Abstract
OBJECTIVE: To explore the association between measures of insulin resistance with objectively assessed physical activity.
DESIGN: School-based, cross-sectional study.
SUBJECTS: A randomly selected sample of 589 children (310 girls, 279 boys, mean (standard deviations, s.d.) age=9.7 (0.44) y, weight=33.6 (6.4) kg, height=1.39 (0.06) m) from Denmark.
METHODS: Fasting blood samples were analysed for serum insulin and glucose. Physical activity was measured with the uniaxial Computer Science and Applications (CSA) model 7164 accelerometer, worn for at least 3 days (≥10 h day−1). Adiposity was assessed by the sum of four skinfolds. Multiple linear regression were performed to model insulin and glucose from average CSA output, adjusted for age, gender, puberty, ethnicity, birth weight, parental smoking, socioeconomic group, and CSA unit. In addition, we adjusted for skinfold thickness.
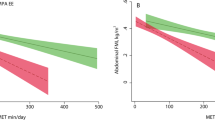
RESULTS: Mean fasting serum glucose ranged from 4.1 to 6.5 mmol l−1 with a mean (s.d.) of 5.1 (0.37) mmol l−1. Fasting insulin was negatively correlated with CSA output on levels of adjustment. Fasting glucose was not significantly associated with physical activity. However, in girls both indices of insulin resistance were significantly related to activity, whereas in boys none of the associations were significant.
CONCLUSION: Physical activity is inversely associated with fasting insulin in the nondiabetic range of fasting glucose. The relationship was stronger for insulin than for glucose, indicating compensatory action by the β cells. Our data emphasise the importance of physical activity in children for the maintenance of metabolic control.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
American Diabetes Association. Type 2 diabetes in children and adolescents. American Diabetes Association. Diabetes Care 2000; 23: 381–389.
Ehtisham S, Barrett TG, Shaw NJ . Type 2 diabetes mellitus in UK children—an emerging problem. Diabetic Med 2000; 17: 867–871.
Goran MI, Ball GD, Cruz ML . Obesity and risk of type 2 diabetes and cardiovascular disease in children and adolescents. J Clin Endocrinol Metab 2003; 88: 1417–1427.
Anavian J, Brenner DJ, Fort P, Speiser PW . Profiles of obese children presenting for metabolic evaluation. J Pediatr Endocrinol Metab 2001; 14: 1145–1150.
Ku CY, Gower BA, Hunter GR, Goran MI . Racial differences in insulin secretion and sensitivity in prepubertal children: role of physical fitness and physical activity. Obes Res 2000; 8: 506–515.
Raitakari OT, Taimela S, Porkka KV, Telama R, Valimaki I, Akerblom HK, Viikari JS . Associations between physical activity and risk factors for coronary heart disease: the Cardiovascular Risk in Young Finns Study. Med Sci Sports Exerc 1997; 29: 1055–1061.
Schmitz KH, Jacobs Jr DR, Hong CP, Steinberger J, Moran A, Sinaiko AR . Association of physical activity with insulin sensitivity in children. Int J Obes Relat Metab Disord 2002; 26: 1310–1316.
Kohl III HW, Fulton JE, Caspersen CJ . Assessment of physical activity among children and adolescents: a review and synthesis. Prev Med 2000; 31: S54–S76.
Baranowski T, Dworkin R, Cieslik C, Hooks P, Clearman D, Ray L . Reliability and validity of self report of aerobic activity: Family Health Project. Res Q 1984; 55: 309–317.
Saris WH . The assessment and evaluation of daily physical activity in children. A review. Acta Paediatr Scand Suppl 1985; 318: 37–48.
Sallis JF, Buono MJ, Freedson PS . Bias in estimating caloric expenditure from physical activity in children. Implications for epidemiological studies. Sports Med 1991; 11: 203–209.
Craig SB, Bandini LG, Lichtenstein AH, Schaefer EJ, Dietz WH . The impact of physical activity on lipids, lipoproteins, and blood pressure in preadolescent girls. Pediatrics 1996; 98 (Part 1): 389–395.
Ozanne SE, Hales CN . Early programming of glucose–insulin metabolism. Trends Endocrinol Metab 2002; 13: 368–373.
Li C, Johnson MS, Goran MI . Effects of low birth weight on insulin resistance syndrome in caucasian and African–American children. Diabetes Care 2001; 24: 2035–2042.
Harder T, Kohlhoff R, Dorner G, Rohde W, Plagemann A . Perinatal ‘programming’ of insulin resistance in childhood: critical impact of neonatal insulin and low birth weight in a risk population. Diabetic Med 2001; 18: 634–639.
Gutin B, Litaker M, Islam S, Manos T, Smith C, Treiber F . Body-composition measurement in 9–11-y-old children by dual-energy X-ray absorptiometry, skinfold-thickness measurements, and bioimpedance analysis. Am J Clin Nutr 1996; 63: 287–292.
Marshall W, Tanner JM . Variations in pattern of pubertal changes in girls. Arch Dis Child 1969; 44: 291–301.
Marshall W, Tanner JM . Variations in the pattern of pubertal changes in boys. Arch Dis Child 1970; 45: 13–23.
Tryon WW, Williams R . Fully proportional actigraphy: A new instrument. Behav Res Methods Instr Comput 1996; 28: 392–403.
Brage S, Brage N, Wedderkopp N, Froberg K . Reliability and validity of the Computer Science and Applications accelerometer in a mechanical setting. Meas Phys Educ Exerc Sci 2003; 7: 101–119.
Metcalf BS, Curnow JS, Evans C, Voss LD, Wilkin TJ . Technical reliability of the CSA activity monitor: the EarlyBird Study. Med Sci Sports Exerc 2002; 34: 1533–1537.
Petersen TA, Rasmussen S, Madsen M . BMI of Danish school children measured during the periods 1986/1987–1996/1997 compared to Danish measurement in 1971/1972. Ugeskr Laeger 2002; 164: 5006–5010.
Ekelund U, Sjostrom M, Yngve A, Poortvliet E, Nilsson A, Froberg K, Wedderkopp N, Westerterp K . Physical activity assessed by activity monitor and doubly labeled water in children. Med Sci Sports Exerc 2001; 33: 275–281.
Trost SG, Ward DS, Moorehead SM, Watson PD, Riner W, Burke JR . Validity of the computer science and applications (CSA) activity monitor in children. Med Sci Sports Exerc 1998; 30: 629–633.
Brage S, Wedderkopp N, Andersen LB, Froberg K . Influence of step frequency on movement intensity predictions with the CSA accelerometer: a field validation study in children. Ped Exerc Sci 2003; 15: 277–287.
Brage S, Wedderkopp N, Franks PW, Andersen LB, Froberg K . Reexamination of validity and reliability of the CSA monitor in walking and running. Med Sci Sports Exerc 2003; 35: 1447–1454.
Cavagna GA, Franzetti P . The determinants of the step frequency in walking in humans. J Physiol (Lond) 1986; 373: 235–242.
Cavagna GA, Franzetti P, Heglund NC, Willems P . The determinants of the step frequency in running, trotting and hopping in man and other vertebrates. J Physiol (Lond) 1988; 399: 81–92.
Caprio S, Plewe G, Diamond MP, Simonson DC, Boulware SD, Sherwin RS, Tamborlane WV . Increased insulin secretion in puberty: a compensatory response to reductions in insulin sensitivity. J Pediatr 1989; 114: 963–967.
Lestradet H, Deschamps I, Giron B . Insulin and free fatty acid levels during oral glucose tolerance tests and their relation to age in 70 healthy children. Diabetes 1976; 25: 505–508.
Johnson MS, Figueroa-Colon R, Huang TTK, Dwyer JH, Goran MI . Longitudinal changes in body fat in African American and Caucasian children: influence of fasting insulin and insulin sensitivity. J Clin Endocrinol Metab 2001; 86: 3182–3187.
Matsui I, Nambu S, Baba S . Evaluation of fasting serum insulin levels among Japanese school-age children. J Nutr Sci Vitaminol (Tokyo) 1998; 44: 819–828.
Campaigne BN, Gilliam TB, Spencer ML, Lampman RM, Schork MA . Effects of a physical activity program on metabolic control and cardiovascular fitness in children with insulin-dependent diabetes mellitus. Diabetes Care 1984; 7: 57–62.
Kahle EB, O'Dorisio TM, Walker RB, Eisenman PA, Reiser S, Cataland S, Zipf WB . Exercise adaptation responses for gastric inhibitory polypeptide (GIP) and insulin in obese children. Possible extra-ancreatic effects. Diabetes 1986; 35: 579–582.
Kahle EB, Zipf WB, Lamb DR, Horswill CA, Ward KM . Association between mild, routine exercise and improved insulin dynamics and glucose control in obese adolescents. Int J Sports Med 1996; 17: 1–6.
Hardin DS, Hebert JD, Bayden T, Dehart M, Mazur L . Treatment of childhood syndrome X. Pediatrics 1997; 100: E5.
Ferguson MA, Gutin B, Le NA, Karp W, Litaker M, Humphries M, Okuyama T, Riggs S, Owens S . Effects of exercise training and its cessation on components of the insulin resistance syndrome in obese children. Int J Obes Relat Metab Disord 1999; 23: 889–895.
Escobar O, Mizuma H, Sothern MS, Blecker U, Udall Jr JN, Suskind RM, Hilton C, Vargas A . Hepatic insulin clearance increases after weight loss in obese children and adolescents. Am J Med Sci 1999; 317: 282–286.
McMurray RG, Bauman MJ, Harrell JS, Brown S, Bangdiwala SI . Effects of improvement in aerobic power on resting insulin and glucose concentrations in children. Eur J Appl Physiol 2000; 81: 132–139.
Sudi KM, Gallistl S, Trobinger M, Payerl D, Weinhandl G, Muntean W, Aigner R, Borkenstein MH . The influence of weight loss on fibrinolytic and metabolic parameters in obese children and adolescents. J Pediatr Endocrinol Metab 2001; 14: 85–94.
Kang HS, Gutin B, Barbeau P, Owens S, Lemmon CR, Allison J, Litaker MS, Le NA . Physical training improves insulin resistance syndrome markers in obese adolescents. Med Sci Sports Exerc 2002; 34: 1920–1927.
Gutin B, Cucuzzo N, Islam S, Smith C, Stachura ME . Physical training, lifestyle education, and coronary risk factors in obese girls. Med Sci Sports Exerc 1996; 28: 19–23.
Le Stunff C, Fallin D, Schork NJ, Bougneres P . The insulin gene VNTR is associated with fasting insulin levels and development of juvenile obesity. Nat Genet 2000; 26: 444–446.
Zierath JR . Invited review: EXERCISE training-induced changes in insulin signaling in skeletal muscle. J Appl Physiol 2002; 93: 773–781.
Greco AV, Mingrone G, Giancaterini A, Manco M, Morroni M, Cinti S, Granzotto M, Vettor R, Camastra S, Ferrannini E . Insulin resistance in morbid obesity: reversal with intramyocellular fat depletion. Diabetes 2002; 51: 144–151.
Ashley MA, Buckley AJ, Criss AL, Ward JA, Kemp A, Garnett S, Cowell CT, Baur LA, Thompson CH . Familial, anthropometric, and metabolic associations of intramyocellular lipid levels in prepubertal males. Pediatr Res 2002; 51: 81–86.
Derave W, Eijnde BO, Verbessem P, Ramaekers M, Van Leemputte M, Richter EA, Hespel P . Combined creatine and protein supplementation in conjunction with resistance training promotes muscle GLUT-4 content and glucose tolerance in humans. J Appl Physiol 2003; 94: 1910–1916.
Ritenbaugh C, Teufel-Shone NI, Aickin MG, Joe JR, Poirier S, Dillingham DC, Johnson D, Henning S, Cole SM, Cockerham D . A lifestyle intervention improves plasma insulin levels among Native American high school youth. Prev Med 2003; 36: 309–319.
Acknowledgements
We acknowledge the statistical assistance of Dr Jian'an Luan, MRC Epidemiology Unit, Cambridge, UK. The study received financial support from the Danish Medical Research Council and the Danish Heart Foundation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Brage, S., Wedderkopp, N., Ekelund, U. et al. Objectively measured physical activity correlates with indices of insulin resistance in Danish children.. Int J Obes 28, 1503–1508 (2004). https://doi.org/10.1038/sj.ijo.0802772
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ijo.0802772
Keywords
This article is cited by
-
Validation of the Activity Preference Assessment: a tool for quantifying children’s implicit preferences for sedentary and physical activities
International Journal of Behavioral Nutrition and Physical Activity (2020)
-
Physical activity and sedentary behaviour in relation to cardiometabolic risk in children: cross-sectional findings from the Physical Activity and Nutrition in Children (PANIC) Study
International Journal of Behavioral Nutrition and Physical Activity (2014)
-
Physical activity, sedentary time, and liver enzymes in adolescents: the HELENA study
Pediatric Research (2014)
-
Physical activity and clustered cardiovascular disease risk factors in young children: a cross-sectional study (the IDEFICS study)
BMC Medicine (2013)
-
Age and menarcheal status do not influence metabolic response to aerobic training in overweight girls
Diabetology & Metabolic Syndrome (2013)