Abstracts
Background
Needle localization breast biopsy (NLBB) is presently the primary means of localizing non-palpable lesions. Disadvantages of NLBB include vasovagal episodes, patient discomfort, and miss rates. Because hematomas naturally fill the cavity after vacuum-assisted breast biopsies (VABB), we hypothesized that ultrasound (US) could be used to find and accurately excise the actual biopsy site of non-palpable breast lesions without a needle.
Methods
This is a retrospective study from January 2000 to July 2005. Electronic chart review identified patients with non-palpable breast lesions detected by means of mammogram who then underwent lumpectomy via NLBB or the hematoma-directed ultrasound-guided technique (HUG). HUG involved localizing the hematoma with a 7.5-MHz US probe and using the “line of sight” technique straight down toward the chest wall. A block of tissue encompassing the hematoma was then excised.
Results
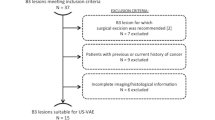
Localization procedures were performed in 186 patients—63 (34%) via needle localization and 123 (66%) via HUG. The previous VABB site in 100% of patients was successfully excised using HUG, 65 of 123 (53%) were benign and 58 of 123 (47%) were malignant; margins were positive in 13 of these 58 (22%). NLBB was successful in 100% of patients, 44 of 63 (70%) were benign and 19 of 63 (30%) were malignant; margins were positive in 14 of these 19 (73%). Margin positivity was significantly higher for NLBB than HUG (P = 0.0001, Fisher Exact).
Conclusions
This study suggests that HUG is more accurate in localizing non-palpable lesions than NLBB. By eliminating the additional procedure needed for NLBB, HUG may also be more time- and cost efficient. HUG makes VABB not only a less invasive diagnostic procedure, but also a localization procedure.






Similar content being viewed by others
Reference
Burns R. Image-guided breast biopsy. Am J Surg 1997; 173:9–11
Potterton AJ, Peakman DJ, Young JR. Ultrasound demonstration of small breast cancers detected by mammographic screening. Clin Radiol 1994; 49(11):808–813
Smith LF, Henry-Tillman R, Rubio IT, Korourian S, Klimberg VS. Intraoperative localization after stereotactic breast biopsy without a needle. Am J Surg 2001; 182(6):584–589
Rissanen TJ, Makarainen HP, Mattila SI, et al. Wire localized biopsy of breast lesions: A review of 425 cases found in screening or clinical mammography. Clin Radiol 1993; 47(1):14–22
Hasselgren PO, Hummel RP, Georgian-Smith D, Fieler M. Breast biopsy with needle localization: accuracy of specimen x-ray and management of missed lesions. Surgery 1993; 114(4):836–840; discussion 840–842
Homer MJ, Smith TJ, Safaii H. Prebiopsy needle localization. methods, problems, and expected results. Radiol Clin North Am 1992; 30(1):139–153
Snider HC, Jr, Morrison DG. Intraoperative ultrasound localization of nonpalpable breast lesions. Ann Surg Oncol 1999; 6(3):308–314
Burbank F, Forcier N. Tissue marking clip for stereotactic breast biopsy: initial placement accuracy, long-term stability, and usefulness as a guide for wire localization. Radiology 1997; 205(2):407–415
Liberman L, Dershaw DD, Morris EA, Abramson AF, Thornton CM, Rosen PP. Clip placement after stereotactic vacuum-assisted breast biopsy. Radiology 1997; 205(2):417–422
Fajardo LL, Bird RE, Herman CR, DeAngelis GA. Placement of endovascular embolization microcoils to localize the site of breast lesions removed at stereotactic core biopsy. Radiology 1998; 206(1):275–278
Gray RJ, Salud C, Nguyen K, et al. Randomized prospective evaluation of a novel technique for biopsy or lumpectomy of nonpalpable breast lesions: radioactive seed versus wire localization. Ann Surg Oncol 2001; 8(9):711–715
Children’s Mercy hospitals and clinics, STATS: Steve’s Attempt to Teach Statistics.http://www.cmh.edu/stats/ask/fishers.asp
Parker SH, Lovin JD, Jobe WE, et al. Stereotactic breast biopsy with a biopsy gun. Radiology 1990; 176(3):741–747
Lee CH, Egglin TK, Philpotts L, Mainiero MB, Tocino I. Cost-effectiveness of stereotactic core needle biopsy: analysis by means of mammographic findings. Radiology 1997; 202(3):849–854
Liberman L, Dershaw DD, Morris EA, Abramson AF, Thornton CM, Rosen PP. Clip placement after stereotactic vacuum-assisted breast biopsy. Radiology 1997; 205(2):417–422
Israel PZ, Fine RE. Stereotactic needle biopsy for occult breast lesions: a minimally invasive alternative. Am Surg 1995; 61:87–91
Velanovich V, Lewis FR, Jr, Nathanson SD, et al. Comparison of mammographically guided breast biopsy techniques. Ann Surg 1999; 229:625–630; discussion 630–633
Fuhrman GM, Cederbom GJ, Bolton JS, et al. Image-guided core-needle breast biopsy is an accurate technique to evaluate patients with nonpalpable imaging abnormalities. Ann Surg 1998; 227:932–939
Meyer JE, Smith DN, Lester SC, et al. Large-core needle biopsy of nonpalpable breast lesions. JAMA 1999; 281:1638–1641
Yim JH, Barton P, Weber B, et al. Mammographically detected breast cancer. Benefits of stereotactic core versus wire localization biopsy. Ann Surg 1996; 223(6):688–697; discussion 697–700
Bassett L, Winchester DP, Caplan RB, et al. Stereotactic core-needle biopsy of the breast: a report of the joint task force of the American College of Radiology, American College of Surgeons, and College of American Pathologists. CA Cancer J Clin 1997; 47(3):171–190
Smith LF, Rubio IT, Henry-Tillman R, Korourian S, Klimberg VS. Intraoperative ultrasound-guided breast biopsy. Am J Surg 2000; 180(6):419–423
Schwartz GF, Goldberg BB, Rifkin MD, D’Orazio SE. Ultrasonography: an alternative to x-ray-guided needle localization of nonpalpable breast masses. Surgery 1988; 104(5):870–873
Harlow SP, Krag DN, Ames SE, Weaver DL. Intraoperative ultrasound localization to guide surgical excision of nonpalpable breast carcinoma. J Am Coll Surg 1999; 189(3):241–246
Rubio IT, Henry-Tillman R, Klimberg VS. Surgical use of breast ultrasound. Surg Clin North Am 2003; 83(4):771–788
Henry-Tillman R, Johnson AT, Smith LF, Klimberg VS. Intraoperative ultrasound and other techniques to achieve negative margins. Semin Surg Oncol 2001; 20(3):206–213
Klimberg VS, Harms S, Korourian S. Assessing margin status. Surg Oncol 1999; 8(2):77–84
Pezner RD, Lipsett JA, Desai K, et al. To boost or not to boost: decreasing radiation therapy in conservative breast cancer treatment when “inked” tumor resection margins are pathologically free of cancer. Int J Radiat Oncol Biol Phys 1988; 14(5):873–877
Spivack B, Khanna MM, Tafra L, Juillard G, Giuliano AE. Margin status and local recurrence after breast-conserving surgery. Arch Surg 1994; 129(9):952–956; discussion 956–957
Freedman G, Fowble B, Hanlon A, et al. Patients with early stage invasive cancer with close or positive margins treated with conservative surgery and radiation have an increased risk of breast recurrence that is delayed by adjuvant systemic therapy. Int J Radiat Oncol Biol Phys 1999; 44(5):1005–1015
Park CC, Mitsumori M, Nixon A, et al. Outcome at 8 years after breast-conserving surgery and radiation therapy for invasive breast cancer: influence of margin status and systemic therapy on local recurrence. J Clin Oncol 2000; 18(8):1668–1675
Fortin A, Larochelle M, Laverdiere J, Lavertu S, Tremblay D. Local failure is responsible for the decrease in survival for patients with breast cancer treated with conservative surgery and postoperative radiotherapy. J Clin Oncol 1999; 17(1):101–109
Singletary SE. Surgical margins in patients with early-stage breast cancer treated with breast conservation therapy. Am J Surg 2002; 184(5):383–393
Swanson GP, Rynearson K, Symmonds R. Significance of margins of excision on breast cancer recurrence. Am J Clin Oncol 2002; 25(5):438–441
Lechner M, Day D, Elvecrog EL, et al. Ultrasound visibility of a new biopsy marker on serial evaluations. Radiology 2002; 225:115
Birdwell RL, Jackman RJ. Clip or marker migration 5–10 weeks after stereotactic 11-gauge vacuum-assisted breast biopsy: report of two cases. Radiology 2003; 29(2):541–544
Parikh JR. Ultrasound demonstration of clip migration to skin within 6 weeks of 11-gauge vacuum-assisted stereotactic breast biopsy. Breast J 2004; 0(6):539–542
Burnside ES, Sohlich RE, Sickles EA. Movement of a biopsy-site marker clip after completion of stereotactic directional vacuum-assisted breast biopsy: case report. Radiology 2001; 21(2):504–507
Philpotts LE, Lee CH. Clip migration after 11-gauge vacuum-assisted stereotactic biopsy: case report. Radiology 2002; 22(3):794–796
Harris AT. Clip migration within 8 days of 11-gauge vacuum-assisted stereotactic breast biopsy: case report. Radiology 2003; 28(2):552–554
Parikh JR. Clip migration within 15 days of 11-gauge vacuum-assisted stereotactic breast biopsy: case report. Am J Roentgenol 2005; 84(3 Suppl):S43–46
Parikh JR. Delayed migration of Gel Mark Ultra Clip within 15 days of 11-gauge vacuum-assisted stereotactic breast biopsy. Am J Roentgenol 2005; 85(1):203–206
Nurko J, Mancino AT, Whitacre E, Edwards MJ. Surgical benefits conveyed by biopsy site marking system using ultrasound localization. Am J Surg 2005; 190(4):618–622
Mullen DJ, Eisen RN, Newman RD, Perrone PM, Wilsey JC. The use of carbon marking after stereotactic large-core-needle breast biopsy. Radiology 2001; 218(1):255–260
Gray RJ, Salud C, Nguyen K, et al. Randomized prospective evaluation of a novel technique for biopsy or lumpectomy of nonpalpable breast lesions: radioactive seed versus wire localization. Ann Surg Oncol 2001; 8(9):711–715
Kass R, Kumar G, Klimberg VS, et al. Clip migration in stereotactic biopsy. Am J Surg 2002; 184(4):325–331
Gennari R, Galimberti V, De Cicco C, et al. Use of technetium-99m-labeled colloid albumin for preoperative and intraoperative localization of nonpalpable breast lesions. J Am Coll Surg 2000; 190(6):692–698; discussion 698–699
Thind CR, Desmond S, Harris O, Nadeem R, Chagla LS, Audisio RA. Radio-guided localization of clinically occult breast lesions (ROLL): a DGH experience. Clin Radiol 2005; 60(6):681–686
Zgajnar J, Hocevar M, Frkovic-Grazio S, Hertl K, Schweiger E, Besic N. Radioguided occult lesion localization (ROLL) of the nonpalpable breast lesions. Neoplasma 2004; 51(5):385–389
Author information
Authors and Affiliations
Corresponding author
Additional information
Margaret Thompson: Supported by the Virginia Clinton Kelley/Fashion Footwear Association of New York Breast Cancer Research Fellowship
Aaron Margulies: Supported by the Susan G. Komen Breast Cancer Clinical Fellowship
Rights and permissions
About this article
Cite this article
Thompson, M., Henry-Tillman, R., Margulies, A. et al. Hematoma-Directed Ultrasound-Guided (HUG) Breast Lumpectomy. Ann Surg Oncol 14, 148–156 (2007). https://doi.org/10.1245/s10434-006-9076-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-006-9076-y