Abstract
OBJECTIVE: To determine if type of hospital ownership is associated with preventable adverse events.
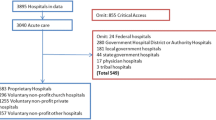
DESIGN: Medical record review of a random sample of 15,000 nonpsychiatric, non-Veterans Administration hospital discharges in Utah and Colorado in 1992.
MEASUREMENTS AND MAIN RESULTS: A two-stage record review process using nurse and physician reviewers was used to detect adverse events. Preventability was then judged by 2 study investigators who were blinded to hospital characteristics. The association among preventable adverse events and hospital ownership was evaluated using logistic regression with nonprofit hospitals as the reference group while controlling for other patient and hospital characteristics. We analyzed 4 hospital ownership categories: nonprofit, for-profit, major teaching government (e.g., county or state ownership), and minor or nonteaching government.
RESULTS: When compared with patients in nonprofit hospitals, multivariate analyses adjusting for other patient and hospital characteristics found that patients in minor or nonteaching government hospitals were more likely to suffer a preventable adverse event of any type (odds ratio [OR] 2.46; 95% confidence interval [CI], 1.45 to 4.20); preventable operative adverse events (OR, 4.85; 95% CI, 2.44 to 9.62); and preventable adverse events due to delayed diagnoses and therapies (OR, 4.27; 95% CI, 1.48 to 12.31). Patients in forprofit hospitals were also more likely to suffer preventable adverse events of any type (OR, 1.57; 95% CI, 1.03 to 2.38); preventable operative adverse events (OR, 2.63; 95% CI, 1.42 to 4.87); and preventable adverse events due to delayed diagnoses and therapies (OR, 4.15; 95% CI, 1.84 to 9.34). Patients in major teaching government hospitals were less likely to suffer preventable adverse drug events (OR, 0.38; 95% CI, 0.16 to 0.89).
CONCLUSIONS: Patients in for-profit and minor teaching or nonteaching government-owned hospitals were more likely to suffer several types of preventable adverse events. Further research is needed to determine how these events could be prevented.
Similar content being viewed by others
References
Eckholm E. While congress remains silent, healthcare transforms itself. New York Times. December 18, 1994:A1.
Tomsho R. Giant hospital chain uses tough tactics to push fast growth. Wall Street Journal. July 12, 1994:A1, A6.
Gray B. H. Conversion of HMO’s and hospitals: what’s at stake? Health Aff (Millwood). 1997;16(2):29–47.
Ad Hoc Committee to Defend Health. For our patients, not for profits: a call to action. JAMA. 1997;278:1733–4.
Prospective Payment Assessment Commission. Annual Report. Washington, DC; 1991.
Andrulis DP. The public sector in health care: evolution or dissolution? Health Aff (Millwood). 1997;16(4):131–40.
Arrow KJ. Uncertainty and the Welfare economics of medical care. Am Econ Rev. 1963;53:941–73.
Starr P. The Social Transformation of American Medicine. New York, NY: Basic Books; 1982.
Pellegrino E. In: Williams K, Donnelly P, eds. Medical Care Quality and the Public Trust. Chicago, Ill: Pluribus Press; 1982;ix-xiv.
Ginzberg E. For-profit medicine, reassessment. N Engl J Med. 1988;319:757–61.
Relman AS. The new medical-industrial complex. N Engl J Med. 1980;303:963–70.
Relman AS. Shattuck Lecture. The health care industry: where is it taking us? N Engl J Med. 1991;325:854–9.
Shortell SM, Hughes EF. The effects of regulation, completion, and ownership on mortality rates among hospitalized inpatients. N Engl J Med. 1988;318:1100–7.
Gray BH, McWerney WS. For-profit enterprise in health care. The institute of medicine study. N Engl J Med. 1986;314:1523–8.
Watt JM, Derzon RA, Renn SC, Schramm CS, Hahn JS, Pillari GD. The comparative economic performance of investor-owned chain and not-for-profit hospitals. N Engl J Med. 1986;314:89–96.
Pattison RV, Katz HM. Investor-owned and not-for-profit hospitals: comparison based on California data. N Engl J Med. 1983;309:347–53.
Campbell P, Kane N. Physician-management relationships at HCA: a case study. J Health Polit Policy Law. 1990;15(3):591–605.
Kuttner R. Columbia/HCA and the resurgence of the for-profit hospital business (first of two parts). N Engl J Med. 1996;335:446–51.
Kuttner R. Columbia/HCA and the resurgence of the for-profit hospital business (second of two parts). N Engl J Med. 1996;335(6):446–51.
Taylor DH, Whellan DJ, Sloan FA. Effects of admission to a teaching hospital on the cost and quality of care for Medicare beneficiaries. N Engl J Med 1999;340:293–9.
Burstin HR, Lipsitz SR, Udvarhelyi IS, Brennan TA. The effect of hospital financial characteristics on quality of care. JAMA. 1993;270:845–9.
Hartz AJ, Krakauer H, Kuhn EM, et al. Hospital characteristics and mortality rates. N Engl J Med. 1989;321:1720–5.
Hartz AJ, Gottlieb MS, Kuhn EM, Rimm AA. Relationship of hospital characteristics and the results of peer review in six larger states. Med Care. 1991;291:1028–38.
Hospital Association Guide to Hospitals. Chicago, Ill: American Hospital Association, 1993.
Health Care Investment Analysts. Directory of U.S. Hospitals. Baltimore, Md: HCIA; 1993.
Brennan TA, Leape LL, Laird NM, et al. Incidence of adverse events and negligence in hospitalized patients: results of the Harvard Medical Practice Study I. N Engl J Med. 1991;324:370–6.
Localio AR, Weaver SL, Landis R, et al. Identifying adverse events caused by care: degree of physician agreement in retrospective chart review. Ann Intern Med. 1996;125:457–64.
Bates DW, Cullen DJ, Laird N et al., for the ADE Prevention Study Group. Incidence of adverse drug events and potential adverse drug events: implications for prevention. JAMA. 1995;274:29–34.
Charlson ME, Pompei P, Ales KL, Mackenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40:373–83.
Diggle PJ, Liang K, Zeger SL. Analysis of Longitudinal Data. Oxford, UK: Clarendon Press; 1995.
Thomas EJ, Studdert DM, Burstin HR, et al. Incidence and types of adverse events and negligent care in Utah and Colorado in 1992. Med Care. 2000. In press.
Bloche MG. Should government intervene to protect nonprofits? Health Aff (Millwood). September/October 1998:7–25.
Schlesinger M, Gray BH, Bradley E. Charity and community: the role of non-profit ownership in a managed health care system. J Health Polit Policy Law. 1996;21:697–751.
Andrulis D, Acuff KL, Weiss KB, Anderson RJ. Public hospitals and health reform: choices and challenges. Am J Public Health. 1996;86:162–5.
Colorado Hospitals Reference Guide. Denver, Colo: Colorado Hospital Association; 1997.
Ginzberg E. The patient as profit center: Hospital Inc. comes to town. The Nation November 1996:18–22.
Cherry RL. Agents of nursing home quality of care: ombudsmen and staff ratios revisited. Gerontologist. 1991;31(3):302–8.
Iezzoni LI, Daley J, Heeren T, et al. Using administrative data to screen hospitals for high complication rates. Inquiry. 1994;31(1):40–55.
Munro DJ. The influence of registered nurse staffing on the quality of nursing home care. Res Nurs Health. 1990;13:263.
Silber JH, Rosenbaum PR, Schwartz JS, Ross RN, Williams SV. Evaluation of the complication rate as a measure of quality of care in coronary artery bypass graft surgery. JAMA. 1995;274(4):317–23.
Wan TT, Shukla RK. Contextual and organizational correlates of the quality of hospital nursing care. QRB Qual Rev Bull. 1987;13(2):61–4.
Limbacher PB. Another hit for Columbia. Mod Healthcare. 1998;28:2–4.
Limbacher P. Columbia: year in review—Federal probe, new management leave their mark. Mod Healthcare. 1998;28:26–30.
Hasan M. Let’s end the non-profit charade. N Engl J Med. 1996;335:1057–8.
Leape LL. Error in medicine. JAMA. 1994;272:1851–7.
Perrow C. Normal Accidents: Living with High Risk Technologies. New York, NY: Basic Books; 1984.
Reason J. Human Error. New York, NY: Cambridge University Press; 1990.
Moray N. Error reduction as a systems problem. In: Bogner MS, ed. Human Error in Medicine. Hillsdale, NJ: Erlbaum; 1994.
Brennan TA, Berwick DM. New Rules: Regulation, Markets and the Quality of American Health Care. San Francisco, Calif: Jossey-Bass Inc; 1996.
Elmore JG, Wells CK, Lee CH, Howard DH, Feinstein AR. Variability in radiologists’ interpretations of mammograms. N Engl J Med. 1994;331:1493–9.
Shekelle PG, Kahan JP, Bernstein SJ, Leape LL, Kamberg CJ, Park RE. The reproductibility of a method to identify the overuse and underuse of medical procedures. N Engl J Med. 1988;338:1888–95.
Brennan TA, Hebert LE, Laird NM, et al. Hospital characteristics associated with adverse events and substandard care. JAMA. 1991;265:3265–9.
Mitchell PH, Shortell SM. Adverse outcomes and variations in organization of care delivery. Med Care. 1997;35:NS19-NS32.
Leape LL, Bates DW, Cullen DJ, et al. Systems analysis of adverse drug events: ADE prevention group. JAMA. 1995;274(1):35–43.
Author information
Authors and Affiliations
Corresponding author
Additional information
Funding for this work was provided by the Robert Wood Johnson Foundation.
Rights and permissions
About this article
Cite this article
Thomas, E.J., Orav, E.J. & Brennan, T.A. Hospital ownership and preventable adverse events. J GEN INTERN MED 15, 211–219 (2000). https://doi.org/10.1111/j.1525-1497.2000.07003.x
Issue Date:
DOI: https://doi.org/10.1111/j.1525-1497.2000.07003.x