SY) from the Ministry of Education, Culture, Sports, Science and Technology of Japan.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Edited by Dr. H Ichijo
Rights and permissions
About this article
Cite this article
Tajiri, S., Oyadomari, S., Yano, S. et al. Ischemia-induced neuronal cell death is mediated by the endoplasmic reticulum stress pathway involving CHOP. Cell Death Differ 11, 403–415 (2004). https://doi.org/10.1038/sj.cdd.4401365
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.cdd.4401365
Keywords
This article is cited by
-
Hypothermia increases adenosine monophosphate and xanthosine monophosphate levels in the mouse hippocampus, preventing their reduction by global cerebral ischemia
Scientific Reports (2024)
-
Rapamycin Alleviates Neuronal Injury and Modulates Microglial Activation After Cerebral Ischemia
Molecular Neurobiology (2024)
-
Involvement of Proteasomal and Endoplasmic Reticulum Stress in Neurodegeneration After Global Brain Ischemia
Molecular Neurobiology (2023)
-
Peptidylarginine deiminase 2 promotes T helper 17-like T cell activation and activated T cell-autonomous death (ACAD) through an endoplasmic reticulum stress and autophagy coupling mechanism
Cellular & Molecular Biology Letters (2022)
-
Zinc Accumulation Aggravates Cerebral Ischemia/Reperfusion Injury Through Inducing Endoplasmic Reticulum Stress
Neurochemical Research (2022)