Abstract
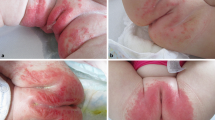
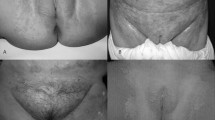
Eruptions in the diaper area are the most common dermatologic problem in infancy. Such eruptions can be subdivided into primary diaper dermatitis, an acute inflammation of the skin in the diaper area with an ill-defined and multifactorial etiology, and secondary diaper dermatitis, a term which encompasses eruptions in the diaper area with defined etiologies. The most important factors in the development of primary diaper dermatitis are: (i) water/moisture, (ii) friction, (iii) urine, (iv) feces, and (v) microorganisms (sometimes). Possible treatments include minimizing diaper use and using disposable diapers, barrier creams, mild topical cortisones, and antifungal agents. A variety of other inflammatory and infectious processes can occur in the diaper area and an awareness of these secondary types of diaper dermatitis aids in the accurate diagnosis and treatment of patients.




Similar content being viewed by others
References
Levy M. Diaper rash syndrome or dermatitis. Cutis. 2001; 67 (5 Suppl.): 37–8
Wolf R, Wolf D, Tuzun B, et al. Diaper dermatitis. Clin Dermatol. 2000; 18: 657–60
Leyden JJ. Diaper dermatitis. Dermatol Clin. 1986; 4: 23–8
Atherton DJ. The aetiology and management of irritant diaper dermatitis. J Eur Acad Dermatol Venereol. 2001; 15 Suppl. 1: 1–4
Zimmerer RE, Lawson KD, Calvert CJ. The effects of wearing diapers on skin. Pediatr Dermatol. 1986; 3: 95–101
Flagothier C, Pierard-Franchimont C, Pierard GE. How I explore diaper dermatitis. Rev Med Liege. 2004; 59: 106–9
Berg RW, Buckingham KW, Stewart RL. Etiologic factors in diaper dermatitis: the role of urine. Pediatr Dermatol. 1986; 3: 102–6
Donaldson RM. Normal bacterial populations of the intestine and their relation to intestinal function. N Engl J Med. 1964; 270: 938–45
Berg RW, Milligan MC, Sarbaugh FC. Association of skin wetness and pH with diaper dermatitis. Pediatr Dermatol. 1994; 11: 18–20
Buckingham KW, Berg RW. Etiologic factors in diaper dermatitis: the role of feces. Pediatr Dermatol. 1986; 3: 107–12
Atherton DJ. A review of the pathophysiology, prevention and treatment of irritant diaper dermatitis. Curr Med Res Opin. 2004; 20: 645–9
Ferrazzini G, Kaiser RR, Hirsig Cheng SK, et al. Microbiological aspects of diaper dermatitis. Dermatology. 2003; 206: 136–41
Weston WL, Lane AT, Weston JA. Diaper dermatitis: current concepts. Pediatrics. 1980; 66: 532–6
Gokalp AS, Aldirmaz C, Oguz A, et al. Relation between the intestinal flora and diaper dermatitis in infancy. Trop Geogr Med. 1990; 42: 238–40
Brook I. The effects of amoxicillin therapy on skin flora in infants. Pediatr Dermatol. 2000; 17: 360–3
Honig PJ, Gribetz B, Leyden JJ, et al. Amoxicillin and diaper dermatitis. J Am Acad Dermatol. 1988; 19 (2 Pt 1): 275–9
Rattet JP, Headley JL, Barr RJ. Diaper dermatitis with psoriasiform ID eruption. Int J Dermatol. 1981; 20: 122–5
Hamada T. Granuloma intertriginosum infantum (granuloma glutaeale infantum) [letter]. Arch Dermatol. 1975; 111: 1072–3
Tappeiner J, Pfleger L. Granuloma gluteale infantum. Hautarzt. 1971; 22: 383–8
Uyeda K, Nakayasu K, Takaishi Y, et al. Kaposi sarcoma-like granuloma on diaper dermatitis: a report of five cases. Arch Dermatol. 1973; 107: 605–7
Hurwitz. Clinical pediatric dermatology. 2nd Ed. Cutaneous disorders of the newborn. Philadelphia (PA): Saunders, 1993: 7–45
De Zeeuw R, Van Praag MC, Oranje AP. Granuloma gluteale infantum: a case report. Pediatr Dermatol. 2000; 17: 141–3
Bonifazi E, Garofalo L, Lospalluti M, et al. Granuloma gluteale infantum with atrophic scars: clinical and histological observations in eleven cases. Clin Exp Dermatol. 1981; 6: 23–9
Bluestein J, Fumer BB, Phillips D. Granuloma gluteale infantum: case report and review of the literature. Pediatr Dermatol. 1990; 7: 196–8
Uyeda K, Nakayasu K, Takaishi Y, et al. Electron microscopic observations of the so-called granuloma glutaeale infantum. J Cutan Pathol. 1974; 1: 26–32
Virgili A, Corazza M, Califano A. Diaper dermatitis in an adult: a case of erythema papuloerosive of Sevestre and Jacquet. J Reprod Med. 1998; 43: 949–51
Maekawa Y, Kiyoi K, Kunitake Y. Hemilateral distribution of papular lesions on the buttock histologically resembling granuloma gluteale infantum. J Dermatol. 2001; 28: 231–3
Silverberg NB, Laude TA. Jacquet diaper dermatitis: a diagnosis of etiology [letter]. Pediatr Dermatol. 1998; 15: 489
Rodriguez-Poblador J, Gonzalez-Castro U, Herranz-Martinez S, et al. Jacquet erosive diaper dermatitis after surgery for Hirschsprung disease. Pediatr Dermalot. 1998; 15: 46–7
Hara M, Watanabe M, Tagami H. Jacquet erosive diaper dermatitis in a young girl with urinary incontinence. Pediatr Dermatol. 1991; 8: 160–1
Goldberg NS, Esterly NB, Rothman KF, et al. Perianal pseudoverrucous papules and nodules in children. Arch Dermatol. 1992; 128: 240–2
Tamaki K. Diaper dermatitis and perianal pseudoverrucous papules [letter]. Arch Dermatol. 1992; 128: 1277
Coppo P, Salomone R. Pseudoverrucous papules: an aspect of incontinence in children. J Fur Acad Dermatol Venereol. 2002; 16: 409–10
Amity SA, Pride HB, Tyler WB. Perianal pseudoverrucose papules and nodules mimicking condylomata acuminata and child sexual abuse. Cutis. 2001; 67: 335–8
Rodriguez Cano L, Garcia-Patos Briones V, Pedragosa Jove R, et al. Perianal pseudoverrucous papules and nodules after surgery for Hirschsprung disease. J Pediatr. 1994; 125 (6 Pt 1): 914–6
Bourrat E, Vaquin C, Prigent F, et al. Perianal papulonodular dermatitis in Hirschsprung disease. Ann Dermatol Venereol. 1996; 123: 549–51
Rowen JL. Mucocutaneous candidiasis. Semin Perinatol. 2003; 27: 406–13
Philipp R, Hughes A, Golding J. Getting to the bottom of nappy rash. ALSPAC Survey Team. Avon Longitudinal Study of Pregnancy and Childhood. Br J Gen Pract. 1997; 47: 493–7
Verbov J. Skin problems in children. Practitioner. 1976; 217: 403–15
Odueko OM, Onayemi O, Oyedeji GA. A prevalence survey of skin diseases in Nigerian children. Niger J Med. 2001; 10: 64–7
Nanda A, Al-Hasawi F, Alsaleh QA. A prospective survey of pediatric dermatology clinic patients in Kuwait: an analysis of 10,000 cases. Pediatr Dermatol. 1999; 16: 6–11
Jordan WE, Lawson KD, Berg RW, et al. Diaper dermatitis: frequency and severity among a general infant population. Pediatr Dermatol. 1986; 3: 198–207
Visscher MO, Chatterjee R, Munson KA, et al. Development of diaper rash in the newborn. Pediatr Dermatol. 2000; 17: 52–7
Yates VM. Diaper dermatitis. In: Lebwohl MG, Heymann WR, Berth-Jones J, Coulson I, editors. Treatment of skin disease. London: Mosby, 2002: 161–162
Berg RW. Etiology and pathophysiology of diaper dermatitis. Adv Dermatol. 1988; 3: 75–98
Kazaks EL, Lane AT. Diaper dermatitis. Pediatr Clin North Am. 2000; 47: 909–19
Spraker MK. Update: diapers and diaper dermatitis. Pediatr Dermatol. 2000; 17: 75–83
Davis JA, Leyden JJ, Grove GL, et al. Comparison of disposable diapers with fluff absorbent and fluff plus absorbent polymers: effects on skin hydration, skin pH, and diaper dermatitis. Pediatr Dermatol. 1989; 6: 102–8
Odio M, Streicher-Scott J, Hansen RC. Disposable baby wipes: efficacy and skin mildness. Dermatol Nurs 2001; 13: 107–12, 117–8, 121
Prasad HR, Srivastava P, Verma KK. Diaper dermatitis: an overview. Indian J Pediatr. 2003; 70: 635–7
Jaffe GV, Grimshaw JJ. An open trial of clotrimazole plus hydrocortisone cream in the treatment of napkin dermatitis in general practice. Pharmatherapeutica. 1985; 4: 314–8
Bowring AR, Mackay D, Taylor FR. The treatment of napkin dermatitis: a doubleblind comparison of two steroid-antibiotic combinations. Pharmatherapeutica. 1984; 3: 613–7
Railan D, Wilson JK, Feldman SR, et al. Pediatricians who prescribe clotrimazole-betamethasone dipropionate (Lotrisone) often utilize it in inappropriate settings regardless of their knowledge of the drug’s potency [abstract]. Dermatol Online. 2002; 8: 3
Ward DB, Fleischer AB, Feldman SR, et al. Characterization of diaper dermatitis in the United States. Arch Pediatr Adolesc Med. 2000; 154: 943–6
Concannon P, Gisoldi E, Phillips S, et al. Diaper dermatitis: a therapeutic dilemma. Results of a double-blind placebo controlled trial of miconazole nitrate 0.25%. Pediatr Dermatol. 2001; 18: 149–55
Pierard-Franchimont C, Letawe C, Pierard GE. Tribological and mycological consequences of the use of a miconazole nitrate-containing paste for the prevention of diaper dermatitis: an open pilot study. Fur J Pediatr. 1996; 155: 756–8
Odio M, Friedlander SF. Diaper dermatitis and advances in diaper technology. Curr Opin Pediatr. 2000; 12: 342–6
Baldwin S, Odio MR, Haines SL, et al. Skin benefits from continuous topical administration of a zinc oxide/petrolatum formulation by a novel disposable diaper. J Fur Acad Dermatol Venereol. 2001; 15 Suppl. 1: 5–11
Wilson PA, Dallas MJ. Diaper performance: maintenance of healthy skin. Pediatr Dermatol. 1990; 7: 179–84
Campbell RL, Seymour JL, Stone LC, et al. Clinical studies with disposable diapers containing absorbent gelling materials: evaluation of effects on infant skin condition. J Am Acad Dermatol. 1987; 17: 978–87
Akin F, Spraker M, Aly R, et al. Effects of breathable disposable diapers: reduced prevalence of Candida and common diaper dermatitis [abstract]. Pediatr Dermatol. 2001; 18: 282–90
Gibbs DL, Kashin P, Jevons S. Comparative and non-comparative studies of the efficacy and tolerance of tioconazole cream 1% versus another imidazole and/or placebo in neonates and infants with candidal diaper rash and/or impetigo. J Int Med Res. 1987; 15: 23–31
de Wet PM, Rode H, van Dyk A, et al. Perianal candidosis: a comparative study with mupirocin and nystatin. Int J Dermatol. 1999; 38: 618–22
Minnich SM, Moeschberger M, Anderson J. Effect of oxyquinoline ointment on diaper dermatitis. Dermatol Nurs. 1991; 3: 25–8, 40
Munz D, Powell KR, Pai CH. Treatment of candidal diaper dermatitis: a double-blind placebo-controlled comparison of topical nystatin with topical plus oral nystatin. J Pediatr. 1982; 101: 1022–5
Lubec G. Treatment of diaper rash with Parfenac lipid ointment (bufexamac): a study by Austrian pediatricians. Padiatr Padol. 1989; 24: 227–36
Arad A, Mimouni D, Ben-Amitai D, et al. Efficacy of topical application of eosin compared with zinc oxide paste and corticosteroid cream for diaper dermatitis. Dermatology. 1999; 199: 319–22
Collipp PJ. Effect of oral zinc supplements on diaper rash in normal infants. J Med Assoc Ga. 1989; 78: 621–3
Bosch-Banyeras JM, Catala M, Mas P, et al. Diaper dermatitis: value of vitamin A topically applied. Clin Pediatr (Phila). 1988; 27: 448–50
Markham T, Kennedy F, Collins P. Topical sucralfate for erosive irritant diaper dermatitis. Arch Dermatol. 2000; 136: 1199–200
Leyden JJ. Corn starch, Candida albicans, and diaper rash. Pediatr Dermatol. 1984; 1: 322–5
White CM, Gailey RA, Lippe S. Cholestyramine ointment to treat buttocks rash and anal excoriation in an infant. Ann Pharmacother. 1996; 30: 954–6
Mowad CM, McGinley KJ, Foglia A, et al. The role of extracellular polysaccharide substance produced by Staphylococcus epidermidis in miliaria. J Am Acad Dermatol. 1995; 33 (5 Pt 1): 729–33
Boiko S. Treatment of diaper dermatitis. Dermatol Clin. 1999; 17: 235–40
Boiko S. Diapers and diaper rashes. Dermatol Nurs. 1997; 9: 33–9, 43–6, 66, 70
Sires UI, Mallory SB. Diaper dermatitis: how to treat and prevent. Postgrad Med. 1995; 98: 79–84, 86
Watanabe M, Tabata N, Tagami H. Explosive diaper pustular psoriasis. Pediatr Dermatol. 2002; 19: 564–5
Patrizi A, Neri I, Misciali C, et al. Granular parakeratosis: four paediatric cases. Br J Dermatol. 2002; 147: 1003–6
Chang MW, Kaufmann JM, Orlow SJ, et al. Infantile granular parakeratosis: recognition of two clinical patterns. J Am Acad Dermatol. 2004; 50 (5 Suppl.): S93–6
Lee JY, Chang SE, Sub CW, et al. A case of acrodermatitis enteropathica-like dermatosis caused by omithine transcarbamylase deficiency. J Am Acad Dermatol. 2002; 46: 965–7
Higuchi R, Mizukoshi M, Koyama H, et al. Intractable diaper dermatitis as an early sign of biotin deficiency. Acta Paediatr. 1998; 87: 228–9
Perafan-Riveros C, Franca LF, Alves AC, et al. Acrodermatifs enteropathica: case report and review of the literature. Pediatr Dermatol. 2002; 19: 426–31
Guerrero Vazquez J, Garces Ramos A, Olmedo San Laureano S, et al. Diaper rash in Kawasaki disease [published erratum appears in An Esp Pediatr 1990; 32: 565] [in Spanish]. An Esp Pediatr. 1990; 32: 246–8
Krowchuk DP, Bass J, Elgart GW. Kawasaki disease with an exanthem limited to the diaper area. Am J Dis Child. 1988; 142: 1136–7
Honda M. Differential diagnosis of unusual skin diseases in infants. Pediatrician. 1987; 14 Suppl. 1: 15–7
Siegfried S, Nopper AJ, Draelos Z, et al. Principles of treatment in pediatric dermatology. In: Schacher L, Hansen R, editors. Pediatric dermatology. 3rd ed. Edinburgh: Mosby, 2003: 87–128
Fisher AA. Allergic contact dermatitis in early infancy. Cutis. 1994; 54: 300–2
Belhadjali H, Giordano-Labadie F, Rance F, et al. “Lucky Luke” contact dermatitis from diapers: a new allergen? [abstract]. Contact Dermatitis. 2001; 44: 248
Draelos ZD. Hydrogel barrier/repair creams and contact dermatitis [abstract]. Am J Contact Dermatol. 2000; 11: 222–5
Larralde M, Raspa ML, Silvia H, et al. Diaper dermatitis: a new clinical feature. Pediatr Dermatol. 2001; 18: 167–8
Rout S, Ducombs G, Leaute-Labreze C, et al. ‘Lucky Luke’ contact dermatitis due to rubber components of diapers. Contact Dermatitis. 1998; 38: 363–4
Hoppe JE. Treatment of oropharyngeal candidiasis and candidal diaper dermatitis in neonates and infants: review and reappraisal. Pediatr Infect Dis J. 1997; 16: 885–94
Passeron T, Desruelles F, Gari-Toussaint M, et al. Invasive fungal dermatitis in a 770 gram neonate. Pediatr Dermatol. 2004; 21: 260–1
Dorko E, Viragova S, Pilipcinec E, et al. Candida: agent of the diaper dermatitis?. Folia Microbiol (Praha). 2003; 48: 385–8
Baudraz-Rosselet F, Ruffieux P, Mancarella A, et al. Diaper dermatitis due to Trichophyton verrucosum. Pediatr Dermatol. 1993; 10: 368–9
Hayden GF. Dermatophyte infection in the diaper area: report of two cases. Pediatr Infect Dis. 1985; 4: 289–91
Kahana M, Levi A, Cohen M, et al. Dermatophytosis of the diaper area. Clin Pediatr (Phila). 1987; 26: 149–51
Rasmussen JE. Classification of diaper dermatitis: an overview. Pediatrician 1987; 14 Suppl. 1: 6–10
Rehder PA, Eliezer ET, Lane AT. Perianal cellulitis: cutaneous group A strepto-coccal disease. Arch Dermatol. 1988; 124: 702–4
Brook I. Microbiology of secondarily infected diaper dermatitis. Int J Dermatol. 1992; 31: 700–2
Thiboutot DM, Beckford A, Mart CR, et al. Cytomegalovirus diaper dermatitis. Arch Dermatol. 1991; 127: 396–8
Jenson HB, Shapiro ED. Primary herpes simplex virus infection of a diaper rash. Pediatr Infect Dis J; 1987; 6: 1136–8
Graham-Brown RA, Lister DM, Burns DA. Herpetiform napkin dermatitis: napkin dermatitis simulating an acute herpes simplex infection. Br J Dermatol. 1986; 114: 746–7
Acknowledgments
No sources of funding were used to assist in the preparation of this review. The author has no conflicts of interest that are directly relevant to the content of this review.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Scheinfeld, N. Diaper Dermatitis. Am J Clin Dermatol 6, 273–281 (2005). https://doi.org/10.2165/00128071-200506050-00001
Published:
Issue Date:
DOI: https://doi.org/10.2165/00128071-200506050-00001