Abstract
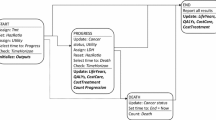
Schizophrenia is a chronic disease characterized by periods of relative stability interrupted by acute episodes (or relapses). The course of the disease may vary considerably between patients. Patient histories show considerable inter- and even intra-individual variability. We provide a critical assessment of the advantages and disadvantages of three modelling techniques that have been used in schizophrenia: decision trees, (cohort and micro-simulation) Markov models and discrete event simulation models. These modelling techniques are compared in terms of building time, data requirements, medico-scientific experience, simulation time, clinical representation, and their ability to deal with patient heterogeneity, the timing of events, prior events, patient interaction, interaction between covariates and variability (first-order uncertainty).
We note that, depending on the research question, the optimal modelling approach should be selected based on the expected differences between the comparators, the number of co-variates, the number of patient subgroups, the interactions between co-variates, and simulation time. Finally, it is argued that in case micro-simulation is required for the cost-effectiveness analysis of schizophrenia treatments, a discrete event simulation model is best suited to accurately capture all of the relevant interdependencies in this chronic, highly heterogeneous disease with limited long-term follow-up data.








Similar content being viewed by others
Notes
A probabilistic simulation generally requires a minimum of 1000 simulations of cohorts. This may be quite time consuming for a patient-level simulation model, as each cohort requires a number of patient simulations to generate the cohort. If the probabilistic simulation takes too long, one could consider using a meta model. By using a meta model, one reduces one layer of simulations, i.e. the patient-level simulation, of the micro-simulation models. This substantially reduces simulation time of the probabilistic sensitivity analysis. A recently introduced meta-modelling approach is the Gaussian process. Gaussian process models have the advantage that they can be fitted on fewer probabilistic input and output combinations and that they can be applied for nonlinear models.
References
Brennan A, Akehurst R. Modelling in health economic evaluation. What is its place? What is its value? Pharmacoeconomics 2000; 17: 445–459
Buxton MJ, Drummond MF, van Hout BA, et al. Modelling in economic evaluation: an unavoidable fact of life. Health Econ 1997; 6: 217–227
Karnon J, Brown J. Selecting a decision model for economic evaluation: a case study and review. Health Care Manag Sci 1998; 1: 133–140
Barton P, Bryan S, Robinson S. Modelling in the economic evaluation of health care: selecting the appropriate approach. J Health Serv Res Policy 2004 Apr; 9 (2): 110–118
Brennan A, Chick SE, Davies R. A taxonomy of model structures for economic evaluation of health technologies. Health Econ 2006; 15: 1295–1310
Glazer W, Ereshefsky L. A pharmacoeconomic model of outpatient antipsychotic therapy in “revolving door” schizophrenic patients. J Clin Psychiatry 1996; 57: 337–345
Edwards N, Rupnow F, Pashos C, et al. Cost-effectiveness model of long-acting risperidone in schizophrenia in the US. Pharmacoeconomics 2005; 23: 299–314
Palmer A, Revicki D, Genduso L, et al. A cost-effectiveness clinical decision analysis model for schizophrenia. Am J Manag Care 1998: 4: 345–355
Almond S, O’Donnel O. Cost analysis of the treatment of schizophrenia in the UK. A comparison of olanzapine and haloperidol. Pharmacoeconomics 1998; 13 (5): 575–588
Law A, Kelton D. Simulation modeling and analysis. 2nd ed. Singapore: McGraw-Hill, 1999
Heeg BMS, Buskens E, Knapp M, et al. Modelling the treated course of schizophrenia: development of a discrete event simulation model. Pharmacoeconomics 2005; 23 Suppl. 1: 17–33
Chue PS, Heeg BMS, Buskens E, et al. Modelling the impact of compliance on the costs and effects of long-acting risperidone in Canada. Pharmacoeconomics 2005; 23 Suppl. 1: 62–74
Laux G, Heeg BMS, van Hout BA, et al. Costs and effects of long-acting risperidone compared with oral atypical and conventional depot formulations in Germany. Pharmacoeconomics 2005; 23 Suppl. 1: 49–61
De Graeve D, Smet A, Mehnert A, et al. Long-acting risperidone compared with oral olanzapine and haloperidol depot in schizophrenia: a Belgian cost-effectiveness analysis. Pharmacoeconomics 2005; 23 Suppl. 1: 35–47
Hunink M, Glasziou P. Decision making in health and medicine: integrating evidence and values. 3rd ed. Cambridge: The press syndicate of the University of Cambridge, 2004
Vera-Llonch M, Delea T, Richardson E, et al. Outcomes and costs of risperidone versus olanzapine in patients with chronic schizophrenia or schizoaffective disorders: a Markov model. Value Health 2004; 7: 569–584
Clewell J, Baker R. Comments to the editor on “Outcomes and costs of risperidone versus olanzapine in patients with chronic schizophrenia or schizoaffective disorder: a Markov model”. Value Health 2005; 8: 175
Limpscomb J. Time preference for health in cost-effectiveness analysis. Med Care 1989; 27: S23–S53
Oakley J, O’Hagan A. Probabilistic sensitivity analyses of complex models: a Bayesian approach. J R Statist Soc 2005; 3: 751–769
Karnon J. Alternative decision modelling techniques for the evaluation of health care technologies: Markov processes versus discrete event simulation. Health Econ 2003; 12: 837–848
Habbema J, Lubbe J, van Oortmarssen GJ, et al. A simulation approach to cost-effectiveness and cost benefit calculations of screening for the early detection of disease. Eur J Operat Res 1987; 29: 159–166
van Hout BA, Bonsel G, Habbema D, et al. Heart transplantation in the Netherlands; costs, effects and scenarios. J Health Econ 1993; 12: 73–93
Caro J. Pharmacoeconomic analyses using discrete event simulation. Pharmacoeconomics 2005; 23 (4): 323–332
Rubio G, Martinez I, Ponce G, et al. Long-acting injectable risperidone compared with zuclopenthixol in the treatment of schizophrenia with substance abuse comorbidity. Can J Psychiatry 2006 Jul; 51 (8): 531–539
Davis JM, Chen N, Glick ID. A meta-analysis of the efficacy of second-generation antipsychotics. Arch Gen Psychiatry 2003 Jun; 60 (6): 553–564
Schooler N, Rabinowitz J, Davidson M, et al. Risperidone and haloperidol in first-episode psychosis: a long-term randomized trial. Am J Psychiatry 2005; 162: 1–7
Bagnall AM, Jones L, Ginnelly L, et al. A systematic review of atypical antipsychotic drugs in schizophrenia. Health Technol Assess 2003; 7 (13): 1–193
Lieberman J, Stroup S, McEvoy P, et al. Effectiveness of antipsychotic drugs in patients with chronic schizophrenia. N Engl J Med 2005; 353: 1209–1223
Geddes J, Freemantle N, Harrison P, et al. Atypical antipsychotics in the treatment of schizophrenia: systematic overview and meta-regression analysis. BMJ 2000 Dec 2; 321: 1371–1376
Emsley RA, Raniwalla J, Bailey PJ, et al. A comparison of the effects of quetiapine (’seroquel’) and haloperidol in schizophrenic patients with a history of and a demonstrated, partial response to conventional antipsychotic treatment. PRIZE Study Group. Int Clin Psychopharmacol 2000; 15: 121–131
Revicki D, Genduso L, Hamilton S, et al. Olanzapine versus haloperidol in the treatment of schizophrenia and other psychotic disorders: quality of life and clinical outcomes of a randomized clinical trial. Quality Life Res 1999; 8: 417–421
Lindenmayer JP, Czobor P, Volavka JLJ. Effects of atypical antipsychotics on the syndromal profile in treatment-resistant schizophrenia. J Clin Psychiatry 2004; 4: 551–556
Turner MS, Stewart DW. Review of the evidence for the long-term efficacy of atypical antipsychotic agents in the treatment of patients with schizophrenia and related psychoses. J Psychopharmacol 2006 Nov; 20 (6 Suppl.): 20–37
Jones PB, Barnes TR, Davies L, et al. Randomized controlled trial of the effect on quality of life of second- vs first-generation antipsychotic drugs in schizophrenia: Cost Utility of the Latest Antipsychotic Drugs in Schizophrenia Study (CUt-LASS 1). Arch Gen Psychiatry 2006 Oct; 63 (10): 1079–1087
Mahmoud R, Engelhart L, Janagap C, et al. Risperidone versus conventional antipsychotics for schizophrenia and schizoaffective disorder: symptoms, quality of life and resource use under customary clinical care. Clin Drug Invest 2004; 24: 275–286
Kane JM, Meltzer HY, Carson Jr WH, et al. Aripiprazole for treatment-resistant schizophrenia: results of a multicenter, randomized, double-blind, comparison study versus perphenazine. J Clin Psychiatry 2007 Feb; 68 (2): 213–223
Rabinowitz J, Lichtenberg P, Kaplan Z, et al. Rehospitalization rates of chronically ill schizophrenic patients discharged on a regimen of risperidone, olanzapine, or conventional antipsychotics. Am J Psychiatry 2001; 158: 266–269
Tunis S, Faries D, Nyhuis AW, et al. Cost-effectiveness of olanzapine as first-line treatment for schizophrenia: results from a randomized, open-label, 1-year trial. Value Health 2006; 9 (5): 357
Lenert L, Sturley A, Rapaport M, et al. Public preferences for health states with schizophrenia and a mapping function to estimate utilities from positive and negative symptom scale scores. Schizophr Res 2004; 71: 155–165
Weinstein MC, O’Brien B, Hornberger J, et al. Principles of good practice for decision analytic modeling in health-care evaluation: report of the ISPOR task force on good research practices. Value Health 2003; 6: 9–17
Weinstein MC, Siegel JE, Gold MR, et al. Recommendations of the Panel on Cost-effectiveness in Health and Medicine. JAMA 1996 Oct 16; 276 (15): 1253–1258
Sculpher M, Fenwick E, Claxton K. Assessing quality in decision analytic cost-effectiveness models: a suggested framework and example of application. Pharmacoeconomics 2000; 17: 461–477
Acknowledgements
Johnson & Johnson provided funding to Pharmerit BV to conduct the analysis and prepare the article. Sue Caleo is an employee of Johnson & Johnson. All remaining authors are employees of Pharmerit BV, which acted as a paid consultant to Johnson & Johnson, who market various antipsychotics.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Heeg, B.M.S., Damen, J., Buskens, E. et al. Modelling Approaches. Pharmacoeconomics 26, 633–648 (2008). https://doi.org/10.2165/00019053-200826080-00002
Published:
Issue Date:
DOI: https://doi.org/10.2165/00019053-200826080-00002