Abstract
Background
As many as 1,000,000 breast biopsies are performed annually in the United States. Although substantial effort has been devoted to estimating breast cancer risk, there have been no studies to predict outcome in women undergoing breast biopsy.
Methods
A population-based study was undertaken to develop and test models for predicting the probability of invasive breast cancer and/or ductal carcinoma-in-situ in 7670 women undergoing breast biopsy after mammography. Logistical prediction models were developed by using data from 6129 randomly selected women and tested with data from the remaining women.
Results
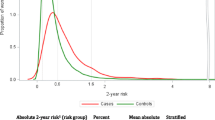
The overall cancer prevalence among women undergoing biopsy was 22.4%. Prevalence in women with mammograms highly suggestive of malignancy (category 5) was 84.6%, with minimal variation in individual cancer probabilities due to age. A total of 24.6% of women with suspicious mammograms (category 4) had cancer, but individual probability estimates ranged from .01 to .86, depending on age, presence of a lump, previous biopsy, menopausal status, and use of postmenopausal hormone therapy. These variables also influenced biopsy outcome in women with other mammography assessments (categories 0–3), but the overall prevalence was lower (8.6%), and estimated probabilities ranged from .01 to .45. When cancer was present, the probability of invasive disease was influenced by mammogram assessment category, absence of mammogram calcifications, and presence of a lump.
Conclusions
The probabilities of invasive cancer and ductal carcinoma-in-situ in women undergoing biopsy can be more accurately predicted by using clinical characteristics in addition to mammography findings. This information could potentially influence decisions regarding immediate biopsy or continued surveillance.




Similar content being viewed by others
References
Burns RP. Image-guided breast biopsyAm J Surg 1997;173:9–11
Hall JA, Murphy DC, Hall BR, Hall KA. Open surgical biopsy for nonpalpable mammographic abnormalities: still an option compared with core needle biopsy. Am J Obstet Gynecol 1998;178:1245–50
Poplack SP, Tosteson AN, Grove MR, Wells WA, Carney PA. Mammography in 53,803 women from the New Hampshire Mammography Network. Radiology 2000;217:832–40
Brett J, Austoker J, Ong G. Do women who undergo further investigation for breast screening suffer adverse psychological consequences? A multi-centre follow-up study comparing different breast screening result groups five months after their last breast screening appointment. J Public Health Med 1998;20:396–403
Gram IT, Lund E, Slenker SE. Quality of life following a false positive mammogram. Br J Cancer 1990;62:1018–22
Lerman C, Trock B, Rimer BK, Boyce A, Jepson C, Engstrom PF. Psychological and behavioral implications of abnormal mammogramsAnn Intern Med 1991;114:657–61
D’Orsi CJ, Bassett LW, Feig SA, et al. Illustrated Breast Imaging Reporting and Data System: Illustrated BI-RADS™. 3rd ed. Reston, VA: American College of Radiology, 1998
Liberman L, Abramson AF, Squires FB, Glassman JR, Morris EA, Dershaw DD. The breast imaging reporting and data system: positive predictive value of mammographic features and final assessment categories. AJR Am J Roentgenol 1998;171:35–40
Orel SG, Kay N, Reynolds C, Sullivan DC. BI-RADS categorization as a predictor of malignancy. Radiology 1999;211:845–50
Geller BM, Worden JK, Ashley JA, Oppenheimer RG, Weaver DL. Multipurpose statewide breast cancer surveillance system: the Vermont experience. J Registry Manage 1996;23:168–74
Hilsenbeck SG. Quality control. In: Menck H, Smart C, eds. Central Cancer Registries: Design, Management, and Use. Chur, Switzerland: Harwood Academic Publishers, 1994
Osius G, Rojek D. Normal goodness-of-fit tests for multinomial models with large degrees of freedom. J Am Stat Assoc 1992;87:1145–52
Rosenberg RD, Lando JF, Hunt WC, et al. The New Mexico Mammography Project: screening mammography performance in Albuquerque, New Mexico, 1991 to 1993. Cancer 1996;78:1731–9
Fuhrman GM, Cederbom GJ, Bolton JS, et al. Image-guided core-needle biopsy is an accurate technique to evaluate patients with nonpalpable imaging abnormalities. Ann Surg 1998;227:932–9
Liberman L. Percutaneous image-guided core breast biopsy. Radiol Clin North Am 2002;40:483–500
Acknowledgments
Supported by a grant (UO1-CA70013) from the National Cancer Institute.
Author information
Authors and Affiliations
Corresponding author
Additional information
The views expressed in this article are solely those of the authors and do not necessarily represent the official views of the National Cancer Institute or the Federal government.
Rights and permissions
About this article
Cite this article
Weaver, D.L., Vacek, P.M., Skelly, J.M. et al. Predicting Biopsy Outcome After Mammography: What Is the Likelihood the Patient Has Invasive or In Situ Breast Cancer?. Ann Surg Oncol 12, 660–673 (2005). https://doi.org/10.1245/ASO.2005.09.008
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/ASO.2005.09.008