Abstract
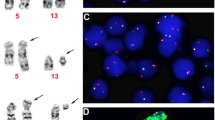
Detection of the FIP1L1-PDGFRA fusion gene or the corresponding cryptic 4q12 deletion supports the diagnosis of chronic eosinophilic leukemia (CEL) in patients with chronic hypereosinophilia. We retrospectively characterized 17 patients fulfilling WHO criteria for idiopathic hypereosinophilic syndrome (IHES) or CEL, using nested RT-PCR and interphase fluorescence in situ hybridization (FISH). Eight had FIP1L1-PDGFRA (+) CEL, three had FIP1L1-PDGFRA (−) CEL and six had IHES. FIP1L1-PDGFRA (+) CEL responded poorly to steroids, hydroxyurea or interferon-α, and had a high probability of eosinophilic endomyocarditis (n=4) and disease-related death (n=4). In FIP1L1-PDGFRA (+) CEL, palpable splenomegaly was present in 5/8 cases, serum vitamin B12 was always markedly increased, and marrow biopsies revealed a distinctively myeloproliferative aspect. Imatinib induced rapid complete hematological responses in 4/4 treated FIP1L1-PDGFRA (+) cases, including one female, and complete molecular remission in 2/3 evaluable cases. In the female patient, 1 log reduction of FIP1L1-PDGFRA copy number was reached as by real-time quantitative PCR (RQ-PCR). Thus, correlating IHES/CEL genotype with phenotype, FIP1L1-PDGFRA (+) CEL emerges as a homogeneous clinicobiological entity, where imatinib can induce molecular remission. While RT-PCR and interphase FISH are equally valid diagnostic tools, the role of marrow biopsy in diagnosis and of RQ-PCR in disease and therapy monitoring needs further evaluation.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Bain BJ . Eosinophilic leukaemias and the idiopathic hypereosinophilic syndrome. Br J Haematol 1996; 95: 2–9.
Bain BJ . Hypereosinophilia. Curr Opin Hematol 2000; 7: 21–25.
Chusid MJ, Dale DC, West BC, Wolff SM . The hypereosinophilic syndrome: analysis of fourteen cases with review of the literature. Medicine (Baltimore) 1975; 54: 1–27.
Bain B, Pierre R, Imbert M, Vardiman JW, Brunning RD, Flandrin G . Chronic eosinophilic leukemia and the hypereosinophilic syndrome. In: Jaffe ES, Harris NL, Vardiman JW (eds) WHO Classification of Tumours: Pathology and Genetics. Tumors of Haematopoietic and Lymphoid tissues. Lyon: IARC Press, 2001, pp 29–31.
Zittoun J, Farcet JP, Marquet J, Sultan C, Zittoun R . Cobalamin (vitamin B12) and B12 binding proteins in hypereosinophilic syndromes and secondary eosinophilia. Blood 1984; 63: 779–783.
Fauci AS, Harley JB, Roberts WC, Ferrans VJ, Gralnick HR, Bjornson BH . NIH conference. The idiopathic hypereosinophilic syndrome. Clinical, pathophysiologic, and therapeutic considerations. Ann Intern Med 1982; 97: 78–92.
Weller P, Bubley G . The idiopathic hypereosinophilic syndrome. Blood 1994; 83: 2759–2779.
Cools J, DeAngelo DJ, Gotlib J, Stover EH, Legare RD, Cortes J et al. A tyrosine kinase created by fusion of the PDGFRA and FIP1L1 genes as a therapeutic target of imatinib in idiopathic hypereosinophilic syndrome. N Engl J Med 2003; 348: 1201–1214.
Cools J, Stover EH, Boulton CL, Gotlib J, Legare RD, Amaral SM et al. PKC412 overcomes resistance to imatinib in a murine model of FIP1L1-PDGFRalpha-induced myeloproliferative disease. PG-459-69. Cancer Cell 2003; 5: 459–469.
Gleich GJ, Leiferman KM, Pardanani A, Tefferi A, Butterfield JH . Treatment of hypereosinophilic syndrome with imatinib mesilate. Lancet 2002; 359: 1577–1578.
Pardanani A, Reeder T, Porrata LF, Li C-Y, Tazelaar HD, Baxter EJ et al. Imatinib therapy for hypereosinophilic syndrome and other eosinophilic disorders. Blood 2003; 101: 3391–3397.
Cortes J, Ault P, Koller C, Thomas D, Ferrajoli A, Wierda W et al. Efficacy of imatinib mesylate in the treatment of idiopathic hypereosinophilic syndrome. Blood 2003; 101: 4714–4716.
Malbrain ML, Van den Bergh H, Zachee P . Further evidence for the clonal nature of the idiopathic hypereosinophilic syndrome: complete haematological and cytogenetic remission induced by interferon-alpha in a case with a unique chromosomal abnormality. Br J Haematol 1996; 92: 176–183.
Mitelman F, ISCN. An International System for Human Cytogenetic Nomenclature. Basel: S Karger, 1995.
Vandesompele J, De Preter K, Pattyn F, Poppe B, Van Roy N, De Paepe A et al. Accurate normalization of real-time quantitative RT-PCR data by geometric averaging of multiple internal control genes. Genome Biol 2002; 3, RESEARCH0034.1-0034.11.
Cools J, Quentmeier H, Huntly BJ, Marynen P, Griffin JD, Drexler HG et al. The EOL-1 cell line as an in vitro model for the study of FIP1L1-PDGFRA positive chronic eosinophilic leukemia. Blood 2003, Nov 20 [Epub ahead of print], in press.
Martin-Subero JI, Harder L, Gesk S, Schlegelberger B, Grote W, Martinez-Climent JA et al. Interphase FISH assays for the detection of translocations with breakpoints in immunoglobulin light chain loci. Int J Cancer 2002; 98: 470–474.
Pardanani A, Ketterling RP, Brockman SR, Flynn HC, Paternoster SF, Shearer BM et al. CHIC2 deletion, a surrogate for FIP1L1-PDGFRA fusion, occurs in systemic mastocytosis associated with eosinophilia and predicts response to imatinib mesylate therapy. Blood 2003; 102: 3093–3096.
Klion AD, Noel P, Akin C, Law MA, Gilliland DG, Cools J et al. Elevated serum tryptase levels identify a subset of patients with a myeloproliferative variant of idiopathic hypereosinophilic syndrome associated with tissue fibrosis, poor prognosis, and imatinib responsiveness. Blood 2003; 101: 4660–4666.
Roufosse FE, Goldman M, Cogan E . Hypereosinophilic syndrome. N Engl J Med 2003; 348: 2687.
Valent P, Horny HP, Li CY, Longley BJ, Metcalfe DD, Parwaresch RM et al. Mastocytosis. In: Jaffe ES, Harris NL, Vardiman JW (eds) WHO Classification of Tumours: Pathology and Genetics. Tumors of Haematopoietic and Lymphoid tissues. Lyon: IARC Press, 2001, pp 292–302.
Acknowledgements
We thank Dr C Peeters-De Wolf for critical reading and helpful discussions, Ursula Pluys for technical assistance with FISH, Drs H Van Keer, J Billiet and M Pilet for retrieving laboratory data and G Verbeke for statistical advice. This paper presents research results of the Belgian Programme of Interuniversity Poles of Attraction, initiated by the Belgian State, Prime Minister's Office, Science Policy Programming. The scientific responsibility is assumed by the authors. PV is a senior clinical investigator, JC a postdoctoral research fellow of Fonds voor Wetenschappelijk Onderzoek Vlaanderen. LM is partially supported by the Salus Sanguinis Foundation. This work was supported by grant G.0120.00 of the Fonds voor Wetenschappelijk Onderzoek Vlaanderen.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Vandenberghe, P., Wlodarska, I., Michaux, L. et al. Clinical and molecular features of FIP1L1-PDFGRA (+) chronic eosinophilic leukemias. Leukemia 18, 734–742 (2004). https://doi.org/10.1038/sj.leu.2403313
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.leu.2403313
Keywords
This article is cited by
-
Osteolytic lesion as initial presentation in FIP1L1-PDGFRA-rearranged myeloid/lymphoid neoplasm with eosinophilia: a case report
Annals of Hematology (2024)
-
31/w mit Schwindel, Hypästhesien der Beine und Sehstörungen
Der Onkologe (2022)
-
Myeloid Neoplasm with PDGFRA Rearrangement Manifesting as a Retromolar Pad Mass
Head and Neck Pathology (2021)
-
Paratrabecular myelofibrosis and occult mastocytosis are strong morphological clues to suspect FIP1L1-PDGFRA translocation in hypereosinophilia
Indian Journal of Hematology and Blood Transfusion (2020)