-
PDF
- Split View
-
Views
-
Cite
Cite
Jutta Passlick-Deetjen, Eva Bedenbender-Stoll, Why thermosensing? A primer on thermoregulation, Nephrology Dialysis Transplantation, Volume 20, Issue 9, September 2005, Pages 1784–1789, https://doi.org/10.1093/ndt/gfh901
Close - Share Icon Share
Introduction
Symptomatic hypotension is a frequent complication during haemodialysis treatment sessions. One of the reasons is rapid blood volume reduction with inadequate vasoconstriction. Furthermore, heat accumulation during dialysis occurs and leads to decreased peripheral resistance and thus decreased venous return. As a consequence, cooler than the usual dialysate temperatures were used and showed an advantage for cardiovascular stability during haemodialysis [1–12]. This practice has not been applied in clinical routine up to now, as patients dependent on their actual temperature suffered from shivering. If future practice would take the optimal individualized dialysate temperature of patients into account, the quality of dialysis treatment could be further improved. The question, however, is which is the optimal dialysate temperature, and how can it be achieved? In order to answer this question in more detail some principles of thermoregulation will be discussed.
Principles of thermoregulation
Humans are homeothermic organisms and body temperature regulation is tight as this is essential for cell functioning [13,14].
General principles of heat gain and heat loss of the body
The body constantly produces heat (energy) and exchanges it with the environment. Body temperature is kept constant if energy gain equals energy loss [15,16]. If energy gain does not equal energy loss the extra heat is ‘stored’, or lost from the body [14].
There are three principal components of human energy (heat) generation: basal metabolic heat production, thermogenesis via food and physical activity [17]. Further heat is produced through metabolism modulated by hormones (e.g. catecholamines and thyroxin) [14], emotions and medication [17]. The basal metabolic rate is the energy produced by a resting individual in a thermoneutral environment (20–27°C) in a supine position at complete rest after sleep, 12 h after the last meal [15,17]. It is the energy amount needed for basic functions such as respiration and cardiac function to provide body cells with oxygen and nutrients [16].
In humans the main heat exchange with the environment takes place by convection, evaporation and radiation via the skin. Sweating for thermoregulation sets in only when the ambient temperature exceeds 30°C [14].
Aschoff [reviewed in 13] was the first to suggest that one should differentiate between ‘body core temperature’, which is maintained around 37°C and ‘body shell temperature’, which depends largely on the environmental temperature [13]. In a cold environment the shell is thick and skin temperature much lower than in a warm environment, where the shell may be <1 cm. Besides the air temperature, air movement and thermal radiation, sweat secretion, skin blood flow and the temperature of the underlying tissue also influence body shell or skin temperature [14].
In order to regulate body core and shell temperature the human brain coordinates a range of behavioural and autonomic control mechanisms [18]. Body core and shell temperature changes are sensed by either cutaneous or deep body thermoreceptors [14]. Bare nerve endings just underneath the skin are very temperature sensitive. They are classified as either warm or cold receptors [14]. Cold receptors react in a range of −5 to 43°C, warm receptors only above 30°C, their static impulse frequency rises with temperature, reaches a maximum and falls again at high temperatures. There is some overlap of the static discharge of warm and cold receptor populations in a range from about 30 to 43°C [19]. [The data for cold receptors static discharge frequency were obtained from animal experiments, data for warm receptors static discharge frequency were obtained both in humans and experimental animals.] A dynamic response of nerves is given if temperature changes rapidly. On sudden heating of the skin, warm receptors respond with a transient overshoot in frequency. On the other hand the activity of cold receptors is suppressed. Sudden cooling causes reverse effects [14].
Body core thermoreceptors are concentrated in the hypothalamus but they are also located at other core sites, including the midbrain, medulla, spinal cord, cortex and deep abdominal structures [14,15,20].
Skin and body core temperature receptors transmit their information through afferent nerves to the brainstem, especially to the pre-optic/anterior hypothalamus [14]. Neurons of the pre-optic/anterior hypothalamus have a key function in coordinating many (but not all) effector mechanisms by efferent connections [14,18]. In a simplified model the area of the pre-optic/anterior hypothalamus can be related to a thermostat, which initiates thermoregulatory responses when the temperature sensed is different from a specific thermoregulatory set point [14,21].
The reflex control of e.g. sweating and skin blood flow depends on the integrated body core and skin temperature. Each of these responses has a core temperature threshold, which depends on mean skin temperature. Any change of core temperature elicits a 9× thermoregulatory response compared to the same change in skin temperature [14]. For example, if body core temperature during dialysis increases from 36.5 to 37.0°C, which frequently happens, this has a 9× greater effect on skin blood flow compared to an increase in mean skin temperature of 0.5°C.
Other autonomic changes, like metabolic heat production by muscle activity and shivering, evaporation of water by sweating and behavioural changes, such as adjusting environmental temperature or clothing, are all part of temperature regulation [22].
Control of skin blood flow
Most heat exchange of the body with the environment occurs via the skin [23]. In a person who is not sweating, the body controls convective and radiative heat loss by varying skin blood flow. Lowering skin blood flow results in an adaptation of skin temperature to ambient temperature, whereas an increase in skin blood flow brings skin temperature nearer to core temperature [14].
Neural reflex control of skin blood flow is mediated through two populations of sympathetic nerves: the known adrenergic vasoconstrictor system and a less well understood sympathetic vasodilator system, which is responsible for 80–90% of the substantial cutaneous vasodilatation that occurs with whole body heat stress [21].
In most circumstances it is sufficient to decrease and increase sympathetic vasoconstrictor nerve activity in order to regulate body temperature within narrow limits [24]. During heat stress, however, this tonic sympathetic vasoconstriction is released and cutaneous active vasodilatation is initiated, causing a rise in skin blood flow, convection of heat from internal organs and striated muscles to the body surface and an increase in skin temperature [25].
The neural mechanism of cutaneous active vasodilatation is not completely understood. Apparently it is mediated by cholinergic nerves; the transmitter, however, is not only acetylcholine, but co-transmitters, such as vasoactive intestinal polypeptide, are also released to elicit a response [23].
Under thermoneutral conditions and at rest total skin blood flow is ∼200–500 ml/min (5–10% of cardiac output) [23,26]. Active vasodilatation in response to heat stress, as in haemodialysis, can increase skin blood flow to 8 l/min, which is about 60% of the cardiac output [23,24].
Individual differences in temperature regulation
Thermoregulation of body core temperature is influenced by physiological (e.g. time of day, age, gender) and pathological (e.g. fever) factors [adapted from 14].
Body core temperature undergoes diurnal variation with a nadir in the early morning and a peak in the evening [27].
In elderly individuals the thermoregulatory response to cold exposure is often inadequate [28–30]. This may partly be due to decreased heat conservation during cold exposure caused by ineffective vasoconstriction [29–32] or reduction of metabolically active tissue [31]. Decreased sweat gland function and/or reduced skin vasodilatory response may underlie the reduced thermoregulatory response to heat stress in elderly individuals [28].
Furthermore, thermoregulation depends on gender. For example, after heat stress women had higher skin temperatures and lower sweat rates than men, but when subjects were matched for body fatness, heat storage and tolerance time, there was no difference between genders [33]. Some gender-related differences may be caused by different body composition and anthropometry [34] as well as by hormonal differences, body water regulation, exercise capacity [35] or others [34].
The challenge of thermoregulation in haemodialysis patients
Body temperature in healthy subjects and in haemodialysis patients
In the late 19th century Wunderlich et al. took axillary temperature readings from 25 000 patients and found body temperatures in a range between 36.2 and 37.5°C, with 37°C as the mean temperature. He also recognized a circadian pattern as well as gender and age related differences. In spite of these individual differences, 37°C has been uncritically accepted as the ‘normal body temperature’ [36]. Investigations comparing a thermometer that is believed to have beeen one of Wunderlich's thermometers with more modern instruments showed, however, that the calibration of Wunderlich's instrument may have been too high by 1.4°C to 2.2°C [37]. More recent studies measured mean body temperature in healthy subjects aged 18–40 years around 36.8°C [38] or 36.86°C in subjects aged 64 years and older [39].
In haemodialysis patients different mean body temperatures were measured. Fine and Penner [2] showed that 62.5% of 128 HD patients had predialysis body temperatures below 36.5°C. In contrast, Pérgola et al. [36] showed that the body temperature of haemodialysis patients was only slightly lower than in healthy subjects when artefacts from circadian changes were taken into consideration. Another study in 24 HD patients (during 81 treatments) showed that 88% of the patients had pre-dialytic body temperatures below 37°C but there were large inter- and intra-individual differences in the values for pre-dialytic body temperature [M. Krämer, unpublished data], probably based on circadian rhythm, age and gender.
Despite these investigations, dialysate temperature is usually uniformly fixed at 37°C. Based on the above mentioned regulatory mechanisms in response to changes in body core temperature, there is an obvious need to individualize dialysate temperature.
But if individualization is necessary, the pre-condition is exact measurement of body temperature. Unfortunately the different methods of body temperature estimation yield substantially different results.
What is the best method for estimating body temperature in order to adapt and individualize dialysate temperature?
Oral, tympanic and axillary temperatures are not very accurate. Oesophageal temperature measurement is difficult, and uncomfortable as a thermistor has to be inserted; furthermore irritation of nasal passages may influence the result. Rectal temperature measurement seems to be an accurate method for estimating core temperature, but is not suitable as it is labour intensive and has a prolonged response time [40].
During dialysis, however, the most practical site to assess body temperature would be the vascular access, which is mostly placed on the arm. In the arterial and venous lines of the extracorporeal blood circulation, temperature can be measured non-invasively with, e.g., a blood temperature monitor (BTM), which is a device integrated in standard HD machines. After correction of arterial blood temperature for recirculation, approximate body temperature can be estimated [41].
Influence of the extracorporeal circuit on body temperature
In the past a standard dialysate temperature ≥37°C was used because of the assumption that this may be a physiological temperature [42] and that a dialysate temperature above core temperature compensates for heat loss from the extracorporeal circuit [43]. But in fact patients experience heat gain during such standard haemodialysis and their body temperature increases by up to 0.67°C [44] with the respective consequences. The temperature rise may be caused by transfer of heat into the body, by endogenous heat production and by a reduced heat loss via the skin, which leads to heat accumulation [45].
In order to avoid net uptake of heat (energy) initially, so-called thermoneutral dialysis was applied in a study by Maggiore et al. [46]. This procedure implies that there is no heat transfer from the extracorporeal blood and the dialysate (ΔEnergy = 0 KJ/h) to the patient. Nevertheless, the body core temperature increased on average by 0.47°C. This observation led to the conclusion that external transfer of heat is not the only cause of heat gain during dialysis.
In contrast to some results which showed that haemodialysis patients have resting energy expenditure (REE) comparable to that of healthy persons [47–49], Ikizler et al. [50] studied 10 dialysis patients and found higher than normal REE levels, which further increased during haemodialysis. Considering that patients had no residual renal function the higher REE is all the more notable as a functioning kidney accounts for 8% of REE [50]. The rise in metabolic rate, i.e. REE, during dialysis may be caused by the dialysis procedure per se. Presumably shifts of solutes and water between body compartments lead to energy-expending processes. Sympathetic activation as the result of blood volume reduction may also increase muscle activity and muscular energy production [45].
Another reason for the increase of body temperature may be the decreased dissipation of heat via the body surface. The physiological response to acute blood volume reduction as a result of ultrafiltration is an increase in sympathetic vasoconstriction of the peripheral blood vessels. Consequently, skin blood flow declines and heat exchange between the body and the environment decreases [45]. This mechanism was first described by Gotch et al. [51] and confirmed by a study of Rosales et al. [52]. In this study haemodialysis patients were treated with the BTM (Fresenius Medical Care, Bad Homburg, Germany) which kept body temperature constant (isothermic dialysis) [52]. They demonstrated that the amount of energy that must be withdrawn in order to keep the body temperature constant was perfectly correlated to the ultrafiltration volume.
Why thermosensing?
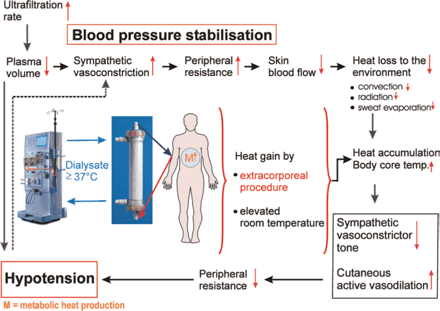
Accumulation of heat induced by ultrafiltration continues until a threshold body core temperature is reached. At this point sympathetic vasoconstriction ceases, and active vasodilatation begins. Peripheral resistance decreases with a hypotensive episode as the end result [45]. Figure 1 summarizes possible causes of heat accumulation and triggers of symptomatic hypotension during dialysis.
Possible causes for heat accumulation during haemodialysis resulting in hypotension.
The fact that high dialysate temperatures (≥37°C) cause haemodynamic instability has been confirmed by numerous studies [1–12]. In spite of its proven advantage for cardiovascular stability cold dialysis has not been widely used in dialysis practise. Patients often complain that they feel ‘cold’ when dialysate temperature is lowered but not individualized [2,8,53].
The above-mentioned points lead to the conclusion that there is not one single optimal dialysate temperature. There are major inter- and intra-individual differences in body core and skin temperatures of haemodialysis patients. The risks of hypotensive episodes varies also: such episodes are more frequent during the warm summer months [54–56].
Dialysis treatment per se has an effect on the patients’ thermoregulatory system and cardiac stability. The dialysate temperature should therefore be continuously adjusted in order to maintain the body temperature of the patient at the predialysis value throughout the dialysis session. This goal can only be achieved by blood temperature controlled dialysis under isothermic conditions. Isothermic dialysis keeps body core temperature constant and removes the extra heat, which is produced by the dialytic process and by the individually variable metabolic and sympathetic response of the dialysis patient. Patients with low body core temperatures and with an increased risk of suffering from symptomatic hypotension will benefit especially from isothermic dialysis.
Thermosensing during dialysis—optimal conditions for cardiovascular stability
Maggiore et al. [46] compared the effects of BTM-controlled dialysis with thermoneutral (dialysate temperature equals patient's temperature) and isothermic (patient's temperature is kept constant) conditions on 95 hypotensive-prone haemodialysis patients. During isothermic dialysis the temperature of the patient was kept constant by adjusting the dialysate temperature according to the actually measured ‘arterial’ temperature at the vascular access.
During thermoneutral HD the frequency of hypotensive episodes was nearly identical to that observed with standard HD during the screening phase. However with, isothermic dialysis, the incidence of sessions with hypotensive episodes decreased from 50 to 25%. Blood pressure decrease and the increase in heart rate were less pronounced during isothermic HD than during thermoneutral HD.
The results document that haemodynamic stability is improved with isothermic HD vs standard HD (screening phase) [46] possibly because of increased peripheral vascular resistance [4,57], increased nor-epinephrine levels [4] or increased left ventricular contractility [58].
Conclusion
Because of the considerable variations in body temperature and its regulation, it does not make sense to believe in the Communist dogma that ‘one dialysate temperature fits all’ at all times of the year and throughout the day. As a consequence the dialysis treatment must be adapted to the patient's individual condition and response to treatment. Nephrologists should take into consideration that a change in core temperature by a few tenths of a degree Centigrade—not uncommon during dialysis—causes a huge change in skin blood flow response. Therefore, dialysate temperature should be individualized.
Conflict of interest statement. J. Passlick-Deetjen is an employee of Fresenius Medical Care. E. Bedenbender-Stoll declares no conflicts on interest.
References
Ayoub A, Finlayson M. Effect of cool temperature dialysate on the quality and patients’ perception of haemodialysis.
Fine A, Penner B. The protective effect of cool dialysate is dependent on patients’ predialysis temperature.
Maggiore Q, Dattolo P, Piacenti M et al. Thermal balance and dialysis hypotension.
Jost CM, Agarwal R, Khair-el-Din T, Grayburn PA, Victor RG, Henrich WL. Effects of cooler temperature dialysate on hemodynamic stability in ‘problem’ dialysis patients.
Kerr PG, van Bakel C, Dawborn JK. Assessment of the symptomatic benefit of cool dialysate.
Marcen R, Orofino L, Quereda C, Pascual J, Ortuno J. Effects of cool dialysate in dialysis-related symptoms.
Bazzato G, Coli U, Landini S et al. Temperature monitoring in dialysis-induced hypotension.
Sherman RA, Rubin MP, Cody RP, Eisinger RP. Amelioration of hemodialysis-associated hypotension by the use of cool dialysate.
Pizzarelli F, Sisca S, Zoccali C et al. Blood temperature and cardiovascular stability in hemofiltration.
Coli U, Landini S, Lucatello S et al. Cold as cardiovascular stabilizing factor in hemodialysis: hemodynamic evaluation.
Maggiore Q, Pizzarelli F, Sisca S et al. Blood temperature and vascular stability during hemodialysis and hemofiltration.
Maggiore Q, Pizzarelli F, Zoccali C, Sisca S, Nicolo F, Parlongo S. Effect of extracorporeal blood cooling on dialytic arterial hypotension.
Gilbert SS, van den Heuvel CJ, Ferguson SA, Dawson D. Thermoregulation as a sleep signalling system.
Adair ER, Black DR. Thermoregulatory responses to RF energy absorption.
Levine JA. Nonexercise activity thermogenesis (NEAT): environment and biology.
McAllen RM. Preoptic thermoregulatory mechanisms in detail.
Jessen C.
Charkoudian N. Skin blood flow in adult human thermoregulation: how it works, when it does not, and why.
Cooper KE. Some responses of the cardiovascular system to heat and fever.
Bennett LA, Johnson JM, Stephens DP, Saad AR, Kellogg DL Jr. Evidence for a role for vasoactive intestinal peptide in active vasodilatation in the cutaneous vasculature of humans.
Johnson JM, Proppe DW.
Van Someren EJ, Raymann RJ, Scherder EJ, Daanen HA, Swaab DF. Circadian and age-related modulation of thermoreception and temperature regulation: mechanisms and functional implications.
Rowell LB. Cardiovascular adjustments of thermal stress. In: Sheperd J, Abboud F, eds.
Aoki K, Stephens DP, Johnson JM. Diurnal variation in cutaneous vasodilator and vasoconstrictor systems during heat stress.
Inoue Y, Nakao M, Araki T, Ueda H. Thermoregulatory responses of young and older men to cold exposure.
Khan F, Spence VA, Belch JJ. Cutaneous vascular responses and thermoregulation in relation to age.
Wagner JA, Robinson S, Marino RP. Age and temperature regulation of humans in neutral and cold environments.
Florez-Duquet M, McDonald RB. Cold-induced thermoregulation and biological aging.
Kenney WL, Armstrong CG. Reflex peripheral vasoconstriction is diminished in older men.
McLellan TM. Sex-related differences in thermoregulatory responses while wearing protective clothing.
Stocks JM, Taylor NA, Tipton MJ, Greenleaf JE. Human physiological responses to cold exposure.
Kaciuba-Uscilko H, Grucza R. Gender differences in thermoregulation.
Pérgola PE, Habiba NM, Johnson JM. Body temperature regulation during hemodialysis in long-term patients: is it time to change dialysate temperature prescription?
Mackowiak PA, Worden G. Carl Reinhold August Wunderlich and the evolution of clinical thermometry.
Mackowiak PA, Wasserman SS, Levine MM. A critical appraisal of 98.6°F, the upper limit of the normal body temperature, and other legacies of Carl Reinhold August Wunderlich.
McGann KP, Marion GS, Camp L, Spangler JG. The influence of gender and race on mean body temperature in a population of healthy older adults.
Moran DS, Mendal L. Core temperature measurement: methods and current insights.
Locatelli F, Buoncristiani U, Canaud B, Kohler H, Petitclerc T, Zucchelli P. Haemodialysis with on-line monitoring equipment: tools or toys?
Maggiore Q, Dattolo P, Piacenti M et al. Thermal balance and dialysis hypotension.
Schneditz D. Temperature in hemodialysis.
Donauer J, Böhler J. Rationale for the use of blood volume and temperature control devices during hemodialysis.
Maggiore Q, Pizzarelli F, Santoro A et al. Study Group of Thermal Balance and Vascular Stability. The effects of control of thermal balance on vascular stability in hemodialysis patients: results of the European randomized clinical trial.
Kuhlmann U, Schwickardi M, Lange, H. Energy expenditure in patients with renal failure.
Monteon FJ, Laidlaw SA, Shaib JK, Kopple JD. Energy expenditure in patients with chronic renal failure.
Schneeweiss B, Graninger W, Stockenhuber F et al. Energy metabolism in acute and chronic renal failure.
Ikizler TA, Wingard RL, Sun M, Harvell J, Parker RA, Hakim RM. Increased energy expenditure in hemodialysis patients.
Gotch FA, Keen ML, Yarian SR. An analysis of thermal regulation in hemodialysis with one and three compartment models.
Rosales LM, Schneditz D, Chmielnicki H, Shaw K, Levin NW. Exercise and extracorporeal blood cooling during hemodialysis.
Provenzano R, Sawaya B, Frinak S et al. The effect of cooled dialysate on thermal energy balance in hemodialysis patients.
Verdon F, Boudry JF, Chuat M, Studer JP, Truong CB, Jacot E. Seasonal variations in arterial pressure in hypertensive patients.
Argani H, Javanshir MR. Seasonal variations of blood pressure in hemodialysis and renal transplant recipients.
Cheung AK, Yan G, Greene T et al. Hemodialysis Study Group. Seasonal variations in clinical and laboratory variables among chronic hemodialysis patients.
Kaufman AM, Morris AT, Lavarias VA et al. Effects of controlled blood cooling on hemodynamic stability and urea kinetics during high-efficiency hemodialysis.
Author notes
1Fresenius Medical Care, Bad Homburg v. d. H., Heinrich-Heine University, Düsseldorf, Germany and 2Ginsterweg 8, 61169 Friedberg, Germany





Comments