Abstract
OBJECTIVES: To review recent findings on the epidemiology, burden, diagnosis, comorbidity, and treatment of depression, particularly in general medical settings; to delineate barriers to the recognition, diagnosis, and optimal management of depression in general medical settings; and to summarize efforts under way to reduce some of these barriers.
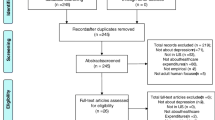
DESIGN: Medline serches were conducted to identify scientific articles published during the previous 10 years addressing depression in general medical settings and epidemiology, co-occurring conditions, diagnosis, costs, outcomes, and treatment. Articles relevant to the objective were selected and summarized.
CONCLUSIONS: Depression occurs commonly, causing suffering, functional impairment, increased risk of suicide, added health care costs, and productivity losses. Effective treatments are available both when depression occurs alone and when it co-occurs with general medical illnesses. Many cases of depression seen in general medical settings are suitable for treatment within those settings. About half of all cases of depression in primary care settings are recognized, although subsequent treatments often fall short of existing practice guidelines. When treatments of documented efficacy are used, short-term patient outcomes are generally good. Barriers to diagnosing and treating depression include stigma; patient somatization and denial; physician knowledge and skill deficits; limited time; lack of availability of providers and treatments; limitations of third-party coverage; and restrictions on specialist, drug, and psychotherapeutic care. Public and professional education efforts, destigmatization, and improvement in access to mental health care are all needed to reduce these barriers.
Similar content being viewed by others
References
Council on Scientific Affairs, American Medical Association. Informational Reports. Comorbidity; Epidemiology of Depression; Diagnosis of Depression; Treatment of Depression. Presented at the American Medical Association Annual Meeting, Chicago, Ill, June 23–27. 1991.
Robins LW, Helzer JE, Weissman MM, et al. Lifetime prevalence of specific psychiatric disorders in three sites. Arch Gen Psychiatry. 1984;41:949–58.
Kessler RC, McGonagle KA, Zhao S, et al. Lifetime and 12-month prevalence of psychiatric disorders in the United States: results from the National Comorbidity Survey. Arch Gen Psychiatry. 1994;51:8–19.
Sansone R, Sansone L. Dysthymic disorder: the chronic depression. Am Fam Physician. 1996;53:2588–94.
Myer J, Weissman MM, Tischler GL, et al. Six-month prevalence of psychiatric disorders in three communities: 1908 to 1982. Arch Gen Psychiatry. 1984;41:959–67.
Montano CB. Recognition and treatment of depression in a primary care setting. J Clin Psychiatry. 1994;55(12, suppl):18–34.
Katon W, Schulberg H. Epidemiology of depression in primary care. Gen Hosp Psychiatry. 1992;14:237–47.
Barrett JE, Barrett JA, Oxman TE, et al. The prevalence of psychiatric disorders in a primary care practice. Arch Gen Psychiatry. 1988;45:1100–6.
Schulberg HC, Madonia MJ, Block MR, et al. Major depression in primary care practice: clinical characteristics and treatment implications. Psychosomatics. 1995;36:129–37.
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4th ed. Washington, DC: American Psychiatric Press; 1994:320–7.
Coghill SR, Caplan GR. Impact of maternal postnatal depression on cognitive development of young children. BMJ. 1986;292:116–7.
Wells KB, Stewart A, Hays RD, et al. The functioning and wellbeing of depressed patients: results from the Medical Outcomes Study. JAMA. 1989;62:914–9.
Murray CJL, Lopez AD, eds. The Global Burden of Disease. Cambridge, Mass: Harvard University Press; 1996:21.
Greenberg PE, Stiglin LE, Finkelstein SN, et al. The economic burden of depression in 1990. J Clin Psychiatry. 1993;54:405–18.
Greenberg PE, Kessler RC, Nells TL, et al. Depression in the workplace: an economic perspective. In: Feighner JP, Boyer WF, eds. Selective Serotonin Uptake Inhibitors: Advances in Basic Research and Clinical Practice. 2nd ed. New York, NY: John Wiley and Sons; 1996.
Callahan CM, Kesterson JO, Tierney WM. Association of symptoms of depression with diagnostic test charges among older adults. Ann Intern Med. 1997;126:426–32.
Henks HJ, Katzelnick DJ, Kobak KA, et al. Medical costs attributed to depression among patients with a history of high medical expenses in a health maintenance organization. Arch Gen Psychiatry. 1996;53:899–904.
Unutzer J, Patrick DL, Simon G, et al. Depressive symptoms and the cost of health services in HMO patients aged 65 and older: a 4-year prospective study. JAMA. 1997;277:1618–23.
Simon GE, VonKorff M, Barlow W. Health care costs of primary care patients with recognized depression. Arch Gen Psychiatry. 1995;52:850–6.
US Preventive Services Task Force. Guide to Clinical Preventive Services. 2nd ed. Baltimore, Md: Williams and Wilkins; 1996.
Periodic Health examination, 1990 update, 2: early detection of depression and prevention of suicide. Can Med Assoc J. 1990;142:1233–8.
Goldberg DP. The Detection of Psychiatric Illness by Questionnaire. London, UK: Oxford University Press; 1972.
Beck AT, Beck RW. Screening depressed patients in family practice: a rapid technic. Postgrad Med. 1972;52:81–5.
Derogatis LR. The SCL-90-R. Baltimore, Md: Clinical Psychometrics Research; 1975.
Rush AJ, Gullion CM, Basco MR, et al. The Inventory of Depressive Symptomatology (IDS): psychometric properties. Psychol Med. 1996;26:477–86.
Zung WKW. A self-rating depression scale. Arch Gen Psychiatry. 1965;12:63–70.
Radloff LS. The CES-D scale: a self-report depression scale for research in the general population. Appl Psychol Measure 1992;7:343–51.
Sheikh JI, Yesavage JA. Geriatric Depression Scale (GDS): recent evidence and development of a shorter version. Clin Gerontol. 1986;5:165–73.
Lyness JM, Noel TK, Cox C, et al. Screening for depression in elderly primary care patients. Arch Intern Med. 1997;157:449–54.
Weissman M, Olfson M, Leon AC, et al. Brief diagnostic interviews (SDDS-PC) for multiple mental disorders in primary care. Arch Fam Med. 1995;4:220–7.
Spitzer RL, Williams JBW, Kroenke K, et al. Utility of a new procedure for diagnosing mental disorders in primary care: the PRIME-MD 1000 study. JAMA. 1994;272:1749–56.
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 4th ed. Primary Care Version. Washington, DC: American Psychiatric Press; 1995.
Wolraich ML, Felice ME, Drotar D, eds. Diagnostic and Statistical Manual for Primary Care, Child and Adolescent Version. Elk Grove Village, Ill: American Academy of Pediatrics; 1996.
Ustun B, Goldberg D, Cooper J, et al. New classification for mental disorders with management guidelines for use in primary care, the ICD-10 PHC chapter 5. Br J Gen Pract. 1995;45:211–5.
Glassman AH. Cigarette smoking: implications for psychiatric illness. Am J Psychiatry. 1993;150:546–51.
Stoudemire A, Fogel BS. Principles of Medical Psychiatry. 2nd ed. Orlando, Fla: Grune & Stratton; 1993.
Rundell JR, Wise MG, eds. American Psychiatric Press Textbook of Consultation-Liaison Psychiatry. Washington, DC: American Psychiatric Press; 1996.
Nesse R, Finlayson R. Management of depression in patients with coexisting medical illness. Am Fam Physician. 1996:53:2123–33.
Caine ED, Lyness JM, Conwell Y. Diagnosis of late-life depression: preliminary studies in primary care settings. Am J Geriatr Psychiatry. 1996;4(suppl):S45–50.
Callahan CM, Hendrie HC, Tierney WM. The recognition and treatment of late-life depression: a view from primary care. Int J Psychiatry Med. 1996;26:155–71.
Covinsky KE, Fortinsky RH, Palmer RM, et al. Relation between symptoms of depression and health status outcomes in acutely ill hospitalized older persons. Ann Intern Med. 1997;126:417–25.
Quill TE. Doctor, I want to die. Will you help me? JAMA. 1993;270:870–3.
Masand PS, Chengappa KNR, Edwards W. Somatic treatments. In: Goldman LS, Wise T, Brody D, eds. Psychiatry for Primary Care Physicians. Chicago, Ill: American Medical Association; 1998:331–64.
Jarrett RB, Rush AJ. Short-term psychotherapy of depressive disorders: current status and future directions. Psychiatry. 1994;57:115–32.
McLean PD, Hakstian AR. Clinical depression: comparative efficacy of outpatient treatments. J Consult Clin Psychol. 1979;47:818–36.
Shea MT, Elkin E, Hirschfeld RMA. Psychotherapeutic treatment of depression. In: Frances AJ, Hales RE, eds. Review of Psychiatry. Washington, DC: American Psychiatric Press; 1988:235–55.
Brodaty H, Andrews G. Brief psychotherapy in family practice: a controlled prospective intervention trial. Br J Psychiatry. 1983;143:11–9.
Mynors-Wallis LM, Gath DH, Lloyd-Thomas AR, et al. Randomised controlled trial comparing problem-solving treatment with amitriptyline and placebo for major depression in primary care. BMJ. 1995;310:441–5.
Clarkin JF, Pilkonis PA, Magruder KM. Psychotherapy of depression: implications for reform of the health care system. Arch Gen Psychiatry. 1996;53:717–23.
Kupfer DJ, Frank E, Perel JM, et al. Five-year outcome for maintenance therapies in recurrent depression. Arch Gen Psychiatry. 1992;49:769–73.
Frank E, Kupfer DJ, Wagner EF, et al. Efficacy of interpersonal psychotherapy as a maintenance treatment of recurrent depression: contributing factors. Arch Gen Psychiatry. 1991;48:1053–9.
Agency for Health Care Policy and Research. Depression in Primary Care. Washington, DC: US Government Printing Office; 1993.
Regier DA, Narrow WE, Rae DS, et al. The de facto US mental and addictive disorders service system: Epidemiologic Catchment Area prospective 1-year prevalence rates of disorders and services. Arch Gen Psychiatry. 1993;50:85–94.
Goldberg D. Epidemiology of mental disorders in primary care settings. Epidemiol Rev. 1995;7:182–90.
Wells KB, Hays RD, Burnam A, et al. Detection of depressive disorder for patients receiving prepaid or fee-for-service care: results from the Medical Outcomes Study. JAMA. 1989;262:3298–302.
Wells KB. Depression in medical settings: implications of three health policy studies for consultation-liaison psychiatry. Psychosomatics. 1994;35:279–96.
Badger LW, deGruy FV, Hartman J, et al. Psychosocial interest, medical interviews, and the recognition of depression. Arch Fam Med. 1994;3:899–907.
Robbins JM, Kirmayer LJ, Cathbras P, et al. Physician characteristics and the recognition of depression and anxiety in primary care. Med Care. 1994;32:795–812.
Simon GE, VonKorff M. Recognition, management, and outcomes of depression in primary care. Arch Fam Med. 1995;4:99–105.
Tiemens BG, Ormel J, Simon GE. Occurrence, recognition, and outcome of psychological disorders in primary care. Am J Psychiatry. 1996;153:636–44.
Katon W, Gonzales J. A review of randomized trials of psychiatric consultation-liaison studies in primary care. Psychosomatics. 1994;35:268–78.
Schulberg HC, Magruder KM, deGruy F. Major depression in primary medical care practice: research trends and future priorities. Gen Hosp Psychiatry. 1996;18:395–406.
Higgins ES. A review of unrecognized mental illness in primary care. Arch Fam Med. 1994;3:908–17.
Chang G. Wamer V, Weissman MM. Physicians’ recognition of psychiatric disorders in children and adolescents. Am J Dis Child. 1988;142:736–9.
Costello EJ, Edelbrock C, Costello AJ, et al. Psychopathology in pediatric primary care: the new hidden morbidity. Pediatrics. 1988;82:415–24.
Canning EH, Hanser SB, Shade KA, et al. Mental disorders in chronically ill children: parent-child discrepancy and physician identification. Pediatrics. 1992;90:692–6.
Lavigne JV, Binns HJ, Christoffel KK, et al. Behavioral and emotional problems among preschool children in pediatric primary care: prevalence and pediatricians’ recognition. Pediatrics. 1993;91:649–55.
Katon W, Von Korff M, Lin E, et al. Adequacy and duration of antidepressant treatment in primary care. Med Care. 1992;30:67–76.
Wells KB, Sturm R, Sherbourne CD, Meredith LS. Caring for Depression. Cambridge, Mass: Harvard University Press; 1996.
Schulberg HC, Block MR, Madonia MT, et al. The ‘usual’ care of major depression in primary care practice. Arch Fam Med. 1997;6:334–9.
Meredith LS, Wells KB, Kaplan SH. Counseling provided for depression: role of clinician specialty and payment system. Arch Gen Psychiatry. 1996;53:905–12.
Katzelnick DJ, Kobak KA, Greist JH, et al. Effect of primary care treatment of depression on service use by patients with high medical expenditures. Psychiatr Serv. 1997;48:59–64.
Sturm R, Wells KB. How can care for depression become more cost-effective? JAMA. 1995;273:51–8.
Schulberg HC, Block MR, Madonia MJ, et al. Treating major depression in primary care practice. Arch Gen Psychiatry. 1996;53:913–9.
Schulberg HC, Block MR, Madonia MJ, et al. Applicability of clinical pharmacotherapy guidelines for major depression in primary care settings. Arch Fam Med. 1995;4:106–12.
Coulehan JL, Schulberg HC, Block MR, et al. Treating depressed primary care patients improves their physical, mental, and social functioning. Arch Intern Med. 1997;157:1113–20.
Katon W, Robinson P, Von Korff M, et al. A multifaceted intervention to improve treatment of depression in primary care. Arch Gen Psychiatry. 1996;53:924–32.
Katon W, Von Korff M, Lin E, et al. Collaborative management to achieve treatment guidelines: impact on depression in primary care. JAMA. 1995;273:1026–31.
Von Korff M, Katon W, Bush T, et al. Treatment costs, cost offset, and cost-effectiveness of collaborative management of depression. Psychosomatic Med. 1998;60:143–9.
Rost K, Smith R, Matthews DB, et al. The deliberate misdiagnosis of major depression in primary care. Arch Fam Med. 1994;3:333–7.
Docherty JP. Barriers to the diagnosis of depression in primary care. J Clin Psychiatry. 1997;58(suppl 1):5–10.
Goldman LS. Psychiatry in primary care: possible roles for organized medicine. Psychiatr Ann. 1997;27:425–9.
Cohen-Cole S. The Medical Interview: The Three Function Approach. St. Louis, Mo: Mosby-Yearbook; 1991.
Barsky AJ, Borus JB. Somatization and medicalization in the era of managed care. JAMA. 1995;274:1931–4.
Goldberg D. Detection and assessment of emotional disorders in a primary care setting. Int J Ment Health. 1979;8:30–48.
Eisenberg L. Treating depression and anxiety in primary care: closing the gap between knowledge and practice. N Engl J Med. 1992;326:1080–3.
Tylee AT, Freeling P, Kerry S. Why do general practitioners recognize major depression in one woman patient yet miss it in another? Br J Gen Pract. 1993;43:327–30.
Rollman BL, Block MR, Schulberg HC. Symptoms of major depression and tricyclic side effects in primary care patients. J Gen Intern Med. 1997;12:284–91.
Simon GE, Lin EH, Katon W, et al. Outcomes of “inadequate” antidepressant treatment. J Gen Intern Med. 1995;10:663–70.
Basco MR, Rush AJ. Compliance with pharmacotherapy in mood disorders. Psychiatric Ann. 1995;25:269–70,276,278–9.
Simon GE, VonKorff M, Heiligenstein JH, et al. Initial antidepressant choice in primary care: effectiveness and cost of fluoxetine vs tricyclic antidepressants. JAMA. 1996;275:1897–902.
Sclar D, Robison LM, Skaer TL, et al. Antidepressant pharmacotherapy: economic outcomes in a health maintenance organization. Clin Ther. 1994;16:715–30.
Hirschfield RMA, Keller MB, Panico S, et al. The National Depressive and Manic-Depressive Association consensus statement on the undertreatment of depression. JAMA. 1997;277:333–40.
Cole SA, Sullivan M, Kathol R, et al. A model curriculum for mental disorders and behavioral problems in primary care. Gen Hosp Psychiatry. 1995;17:13–8.
Commission on Health Care Services. White Paper on the Provision of Mental Health Care Services by Family Physicians. Kansas City, Mo: The American Academy of Family Physicians; 1994.
Jones LR, Knopke HJ, Parlour RR, et al. A curriculum for the psychiatric training of family physicians. Gen Hosp Psychiatry. 1981;3:189–98.
American Psychiatric Association Work Group on Major Depressive Disorder. Practice guideline for major depressive disorder in adults. Am J Psychiatry. 1993;150(suppl):1–26.
Brown J, Stewart M, McCracken E, et al. The patient-centered clinical method, II: definition and application. Fam Pract. 1986;3:75–9.
Gask L, Goldberg D. Impact on patient care, satisfaction, and clinical outcome of improving the psychiatric skills of general practitioners. Eur J Psychiatry. 1993;7:203–18.
Regier DA, Hirschfield RMA, Goodwin FK, et al. The NIMH Depression Awareness, Recognition, and Treatment Program: structure, aim, and scientific basis. Am J Psychiatry. 1988;145:1351–7.
Paykel ES, Tylee A, Wright A, et al. The Defeat Depression Campaign: psychiatry in one public arena. Am J Psychiatry. 1997;154(suppl):59–65.
Author information
Authors and Affiliations
Consortia
Additional information
Address correspondence and reprint requests to Dr. Bresolin: Secretary to the Council on Scientific Affairs, American Medical Association, 515 N. State Street, Chicago, IL 60610.
Members and staff of the Council on Scientific Affairs at the time this report was prepared: Ronald M. Davis, MD, Detroit, Mich (Chair); Joseph A. Riggs, MD, Haddon Fields, NJ (Chair-Elect); Roy D. Altman, MD, Miami, Fla; Hunter C. Champion, New Orleans, La; Scott D. Deitchman, MD, MPH, Decatur, Ga; Myron Genel, MD, New Haven, Conn; John P. Howe III, MD, San Antonio, Tex; Mitchell S. Karlan, MD, Los Angeles, Calif; Mohamed Khaleem Khan, MD, PhD, Boston, Mass; Nancy H. Nielsen, MD, PhD, Buffalo, NY; Michael A. Williams, MD, Baltimore, Md; Donald C. Young, MD, Iowa City, Iowa; Linda B. Bresolin, PhD (CSA Secretary), Barry D. Dickinson, PhD (CSA Assistant Secretary), Chicago, III; Larry S. Goldman, MD (Department of Psychiatry, University of Chicago).
Rights and permissions
About this article
Cite this article
Goldman, L.S., Nielsen, N.H., Champion, H.C. et al. Awareness, diagnosis, and treatment of depression. J GEN INTERN MED 14, 569–580 (1999). https://doi.org/10.1046/j.1525-1497.1999.03478.x
Issue Date:
DOI: https://doi.org/10.1046/j.1525-1497.1999.03478.x